Abstract
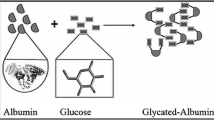
Glycation is a non-enzymatic reaction that is initiated by the primary addition of sugars to amino groups of proteins. In the early phase of glycation, the synthesis of intermediates leads to formation of Amadori compounds. In the last phase, advanced glycation end products (AGE) are irreversibly formed following a complex cascade of reactions. It has recently been shown that glycation also affects diabetes-related complications and Alzheimer’s disease. In this study, human serum albumin at a concentration of 10 mg/ml was incubated in PBS with 40 mM of glucose and in different concentrations of papaverine (25, 100, 250, 500 μM) for 42 days at 37 °C. HSA with no additives as well as with glucose 40 mM were incubated as a control and as a glycated sample, respectively. Following the incubation, the samples were prepared for circular dichroism, fluorescence and absorbance techniques. The results showed that in presence of papaverine and glucose, the glycation of HSA increased notably compared with the glycated sample. In conclusion, in this work, we showed that papaverine affects HSA and increases its glycation level.









Similar content being viewed by others
References
Uribarri, J., Woodruff, S., Goodman, S., Cai, W., Chen, X., Pyzik, R., et al.: Advanced glycation end products in foods and a practical guide to their reduction in the diet. J. Am. Diet. Assoc. 110(6), 911–916 e12 (2010)
Rabbani, N., Chittari, M.V., Bodmer, C.W., Zehnder, D., Ceriello, A., Thornalley, P.J.: Increased glycation and oxidative damage to apolipoprotein B100 of LDL cholesterol in patients with type 2 diabetes and effect of metformin. Diabetes 59(4), 1038–1045 (2010)
Ulrich, P., Cerami, A.: Protein glycation, diabetes, and aging. Recent Prog. Horm. Res. 56, 1–21 (2001)
Nathan, D.M., Cleary, P.A., Backlund, J.Y., Genuth, S.M., Lachin, J.M., Orchard, T.J., et al.: Intensive diabetes treatment and cardiovascular disease in patients with type 1 diabetes. N. Engl. J. Med. 353(25), 2643–2653 (2005)
Vlassara, H., Cai, W., Crandall, J., Goldberg, T., Oberstein, R., Dardaine, V., et al.: Inflammatory mediators are induced by dietary glycotoxins, a major risk factor for diabetic angiopathy. Proc. Natl. Acad. Sci. U.S.A. 99(24), 15596–15601 (2002)
Zieman, S.J., Melenovsky, V., Kass, D.A.: Mechanisms, pathophysiology, and therapy of arterial stiffness. Arterioscler. Thromb. Vasc. Biol. 25(5), 932–943 (2005)
Twigg, S.M., Cao, Z.,McLennan, S.V., Burns,W.C., Brammar, G., Forbes, J.M., et al.: Renal connective tissue growth factor induction in experimental diabetes is prevented by aminoguanidine. Endocrinology 143(12), 4907–4915 (2002)
Forbes, J.M., Cooper, M.E., Oldfield, M.D., Thomas, M.C.: Role of advanced glycation end products in diabetic nephropathy. J. Am. Soc. Nephrol. 14(8 Suppl 3), S254–S258 (2003)
Gallicchio, M.A., McRobert, E.A., Tikoo, A., Cooper, M.E., Bach, L.A.: Advanced glycation end products inhibit tubulogenesis and migration of kidney epithelial cells in an ezrin-dependent manner. J. Am. Soc. Nephrol. 17(2), 414–421 (2006)
Stitt, A.W.: Advanced glycation: an important pathological event in diabetic and age related ocular disease. Br. J. Ophthalmol. 85(6), 746–753 (2001)
Okamoto, K., Martin, D.P., Schmelzer, J.D., Mitsui, Y., Low, P.A.: Pro- and anti-inflammatory cytokine gene expression in rat sciatic nerve chronic constriction injury model of neuropathic pain. Exp. Neurol. 169(2), 386–391 (2001)
Rohrer, L., Hersberger, M., von Eckardstein, A.: High density lipoproteins in the intersection of diabetes mellitus, inflammation and cardiovascular disease. Curr. Opin. Lipidol. 15(3), 269–278 (2004)
Nobecourt, E., Jacqueminet, S., Hansel, B., Chantepie, S., Grimaldi, A., Chapman, M.J., et al.: Defective antioxidative activity of small dense HDL3 particles in type 2 diabetes: relationship to elevated oxidative stress and hyperglycaemia. Diabetologia 48(3), 529–538 (2005)
Soro-Paavonen, A., Zhang, W.Z., Venardos, K., Coughlan, M.T., Harris, E., Tong, D.C.K., et al.: Advanced glycation end-products induce vascular dysfunction via resistance to nitric oxide and suppression of endothelial nitric oxide synthase. J. Hypertens. 28(4), 780–788 (2010)
Zhao, T., Cheng, Y.N., Tan, H.N., Liu, J.F., Xu, H.L., Pang, G.L., et al.: Site-specific chemical modification of human serum albumin with polyethylene glycol prolongs half-life and improves intravascular retention in mice. Biol. Pharm. Bull. 35(3), 280–288 (2012)
Iberg, N., Fluckiger, R.: Nonenzymatic glycosylation of albumin in vivo. Identification of multiple glycosylated sites. J. Biol. Chem. 261(29), 13542–13545 (1986)
Rohovec, J.,Maschmeyer, T., Aime, S., Peters, J.A.: The structure of the sugar residue in glycated human serum albumin and its molecular recognition by phenylboronate. Chemistry 9(10), 2193–2199 (2003)
Anguizola, J., Matsuda, R., Barnaby, O.S., Hoy, K.S., Wa, C., Debolt, E., et al.: Review: glycation of human serum albumin. Clin. Chim. Acta 425C, 64–76 (2013)
Khan, M.W., Qadrie, Z.L., Khan, W.A.: Antibodies against gluco-oxidatively modified human serum albumin detected in diabetes-associated complications. Int. Arch. Allergy Immunol. 153(2), 207–214 (2010)
Barnaby, O.S.: Characterization of Glycation Sites on Human Serum Albumin usingMass Spectrometry, pp. 1–256. Student Research Projects, Dissertations, and Theses - Chemistry Department (2010)
Khan, M.W., Rasheed, Z., Khan, W.A., Ali, R.: Biochemical, biophysical, and thermodynamic analysis of in vitro glycated human serum albumin. Biochemistry (Mosc) 72(2), 146–152 (2007)
Azod, L., Rashidi, M., Afkhami-Ardekani, M., Kiani, G., Khoshkam, F.: Effect of opium addiction on diabetes. Am. J. Drug Alcohol Abuse 34(4), 383–388 (2008)
Merits, V.: The opium alkaloids and diabetes. J. Am. Med. Assoc. 9, 786 (1914)
Opium –Wikipedia, the Free Encyclopedia. http://en.wikipedia.org/wiki/opium(18/10/2010)
Karam, G.A., Rashidinejad, H.R., Aghaee, M.M., Ahmadi, J., Rahmani, M.R., Mahmoodi, M., et al.: Opium can differently alter blood glucose, sodium and potassium in male and female rats. Pak. J. Pharm. Sci. 21(2), 180–184 (2008)
Schmitt, A., Gasic-Milenkovic, J., Schmitt, J.: Characterization of advanced glycation end products: mass changes in correlation to side chain modifications. Anal. Biochem. 346(1), 101–106 (2005)
Valencia, J.V., Weldon, S.C., Quinn, D., Kiers, G.H., DeGroot, J., TeKoppele, J.M., et al.: Advanced glycation end product ligands for the receptor for advanced glycation end products: biochemical characterization and formation kinetics. Anal. Biochem. 324(1), 68–78 (2004)
Sattarahmady, N., Khodagholi, F., Moosavi-Movahedi, A.A., Heli, H., Hakimelahi, G.H.: Alginate as an antiglycating agent for human serum albumin. Int. J. Biol. Macromol. 41(2), 180–184 (2007)
Yan, S.F., Ramasamy, R., Schmidt, A.M.: Mechanisms of disease: advanced glycation end-products and their receptor in inflammation and diabetes complications. Nat. Clin. Pract. Endoc. 4(5), 285–293 (2008)
Sharma, S.D., Pandey, B.N., Mishra, K.P., Sivakami, S.: Amadori product and age formation during nonenzymatic glycosylation of bovine serum albumin in vitro. J. Biochem. Mol. Biol. Biophys. 6(4), 233–242 (2002)
Habeeb, A.F.: Determination of free amino groups in proteins by trinitrobenzenesulfonic acid. Anal. Biochem. 14(3), 328–336 (1966)
Kumar, P.A., Kumar,M.S., Reddy, G.B.: Effect of glycation on alpha-crystallin structure and chaperone-like function. Biochem. J. 408(2), 251–258 (2007)
Barnaby, O.S., Cerny, R.L., Clarke,W., Hage, D.S.: Quantitative analysis of glycation patterns in human serum albumin using 16O/18O-labeling and MALDI-TOF MS. Clin. Chim. Acta 412(17–18), 1606–1615 (2011)
Wa, C., Cerny, R.L., Clarke, W.A., Hage, D.S.: Characterization of glycation adducts on human serum albumin by matrix-assisted laser desorption/ionization time-of-flight mass spectrometry. Clin. Chim. Acta 385(1–2), 48–60 (2007)
Karam, G.A., Reisi, M., Kaseb, A.A., Khaksari, M., Mohammadi, A., Mahmoodi, M.: Effects of opium addiction on some serum factors in addicts with non-insulin-dependent diabetes mellitus. Addict. Biol. 9(1), 53–58 (2004)
Nakayama, M., Saito, A., Kitazawa, H., Takahashi, M., Sato, M., Fuse, K., et al.: Papaverine-induced polymorphic ventricular tachycardia in relation to QTU and giant T-U waves in four cases. Intern. Med. 51(4), 351–356 (2012)
De Bruyne, B., Pijls, N.H., Barbato, E., Bartunek, J., Bech, J.W., Wijns, W., et al.: Intracoronary and intravenous adenosine 5′-triphosphate, adenosine, papaverine, and contrast medium to assess fractional flow reserve in humans. Circulation 107(14), 1877–1883 (2003)
Asgari, S.A., Asli, M.M., Madani, A.H., Maghsoudi, P.A., Ghanaei, M.M., Shakiba, M., et al.: Treatment of loin pain suspected to be renal colic with papaverine hydrochloride: a prospective double-blind randomised study. BJU Int. 110(3), 449–452 (2012)
Greenfield, N.J.: Using circular dichroism spectra to estimate protein secondary structure. Nat. Protoc. 1(6), 2876–2890 (2006)
Khazaei, M.R., Bakhti, M., Habibi-Rezaei, M.: Nicotine reduces the cytotoxic effect of glycated proteins on microglial cells. Neurochem. Res. 35(4), 548–558 (2010)
Jakus, V.: Study of inhibition of protein glycation by fluorescence spectroscopy. Biomed. 54(192), 446 (1997)
Nawale, R.B., Mourya, V.K., Bhise, S.B.: Non-enzymatic glycation of proteins: a cause for complications in diabetes. Indian J. Biochem. Biophys. 43(6), 337–344 (2006)
Watkins, N.G., Neglia-Fisher, C.I., Dyer, D.G., Thorpe, S.R., Baynes, J.W.: Effect of phosphate on the kinetics and specificity of glycation of protein. J. Biol. Chem. 262(15), 7207–7212 (1987)
Belpaire, F.M., Bogaert, M.G.: Metabolism of papaverine. II. Species differences. Xenobiotica 5(7), 421–429 (1975)
Seidler, N.W., Yeargans, G.S.: Effects of thermal denaturation on protein glycation. Life Sci. 70(15), 1789–1799 (2002)
Kapp, E.A., Daya, S., Whiteley, C.G.: Protein-ligand interactions: interaction of nitrosamines with nicotinic acetylcholine receptor. Biochem. Biophys. Res. Commun. 167(3), 1383–1392 (1990)
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ahmadzadeh, A. Papaverine increases human serum albumin glycation. J Biol Phys 40, 97–107 (2014). https://doi.org/10.1007/s10867-013-9337-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10867-013-9337-5