Abstract
Purpose
To analyze tear meniscus measurements with optical coherence tomography (OCT) in patients with canalicular laceration repair.
Methods
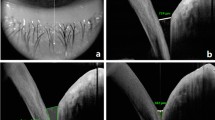
Thirty-four consecutive patients who underwent unilateral canalicular repair due to canalicular laceration between January 2014 and December 2018 were included. All patients had canalicular repair followed by monocanalicular or annular silicone tube intubation. Anatomic patency of canalicular system was tested with probing and irrigation, while functional patency was evaluated with Munk score. Tear meniscus measurements of all patients were obtained following tube removal by spectral OCT. Tear meniscus height (TMH), tear meniscus depth (TMD) and tear meniscus area (TMA) of eyes with canalicular laceration repair and contralateral uninvolved eyes were compared.
Results
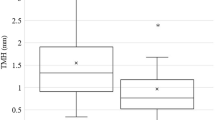
Average age of 34 patients was 32.8 ± 21.3 years (range 4–68 years). Lower canaliculus was involved in 27 (79.4%), upper canaliculus in five (14.7%), and both canaliculi in two (5.9%) patients. Mean follow-up period was 6.5 ± 5.7 months. Anatomic patency rate was 100%, and functional patency (patients free of epiphora) was 91.2%. Average TMH (317.9 ± 133.1 µm), TMD (198.1 ± 82.5 µm) and TMA (29,792.1 ± 21,285.3 μm2) values of eyes with canalicular repair were not significantly different from TMH (308.9 ± 111.9 µm), TMD (184.5 ± 61.4 µm) and TMA (26,682.5 ± 16,178.1 μm2) values of contralateral control eyes (p values: 0.758, 0.225 and 0.778, respectively). There was a strong positive correlation between TMA and Munk score (r = 0.637, p < 0.001) and moderate positive correlation between TMH (r = 521, p = 0.002), TMD (r = 0.481, p = 0.004) and Munk score.
Conclusion
Tear meniscus measurement with OCT is a rapid, quantitative and objective tool for evaluation of canalicular patency in patients with canalicular laceration repair.


Similar content being viewed by others
References
Han SB, Liu YC, Noriega KM, Mehta JS (2016) Applications of anterior segment optical coherence tomography in cornea and ocular surface diseases. J Ophthalmol 2016:4971572
Ibrahim OMA, Dogru M, Takano Y, Satake Y, Wakamatsu TH, Fukagawa K et al (2010) Application of visante optical coherence tomography tear meniscus height measurement in the diagnosis of dry eye disease. Ophthalmology 117:1923–1929
Zhou S, Li Y, Lu ATH et al (2009) Reproducibility of tear meniscus measurement by Fourier-domain optical coherence tomography: a pilot study. Ophthalmic Surg Laser Imaging 40:442–447
Nguyen P, Huang D, Li Y, Liu P, Tang M, Yiu SC et al (2012) Correlation between optical coherence tomography-derived assessments of lower tear meniscus parameters and clinical features of dry eye disease. Cornea 31:680–685
Akiyama R, Usui T, Yamagami S (2015) Diagnosis of dry eye by tear meniscus measurements using anterior segments swept source optical coherence tomography. Cornea 34:115–120
Qiu X, Gong L, Sun X, Jin H (2011) Age-related variations of human tear meniscus and diagnosis of dry eye with fourier-domain anterior segment optical coherence tomography. Cornea 30:543–549
Johnson ME, Murphy PJ (2005) The agreement and repeatability of tear meniscus height measurement methods. Optom Vis Sci 82:1030–1037
Eroglu FC, Karalezli A, Dursun R (2016) Is optical coherence tomography an effective device for evaluation of tear film meniscus in patients with acne rosacea? Eye 30:545–552
Baek J, Doh SH, Chung SK (2015) Assessment of the tear meniscus using optical coherence tomography in patients with type 2 diabetes mellitus. Cornea 34:1534–1540
Park DI, Lew H, Lee SY (2012) Tear meniscus measurement in nasolacrimal duct obstruction patients with Fourier-domain optical coherence tomography: novel three-point capture method. Acta Ophthalmol 90:783–787
Czajkowski G, Kaluzny BJ, Laudencka A, Malukiewicz G, Kaluzny JJ (2012) Tear meniscus measurement by spectral optical coherence tomography. Optom Vis Sci 89:336–342
García-Resúa C, Santodomingo-Rubido J, Lira M, Giraldez MJ, Vilar EY (2009) Clinical assessment of the lower tear meniscus height. Ophthalmic Physiol Opt 29:487–496
Adhi M, Duker JS (2013) Optical coherence tomography—current and future applications. Curr Opin Ophthalmol 24:213–221
Chen F, Shen M, Chen W, Wang J, Li M, Yuan Y et al (2010) Tear meniscus volume in dry eye after punctual occlusion. Invest Ophthalmol Vis Sci 51:1965–1969
Roh JH, Chi MJ (2010) Efficacy of dye disappearance test and tear meniscus height in diagnosis and postoperative assessment of nasolacrimal duct obstruction. Acta Ophthalmol 88:73–77
Ohtomo K, Ueta T, Fukuda R, Usui T, Miyai T, Shirakawa R et al (2014) Tear meniscus volume changes in dacryocystorhinostomy evaluated with quantitative measurement using anterior segment optical coherence tomography. Invest Ophthalmol Vis Sci 55:2057–2061
Kim SE, Lee SJ, Lee SY, Yoon JS (2012) Outcomes of 4-snip punctoplasty for severe punctal stenosis: measurement of tear meniscus height by optical coherence tomography. Am J Ophthalmol 153:769–773
Munk PL, Lin DT, Morris DC (1990) Epiphora: treatment by means of dacryocystoplasty with balloon dilation of the nasolacrimal drainage apparatus. Radiology 177:687–690
Shen M, Li J, Wang J, Ma H, Cai C, Tao A et al (2009) Upper and lower tear menisci in the diagnosis of dry eye. Invest Ophthalmol Vis Sci 50:2722–2726
Schneider CA, Rasband WS, Eliceiri KW (2012) NIH Image to ImageJ: 25 years of image analysis. Nat Methods 9:671–675
Savini G, Prabhawasat P, Kojima T, Grueterich M, Espana E, Goto E (2008) The challenge of dry eye diagnosis. Clin Ophthalmol 2:31–55
O’Donnell B, Shah R (2001) Dacryocystorhinostomy for epiphora in the presence of a patent lacrimal system. Clin Exp Ophthalmol 29:27–29
At’kova EL, Yartsev VD, Krakhovetskiy NN, Root AO, Reyn DA (2016) Use of optical coherence tomography based lacrimal meniscometry in dacryology. Vestn Ophthalmol 132:101–107
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Karadenız Ugurlu, S., Altın Ekın, M. & Aytogan, H. Assessment of tear meniscus by optical coherence tomography in patients with canalicular laceration repair. Int Ophthalmol 40, 13–18 (2020). https://doi.org/10.1007/s10792-019-01147-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-019-01147-z