Abstract
Background and Aims
Appropriate use of propofol is necessary, and objective monitoring of sedation with propofol may be helpful. Studies on the efficacy of bispectral index (BIS) monitoring in deep sedation have been conducted, but its efficacy in colonoscopy with moderate sedation is unknown. In this study, the efficacy of BIS monitoring during colonoscopy with moderate level sedation via balanced propofol sedation was investigated.
Methods
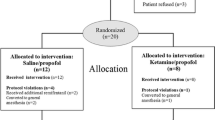
To determine the cut-off value of BIS before the test, an optimal BIS value was determined. Patients who were scheduled to undergo outpatient colonoscopy were prospectively randomized to either a BIS or control group. Finally, a total of 115 patients were selected for this study. The satisfaction level, the complication, and the dosage of the administered propofol were compared.
Results
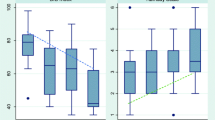
The BIS values and the modified observer’s assessment of alertness/sedation scores (MOAA/S) were positively correlated (r = 0.66 and p < 0.001). The optimal cut-off value of BIS for maintaining moderate sedation was 81, and the area under the ROC curve was 0.88 (95 % CI 0.82–0.93), indicating high prediction accuracy. However, there was no difference between the BIS group and the control group in levels of satisfaction of either patients or endoscopists. In addition, there was no difference in the complication and the required dose of propofol between both groups.
Conclusions
BIS and clinical sedation scores, MOAA/S scores, showed a high level of correlation. However, no significant efficacy was observed in the BIS group who underwent outpatient colonoscopy.



Similar content being viewed by others
References
Vargo JJ, Cohen LB, Rex DK, et al. Position statement: nonanesthesiologist administration of propofol for GI endoscopy. Gastrointest Endosc. 2009;70:1053–1059.
Cohen LB, Hightower CD, Wood DA, et al. Moderate level sedation during endoscopy: a prospective study using low-dose propofol, meperidine/fentanyl, and midazolam. Gastrointest Endosc. 2004;59:795–803.
Sipe BW, Scheidler M, Baluyut A, et al. A prospective safety study of a low-dose propofol sedation protocol for colonoscopy. Clin Gastroenterol Hepatol. 2007;5:563–566.
Cohen LB, Dubovsky AN, Aisenberg J, et al. Propofol for endoscopic sedation: A protocol for safe and effective administration by the gastroenterologist. Gastrointest Endosc. 2003;58:725–732.
VanNatta ME, Rex DK. Propofol alone titrated to deep sedation versus propofol in combination with opioids and/or benzodiazepines and titrated to moderate sedation for colonoscopy. Am J Gastroenterol. 2006;101:2209–2217.
Wehrmann T, Riphaus A. Sedation with propofol for interventional endoscopic procedures: a risk factor analysis. Scand J Gastroenterol. 2008;43:368–374.
Johansen JW. Update on bispectral index monitoring. Best Pract Res Clin Anaesthesiol. 2006;20:81–99.
Paspatis GA, Chainaki I, Manolaraki MM, et al. Efficacy of bispectral index monitoring as an adjunct to propofol deep sedation for ERCP: a randomized controlled trial. Endoscopy. 2009;41:1046–1051.
Imagawa A, Fujiki S, Kawahara Y, et al. Satisfaction with bispectral index monitoring of propofol-mediated sedation during endoscopic submucosal dissection: a prospective, randomized study. Endoscopy. 2008;40:905–909.
Chen SC, Rex DK. An initial investigation of bispectral monitoring as an adjunct to nurse-administered propofol sedation for colonoscopy. Am J Gastroenterol. 2004;99:1081–1086.
Drake LM, Chen SC, Rex DK. Efficacy of bispectral monitoring as an adjunct to nurse-administered propofol sedation for colonoscopy: a randomized controlled trial. Am J Gastroenterol. 2006;101:2003–2007.
Billard V, Gambus PL, Chamoun N, et al. A comparison of spectral edge, delta power, and bispectral index as EEG measures of alfentanil, propofol, and midazolam drug effect. Clin Pharmacol Ther. 1997;61:45–58.
Bower AL, Ripepi A, Dilger J, et al. Bispectral index monitoring of sedation during endoscopy. Gastrointest Endosc. 2000;52:192–196.
Glass PS, Bloom M, Kearse L, et al. Bispectral analysis measures sedation and memory effects of propofol, midazolam, isoflurane, and alfentanil in healthy volunteers. Anesthesiology. 1997;86:836–847.
Cohen LB, Delegge MH, Aisenberg J, et al. AGA Institute review of endoscopic sedation. Gastroenterology. 2007;133:675–701.
American Society of Anesthesiologists Task Force on Sedation and Analgesia by Non-Anesthesiologists. Practice guidelines for sedation and analgesia by non-anesthesiologists. Anesthesiology. 2002;96:1004–1017.
Aldrete JA. Modifications to the postanesthesia score for use in ambulatory surgery. J Perianesth Nurs. 1998;13:148–155.
Sigl JC, Chamoun NG. An introduction to bispectral analysis for the electroencephalogram. J Clin Monit. 1994;10:392–404.
Kearse LA Jr, Rosow C, Zaslavsky A, et al. Bispectral analysis of the electroencephalogram predicts conscious processing of information during propofol sedation and hypnosis. Anesthesiology. 1998;88:25–34.
von Delius S, Thies P, Rieder T, et al. Auditory evoked potentials compared with bispectral index for monitoring of midazolam and propofol sedation during colonoscopy. Am J Gastroenterol. 2009;104:318–325.
Cohen LB, Wecsler JS, Gaetano JN, et al. Endoscopic sedation in the United States: results from a nationwide survey. Am J Gastroenterol. 2006;101:967–974.
Benson AA, Cohen LB, Waye JD, et al. Endoscopic sedation in developing and developed countries. Gut Liver. 2008;2:105–112.
Riphaus A, Rabofski M, Wehrmann T. Endoscopic sedation and monitoring practice in Germany: results from the first nationwide survey. Z Gastroenterol. 2010;48:392–397.
Acknowledgment
This work was supported by the research fund of the Hanyang University Institute of Aging, Society in 2011.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yu, Y.H., Han, D.S., Kim, H.S. et al. Efficacy of Bispectral Index Monitoring During Balanced Propofol Sedation for Colonoscopy: A Prospective, Randomized Controlled Trial. Dig Dis Sci 58, 3576–3583 (2013). https://doi.org/10.1007/s10620-013-2833-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-013-2833-4