Abstract
Purpose
The prevalence of patients living with prolonged interval between initial breast cancer diagnosis and development of subsequent metastatic disease may be increasing with improved treatment. In order to counsel these patients as to their prognosis, we investigated the association between metastatic free interval (MFI) and subsequent survival from newly diagnosed metastatic breast cancer (MBC) in a population-level U.S. cohort.
Methods
The Surveillance, Epidemiology and End Results database was used to identify patients with both an initial stage 1–3 breast cancer diagnosis and subsequent MBC diagnosis recorded from 1988 to 2014. Patients were stratified by MFI (< 5 years, 5–10 years, > 10 years). The association between MFI and metastatic breast cancer-specific mortality (MBCSM) was analyzed with Fine–Gray competing risks regression.
Results
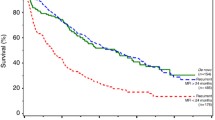
Five-year recurrent metastatic breast cancer-specific survival rate was 23%, 26%, and 35% for patients with MFI < 5, 5–10, and > 10 years, respectively. Patients with > 10 year MFI were less likely to die of breast cancer when compared with a referent group with < 5 years MFI (standard hazard ratio (SHR) 0.77 [95% CI 0.65–0.90] P < 0.001). There was no significant difference for patients with MFI of 5–10 years (SHR 0.92 [95% CI 0.81–1.04, P 0.191]) compared to < 5 years. Other prognostic factors like White race, lower tumor grade, and ER/PR-positive receptors were also associated with improved cancer-specific survival after diagnosis of MBC.
Conclusion
Prolonged MFI greater than 10 years between initial breast cancer diagnosis and subsequent metastatic disease was found to be associated with improved recurrent MBC 5-year survival and decreased risk of breast cancer-specific mortality. This has potential implications for counseling patients as to prognosis, choice of treatment, as well as the stratification of patients considered for MBC clinical trials.



Similar content being viewed by others
References
SEER Cancer stat facts: female breast cancer [https://seer.cancer.gov/statfacts/html/breast.html]. Accessed Mar 2017
Mariotto AB, Etzioni R, Hurlbert M, Penberthy L, Mayer M (2017) Estimation of the Number of Women Living with Metastatic Breast Cancer in the United States. Cancer Epidemiol Biomarkers Prev 26(6):809–815
Nakano M, Fujisue M, Tashima R, Okumura Y, Nishiyama Y, Ohsako T, Toyozumi Y, Arima N, Nishimura R (2015) Survival time according to the year of recurrence and subtype in recurrent breast cancer. Breast 24(5):588–593
Lobbezoo DJ, van Kampen RJ, Voogd AC, Dercksen MW, van den Berkmortel F, Smilde TJ, van de Wouw AJ, Peters FP, van Riel JM, Peters NA et al (2015) Prognosis of metastatic breast cancer: are there differences between patients with de novo and recurrent metastatic breast cancer? Br J Cancer 112(9):1445–1451
Regierer AC, Wolters R, Ufen MP, Weigel A, Novopashenny I, Kohne CH, Samonigg H, Eucker J, Possinger K, Wischnewsky MB (2014) An internally and externally validated prognostic score for metastatic breast cancer: analysis of 2269 patients. Ann Oncol 25(3):633–638
Largillier R, Ferrero JM, Doyen J, Barriere J, Namer M, Mari V, Courdi A, Hannoun-Levi JM, Ettore F, Birtwisle-Peyrottes I et al (2008) Prognostic factors in 1,038 women with metastatic breast cancer. Ann Oncol 19(12):2012–2019
Puente J, Lopez-Tarruella S, Ruiz A, Lluch A, Pastor M, Alba E, de la Haba J, Ramos M, Cirera L, Anton A et al (2010) Practical prognostic index for patients with metastatic recurrent breast cancer: retrospective analysis of 2,322 patients from the GEICAM Spanish El Alamo Register. Breast Cancer Res Treat 122(2):591–600
Dawood S, Broglio K, Ensor J, Hortobagyi GN, Giordano SH (2010) Survival differences among women with de novo stage IV and relapsed breast cancer. Ann Oncol 21(11):2169–2174
Tevaarwerk AJ, Gray RJ, Schneider BP, Smith ML, Wagner LI, Fetting JH, Davidson N, Goldstein LJ, Miller KD, Sparano JA (2013) Survival in patients with metastatic recurrent breast cancer after adjuvant chemotherapy: little evidence of improvement over the past 30 years. Cancer 119(6):1140–1148
Surveillance E, Results E (SEER) (2016) Program (http://www.seer.cancer.gov): Research Data (1973–2014), National Cancer Institute, DCCPS, Surveillance Research Program, released April 2017, based on the November submission
Number of Persons by Race and Hispanic Ethnicity for SEER Participants (2010 Census Data) https://seer.cancer.gov/registries/data.html. Accessed Mar 2017
Healthcare Delivery Research Program: Measures that are limited or not available in the data [https://healthcaredelivery.cancer.gov/seermedicare/considerations/measures.html]. Accessed May 2017
Fine JP, Gray RJ (1999) A proportional hazards model for the subdistribution of a competing risk. J Am Stat Assoc 94(446):496–509
Harper S, Lynch J, Meersman SC, Breen N, Davis WW, Reichman MC (2009) Trends in area-socioeconomic and race-ethnic disparities in breast cancer incidence, stage at diagnosis, screening, mortality, and survival among women ages 50 years and over (1987–2005). Cancer Epidemiol Biomarkers Prev 18(1):121–131
Ooi SL, Martinez ME, Li CI (2011) Disparities in breast cancer characteristics and outcomes by race/ethnicity. Breast Cancer Res Treat 127(3):729–738
Curtis E, Quale C, Haggstrom D, Smith-Bindman R (2008) Racial and ethnic differences in breast cancer survival: how much is explained by screening, tumor severity, biology, treatment, comorbidities, and demographics? Cancer 112(1):171–180
Dunnwald LK, Rossing MA, Li CI (2007) Hormone receptor status, tumor characteristics, and prognosis: a prospective cohort of breast cancer patients. Breast Cancer Res 9(1):R6
Dent R, Trudeau M, Pritchard KI, Hanna WM, Kahn HK, Sawka CA, Lickley LA, Rawlinson E, Sun P, Narod SA (2007) Triple-negative breast cancer: clinical features and patterns of recurrence. Clin Cancer Res 13(15 Pt 1):4429–4434
Lin NU, Vanderplas A, Hughes ME, Theriault RL, Edge SB, Wong YN, Blayney DW, Niland JC, Winer EP, Weeks JC (2012) Clinicopathologic features, patterns of recurrence, and survival among women with triple-negative breast cancer in the National Comprehensive Cancer Network. Cancer 118(22):5463–5472
Gorin SS, Heck JE, Cheng B, Smith SJ (2006) Delays in breast cancer diagnosis and treatment by racial/ethnic group. Arch Intern Med 166(20):2244–2252
Chia SK, Speers CH, D’Yachkova Y, Kang A, Malfair-Taylor S, Barnett J, Coldman A, Gelmon KA, O’Reilly SE, Olivotto IA (2007) The impact of new chemotherapeutic and hormone agents on survival in a population-based cohort of women with metastatic breast cancer. Cancer 110(5):973–979
Warren JL, Mariotto A, Melbert D, Schrag D, Doria-Rose P, Penson D, Yabroff KR (2016) Sensitivity of medicare claims to identify cancer recurrence in elderly colorectal and breast cancer patients. Med Care 54(8):e47–e54
Kennecke H, Yerushalmi R, Woods R, Cheang MC, Voduc D, Speers CH, Nielsen TO, Gelmon K (2010) Metastatic behavior of breast cancer subtypes. J Clin Oncol 28(20):3271–3277
Lobbezoo DJ, van Kampen RJ, Voogd AC, Dercksen MW, van den Berkmortel F, Smilde TJ, van de Wouw AJ, Peters FP, van Riel JM, Peters NA et al (2013) Prognosis of metastatic breast cancer subtypes: the hormone receptor/HER2-positive subtype is associated with the most favorable outcome. Breast Cancer Res Treat 141(3):507–514
SEER Registry Groupings for Analyses [https://seer.cancer.gov/registries/terms.html]. Accessed Dec 2017
Funding
Enoch Chang was supported by the NIDDK of the NIH under Award Number T35DK104689. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
Enoch Chang: Conceptualization, data curation, formal statistical analysis and interpretation of data, funding acquisition, investigation, methodology, software, validation, visualization, writing—original draft, and writing—review and editing. Sarah S. Mougalian: Analysis and interpretation of data, writing—review and editing. Kerin B. Adelson: Analysis and interpretation of data, writing—review and editing. Melissa R. Young: Analysis and interpretation of data, writing—review and editing. James B. Yu: Conceptualization, data curation, formal statistical analysis and interpretation of data, investigation, methodology, project administration, resources, software, supervision, validation, visualization, writing—original draft, and writing—review and editing.
Corresponding author
Ethics declarations
Conflict of interest
Sarah S. Mougalian MD: Consulting role with Eisai. Stocks: Gilead, Coronado Biosciences, Roche. Research funding from Genentech, Pfizer; Kerin B. Adelson MD: Immediate family member is employed with Lyra Health; Consulting role with Wellpoint; Travel, Accommodations, Expenses from Genentech; Honoraria from Genentech; James B. Yu MD, MHS: Consulting role with Augmenix. Research funding from twenty-first Century Oncology.
Rights and permissions
About this article
Cite this article
Chang, E., Mougalian, S.S., Adelson, K.B. et al. Association between prolonged metastatic free interval and recurrent metastatic breast cancer survival: findings from the SEER database. Breast Cancer Res Treat 173, 209–216 (2019). https://doi.org/10.1007/s10549-018-4968-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-018-4968-7