Abstract
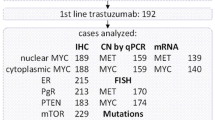
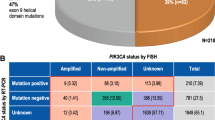
Trastuzumab (T) is effective in metastatic breast cancer (MBC) with HER2 overexpression and/or amplification, but resistance to T develops in a significant number of HER2-positive patients. Understanding the mechanisms of resistance is critical to the care of these patients. Formalin-fixed paraffin-embedded tumor tissue samples were collected from 256 patients with T-treated MBC. Clinical information was collected retrospectively from the patients’ medical records. Central review of HER2 status by fluorescent in situ hybridization (FISH) and/or immunohistochemistry (IHC) revealed that of the 227 eligible patients only 139 (61%) were truly HER2-positive. PTEN, ER, PgR, and Ki67 were evaluated by IHC, while PTEN status was evaluated by FISH as well. PIK3CA mutations were identified with single nucleotide polymorphism (SNP) genotyping. Median time to progression (TTP) was 14.4 months for the HER2-positive and 10.3 for the HER2-negative patients (log-rank, P = 0.22). Survival from the initiation of T (survivalT) was 50.4 months for the HER2-positive and 35.3 for the HER2-negative subgroups (P = 0.006). Higher risk of progression was associated with HER2-positive status and the presence of PIK3CA mutations (P = 0.014). PTEN loss, as determined by IHC, was associated with lower survivalT in the whole population (P = 0.029) and in the HER2-positive population (P = 0.017). PIK3CA mutations and/or PTEN loss status were evaluated together as a single parameter, to estimate the impact of activation of the PI3K/AKT molecular pathway, and it was significantly associated with both decreased TTP (P = 0.003 in the total population, P = 0.004 in HER2-positive patients) and survival (survivalT, P = 0.011 in total, P = 0.006 in HER2-positive). In this trastuzumab-treated breast cancer population, PIK3CA activating mutations were associated with shorter TTP and PTEN loss with decreased survival. The activation of the PI3K/AKT pathway from either defect was associated with both TTP and survival, indicating the adverse effect of this pathway’s status on trastuzumab efficacy.



Similar content being viewed by others
References
Slamon DJ, Clark GM, Wong SG, Levin WJ, Ullrich A, McGuire WL (1987) Human breast cancer: correlation of relapse and survival with amplification of the HER-2/neu oncogene. Science 235(4785):177–182
Slamon DJ, Leyland-Jones B, Shak S, Fuchs H, Paton V, Bajamonde A, Fleming T, Eiermann W, Wolter J, Pegram M, Baselga J, Norton L (2001) Use of chemotherapy plus a monoclonal antibody against HER2 for metastatic breast cancer that overexpresses HER2. N Engl J Med 344(11):783–792. doi:10.1056/NEJM200103153441101
Vogel CL, Cobleigh MA, Tripathy D, Gutheil JC, Harris LN, Fehrenbacher L, Slamon DJ, Murphy M, Novotny WF, Burchmore M, Shak S, Stewart SJ, Press M (2002) Efficacy and safety of trastuzumab as a single agent in first-line treatment of HER2-overexpressing metastatic breast cancer. J Clin Oncol 20(3):719–726
Marty M, Cognetti F, Maraninchi D, Snyder R, Mauriac L, Tubiana-Hulin M, Chan S, Grimes D, Anton A, Lluch A, Kennedy J, O’Byrne K, Conte P, Green M, Ward C, Mayne K, Extra JM (2005) Randomized phase II trial of the efficacy and safety of trastuzumab combined with docetaxel in patients with human epidermal growth factor receptor 2-positive metastatic breast cancer administered as first-line treatment: the M77001 study group. J Clin Oncol 23(19):4265–4274. doi:10.1200/JCO.2005.04.173
Nahta R, Yu D, Hung MC, Hortobagyi GN, Esteva FJ (2006) Mechanisms of disease: understanding resistance to HER2-targeted therapy in human breast cancer. Nat Clin Pract Oncol 3(5):269–280. doi:10.1038/ncponc0509
Berns K, Horlings HM, Hennessy BT, Madiredjo M, Hijmans EM, Beelen K, Linn SC, Gonzalez-Angulo AM, Stemke-Hale K, Hauptmann M, Beijersbergen RL, Mills GB, van de Vijver MJ, Bernards R (2007) A functional genetic approach identifies the PI3K pathway as a major determinant of trastuzumab resistance in breast cancer. Cancer Cell 12(4):395–402. doi:10.1016/j.ccr.2007.08.030
Nagata Y, Lan KH, Zhou X, Tan M, Esteva FJ, Sahin AA, Klos KS, Li P, Monia BP, Nguyen NT, Hortobagyi GN, Hung MC, Yu D (2004) PTEN activation contributes to tumor inhibition by trastuzumab, and loss of PTEN predicts trastuzumab resistance in patients. Cancer Cell 6(2):117–127. doi:10.1016/j.ccr.2004.06.022
Fujita T, Doihara H, Kawasaki K, Takabatake D, Takahashi H, Washio K, Tsukuda K, Ogasawara Y, Shimizu N (2006) PTEN activity could be a predictive marker of trastuzumab efficacy in the treatment of ErbB2-overexpressing breast cancer. Br J Cancer 94(2):247–252. doi:10.1038/sj.bjc.6602926
Fabi A, Metro G, Di Benedetto A, Nistico C, Vici P, Melucci E, Antoniani B, Perracchio L, Sperduti I, Milella M, Cognetti F, Mottolese M (2010) Clinical significance of PTEN and p-Akt co-expression in HER2-positive metastatic breast cancer patients treated with trastuzumab-based therapies. Oncology 78(2):141–149. doi:10.1159/000312656
Gori S, Sidoni A, Colozza M, Ferri I, Mameli MG, Fenocchio D, Stocchi L, Foglietta J, Ludovini V, Minenza E, De Angelis V, Crino L (2009) EGFR, pMAPK, pAkt and PTEN status by immunohistochemistry: correlation with clinical outcome in HER2-positive metastatic breast cancer patients treated with trastuzumab. Ann Oncol 20(4):648–654. doi:10.1093/annonc/mdn681
Pandolfi PP (2004) Breast cancer—loss of PTEN predicts resistance to treatment. N Engl J Med 351(22):2337–2338. doi:10.1056/NEJMcibr043143
Saal LH, Holm K, Maurer M, Memeo L, Su T, Wang X, Yu JS, Malmstrom PO, Mansukhani M, Enoksson J, Hibshoosh H, Borg A, Parsons R (2005) PIK3CA mutations correlate with hormone receptors, node metastasis, and ERBB2, and are mutually exclusive with PTEN loss in human breast carcinoma. Cancer Res 65(7):2554–2559. doi:10.1158/0008-5472-CAN-04-3913
McShane LM, Altman DG, Sauerbrei W, Taube SE, Gion M, Clark GM (2006) REporting recommendations for tumor MARKer prognostic studies (REMARK). Breast Cancer Res Treat 100(2):229–235. doi:10.1007/s10549-006-9242-8
Fountzilas G, Bobos M, Kalogera-Fountzila A, Xiros N, Murray S, Linardou H, Karayannopoulou G, Koutras AK, Bafaloukos D, Samantas E, Christodoulou C, Economopoulos T, Kalogeras KT, Kosmidis P (2008) Gemcitabine combined with gefitinib in patients with inoperable or metastatic pancreatic cancer: a phase II Study of the Hellenic Cooperative Oncology Group with biomarker evaluation. Cancer Invest 26(8):784–793. doi:10.1080/07357900801918611
Gogas H, Pectasides D, Kostopoulos I, Lianos E, Skarlos D, Papaxoinis G, Bobos M, Kalofonos HP, Petraki K, Pavlakis K, Bafaloukos D, Fountzilas G (2010) Paclitaxel and carboplatin as neoadjuvant chemotherapy in patients with locally advanced breast cancer: a phase II Trial of the Hellenic Cooperative Oncology Group. Clin Breast Cancer 10(3):230–237. doi:10.3816/CBC.2010.n.031
Bamias A, Karina M, Papakostas P, Kostopoulos I, Bobos M, Vourli G, Samantas E, Christodoulou C, Pentheroudakis G, Pectasides D, Dimopoulos MA, Fountzilas G (2010) A randomized phase III study of adjuvant platinum/docetaxel chemotherapy with or without radiation therapy in patients with gastric cancer. Cancer Chemother Pharmacol 65(6):1009–1021. doi:10.1007/s00280-010-1256-6
Hugh J, Hanson J, Cheang MC, Nielsen TO, Perou CM, Dumontet C, Reed J, Krajewska M, Treilleux I, Rupin M, Magherini E, Mackey J, Martin M, Vogel C (2009) Breast cancer subtypes and response to docetaxel in node-positive breast cancer: use of an immunohistochemical definition in the BCIRG 001 trial. J Clin Oncol 27(8):1168–1176. doi:10.1200/JCO.2008.18.1024
Wolff AC, Hammond ME, Schwartz JN, Hagerty KL, Allred DC, Cote RJ, Dowsett M, Fitzgibbons PL, Hanna WM, Langer A, McShane LM, Paik S, Pegram MD, Perez EA, Press MF, Rhodes A, Sturgeon C, Taube SE, Tubbs R, Vance GH, van de Vijver M, Wheeler TM, Hayes DF (2007) American Society of Clinical Oncology/College of American Pathologists guideline recommendations for human epidermal growth factor receptor 2 testing in breast cancer. J Clin Oncol 25(1):118–145. doi:10.1200/JCO.2006.09.2775
Cheang MC, Chia SK, Voduc D, Gao D, Leung S, Snider J, Watson M, Davies S, Bernard PS, Parker JS, Perou CM, Ellis MJ, Nielsen TO (2009) Ki67 index, HER2 status, and prognosis of patients with luminal B breast cancer. J Natl Cancer Inst 101(10):736–750. doi:10.1093/jnci/djp082
Christodoulou C, Kostopoulos I, Kalofonos HP, Lianos E, Bobos M, Briasoulis E, Gogas H, Razis E, Skarlos DV, Fountzilas G (2009) Trastuzumab combined with pegylated liposomal doxorubicin in patients with metastatic breast cancer: phase II Study of the Hellenic Cooperative Oncology Group (HeCOG) with biomarker evaluation. Oncology 76(4):275–285. doi:10.1159/000207504
Bohmann K, Hennig G, Rogel U, Poremba C, Mueller BM, Fritz P, Stoerkel S, Schaefer KL (2009) RNA extraction from archival formalin-fixed paraffin-embedded tissue: a comparison of manual, semiautomated, and fully automated purification methods. Clin Chem 55(9):1719–1727. doi:10.1373/clinchem.2008.122572
Perez-Tenorio G, Alkhori L, Olsson B, Waltersson MA, Nordenskjold B, Rutqvist LE, Skoog L, Stal O (2007) PIK3CA mutations and PTEN loss correlate with similar prognostic factors and are not mutually exclusive in breast cancer. Clin Cancer Res 13(12):3577–3584. doi:10.1158/1078-0432.CCR-06-1609
Pohlmann PR, Mayer IA, Mernaugh R (2009) Resistance to trastuzumab in breast cancer. Clin Cancer Res 15(24):7479–7491. doi:10.1158/1078-0432.CCR-09-0636
Kakarala M, Wicha MS (2008) Implications of the cancer stem-cell hypothesis for breast cancer prevention and therapy. J Clin Oncol 26(17):2813–2820. doi:10.1200/JCO.2008.16.3931
Acknowledgments
We would like to thank Ms. Thalia Spinari for tissue collection, Ms. Dimitra Katsala for monitoring the study, Ms. Maria Moschoni for coordinating the data management, and Ms. Stella Dallidou for secretarial assistance. The study was supported by a Hellenic Cooperative Oncology Group grant HER_11P/05.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Razis, E., Bobos, M., Kotoula, V. et al. Evaluation of the association of PIK3CA mutations and PTEN loss with efficacy of trastuzumab therapy in metastatic breast cancer. Breast Cancer Res Treat 128, 447–456 (2011). https://doi.org/10.1007/s10549-011-1572-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-011-1572-5