Abstract
Background
Prucalopride is a selective serotonin receptor agonist with prokinetic activity, indicated for women with chronic constipation in whom laxatives have failed to provide adequate relief. Data suggests an improvement in about 50 % of such patients but whether the therapeutic effect is on patients with slow transit constipation (STC) and/or obstructed defaecation syndrome (ODS), or even those with constipation-predominant irritable bowel syndrome (IBS-C) is unknown. We therefore assessed whether there is any association between prucalopride efficacy and constipation type.
Methods
All patients receiving prucalopride between June 2010 and April 2012 at our institution were identified, and data analysed following a 4-week “test” period. Patients were sub-grouped as those suffering with ODS, STC, mixed (ODS and STC) or IBS-C based on symptomatology and investigations. Subjective assessment of patient satisfaction and continuation of medication were taken as positive outcomes and analysed for each sub-type along with any side effects.
Results
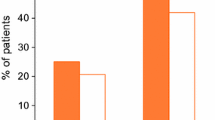
Sixty-nine patients met our criteria. Data were available for 59 women (median age 46 years, range 17–79 years). Sixty-five per cent of prescriptions came from colorectal surgeons. Overall, 25 out of 59 (42 %) patients improved, according to our criteria, after the 4-week trial period. Seventeen patients (29 %) had ODS, 26 (44 %) had STC, 7 (12 %) had mixed symptoms and 9 (15 %) had IBS-C. At 4 weeks, 10 out of 17 patients (59 %) with ODS had improved compared with 4 out of 9 patients (44 %) with IBS-C, 3 out of 7 patients (43 %) with mixed symptoms and 8 out of 26 (31 %) patients with STC. The underlying disorder did not predict whether or not a patient responded to the 4-week trial period (p = 0.32). Nine patients (15 %) experienced side effects that precluded further use.
Conclusions
Patients with all categories of constipation may respond to prucalopride. A trial regime may be indicated regardless of the aetiology of the constipation.
Similar content being viewed by others
References
Higgins PD, Johanson JF (2004) Epidemiology of constipation in North America: a systematic review. Am J Gastroenterol 99:750–759
Peppas G, Alexiou VG, Mourtzoukou E, Falagas ME (2008) Epidemiology of constipation in Europe and Oceania: a systematic review. BMC Gastroenterol 8:5
Glia A, Lindberg G (1997) Quality of life in patients with different types of functional constipation. Scand J Gastroenterol 32:1083–1089
Irvine EJ, Ferazzi S, Pare P, Thompson WG, Rance L (2002) Health-related quality of life in functional GI disorders: focus on constipation and resource utilization. Am J Gastroenterol 97:1986–1993
Tack J, Dubois D, Schenk F (2009) Only 27% of patients with chronic constipation are satisfied with current treatment options. Gut 58(Suppl. II):181
Longstreth GF, Thompson WG, Chey WD, Houghton LA, Mearin F, Spiller RC (2006) Functional bowel disorders. Gastroenterology 130:1480–1491
Bharucha AE, Wald A, Enck P, Rao S (2006) Functional anorectal disorders. Gastroenterology 130:1510–1518
Drossman DA, Camilleri M, Mayer EA, Whitehead WE (2002) AGA technical review on irritable bowel syndrome. Gastroenterology 123:2108–2131
De Schryver AM, Andriesse GI, Samsom M, Smout AJ, Gooszen HG, Akkermans LM (2002) The effects of the specific 5HT(4) receptor agonist, prucalopride, on colonic motility in healthy volunteers. Aliment Pharmacol Ther 16:603–612
National Institute for Health and Clinical Excellence. TA211 Constipation (women)—prucalopride: guidance. 15 Dec 2010
Camilleri M, Kerstens R, Rykx A, Vandeplassche L (2008) A placebo-controlled trial of prucalopride for severe chronic constipation. N Engl J Med 358:2344–2354
Quigley EM, Vandeplassche L, Kerstens R, Ausma J (2009) Clinical trial: the efficacy, impact on quality of life, and safety and tolerability of prucalopride in severe chronic constipation – a 12-week, randomized, double-blind, placebo- controlled study. Aliment Pharmacol Ther 29:315–328
Tack J, van Outryve M, Beyens G, Kerstens R, Vandeplassche L (2009) Prucalopride (Resolor) in the treatment of severe chronic constipation in patients dissatisfied with laxatives. Gut 58:357–365
Attaluri A, Rao S (2006) Diagnostic and therapeutic approaches to patients with constipation. Practical Gastroenterol 30:30–47
Chey WD, Pare P, Viegas A, Ligozio G, Shetzline MA (2008) Tegaserod for female patients suffering from IBS with mixed bowel habits or constipation: a randomized controlled trial. Am J Gastroenterol 103:1217–1225
Layer P, Keller J, Loeffler H, Kreiss A (2007) Tegaserod in the treatment of irritable bowel syndrome (IBS) with constipation as the prime symptom. Ther Clin Risk Manag 3:107–118
Evans BW, Clark WK, Moore DJ, Whorwell PJ (2007) Tegaserod for the treatment of irritable bowel syndrome and chronic constipation. Cochrane Database Syst Rev CD003960
Novick J, Miner P, Krause R et al (2002) A randomized, double-blind, placebo-controlled trial of tegaserod in female patients suffering from irritable bowel syndrome with constipation. Aliment Pharmacol Ther 16:1877–1888
US FDA public health advisory tegaserod maleate (marketed Zelnorm™). http://www.fda.gov/CDER/DRUG/advisory/tegaserod.htm. (Accessed July 2008)
Bannister JJ, Davidson P, Timms JM, Gibbons C, Read NW (1987) Effect of stool size and consistency on defaecation. Gut 28:1242–1245
Bassotti G, Villanacci V, Nascimbeni R et al (2012) Increase of colonic mast cells in obstructed defaecation and their relationship with enteric glia. Dig Dis Sci 57:65–71
Bassotti G, Villanacci V, Bellomi A et al (2012) An assessment of enteric nervous system and estroprogestinic receptors in obstructed defecation associated with rectal intussusception. Neurogastroenterol Mot 24:155–161
Bassotti G, Villanacci V, Nascimbeni R et al (2007) Colonic neuropathological aspects in patients with intractable constipation due to obstructed defecation. Mod Pathol 20:367–374
D’Hoore A, Penninckx F (2006) Laparoscopic ventral recto(colpo)pexy for rectal prolapse: surgical technique and outcome for 109 patients. Surg Endosc 20:1919–1923
Slawik S, Soulsby R, Carter H, Payne H, Dixon AR (2008) Laparoscopic ventral rectopexy, posterior colporrhaphy and vaginal sacrocolpopexy for the treatment of recto-genital prolapse and mechanical outlet obstruction. Colorectal Dis 10:138–143
Collinson R, Wijffels N, Cunningham C, Lindsey I (2010) Laparoscopic ventral rectopexy for internal rectal prolapse: short-term functional results. Colorectal Dis 12:97–104
Lehur PA, Stuto A, Fantoli M et al (2008) ODS II Study Group. Outcomes of stapled transanal rectal resection versus biofeedback for the treatment of outlet obstruction associated with rectal intussusception and rectocele: a multicenter, randomized, controlled trial. Dis Colon Rectum 51:1739
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jadav, A.M., Mcmullin, C.M., Smith, J. et al. The association between prucalopride efficacy and constipation type. Tech Coloproctol 17, 555–559 (2013). https://doi.org/10.1007/s10151-013-1017-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-013-1017-8