Abstract
Background
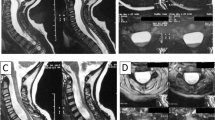
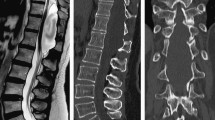
Idiopathic spinal epidural arachnoid cysts (SEACs) are relatively rare lesions with diverse clinical manifestations depending on the affected spinal region and nerve roots. To assess the relationship between clinical presentation and surgical outcome, we conducted a retrospective review of medical records and neuroimages from idiopathic SEAC patients.
Methods
Of 15 consecutive patients with idiopathic SEACs, 14 underwent surgical treatment at the Beijing Tiantan Hospital between January 2008 and July 2013. Case histories, clinical presentations, imaging findings, operative findings, and surgical outcomes were reviewed.
Results
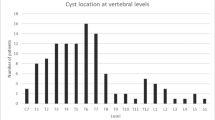
Of the 15 patients, 5 were children (median age, 13 years) and 10 were adults (median age, 35 years). The male-to-female ratio was 4:1. The median disease duration was 1 year in children and 4 years in adults. The most common manifestations were progressive paraparesis (73.3 %) and radiculopathy (66.7 %). All pediatric lesions affected thoracic segments, while 80 % of adult lesions affected lumbar segments. Fourteen patients underwent microsurgical treatment, with cyst excision in nine (combined with fistula closure in four) and partial cyst excision in five (with fistula closure in three). No recurrences were observed during follow-up (average of 23 months). Excellent outcome was achieved in six cases, good outcome in four, fair in two, and poor in two.
Conclusions
Idiopathic SEAC mainly affect the thoracic segments in children and the lumbar segments in adults, and often results in progressive paraparesis and radiculopathy. Early surgical intervention is suggested for progressive symptomatic patients to restore neurological function.


Similar content being viewed by others
References
Agnoli AL, Schonmayr R, Laun A (1982) Intraspinal arachnoid cysts. Acta Neurochir (Wien) 61:291–302
Bartels RH, van Overbeeke JJ (1997) Lumbar cerebrospinal fluid drainage for symptomatic sacral nerve root cysts: an adjuvant diagnostic procedure and/or alternative treatment? Technical case report. Neurosurgery 40:861–864, discussion 864–865
Bayar MA, Yidiz B, Buharali Z (1991) Management problems in cases with a combination of asymptomatic occult intrasacral meningocele and disc prolapse. Acta Neurochir (Wien) 108:67–69
Bellavia R, King JT Jr, Naheedy MH, Lewin JS (2000) Percutaneous aspiration of an intradural/extradural thoracic arachnoid cyst: use of MR imaging guidance. J Vasc Interv Radiol 11:369–372
Bergland RM (1968) Congenital intraspinal extradural cyst. Report of three cases in one family. J Neurosurg 28:495–499
Catala M, Poirier J (1998) Arachnoid cysts: histologic, embryologic and physiopathologic review. Rev Neurol (Paris) 154:489–501
Choi JY, Kim SH, Lee WS, Sung KH (2006) Spinal extradural arachnoid cyst. Acta Neurochir (Wien) 148:579–585, discussion 585
Chynn KY (1967) Congenital spinal extradural cyst in two siblings. Am J Roentgenol Radium Ther Nucl Med 101:204–215
Congia S, Coraddu M, Tronci S, Nurchi G, Fiaschi A (1992) Myelographic and MRI appearances of a thoracic spinal extradural arachnoid cyst of the spine with extra- and intraspinal extension. Neuroradiology 34:444–446
Di Lorenzo N, Fortuna A, Guidetti B (1982) Craniovertebral junction malformations. Clinicoradiological findings, long-term results, and surgical indications in 63 cases. J Neurosurg 57:603–608
Doi H, Toyoda I, Kuwasawa J, Koba S, Matsumoto K (1995) Posterolateral extradural approach for total excision of spinal meningeal cyst (type Ia): case report. No Shinkei Geka 23:339–342
Ergun E, Borcek AO, Cemil B, Dogulu F, Baykaner MK (2008) Should we operate all extradural spinal arachnoid cysts? Report of a case. Turk Neurosurg 18:52–55
Ergun T, Lakadamyali H (2009) Multiple extradural spinal arachnoid cysts causing diffuse myelomalacia of the spinal cord. Neurologist 15:347–350
Funao H, Nakamura M, Hosogane N, Watanabe K, Tsuji T, Ishii K, Kamata M, Toyama Y, Chiba K, Matsumoto M (2012) Surgical treatment of spinal extradural arachnoid cysts in the thoracolumbar spine. Neurosurgery 71:278–284, discussion 284
Gortvai P (1963) Extradural cysts of the spinal canal. J Neurol Neurosurg Psychiatry 26:223–230
Hatashita S, Kondo A, Shimizu T, Kurosu A, Ueno H (2001) Spinal extradural arachnoid cyst—case report. Neurol Med Chir (Tokyo) 41:318–321
Kendall BE, Valentine AR, Keis B (1982) Spinal arachnoid cysts: clinical and radiological correlation with prognosis. Neuroradiology 22:225–234
Kim KS, Weinberg PE (1986) Magnetic resonance imaging of a spinal extradural arachnoid cyst. Surg Neurol 26:249–252
Krings T, Lukas R, Reul J, Spetzger U, Reinges MH, Gilsbach JM, Thron A (2001) Diagnostic and therapeutic management of spinal arachnoid cysts. Acta Neurochir (Wien) 143:227–234, discussion 234–225
Kunz U, Mauer UM, Waldbaur H (1999) Lumbosacral extradural arachnoid cysts: diagnostic and indication for surgery. Eur Spine J 8:218–222
Lake PA, Minckler J, Scanlan RL (1974) Spinal epidural cyst: theories of pathogenesis. Case report. J Neurosurg 40:774–778
Lee CH, Hyun SJ, Kim KJ, Jahng TA, Kim HJ (2012) What is a reasonable surgical procedure for spinal extradural arachnoid cysts: is cyst removal mandatory? Eight consecutive cases and a review of the literature. Acta Neurochir (Wien) 154:1219–1227
Liu JK, Cole CD, Kan P, Schmidt MH (2007) Spinal extradural arachnoid cysts: clinical, radiological, and surgical features. Neurosurg Focus 22:E6
McCrum C, Williams B (1982) Spinal extradural arachnoid pouches. Report of two cases. J Neurosurg 57:849–852
Miyamoto M, Kim K, Matsumoto R, Isobe M, Isu T (2006) Utility of preoperative magnetic resonance imaging myelography for identifying dural defects in patients with spinal extradural arachnoid cysts: case report. Neurosurgery 59:E941, discussion E941
Neo M, Koyama T, Sakamoto T, Fujibayashi S, Nakamura T (2004) Detection of a dural defect by cinematic magnetic resonance imaging and its selective closure as a treatment for a spinal extradural arachnoid cyst. Spine 29:E426–E430, Phila Pa 1976
Oh JK, Lee DY, Kim TY, Yi S, Ha Y, Kim KN, Shin H, Kim DS, Yoon DH (2012) Thoracolumbar extradural arachnoid cysts: a study of 14 consecutive cases. Acta Neurochir (Wien) 154:341–348, discussion 348
Osenbach RK, Godersky JC, Traynelis VC, Schelper RD (1992) Intradural extramedullary cysts of the spinal canal: clinical presentation, radiographic diagnosis, and surgical management. Neurosurgery 30:35–42
Park SH, Kuh SU, Lim BJ (2012) Retroperitoneal spinal extradural arachnoid cyst combined with congenital hemivertebrae. J Korean Neurosurg Soc 52:257–260
Rabb CH, McComb JG, Raffel C, Kennedy JG (1992) Spinal arachnoid cysts in the pediatric age group: an association with neural tube defects. J Neurosurg 77:369–372
Raftopoulos C, Baleriaux D, Hancq S, Closset J, David P, Brotchi J (1995) Evaluation of endoscopy in the treatment of rare meningoceles: preliminary results. Surg Neurol 44:308–317, discussion 317–308
Rimmelin A, Clouet PL, Salatino S, Kehrli P, Maitrot D, Stephan M, Dietemann JL (1997) Imaging of thoracic and lumbar spinal extradural arachnoid cysts: report of two cases. Neuroradiology 39:203–206
Rohrer DC, Burchiel KJ, Gruber DP (1993) Intraspinal extradural meningeal cyst demonstrating ball-valve mechanism of formation. Case reort. J Neurosurg 78:122–125
Swamy KS, Reddy AK, Srivastava VK, Das BS, Reddy GN (1984) Intraspinal arachnoid cysts. Clin Neurol Neurosurg 86:143–148
Swanson HS, Fincher EF (1947) Extradural arachnoidal cysts of traumatic origin. J Neurosurg 4:530–538
Tureyen K, Senol N, Sahin B, Karahan N (2009) Spinal extradural arachnoid cyst. Spine J 9:e10–e15
Yabuki S, Kikuchi S, Ikegawa S (2007) Spinal extradural arachnoid cysts associated with distichiasis and lymphedema. Am J Med Genet A 143A:884–887
Conflicts of interest
All authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Qi, W., Zhao, L., Fang, J. et al. Clinical characteristics and treatment strategies for idiopathic spinal extradural arachnoid cysts: a single-center experience. Acta Neurochir 157, 539–545 (2015). https://doi.org/10.1007/s00701-014-2278-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-014-2278-3