Abstract
Introduction
Cervical spondylotic myelopathy (CSM) can lead to significant disability through a spectrum of clinical manifestations ranging from dexterity loss to more profound weakness, incontinence and paralysis.
Aim
To determine the outcome of surgical decompression for CSM and investigate pre-operative predictors of outcome.
Methods
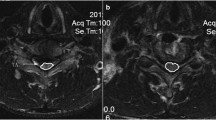
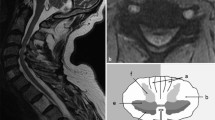
Prospectively collected data on all patients who underwent decompressive surgery for CSM and completed 12-month follow-up were reviewed. Data on age, MRI T1 and T2 signal changes pre-operatively, surgical approach and the Nurick’s Myelopathy Grade (NMG) was analysed pre-operatively and 1 year post-surgery.
Results
Data on 93 consecutive patients who underwent surgery for CSM were reviewed. Median age was 62 (23–94) years and 59 % were male. The median follow-up was 37 (17–88) months. The approach was anterior in 38 (42 %) patients, posterior in 55 (58 %); improvement was not significantly different when the two groups were compared. The number of levels decompressed increased with age (p value <0.0001). The group with a pre-operatively high signal on T1-weighted MRI images [n = 28 (30 %)] was associated with less neurological recovery post-operatively compared to the patients with a normal T1 cord signal. None of the patients deteriorated neurologically post-operatively, while 66 % improved by at least one NMG.
Conclusion
Surgical decompressions for CSM stop the progress of symptoms at 12 months post-surgery and may result in a significant improvement of NMG in two-thirds of the patients. Changes in the T1-weighted MRI images predict worse outcomes following surgery.


Similar content being viewed by others
References
Bartels RH, Fehlings MG, Abumi K (2013) Cervical spondylotic myelopathy: an update: editorial. Eur Spine J. doi:10.1007/s00586-013-3105-x
Clarke E, Robinson PK (1956) Cervical myelopathy: a complication of cervical spondylosis. Brain 79:483–510
Karadimas SK, Erwin WM, Ely CG, Dettori JR, Fehlings MG (2013) Pathophysiology and natural history of cervical spondylotic myelopathy. Spine (Phila Pa 1976) 38:S21–S36. doi:10.1097/BRS.0b013e3182a7f2c3
Matz PG, Anderson PA, Holly LT, Groff MW, Heary RF, Kaiser MG, Mummaneni PV, Ryken TC, Choudhri TF, Vresilovic EJ, Resnick DK (2009) The natural history of cervical spondylotic myelopathy. J Neurosurg Spine 11:104–111. doi:10.3171/2009.1.SPINE08716
Kalsi-Ryan S, Karadimas SK, Fehlings MG (2013) Cervical spondylotic myelopathy: the clinical phenomenon and the current pathobiology of an increasingly prevalent and devastating disorder. Neurosci Rev J Bringing Neurobiol Neurol Psychiatry 19:409–421. doi:10.1177/1073858412467377
Al-Tamimi YZ, Guilfoyle M, Seeley H, Laing RJ (2013) Measurement of long-term outcome in patients with cervical spondylotic myelopathy treated surgically. Eur Spine J Off Pub Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc 22:2552–2557. doi:10.1007/s00586-013-2965-4
Sadasivan KK, Reddy RP, Albright JA (1993) The natural history of cervical spondylotic myelopathy. Yale J Biol Med 66:235–242
Furlan JC, Kalsi-Ryan S, Kailaya-Vasan A, Massicotte EM, Fehlings MG (2011) Functional and clinical outcomes following surgical treatment in patients with cervical spondylotic myelopathy: a prospective study of 81 cases. J Neurosurg Spine 14:348–355. doi:10.3171/2010.10.SPINE091029
Sampath P, Bendebba M, Davis JD, Ducker TB (2000) Outcome of patients treated for cervical myelopathy. A prospective, multicenter study with independent clinical review. Spine (Phila Pa 1976) 25:670–676
Nurick S (1972) The pathogenesis of the spinal cord disorder associated with cervical spondylosis. Brain 95:87–100
Sodeyama T, Goto S, Mochizuki M, Takahashi J, Moriya H (1999) Effect of decompression enlargement laminoplasty for posterior shifting of the spinal cord. Spine (Phila Pa 1976) 24:1527–1531 (discussion 1531–1522)
Rao R, Gourab K, David KS (2006) Operative treatment of cervical spondylotic myelopathy. J Bone Joint Surg Am 88:1619–1640. doi:10.2106/JBJS.F.00014
Sakaura H, Hosono N, Mukai Y, Ishii T, Iwasaki M, Yoshikawa H (2005) Long-term outcome of laminoplasty for cervical myelopathy due to disc herniation: a comparative study of laminoplasty and anterior spinal fusion. Spine (Phila Pa 1976) 30:756–759. doi:10.1097/01.brs.0000157415.79713.7e
Wada E, Suzuki S, Kanazawa A, Matsuoka T, Miyamoto S, Yonenobu K (2001) Subtotal corpectomy versus laminoplasty for multilevel cervical spondylotic myelopathy: a long-term follow-up study over 10 years. Spine (Phila Pa 1976) 26:1443–1447 (discussion 1448)
Fehlings MG, Barry S, Kopjar B, Yoon ST, Arnold P, Massicotte EM, Vaccaro A, Brodke DS, Shaffrey C, Smith JS, Woodard E, Banco RJ, Chapman J, Janssen M, Bono C, Sasso R, Dekutoski M, Gokaslan ZL (2013) Anterior versus posterior surgical approaches to treat cervical spondylotic myelopathy: outcomes of the prospective multicenter AOSpine North America CSM study in 264 patients. Spine (Phila Pa 1976) 38:2247–2252. doi:10.1097/BRS.0000000000000047
Liu T, Xu W, Cheng T, Yang HL (2011) Anterior versus posterior surgery for multilevel cervical myelopathy, which one is better? A systematic review. Eur Spine J Off Pub Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc 20:224–235. doi:10.1007/s00586-010-1486-7
Zhu B, Xu Y, Liu X, Liu Z, Dang G (2013) Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review and meta-analysis. Eur Spine J Off Pub Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc 22:1583–1593. doi:10.1007/s00586-013-2817-2
Lawrence BD, Jacobs WB, Norvell DC, Hermsmeyer JT, Chapman JR, Brodke DS (2013) Anterior versus posterior approach for treatment of cervical spondylotic myelopathy: a systematic review. Spine (Phila Pa 1976) 38:S173–S182. doi:10.1097/BRS.0b013e3182a7eaaf
Kawakami M, Tamaki T, Iwasaki H, Yoshida M, Ando M, Yamada H (2000) A comparative study of surgical approaches for cervical compressive myelopathy. Clin Orthop Relat Res 381:129–136
Chiba K, Toyama Y, Watanabe M, Maruiwa H, Matsumoto M, Hirabayashi K (2000) Impact of longitudinal distance of the cervical spine on the results of expansive open-door laminoplasty. Spine (Phila Pa 1976) 25:2893–2898
Suri A, Chabbra RP, Mehta VS, Gaikwad S, Pandey RM (2003) Effect of intramedullary signal changes on the surgical outcome of patients with cervical spondylotic myelopathy. Spine J Off J North Am Spine Soc 3:33–45
Morio Y, Teshima R, Nagashima H, Nawata K, Yamasaki D, Nanjo Y (2001) Correlation between operative outcomes of cervical compression myelopathy and MRI of the spinal cord. Spine (Phila Pa 1976) 26:1238–1245
Fernandez de Rota JJ, Meschian S, Fernandez de Rota A, Urbano V, Baron M (2007) Cervical spondylotic myelopathy due to chronic compression: the role of signal intensity changes in magnetic resonance images. J Neurosurg Spine 6:17–22. doi:10.3171/spi.2007.6.1.4
Yagi M, Ninomiya K, Kihara M, Horiuchi Y (2010) Long-term surgical outcome and risk factors in patients with cervical myelopathy and a change in signal intensity of intramedullary spinal cord on magnetic resonance imaging. J Neurosurg Spine 12:59–65. doi:10.3171/2009.5.SPINE08940
Cho YE, Shin JJ, Kim KS, Chin DK, Kuh SU, Lee JH, Cho WH (2011) The relevance of intramedullary high signal intensity and gadolinium (Gd-DTPA) enhancement to the clinical outcome in cervical compressive myelopathy. Eur Spine J Off Pub Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc 20:2267–2274. doi:10.1007/s00586-011-1878-3
Avadhani A, Rajasekaran S, Shetty AP (2010) Comparison of prognostic value of different MRI classifications of signal intensity change in cervical spondylotic myelopathy. Spine J Off J North Am Spine Soc 10:475–485. doi:10.1016/j.spinee.2010.03.024
Mizuno J, Nakagawa H, Inoue T, Hashizume Y (2003) Clinicopathological study of “snake-eye appearance” in compressive myelopathy of the cervical spinal cord. J Neurosurg 99:162–168
Kawaguchi Y, Kanamori M, Ishihara H, Ohmori K, Abe Y, Kimura T (2003) Pathomechanism of myelopathy and surgical results of laminoplasty in elderly patients with cervical spondylosis. Spine (Phila Pa 1976) 28:2209–2214. doi:10.1097/01.BRS.0000085029.65713.B0
Lee TT, Manzano GR, Green BA (1997) Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement. J Neurosurg 86:64–68. doi:10.3171/jns.1997.86.1.0064
Chiles BW, 3rd, Leonard MA, Choudhri HF, Cooper PR (1999) Cervical spondylotic myelopathy: patterns of neurological deficit and recovery after anterior cervical decompression. Neurosurgery 44:762–769 (discussion 769–770)
Tetreault LA, Karpova A, Fehlings MG (2013) Predictors of outcome in patients with degenerative cervical spondylotic myelopathy undergoing surgical treatment: results of a systematic review. Eur Spine J Off Pub Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc. doi:10.1007/s00586-013-2658-z
Kohno K, Kumon Y, Oka Y, Matsui S, Ohue S, Sakaki S (1997) Evaluation of prognostic factors following expansive laminoplasty for cervical spinal stenotic myelopathy. Surg Neurol 48:237–245
Kaptain GJ, Simmons NE, Replogle RE, Pobereskin L (2000) Incidence and outcome of kyphotic deformity following laminectomy for cervical spondylotic myelopathy. J Neurosurg 93:199–204
Kato Y, Iwasaki M, Fuji T, Yonenobu K, Ochi T (1998) Long-term follow-up results of laminectomy for cervical myelopathy caused by ossification of the posterior longitudinal ligament. J Neurosurg 89:217–223. doi:10.3171/jns.1998.89.2.0217
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Salem, H.M.I., Salem, K.M.I., Burget, F. et al. Cervical spondylotic myelopathy: the prediction of outcome following surgical intervention in 93 patients using T1- and T2-weighted MRI scans. Eur Spine J 24, 2930–2935 (2015). https://doi.org/10.1007/s00586-015-4028-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-4028-5