Abstract
Background
Earlier studies done to compare the efficacy of use of local anesthetics at intraperitoneal location versus intraincisional use had utilized equal amount of drugs at the two locations, usually 10–20 ml. Using this large amount of drug in the small space of intraincisional location as compared to similar amount of drug in large intraperitoneal space created an inadvertent bias in favor of patients receiving the drug intraincisionally so these patients naturally experienced less pain.
Aims and objectives
To conduct a randomized, triple-blind, placebo-controlled study by standardizing dose of local anesthetic, to compare the effectiveness of intraperitoneal against intraincisional use of ropivacaine 0.2% for post-laparoscopic cholecystectomy pain relief.
Materials and methods
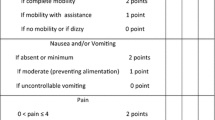
294 patients underwent elective 4-port laparoscopic cholecystectomy. Patients were triple blindly randomized. All patients received ~ 23 ml of solution, of which 20 ml was given intraperitoneally (1 ml/cm; 16 ml along right hemi-dome and 4 ml in gall bladder fossa) and ~ 3 ml intraincisionally (1 ml/cm of length of incision). Solution was either normal saline or drug (0.2% ropivacaine) depending on the group [controls (n = 86), intraperitoneal group (n = 100), and intraincisional group (n = 108)]. 5 different pain scales were used for assessment of overall pain. Pain scores were assessed at 5 points of time.
Results
Patients in intraincisional group showed significantly less overall pain and rescue analgesia requirement (p < 0.05). Intraincisional group showed significantly less overall pain (p < 0.05) as compared to intraperitoneal group; however, use of rescue analgesia was comparable in the two groups (p > 0.05); and shoulder pain was significantly less in intraperitoneal group (p < 0.05).
Conclusion
The intraincisional use of injection ropivacaine at its minimum concentration of 0.2% in minimal doses of 1 ml/cm at the end of procedure provides significantly more post-operative analgesia as compared to intraperitoneal group and controls. However, for controlling shoulder pain, the use of intraperitoneal ropivacaine is desirable.








Similar content being viewed by others
References
Tandon RK (2000) Prevalence and type of biliary stones in India. World J Gastroenterol 6 Suppl 4:4–5
McMahon AJ, Russell IT, Ramsay G, Sunderland G, Baxter JN, Anderson JR, Galloway D, O’Dwyer PJ (1994) Laparoscopic and minilaparotomy cholecystectomy: a randomized trial comparing postoperative pain and pulmonary function. Surgery 115:533–539
Ure BM, Troidl H, Spangenberger W, Dietrich A, Lefering R, Neugebauer E (1994) Pain after laparoscopic cholecystectomy. Intensity and localization of pain and analysis of predictors in preoperative symptoms and intraoperative events. Surg Endosc 8:90–96
Fiorillo MA, Davidson PG, Fiorillo M, D’Anna JA Jr, Sithian N, Silich RJ (1996) 149 ambulatory laparoscopic cholecystectomies. Surg Endosc 10:52–56
Callesen T, Klarskov B, Mogensen TS, Kehlet H (1998) Ambulatory laparoscopic cholecystectomy. Feasibility and convalescence. Ugeskr Laeg 160:2095–2100
de La Coussaye JE, Eledjam JJ, Brugada J, Sassine A (1993) Cardiotoxicity of local anesthetics. Cah Anesthesiol 41:589–598
Whiteside JB, Wildsmith JA (2001) Developments in local anaesthetic drugs. Brit J Anaesth 87:27–35
Wang RD, Dangler LA, Greengrass RA (2001) Update on ropivacaine. Expert Opin Pharmacother 2:2051–2063
Kuthiala G, Chaudhary G (2011) Ropivacaine: A review of its pharmacology and clinical use. Ind J Anaesth 55:104–110
Scott DB, Lee A, Fagan D, Bowler GM, Bloomfield P, Lundh R (1989) Acute toxicity of ropivacaine compared with that of bupivacaine. Anesthe Analg 69:563–569
McClure JH (1996) Ropivacaine. Brit J Anaesth 76:300–307
Zink W, Graf BM (2008) The toxicity of local anesthetics: the place of ropivacaine and levobupivacaine. Curr Opin Anaesthesiol 21:645–650
Ortiz J, Rajagopalan S (2014) A review of local anesthetic techniques for analgesia after laparoscopic surgery. J Minim Invasive Surg Sci 3:e11310
FDA Drugs@FDA: FDA Approved Drug Products-NAROPIN. https://www.accessdata.fda.gov/scripts/cder/daf/index.cfm?event=overview.process&ApplNo=020533;Accessed 09 Aug 2017
Torgerson DJ, Roberts C (1999) Understanding controlled trials. Randomisation methods: concealment. BMJ 319:375–376
Doig GS, Simpson F (2005) Randomization and allocation concealment: a practical guide for researchers. J Crit Care 20
Parker MJ, Manan A, Duffett M (2012) Rapid, easy, and cheap randomization: prospective evaluation in a study cohort. Trials 13:90
Leppert W (2010) Role of intranasal fentanyl in breakthrough pain management in cancer patients. Cancer Manag Res 2:225–232
Cassart M, Pettiaux N, Gevenois PA, Paiva M, Estenne M (1997) Effect of chronic hyperinflation on diaphragm length and surface area. Am J Respir Crit Care Med 156:504–508
Yaksh TL, Wallace MS (2011) Chap. 18. opioids, analgesia, and pain management. In: Brunton LL, Chabner BA, Knollmann BC (eds) Goodman & Gilman’s the pharmacological basis of therapeutics. McGraw-Hill Education, New York, pp 481–526
Kadam P, Bhalerao S (2010) Sample size calculation. Int J Ayur Res 1:55–57
Ingelmo PM, Bucciero M, Somaini M, Sahillioglu E, Garbagnati A, Charton A, Rossini V, Sacchi V, Scardilli M, Lometti A, Joshi GP, Fumagalli R, Diemunsch P (2013) Intraperitoneal nebulization of ropivacaine for pain control after laparoscopic cholecystectomy: a double-blind, randomized, placebo-controlled trial. Brit J Anaesth 110:800–806
El-Labban GM, Hokkam EN, El-Labban MA, Morsy K, Saadl S, Heissam KS (2011) Intraincisional vs intraperitoneal infiltration of local anaesthetic for controlling early post-laparoscopic cholecystectomy pain. J Minim Access Surg 7:173–177
Cha SM, Kang H, Baek CW, Jung YH, Koo GH, Kim BG, Choi YS, Cha SJ, Cha YJ (2012) Peritrocal and intraperitoneal ropivacaine for laparoscopic cholecystectomy: a prospective, randomized, double-blind controlled trial. J Surg Res 175:251–258
Wiesenfeld-Hallin Z (2005) Sex differences in pain perception. Gend Med 2:137–145
Uchiyama K, Kawai M, Tani M, Ueno M, Hama T, Yamaue H (2006) Gender differences in postoperative pain after laparoscopic cholecystectomy. Surg Endosc 20:448–451
Gurusamy KS, Samraj K, Mullerat P, Davidson BR (2007) Routine abdominal drainage for uncomplicated laparoscopic cholecystectomy. Cochrane Database Syst Rev:Cd006004
Overby DW, Apelgren KN, Richardson W, Fanelli R (2010) SAGES guidelines for the clinical application of laparoscopic biliary tract surgery. Surg Endosc 24:2368–2386
Bisgaard T (2005) Treatment of pain after laparoscopic cholecystectomy. Ugeskr Laeg 167:2629–2632
Bisgaard T, Klarskov B, Kristiansen VB, Callesen T, Schulze S, Kehlet H, Rosenberg J (1999) Multi-regional local anesthetic infiltration during laparoscopic cholecystectomy in patients receiving prophylactic multi-modal analgesia: a randomized, double-blinded, placebo-controlled study. Anesth Analg 89:1017–1024
Bisgaard T, Klarskov B, Rosenberg J, Kehlet H (2001) Characteristics and prediction of early pain after laparoscopic cholecystectomy. Pain 90:261–269
Bisgaard T, Klarskov B, Kehlet H, Rosenberg J (2003) Preoperative dexamethasone improves surgical outcome after laparoscopic cholecystectomy: a randomized double-blind placebo-controlled trial. Ann Surg 238:651–660
Bisgaard T (2006) Analgesic treatment after laparoscopic cholecystectomy: a critical assessment of the evidence. Anesthesiology 104:835–846
Elhakim M, Elkott M, Ali NM, Tahoun HM (2000) Intraperitoneal lidocaine for postoperative pain after laparoscopy. Acta Anaesthesiol Scand 44:280–284
Lee I-O, Kim S-H, Kong M-H, Lee M-K, Kim N-S, Choi Y-S, Lim S-H (2001) Pain after laparoscopic cholecystectomy: the effect and timing of incisional and intraperitoneal bupivacaine. Can J Anaesth 48:545–550
Inan A, Sen M, Dener C (2004) Local anesthesia use for laparoscopic cholecystectomy. World J Surg 28:741–744
Roberts KJ, Gilmour J, Pande R, Nightingale P, Tan LC, Khan S (2011) Efficacy of intraperitoneal local anaesthetic techniques during laparoscopic cholecystectomy. Surg Endosc 25:3698–3705
Chakravarty N, Singhai S, Shidhaye RV (2014) Evaluation of intraperitoneal bupivacaine for postoperative analgesia in patients undergoing laparoscopic cholecystectomy: a prospective randomized trial. Anaesth Pain Intensive Care 18:361–366
Papagiannopoulou P, Argiriadou H, Georgiou M, Papaziogas B, Sfyra E, Kanakoudis F (2003) Preincisional local infiltration of levobupivacaine vs ropivacaine for pain control after laparoscopic cholecystectomy. Surg Endosc 17:1961–1964
Cantore F, Boni L, Di Giuseppe M, Giavarini L, Rovera F, Dionigi G (2008) Pre-incision local infiltration with levobupivacaine reduces pain and analgesic consumption after laparoscopic cholecystectomy: a new device for day-case procedure. Int J Surg 6(Suppl 1):S89–S92
Karaman Y, Kebapçı E, Görgün M, Güvenli Y, Tekgül Z (2014) Post-laparoscopic cholecystectomy pain: effects of preincisional infiltration and intraperitoneal levobupivacaine 0.25% on pain control-a randomized prospective double-blinded placebo-controlled trial. Turk J Anaesthesiol Reanim 42:80–85
Papaziogas B, Argiriadou H, Papagiannopoulou P, Pavlidis T, Georgiou M, Sfyra E, Papaziogas T (2001) Preincisional intravenous low-dose ketamine and local infiltration with ropivacaine reduces postoperative pain after laparoscopic cholecystectomy. Surg Endosc 15:1030–1033
Labaille T, Mazoit JX, Paqueron X, Franco D, Benhamou D (2002) The clinical efficacy and pharmacokinetics of intraperitoneal ropivacaine for laparoscopic cholecystectomy. Anesth Analg 94:100–105
Sozbilen M, Yeniay L, Unalp O, Makay O, Ersin S, Pirim A, Ulukaya S, Uyar M (2007) Effects of ropivacaine on pain after laparoscopic cholecystectomy: A prospective, randomized study. Adv Ther 24:247–257
Pappas-Gogos G, Tsimogiannis KE, Zikos N, Nikas K, Manataki A, Tsimoyiannis EC (2008) Preincisional and intraperitoneal ropivacaine plus normal saline infusion for postoperative pain relief after laparoscopic cholecystectomy: a randomized double-blind controlled trial. Surg Endosc 22:2036–2045
Liu Y-Y, Yeh C-N, Lee H-L, Wang S-Y, Tsai C-Y, Lin C-C, Chao T-C, Yeh T-S, Jan Y-Y (2009) Local anesthesia with ropivacaine for patients undergoing laparoscopic cholecystectomy. World J Gastroenterol 15:2376–2380
Liang HS, Feng Y, Liu YZ, An HY, Yang BX (2011) Effect of flurbiprofen combined different concentrations of ropivacaine local infiltration on postoperative analgesia after laparoscopic cholecystectomy. Beijing Da Xue Xue Bao 43:753–756
Bucciero M, Ingelmo PM, Fumagalli R, Noll E, Garbagnati A, Somaini M, Joshi GP, Vitale G, Giardini V, Diemunsch P (2011) Intraperitoneal ropivacaine nebulization for pain management after laparoscopic cholecystectomy: a comparison with intraperitoneal instillation. Anesth Analg 113:1266–1271
Evaristo-Mendez G, Garcia de Alba-Garcia JE, Sahagun-Flores JE, Ventura-Sauceda FA, Mendez-Ibarra JU, Sepulveda-Castro RR (2013) Analgesic efficacy of the incisional infiltration of ropivacaine vs ropivacaine with dexamethasone in the elective laparoscopic cholecystectomy. Cir Cir 81:383–393
Liu D-S, Guan F, Wang B, Zhang T (2015) Combined usage with intraperitoneal and incisional ropivacaine reduces pain severity after laparoscopic cholecystectomy. Int J Clin Exp Med 8:22460–22468
Gupta M, Naithani U, Singariya G, Gupta S (2016) Comparison of 0.25% ropivacaine for intraperitoneal instillation v/s rectus sheath block for postoperative pain relief following laparoscopic cholecystectomy: a prospective study. J Clin Diagn Res 10:Uc10–U15
Abet E, Orion F, Denimal F, Brau-Weber AG, de Kerviler B, Jean MH, Boulanger G, Dimet J, Comy M (2017) Interest of using ropivacaine for outpatient laparoscopic cholecystectomy: prospective randomized trial. World J Surg 41:687–692
Allegri M, Ornaghi M, Ferland CE (2017) Peritoneal nebulization of ropivacaine during laparoscopic cholecystectomy: dose finding and pharmacokinetic study. Pain Res Manag 2017:4260702
Yeh CN, Tsai CY, Cheng CT, Wang SY, Liu YY, Chiang KC, Hsieh FJ, Lin CC, Jan YY, Chen MF (2014) Pain relief from combined wound and intraperitoneal local anesthesia for patients who undergo laparoscopic cholecystectomy. BMC Surg 14:28
Kucuk C, Kadiogullari N, Canoler O, Savli S (2007) A placebo-controlled comparison of bupivacaine and ropivacaine instillation for preventing postoperative pain after laparoscopic cholecystectomy. Surg Today 37:396–400
Babu R, Jain P, Sherif L (2013) Intraperitoneal instillation: ropivacaine vs bupivacaine for post operative pain relief in laparoscopic cholecystectomy. Int J Health Sci Res 3:42–47
Honca M, Kose EA, Bulus H, Horasanli E (2014) The postoperative analgesic efficacy of intraperitoneal bupivacaine compared with levobupivacaine in laparoscopic cholecystectomy. Acta Chir Belg 114:174–178
Parikh GP, Shah VR, Vora KS, Parikh BK, Modi MP, Kumari P (2014) Ultrasound guided peritubal infiltration of 0.25% Bupivacaine versus 0.25% Ropivacaine for postoperative pain relief after percutaneous nephrolithotomy: A prospective double blind randomized study. Ind J Anaesth 58:293–297
Choi GJ, Kang H, Baek CW, Jung YH, Kim DR (2015) Effect of intraperitoneal local anesthetic on pain characteristics after laparoscopic cholecystectomy. World J Gastroenterol 21:13386–13395
Ahn Y, Woods J, Connor S (2011) A systematic review of interventions to facilitate ambulatory laparoscopic cholecystectomy. HPB (Oxford) 13:677–686
Pavlidis TE, Atmatzidis KS, Papaziogas BT, Makris JG, Lazaridis CN, Papaziogas TB (2003) The effect of preincisional periportal infiltration with ropivacaine in pain relief after laparoscopic procedures: a prospective, randomized controlled trial. JSLS 7:305–310
Lee IO, Kim SH, Kong MH, Lee MK, Kim NS, Choi YS, Lim SH (2001) Pain after laparoscopic cholecystectomy: the effect and timing of incisional and intraperitoneal bupivacaine. Can J Anaesth 48:545–550
Nicolau AE, Merlan V, Grecu I, Nicolau M, Micu B (2008) [Multimodal analgesia in elective laparoscopic cholecystectomy. A double-blind randomized controlled trial]. Chirurgia (Bucur) 103:547–551
American Society of Anesthesiologists Task Force on Acute Pain Management (2012) Practice guidelines for acute pain management in the perioperative setting: an updated report by the American Society of Anesthesiologists Task Force on Acute Pain Management. Anesthesiology 116:248–273
Acknowledgements
Professor Ramesh Chand Goel, Department of Statistics, PGIMER, Chandigarh helped in conducting the statistical analysis comprehensively. Department of English, Faculty of Arts, Aligarh Muslim University helped in critically revising the manuscript for English language corrections and grammatical mistakes.
Funding
No external funding source/agency.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
The authors have been associated with the same institution in the time period of 36 months while this study was conducted and no corporate/commercial relationships existed in relation to this study or any other during this time duration. This study received no funding in any form, from any other source whether inside or outside the institution. No financial or any form of vested interest exists between the authors and the manufacturers of Injection Ropin 0.2% marketed by Neon Laboratories Ltd., Mumbai, India. The drug brand was chosen because of its easy and free availability through the hospital drug section. Drs. Singh Mathuria Kaushal-Deep, Afzal Anees, Shehtaj Khan, Mohammad Amanullah Khan, and Mehershree Lodhi have no conflicts of interest or financial ties to disclose
Rights and permissions
About this article
Cite this article
Kaushal-Deep, S.M., Anees, A., Khan, S. et al. Randomized controlled study of intraincisional infiltration versus intraperitoneal instillation of standardized dose of ropivacaine 0.2% in post-laparoscopic cholecystectomy pain: Do we really need high doses of local anesthetics—time to rethink!. Surg Endosc 32, 3321–3341 (2018). https://doi.org/10.1007/s00464-018-6053-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6053-z