Abstract
Background
Endoscopic resection (ER) is curative treatment option for early gastric cancer (EGC). Additional surgery is required when the tumor pathology is beyond ER indication. It is unclear whether tumor size can be correlated with indications for surgery after ER. Therefore, we aimed to access the role of tumor size for surgical decision making after ER.
Methods
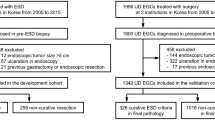
We reviewed clinicopathological data from 3246 patients underwent gastrectomy for EGC. The patients were classified into three groups as follows: the ulcer-negative intramucosal cancer with undifferentiated histology, ulcerative intramucosal cancer with differentiated histology, and minute submucosal (SM1) cancer with differentiated histology. The probability of additional surgery after ER was defined as at least one positive result for lymph node metastasis, lymphovascular invasion or perineural invasion. The probability was compared between individual tumor size and ER size criteria in each group using area under receiver operating characteristic curves.
Results
The probabilities of ulcer-negative intramucosal cancer with undifferentiated histology, SM1 cancer with differentiated histology and ulcerative intramucosal cancer with differentiated histology were 4.2, 22.1 and 2.5 %. In the ulcerative intramucosal cancer with differentiated histology group, these probabilities increased when the difference in tumor size was >1 mm compared with ER size criteria. The probability was not increased when there was a >10-mm tumor size difference compared with ER size criteria in the other two groups.
Conclusions
Tumor size was correlated with ER criteria in patients with ulcerative intramucosal cancer with differentiated histology after ER but was not strictly correlated with ER criteria in the other two patient groups. However, further study may be necessary to validate our results in the future.



Similar content being viewed by others
References
Abe S, Oda I, Suzuki H, Nonaka S, Yoshinaga S, Odagaki T, Taniguchi H, Kushima R, Saito Y (2013) Short- and long-term outcomes of endoscopic submucosal dissection for undifferentiated early gastric cancer. Endoscopy 45(9):703–707
Gotoda T (2007) Endoscopic resection of early gastric cancer. Gastric Cancer 10(1):1–11
Gotoda T, Yanagisawa A, Sasako M, Ono H, Nakanishi Y, Shimoda T, Kato Y (2000) Incidence of lymph node metastasis from early gastric cancer: estimation with a large number of cases at two large centers. Gastric Cancer 3(4):219–225
An JY, Baik YH, Choi MG, Noh JH, Sohn TS, Kim S (2007) Predictive factors for lymph node metastasis in early gastric cancer with submucosal invasion: analysis of a single institutional experience. Ann Surg 246(5):749–753
Park YD, Chung YJ, Chung HY, Yu W, Bae HI, Jeon SW, Cho CM, Tak WY, Kweon YO (2008) Factors related to lymph node metastasis and the feasibility of endoscopic mucosal resection for treating poorly differentiated adenocarcinoma of the stomach. Endoscopy 40(1):7–10
Yamaguchi N, Isomoto H, Fukuda E, Ikeda K, Nishiyama H, Akiyama M, Ozawa E, Ohnita K, Hayashi T, Nakao K, Kohno S, Shikuwa S (2009) Clinical outcomes of endoscopic submucosal dissection for early gastric cancer by indication criteria. Digestion 80(3):173–181
Kang MS, Hong SJ, Kim DY, Han JP, Choi MH, Kim HK, Ko BM, Lee MS (2015) Long-term outcome after endoscopic submucosal dissection for early gastric cancer: focusing on a group beyond the expanded indication. J Dig Dis 16(1):7–13
Ryu KW, Choi IJ, Doh YW, Kook MC, Kim CG, Park HJ, Lee JH, Lee JS, Lee JY, Kim YW, Bae JM (2007) Surgical indication for non-curative endoscopic resection in early gastric cancer. Ann Surg Oncol 14(12):3428–3434
Li H, Lu P, Lu Y, Liu C, Xu H, Wang S, Chen J (2010) Predictive factors of lymph node metastasis in undifferentiated early gastric cancers and application of endoscopic mucosal resection. Surg Oncol 19(4):221–226
Abe N, Watanabe T, Sugiyama M, Yanagida O, Masaki T, Mori T, Atomi Y (2004) Endoscopic treatment or surgery for undifferentiated early gastric cancer? Am J Surg 188(2):181–184
Ito H, Inoue H, Ikeda H, Odaka N, Yoshida A, Satodate H, Onimaru M, Takayanagi D, Santi EG, Kudo SE (2013) Surgical outcomes and clinicopathological characteristics of patients who underwent potentially noncurative endoscopic resection for gastric cancer: a report of a single-center experience. Gastroenterol Res Pract 2013:427405
Kim H, Kim JH, Park JC, Lee YC, Noh SH, Kim H (2011) Lymphovascular invasion is an important predictor of lymph node metastasis in endoscopically resected early gastric cancers. Oncol Rep 25(6):1589–1595
Son SY, Park JY, Ryu KW, Eom BW, Yoon HM, Cho SJ, Lee JY, Kim CG, Lee JH, Kook MC, Choi IJ, Kim YW (2013) The risk factors for lymph node metastasis in early gastric cancer patients who underwent endoscopic resection: is the minimal lymph node dissection applicable? A retrospective study. Surg Endosc 27(9):3247–3253
Katsube T, Murayama M, Yamaguchi K, Usuda A, Shimazaki A, Asaka S, Konnno S, Miyaki A, Usui T, Yokomizo H, Shiozawa S, Yoshimatsu K, Shimakawa T, Naritaka Y (2015) Additional surgery after non-curative resection of ESD for early gastric cancer. Anticancer Res 35(5):2969–2974
Acknowledgments
This work received approval by the Yonsei University College of Medicine Institutional Review Board on January 2013. This research was supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education, Science and Technology (2012R1A1A1042417).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Hae Won Kim, Yoo Jin Lee, Jie-Hyun Kim, Jae Jun Park, Young Hoon Youn, Hyojin Park, Jong Won Kim, Seung Ho Choi, Sung Hoon Noh have no conflict of interest or financial relationships relevant to this publication.
Additional information
Hae Won Kim and Yoo Jin Lee have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Kim, H.W., Lee, Y.J., Kim, JH. et al. The role of tumor size in surgical decision making after endoscopic resection for early gastric cancer. Surg Endosc 30, 2799–2803 (2016). https://doi.org/10.1007/s00464-015-4556-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-015-4556-4