Abstract
Purpose
The purpose of the study was to describe a unique type of low-energy traumatic pediatric thoracic spinal cord injury without radiographic abnormality (SCIWORA) after a back bend during dance practice and analyze the trauma mechanisms and treatment protocols.
Methods
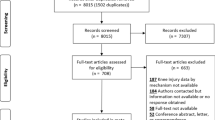
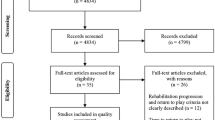
This was a retrospective case series from September 2007 to August 2016. The study was conducted at a tertiary medical center in Beijing, China (Xuanwu Hospital, China International Neuroscience Institute [China-INI], Capital Medical University). A total of 12 pediatric patients who had a clear traumatic history after back bend movements and had been diagnosed with thoracic SCIWORA were included. Clinical and imaging data were obtained for each patient. The follow-up data was analyzed. The traumatic mechanisms were investigated by analyzing the patients’ medical history, spinal diffusion tensor imaging (DTI) and fiber tractography data.
Results
Of the 12 patients, 11 (91.7%) were younger than 8 years old. The mean age of the patients was 6.6 years. All patients had a clear traumatic history of severe thoracic spinal cord injury after performing back bend movements. The mean follow-up time was 36.5 months. During the follow-up period, 1 patient (8.3%) recovered completely, and 11 patients (91.7%) had unfavorable prognoses, including 4 (33.3%) with incomplete recovery and 7 (58.3%) with no change. Two patients underwent spinal DTI, which showed rupture of the nerve fiber bundle in the section of the injury.
Conclusions
Back bend movements performed during dance practice may cause pediatric thoracic SCIWORA, particularly in children younger than 8 years old. We suggest that the mechanism of primary injury is the longitudinal distraction of the thoracic spine during back bend movements, which leads to violent distraction of the spinal cord and blunt injury of nerve axons, nerve cells, and small vessels. Spinal DTI may facilitate the diagnosis and prognostic evaluation of SCIWORA.





Similar content being viewed by others
Abbreviations
- SCIWORA:
-
Spinal cord injury without radiographic abnormality
- MRI:
-
Magnetic resonance imaging
- CT:
-
Computed tomography
- DTI:
-
Diffusion tensor imaging
- ASIA:
-
The American Spinal Injury Association.
References
Pang D, Wilberger JE Jr (1982) Spinal cord injury without radiographic abnormalities in children. J Neurosurg 57(1):114–129. doi:10.3171/jns.1982.57.1.0114
Szwedowski D, Walecki J (2014) Spinal cord injury without radiographic abnormality (SCIWORA)—clinical and radiological aspects. Pol J Radiol 79:461–464. doi:10.12659/PJR.890944
Pang D (2004) Spinal cord injury without radiographic abnormality in children, 2 decades later. Neurosurgery 55:1325–1342 . doi:10.1227/01.NEU.0000143030.85589.E6discussion 1342
Carroll T, Smith CD, Liu X et al (2015) Spinal cord injuries without radiologic abnormality in children: a systematic review. Spinal Cord 53(12):842–848. doi:10.1038/sc.2015.110
Burke DC (1974) Traumatic spinal paralysis in children. Paraplegia 11(4):268–276. doi:10.1038/sc.1973.39
Piatt JH (2015) Pediatric spinal injury in the US: epidemiology and disparities. J Neurosurg—Pediatr 16(4):463–471. doi:10.3171/2015.2.PEDS1515
Hendey GW, Wolfson AB, Mower WR, Hoffman JR, National Emergency X-Radiography Utilization Study Group (2002) Spinal cord injury without radiographic abnormality: results of the National Emergency X-Radiography Utilization Study in blunt cervical trauma. J Trauma 53(1):1–4. doi:10.1097/00005373-200207000-00001
Robles LA (2007) Traumatic spinal cord infarction in a child: case report and review of literature. Surg Neurol 67(5):529–534. doi:10.1016/j.surneu.2006.07.016
Pang D, Pollack IF (1989) Spinal cord injury without radiographic abnormality in children—the SCIWORA syndrome. J Trauma 29(5):654–664. doi:10.1097/00005373-198905000-00021
Walsh JW, Stevens DB, Young AB (1983) Traumatic paraplegia in children without contiguous spinal fracture or dislocation. Neurosurgery 12(4):439–445. doi:10.1227/00006123-198304000-00012
Cheshire DJ (1977) The paediatric syndrome of traumatic myelopathy without demonstrable vertebral injury. Paraplegia 15(1):74–85. doi:10.1038/sc.1977.11
Riviello JJ Jr, Marks HG, Faerber EN, Steg NL (1990) Delayed cervical central cord syndrome after trivial trauma. Pediatr Emerg Care 6(2):113–117. doi:10.1097/00006565-199006000-00012
Yamaguchi S, Hida K, Akino M, Yano S, Saito H, Iwasaki Y (2002) A case of pediatric thoracic SCIWORA following minor trauma. Childs Nerv Syst 18(5):241–243. doi:10.1007/s00381-002-0560-9
Shen H, Tang Y, Huang L et al (2007) Applications of diffusion-weighted MRI in thoracic spinal cord injury without radiographic abnormality. Int Orthop 31(3):375–383. doi:10.1007/s00264-006-0175-y
Wang YJ, Zhou HJ, Wei B et al (2016) Clinical characteristics analysis of 120 cases of pediatric spinal cord injury without radiologic abnormality. Zhonghua Yi Xue Za Zhi 96(2):122–125. doi:10.3760/cma.j.issn.0376-2491.2016.02.010
McDonald JW, Sadowsky C (2002) Spinal-cord injury. Lancet 359(9304):417–425. doi:10.1016/S0140-6736(02)07603-1
Paleologos TS, Fratzoglou MM, Papadopoulos SS, Chatzidakis EE, Gouliamos AD, Kourousis DD (1998) Posttraumatic spinal cord lesions without skeletal or discal and ligamentous abnormalities: the role of MR imaging. J Spinal Disord 11(4):346–349
Schneider RC, Cherry G, Pantek H (1954) The syndrome of acute central cervical spinal cord injury; with special reference to the mechanisms involved in hyperextension injuries of cervical spine. J Neurosurg 11(6):546–577. doi:10.3171/jns.1954.11.6.0546
Leventhal HR (1960) Birth injuries of the spinal cord. J Pediatr 56:447–453. doi:10.1016/S0022-3476(60)80356-3
Kwon BK, Tetzlaff W, Grauer JN, Beiner J, Vaccaro AR (2004) Pathophysiology and pharmacologic treatment of acute spinal cord injury. Spine J 4(4):451–464. doi:10.1016/j.spinee.2003.07.007
Carreon LY, Glassman SD, Campbell MJ (2004) Pediatric spine fractures: a review of 137 hospital admissions. J Spinal Disord Tech 17(6):477–482. doi:10.1097/01.bsd.0000132290.50455.99
Eleraky MA, Theodore N, Adams M, Rekate HL, Sonntag VK (2000) Pediatric cervical spine injuries: report of 102 cases and review of the literature. J Neurosurg 92(1 Suppl):12–17. doi:10.3171/spi.2000.92.1.0012
Hamilton MG, Myles ST (1992) Pediatric spinal injury: review of 174 hospital admissions. J Neurosurg 77(5):700–704. doi:10.3171/jns.1992.77.5.0700
Zwimpfer TJ, Bernstein M (1990) Spinal cord concussion. J Neurosurg 72(6):894–900. doi:10.3171/jns.1990.72.6.0894
Tator CH, Koyanagi I (1997) Vascular mechanisms in the pathophysiology of human spinal cord injury. J Neurosurg 86(3):483–492. doi:10.3171/jns.1997.86.3.0483
Atkinson PP, Atkinson JL (1996) Spinal shock. Mayo Clin Proc 71(4):384–389. doi:10.1016/S0025-6196(11)64067-6
Sąsiadek MJ, Szewczyk P, Bladowska J (2012) Application of diffusion tensor imaging (DTI) in pathological changes of the spinal cord. Med Sci Monit 18(6):RA73–RA79. doi:10.12659/MSM.882891
Sąsiadek M, Szewczyk P (2009) Imaging of the spine: new possibilities and its role in planning and monitoring therapy. Pol J Radiol 74:52–58
Thurnher MM, Law M (2009) Diffusion-weighted imaging, diffusion-tensor imaging, and fiber tractography of the spinal cord. Magn Reson Imaging Clin N Am 17(2):225–244. doi:10.1016/j.mric.2009.02.004
Maier SE, Mamata H (2005) Diffusion tensor imaging of the spinal cord. Ann N Y Acad Sci 1064:50–60. doi:10.1196/annals.1340.011
Shanmuganathan K, Gullapalli RP, Zhuo J, Mirvis SE (2008) Diffusion tensor MR imaging in cervical spine trauma. AJNR Am J Neuroradiol 29(4):655–659. doi:10.3174/ajnr.A0916
Bozzo A, Marcoux J, Radhakrishna M, Pelletier J, Goulet B (2011) The role of magnetic resonance imaging in the management of acute spinal cord injury. J Neurotrauma 28(8):1401–1411. doi:10.1089/neu.2009.1236
Bracken MB, Shepard MJ, Collins WF et al (1990) A randomized, controlled trial of methylprednisolone or naloxone in the treatment of acute spinal-cord injury. Results of the Second National Acute Spinal Cord Injury Study. N Engl J Med 322(20):1405–1411. doi:10.1056/NEJM199005173222001
Bracken MB, Shepard MJ, Holford TR et al (1997) Administration of methylprednisolone for 24 or 48 hours or tirilazad mesylate for 48 hours in the treatment of acute spinal cord injury. Results of the third national Acute Spinal Cord Injury Randomized Controlled Trial. National Acute Spinal Cord Injury Study JAMA 277(20):1597–1604. doi:10.1001/jama.277.20.1597
Hugenholtz H (2003) Methylprednisolone for acute spinal cord injury: not a standard of care. CMAJ 168(9):1145–1146
Pettiford JN, Bikhchandani J, Ostlie DJ, St Peter SD, Sharp RJ, Juang D (2012) A review: the role of high dose methylprednisolone in spinal cord trauma in children. Pediatr Surg Int 28(3):287–294. doi:10.1007/s00383-011-3012-3
Acknowledgements
This study was supported by the National Natural Science Foundation of China (81671202) and the National Natural Science Foundation of China (81271556).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This work was approved by the local ethics board of our institution.
Conflict of interest
None.
Ethical approval
For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Ren, J., Zeng, G., Ma, Yj. et al. Pediatric thoracic SCIWORA after back bend during dance practice: a retrospective case series and analysis of trauma mechanisms. Childs Nerv Syst 33, 1191–1198 (2017). https://doi.org/10.1007/s00381-017-3407-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-017-3407-0