Abstract
Purpose
To develop practical nomograms for predicting the stone-free rate after shock wave lithotripsy (SWL) in patients with a solitary stone in the proximal ureter.
Methods
Between July 2006 and June 2015, 319 patients with a proximal ureteral stone who underwent preoperative non-contrast enhanced computed tomography (NCCT) and subsequently received SWL were identified. Patients’ age, gender, laterality, stone size, mean and maximum Hounsfield Unit (HU) of the stone, and skin-to-stone distance (SSD) were assessed. The stone-free status was defined as no radiopacity detected on the 3-month follow-up plain radiography or NCCT.
Results
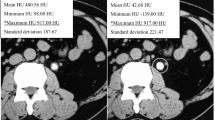
Mean stone size was 10 mm (range 3–20 mm). Mean and maximum HU of the stone ranged from 115 to 1447 (mean 701) and from 265 to 1881 (mean 1062), respectively. The overall stone-free rate was 70%. Multivariate analyses identified stone size (p < 0.001), maximum HU (p < 0.001), and SSD at 90° (p = 0.038) as independent predictive factors for the stone-free status after SWL. Nomograms could be constructed for predicting the probability of stone-free status after SWL corresponding to SSD of 8, 10, and 12 cm using maximum HU and stone size.
Conclusions
This study demonstrated that stone size, maximum HU of the stone, and SSD at 90° are significant predictors of successful SWL outcome in patients with a proximal ureteral stone. We have developed simple and practical nomograms corresponding to three different SSDs for predicting the stone-free rate after SWL.



Similar content being viewed by others
References
Chaussy C, Brendel W, Schmiedt E (1980) Extracorporeally induced destruction of kidney stones by shock waves. Lancet 316:1265–1268. doi:10.1016/S0140-6736(80)92335-1
el-Damanhoury H, Scharfe T, Ruth J et al (1991) Extracorporeal shock wave lithotripsy of urinary calculi: experience in treatment of 3278 patients using the Siemens Lithostar and Lithostar Plus. J Urol 145:484–488
Psihramis KE, Jewett MA, Bombardier C et al (1992) Lithostar extracorporeal shock wave lithotripsy: the first 1000 patients. Toronto Lithotripsy Associates. J Urol 147:1006–1009
Mobley TB, Myers DA, Grine WB et al (1993) Low energy lithotripsy with the Lithostar: treatment results with 19,962 renal and ureteral calculi. J Urol 149:1419–1424
Mobley TB, Myers DA, Jenkins JM et al (1994) Effects of stents on lithotripsy of ureteral calculi: treatment results with 18,825 calculi using the Lithostar lithotriptor. J Urol 152:53–56
Assimos D, Krambeck A, Miller NL et al (2016) Surgical management of stones: American Urological Association/Endourological Society Guideline, PART I. J Urol. doi:10.1016/j.juro.2016.05.090
Turk C, Petrik A, Sarica K et al (2015) EAU Guidelines on urolithiasis. Eur Urol 69:475–482. doi:10.1159/000049803
Kanao K, Nakashima J, Nakagawa K et al (2006) Preoperative nomograms for predicting stone-free rate after extracorporeal shock wave lithotripsy. J Urol 176:1453–1457. doi:10.1016/j.juro.2006.06.089
Wiesenthal JD, Ghiculete D, Ray AA et al (2011) A clinical nomogram to predict the successful shock wave lithotripsy of renal and ureteral calculi. J Urol 186:556–562. doi:10.1016/j.juro.2011.03.109
Joseph P, Mandal a K, Singh SK et al (2002) Computerized tomography attenuation value of renal calculus: can it predict successful fragmentation of the calculus by extracorporeal shock wave lithotripsy? A preliminary study. J Urol 167:1968–1971. doi:10.1016/S0022-5347(05)65064-1
Pareek G, Hedican SP, Lee FT, Nakada SY (2005) Shock wave lithotripsy success determined by skin-to-stone distance on computed tomography. Urology 66:941–944. doi:10.1016/j.urology.2005.05.011
Shen L, Sun X, Cong X et al (2011) Comparison of efficacy of German and Chinese electromagnetic shock wave lithotripters: Dornier compact S vs Huikang MZ-SWL-V. Urology 78:1240–1243. doi:10.1016/j.urology.2011.04.061
Logarakis NF, Jewett M a, Luymes J, Honey RJ (2000) Variation in clinical outcome following shock wave lithotripsy. J Urol 163:721–725
Abe T, Akakura K, Kawaguchi M et al (2005) Outcomes of shockwave lithotripsy for upper urinary-tract stones: a large-scale study at a single institution. J Endourol 19:768–773. doi:10.1089/end.2005.19.768
Buchholz N-PN, Rhabar MH, Talati J (2002) Is measurement of stone surface area necessary for SWL treatment of nonstaghorn calculi? J Endourol 16:215–220. doi:10.1089/089277902753752151
Bandi G, Meiners RJ, Pickhardt PJ, Nakada SY (2009) Stone measurement by volumetric three-dimensional computed tomography for predicting the outcome after extracorporeal shock wave lithotripsy. BJU Int 103:524–528. doi:10.1111/j.1464-410X.2008.08069.x
Kacker R, Zhao L, Macejko A et al (2008) Radiographic parameters on noncontrast computerized tomography predictive of shock wave lithotripsy success. J Urol 179:1866–1871. doi:10.1016/j.juro.2008.01.038
Nakasato T, Morita J, Ogawa Y (2014) Evaluation of Hounsfield units as a predictive factor for the outcome of extracorporeal shock wave lithotripsy and stone composition. Urolithiasis 43:69–75. doi:10.1007/s00240-014-0712-x
Perks AE, Schuler TD, Lee J et al (2008) Stone attenuation and skin-to-stone distance on computed tomography predicts for stone fragmentation by shock wave lithotripsy. Urology 72:765–769. doi:10.1016/j.urology.2008.05.046
Marchini GS, Remer EM, Gebreselassie S et al (2013) Stone characteristics on noncontrast computed tomography: establishing definitive patterns to discriminate calcium and uric acid compositions. Urology 82:539–545. doi:10.1016/j.urology.2013.03.092
Ng CF, Siu DYW, Wong A et al (2009) Development of a scoring system from noncontrast computerized tomography measurements to improve the selection of upper ureteral stone for extracorporeal shock wave lithotripsy. J Urol 181:1151–1157. doi:10.1016/j.juro.2008.10.161
Kim JK, Ha SB, Jeon CH et al (2016) Clinical nomograms to predict stone-free rates after shock-wave lithotripsy†¯: development and internal-validation. PLoS One: 1–12. doi:10.1371/journal.pone.0149333
Park HS, Gong MK, Yoon CY et al (2016) Computed tomography-based novel prediction model for the outcome of shockwave lithotripsy in proximal ureteral stones. J Endourol XX:1–21. doi:10.1089/end.2016.0056
Salinas AS, Lorenzo-Romero J, Segura M et al (1999) Factors determining analgesic and sedative drug requirements during extracorporeal shock wave lithotripsy. Urol Int 63:92–101. doi:10.1159/000030425
Neisius A, Lipkin ME, Rassweiler JJ et al (2015) Shock wave lithotripsy: the new phoenix? World J Urol 33:213–221. doi:10.1007/s00345-014-1369-3
Author contributions
NN: Project development, Data collection, Data analysis, Manuscript writing, KM: Project development, Data collection, Data analysis, Manuscript writing, MM: Data collection, MO: Data collection, Manuscript editing, HK: Data collection, EK: Manuscript editing, AM: Manuscript editing, KM: Manuscript editing, MO: Manuscript editing, Supervision.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None declared.
Funding
There are no funding sources. There are no financial disclosures from any authors.
Human rights
This retrospective study was conducted after receiving approval from the institutional review board.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Niwa, N., Matsumoto, K., Miyahara, M. et al. Simple and practical nomograms for predicting the stone-free rate after shock wave lithotripsy in patients with a solitary upper ureteral stone. World J Urol 35, 1455–1461 (2017). https://doi.org/10.1007/s00345-017-2014-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-017-2014-8