Abstract
Background
Urinary and sexual dysfunction are recognized complications of rectal cancer surgery in men. This study compared robot-assisted total mesorectal excision (RTME) and laparoscopic total mesorectal excision (LTME) with regard to these functional outcomes.
Methods
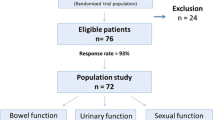
A series of 32 men who underwent RTME between February 1, 2009 and December 31, 2010 were matched 1:1 with patients who underwent LTME. The matching criteria were age, body mass index, tumor distance from the anal verge, neoadjuvant chemoradiation therapy, and tumor stage. Urinary and erectile function were evaluated using the International Prostatic Symptom Score (IPSS) and the five-item version of the International Index of Erectile Function (IIEF-5) scale. Data were collected from the two groups at baseline and at 3, 6, and 12 months after surgery and compared.
Results
The mean IPSS score did not differ between the two groups at baseline at any point of measurement. The mean baseline IIEF-5 score was similar between the two groups and was decreased at 3 months. The mean IIEF-5 score was significantly higher in the RTME group at 6 months than in the LTME group (14.1 ± 6.1 vs. 9.4 ± 6.6; p = 0.024). The interval decrease in IIEF-5 scores was significantly higher in the LTME group than in the RTME group at 6 months (4.9 ± 4.5 vs. 9.2 ± 4.7; p = 0.030).
Conclusions
The men in the RTME group experienced earlier restoration of erectile function than did those in the LTME group. Bladder function was similar during the 12 months after RTME or LTME.




Similar content being viewed by others
References
Heald RJ, Moran BJ, Ryall RD et al (1998) Rectal cancer: the Basingstoke experience of total mesorectal excision, 1978–1997. Arch Surg 133:894–899
Kapiteijn E, Putter H, van de Velde CJ (2002) Impact of the introduction and training of total mesorectal excision on recurrence and survival in rectal cancer in The Netherlands. Br J Surg 89:1142–1149
Maurer CA, Z’Graggen K, Renzulli P et al (2001) Total mesorectal excision preserves male genital function compared with conventional rectal cancer surgery. Br J Surg 88:1501–1505
Jayne DG, Brown JM, Thorpe H et al (2005) Bladder and sexual function following resection for rectal cancer in a randomized clinical trial of laparoscopic versus open technique. Br J Surg 92:1124–1132
Laurent C, Leblanc F, Wutrich P et al (2009) Laparoscopic versus open surgery for rectal cancer: long-term oncologic results. Ann Surg 250:54–61
Kang SB, Park JW, Jeong SY et al (2010) Open versus laparoscopic surgery for mid or low rectal cancer after neoadjuvant chemoradiotherapy (COREAN trial): short-term outcomes of an open-label randomised controlled trial. Lancet Oncol 11:637–645
D’Annibale A, Morpurgo E, Fiscon V et al (2004) Robotic and laparoscopic surgery for treatment of colorectal diseases. Dis Colon Rectum 47:2162–2168
Park JS, Choi GS, Lim KH et al (2010) Robotic-assisted versus laparoscopic surgery for low rectal cancer: case-matched analysis of short-term outcomes. Ann Surg Oncol 17:3195–3202
Pigazzi A, Ellenhorn JD, Ballantyne GH et al (2006) Robotic-assisted laparoscopic low anterior resection with total mesorectal excision for rectal cancer. Surg Endosc 20:1521–1525
Luca F, Valvo M, Ghezzi TL et al (2013) Impact of robotic surgery on sexual and urinary functions after fully robotic nerve-sparing total mesorectal excision for rectal cancer. Ann Surg 257:672–678
Ho VP, Lee Y, Stein SL et al (2011) Sexual function after treatment for rectal cancer: a review. Dis Colon Rectum 54:113–125
Choi HR, Chung WS, Shim BS et al (1996) Translation validity and reliability of I-PSS Korean version. Korean J Urol 37:659–665
Barry MJ, Fowler FJ Jr, O’Leary MP et al (1992) The American Urological Association symptom index for benign prostatic hyperplasia: the Measurement Committee of the American Urological Association. J Urol 148:1549–1557
Ahn TY, Lee DS, Kang WC et al (2001) Validation of an abridged Korean version of the International Index of Erectile Function (IIEF-5) as a diagnostic tool for erectile dysfunction. Korean J Urol 42:535–540
Rosen RC, Cappelleri JC, Smith MD et al (1999) Development and evaluation of an abridged, 5-item version of the International Index of Erectile Function (IIEF-5) as a diagnostic tool for erectile dysfunction. Int J Impot Res 11:319–326
Hendren SK, O’Connor BI, Liu M et al (2005) Prevalence of male and female sexual dysfunction is high following surgery for rectal cancer. Ann Surg 242:212–223
Morino M, Parini U, Allaix ME et al (2009) Male sexual and urinary function after laparoscopic total mesorectal excision. Surg Endosc 23:1233–1240
Quah HM, Jayne DG, Eu KW et al (2002) Bladder and sexual dysfunction following laparoscopically assisted and conventional open mesorectal resection for cancer. Br J Surg 89:1551–1556
Clausen N, Wolloscheck T, Konerding MA (2008) How to optimize autonomic nerve preservation in total mesorectal excision: clinical topography and morphology of pelvic nerves and fasciae. World J Surg 32:1768–1775. doi:10.1007/s00268-008-9625-6
Chang PL, Fan HA (1983) Urodynamic studies before and/or after abdominoperineal resection of the rectum for carcinoma. J Urol 130:948–951
Santangelo ML, Romano G, Sassaroli C (1987) Sexual function after resection for rectal cancer. Am J Surg 154:502–504
Havenga K, Enker WE, McDermott K et al (1996) Male and female sexual and urinary function after total mesorectal excision with autonomic nerve preservation for carcinoma of the rectum. J Am Coll Surg 182:495–502
Enker WE, Havenga K, Polyak T et al (1997) Abdominoperineal resection via total mesorectal excision and autonomic nerve preservation for low rectal cancer. World J Surg 21:715–720. doi:10.1007/s002689900296
Nesbakken A, Nygaard K, Bull-Njaa T et al (2000) Bladder and sexual dysfunction after mesorectal excision for rectal cancer. Br J Surg 87:206–210
Rawlings AL, Woodland JH, Crawford DL (2006) Telerobotic surgery for right and sigmoid colectomies: 30 consecutive cases. Surg Endosc 20:1713–1718
Kim JY, Kim NK, Lee KY et al (2012) A comparative study of voiding and sexual function after total mesorectal excision with autonomic nerve preservation for rectal cancer: laparoscopic versus robotic surgery. Ann Surg Oncol 19:2485–2493
D’Annibale A, Pernazza G, Monsellato I et al (2013) Total mesorectal excision: a comparison of oncological and functional outcomes between robotic and laparoscopic surgery for rectal cancer. Surg Endosc 27:1887–1895
Keating JP (2004) Sexual function after rectal excision. ANZ J Surg 74:248–259
Lindsey I, Guy RJ, Warren BF et al (2000) Anatomy of Denonvilliers’ fascia and pelvic nerves, impotence, and implications for the colorectal surgeon. Br J Surg 87:1288–1299
Breukink SO, van Driel MF, Pierie JP et al (2008) Male sexual function and lower urinary tract symptoms after laparoscopic total mesorectal excision. Int J Colorectal Dis 23:1199–1205
Stamopoulos P, Theodoropoulos GE, Papailiou J et al (2009) Prospective evaluation of sexual function after open and laparoscopic surgery for rectal cancer. Surg Endosc 23:2665–2674
Celentano V, Fabbrocile G, Luglio G et al (2010) Prospective study of sexual dysfunction in men with rectal cancer: feasibility and results of nerve sparing surgery. Int J Colorectal Dis 25:1441–1445
Acknowledgments
This study was supported by a grant from the Korea Health Technology R&D Project, Ministry of Health & Welfare, Republic of Korea (A111345).
Conflict of interest
This study was not conducted under any commercial sponsorship or grant. Soo Yeun Park, Gyu-Seog Choi, Jun Seok Park, Hye Jin Kim, Jong-Pil Ryuk, and Sung-Hwan Yun have no conflicts of interest to report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Park, S.Y., Choi, GS., Park, J.S. et al. Urinary and Erectile Function in Men After Total Mesorectal Excision by Laparoscopic or Robot-Assisted Methods for the Treatment of Rectal Cancer: A Case-Matched Comparison. World J Surg 38, 1834–1842 (2014). https://doi.org/10.1007/s00268-013-2419-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-013-2419-5