Abstract
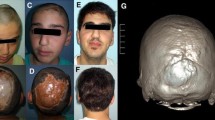
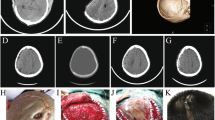
We report a case of sagittal synostosis that was detected because of cranial deformity 5 years after a congenital pigmented nevus of the scalp was resected using the tissue expansion (TE) technique. Currently, no case report describes the association between TE and craniosynostosis. To explain the mechanism of the craniosynostosis in the present case, we considered that the area of placement, number of expanders, injection schedule, age at operation, or a combination of these may have been responsible for early suture fusion. Considering that complete fusion of the sagittal suture was observed on the postoperative computed tomography but that the compensatory change of the cranial shape was relatively minor, we speculated that the changes in the patient’s skull could have been secondary (late-onset) sagittal synostosis caused by the surgery. Because the deformity in secondary craniosynostosis is relatively minor, it may be overlooked by some surgeons. We recommend careful placement of the expander and long-term follow-up, especially in infants.
Level of Evidence: Level V, risk/prognostic study.





Similar content being viewed by others
References
Radovan C (1983) Tissue expansion in soft-tissue reconstruction. Plast Reconstr Surg 74:482–490
Huang X, Qu X, Li Q (2011) Risk factors for complications of tissue expansion: a 20-year systematic review and meta-analysis. Plast Reconstr Surg 128:787–797
Calobrace MB, Downey SE (1997) Calvarial deformity and remodeling following prolonged scalp expansion in a child. Ann Plast Surg 39:186–189
El-Saadi MM, Nasr MA (2008) The effect of tissue expansion on skull bones in the paediatric age group from 2 to 7 years. J Plast Reconstr Aesthet Surg 61:413–418
Zaal LH, van der Horst CM (2009) Results of the early use of tissue expansion for giant congenital melanocytic naevi on the scalp and face. J Plast Reconstr Aesthet Surg 62:216–220
Millet-Declerck M, Calibre C, Herbaux B et al (2012) Long-term results in scalp tissue expansion in children. Eur J Pediatr Surg 22:269–273
Higginbottom MC, Jones KL, James HE (1980) Intrauterine constraint and craniosynostosis. Neurosurgery 6:39–44
Graham JM Jr, Badura RJ, Smith DW (1980) Coronal craniostenosis: fetal head constraint as one possible cause. Pediatrics 65:995–999
Oppenheimer AJ, Rhee ST, Goldstein SA et al (2009) Force-induced craniosynostosis in the murine sagittal suture. Plast Reconstr Surg 124:1840–1848
Chu KF, Sullivan SR, Taylor HO (2013) Pan-suture synostosis after posterior vault distraction. Eplasty 13:52
Colonna M, Cavallini M, de Angelis A et al (1996) The effects of scalp expansion on the cranial bone: a clinical, histological, and instrumental study. Ann Plast Surg 36:255–260
Keskin M, Kelly CP, Yavuzer R et al (2006) External filling ports in tissue expansion: confirming their safety and convenience. Plast Reconstr Surg 117:1543–51
Chung C, Forte AJ, Narayan D et al (2006) Giant nevi: a review. J Craniofac Surg 17:1210–5
Zaal LH, Mooi WJ, Sillevis Smitt JH et al (2004) Classification of congenital melanocytic naevi and malignant transformation: a review of the literature. Br J Plast Surg 57:707–19
Krengel S, Marghoob AA (2012) Current management approaches for congenital melanocytic nevi. Dermatol Clin 30:377–87
Koizumi T, Komuro Y, Hashizume K et al (2010) Cephalic index of Japanese children with normal brain development. J Craniofac Surg 21:1434–7
Conflict of interest
Takada Keiko and Tamada Ikkei declare that they have no conflict of interest.
Statement of Ethical Standards
This study was performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. The formal approval of the ethical committee in our hospital is not required for retrospective observational studies.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Keiko, T., Ikkei, T. Sagittal synostosis after excision of congenital pigmented nevus of the scalp: a possible complication of the tissue expansion technique. Eur J Plast Surg 38, 491–494 (2015). https://doi.org/10.1007/s00238-015-1099-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-015-1099-9