Abstract
Introduction and hypothesis
Treating pelvic organ prolapse (POP) with uterine conservation and sacral hysteropexy has uncertain subjective and objective outcomes. We sought to compare laparoscopic sacral hysteropexy with laparoscopic sacrocolpopexy/total laparoscopic hysterectomy (TLH with LSC).
Methods
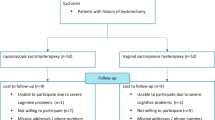
Clinical data of 34 patients who underwent TLH with LSC and 65 patients who underwent laparoscopic sacral hysteropexy performed by the same group of surgeons between January 2008 and December 2013 were reviewed retrospectively. The primary outcome was subjective satisfaction rate based upon validated questionnaire (Patient Global Impression of Change [PGI-C]). Secondary outcomes were: anatomical cure, impact on quality of life based upon validated questionnaires (pelvic floor distress inventory-short form 20 [PFDI-20], Pelvic Floor Impact Questionnaire 7 [PFIQ-7], and Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire-12 [PISQ-12]), surgical complications, and cost.
Results
After a mean follow-up of 33 months, the subjective satisfaction rate was significantly higher in the TLH with LSC cohort (92.3 % vs 100 %; p < 0.001). The POP-Q scores in both groups were significantly improved postoperatively. However, the anatomical cure in the two groups (72.3 % vs 88.2 %; p = 0.07) did not differ significantly The postoperative PFIQ-7 and PFDI-20 scores were significantly better in the TLH with LSC cohort than in the laparoscopic sacral hysteropexy cohort (p = 0.043 and p = 0.035 respectively).
Conclusions
Relative to laparoscopic sacral hysteropexy, the TLH with LSC approach provides similar anatomical results, excellent patient satisfaction, and improved quality of life scores.

Similar content being viewed by others
References
Ganatra AM, Rozet F, Sanchez-Salas R, Barret E, Galiano M, Cathelineau X, Vallancien G (2009) The current status of laparoscopic sacrocolpopexy: a review. Eur Urol 55(5):1089–1103. doi:10.1016/j.eururo.2009.01.048
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89(4):501–506. doi:10.1016/s0029-7844(97)00058-6
Denman MA, Gregory WT, Boyles SH, Smith V, Edwards SR, Clark AL (2008) Reoperation 10 years after surgically managed pelvic organ prolapse and urinary incontinence. Am J Obstet Gynecol 198(5):555. doi:10.1016/j.ajog.2008.01.051, e551-555
Antosh DD, Grotzke SA, McDonald MA, Shveiky D, Park AJ, Gutman RE, Sokol AI (2012) Short-term outcomes of robotic versus conventional laparoscopic sacral colpopexy. Female Pelvic Med Reconstr Surg 18(3):158–161. doi:10.1097/SPV.0b013e31824b218d
Nygaard IE, McCreery R, Brubaker L, Connolly A, Cundiff G, Weber AM, Zyczynski H (2004) Abdominal sacrocolpopexy: a comprehensive review. Obstet Gynecol 104(4):805–823. doi:10.1097/01.aog.0000139514.90897.07
Korbly NB, Kassis NC, Good MM, Richardson ML, Book NM, Yip S, Saguan D, Gross C, Evans J, Lopes VV, Harvie HS, Sung VW (2013) Patient preferences for uterine preservation and hysterectomy in women with pelvic organ prolapse. Am J Obstet Gynecol 209(5):470. doi:10.1016/j.ajog.2013.08.003, e471-476
Lin L, Wang P, Wang Q, Yi T (2014) Laparoscopic modified sacral hysteropexy: initial experience with an original surgical approach to uterovaginal prolapse. J Minim Invasive Gynecol 21(3):431–435. doi:10.1016/j.jmig.2013.11.008
Cundiff GW, Varner E, Visco AG, Zyczynski HM, Nager CW, Norton PA, Schaffer J, Brown MB, Brubaker L (2008) Risk factors for mesh/suture erosion following sacral colpopexy. Am J Obstet Gynecol 199(6):688. doi:10.1016/j.ajog.2008.07.029, e681–685
Leron E, Stanton SL (2001) Sacrohysteropexy with synthetic mesh for the management of uterovaginal prolapse. BJOG 108(6):629–633
Barranger E, Fritel X, Pigne A (2003) Abdominal sacrohysteropexy in young women with uterovaginal prolapse: long-term follow-up. Am J Obstet Gynecol 189(5):1245–1250
Bedford ND, Seman EI, O’Shea RT, Keirse MJ (2013) Effect of uterine preservation on outcome of laparoscopic uterosacral suspension. J Minim Invasive Gynecol 20(2):172–177. doi:10.1016/j.jmig.2012.10.014
Bump RC, Mattiasson A, Bo K, Brubaker LP, DeLancey JO, Klarskov P, Shull BL, Smith AR (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175(1):10–17
Mitropoulos D, Artibani W, Graefen M, Remzi M, Roupret M, Truss M (2013) Reporting and grading of complications after urologic surgical procedures: an ad hoc EAU guidelines panel assessment and recommendations. Actas Urol Esp 37(1):1–11. doi:10.1016/j.acuro.2012.02.002
Srikrishna S, Robinson D, Cardozo L (2010) Validation of the Patient Global Impression of Improvement (PGI-I) for urogenital prolapse. Int Urogynecol J 21(5):523–528. doi:10.1007/s00192-009-1069-5
Barber MD, Walters MD, Bump RC (2005) Short forms of two condition-specific quality-of-life questionnaires for women with pelvic floor disorders (PFDI-20 and PFIQ-7). Am J Obstet Gynecol 193(1):103–113. doi:10.1016/j.ajog.2004.12.025
Zhu L, Yu S, Xu T, Yang X, Lu Y, Li B, Lang J (2011) Chinese validation of the Pelvic Floor Impact Questionnaire Short Form. Menopause 18(9):1030–1033. doi:10.1097/gme.0b013e31820fbcbe
Zhu L, Yu S, Xu T, Yang X, Lu Y, Lang J (2012) Validation of the Chinese version of the Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire short form (PISQ-12). Int J Gynaecol Obstet 116(2):117–119. doi:10.1016/j.ijgo.2011.08.021
Cvach K, Geoffrion R, Cundiff GW (2012) Abdominal sacral hysteropexy: a pilot study comparing sacral hysteropexy to sacral colpopexy with hysterectomy. Female Pelvic Med Reconstr Surg 18(5):286–290. doi:10.1097/SPV.0b013e3182673772
Marcickiewicz J, Kjollesdal M, Engh ME, Eklind S, Axen C, Brannstrom M, Stjerndahl JH (2007) Vaginal sacrospinous colpopexy and laparoscopic sacral colpopexy for vaginal vault prolapse. Acta Obstet Gynecol Scand 86(6):733–738. doi:10.1080/00016340701332811
Maher CF, Feiner B, DeCuyper EM, Nichlos CJ, Hickey KV, O’Rourke P (2011) Laparoscopic sacral colpopexy versus total vaginal mesh for vaginal vault prolapse: a randomized trial. Am J Obstet Gynecol 204(4):360. doi:10.1016/j.ajog.2010.11.016, e361–367
Sanses TV, Shahryarinejad A, Molden S, Hoskey KA, Abbasy S, Patterson D, Saks EK, Weber Lebrun EE, Gamble TL, King VG, Nguyen AL, Abed H, Young SB (2009) Anatomic outcomes of vaginal mesh procedure (Prolift) compared with uterosacral ligament suspension and abdominal sacrocolpopexy for pelvic organ prolapse: a Fellows’ Pelvic Research Network study. Am J Obstet Gynecol 201(5):519. doi:10.1016/j.ajog.2009.07.004, e511–518
Price N, Slack A, Jackson SR (2010) Laparoscopic hysteropexy: the initial results of a uterine suspension procedure for uterovaginal prolapse. BJOG 117(1):62–68. doi:10.1111/j.1471-0528.2009.02396.x
Carramao S, Auge AP, Pacetta AM, Duarte E, Ayrosa P, Lemos NL, Aoki T (2009) A randomized comparison of two vaginal procedures for the treatment of uterine prolapse using polypropylene mesh: hysteropexy versus hysterectomy. Rev Col Bras Cir 36(1):65–72
Ren C, Zhu L, Lang JH, Shi HH (2007) Modified total pelvic floor reconstruction for repair of severe pelvic organ prolapse. Zhongguo Yi Xue Ke Xue Yuan Xue Bao 29(6):760–764
Wu JM, Wells EC, Hundley AF, Connolly A, Williams KS, Visco AG (2006) Mesh erosion in abdominal sacral colpopexy with and without concomitant hysterectomy. Am J Obstet Gynecol 194(5):1418–1422. doi:10.1016/j.ajog.2006.01.051
Tan-Kim J, Menefee SA, Luber KM, Nager CW, Lukacz ES (2011) Prevalence and risk factors for mesh erosion after laparoscopic-assisted sacrocolpopexy. Int Urogynecol J 22(2):205–212. doi:10.1007/s00192-010-1265-3
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pan, K., Cao, L., Ryan, N.A. et al. Laparoscopic sacral hysteropexy versus laparoscopic sacrocolpopexy with hysterectomy for pelvic organ prolapse. Int Urogynecol J 27, 93–101 (2016). https://doi.org/10.1007/s00192-015-2775-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-015-2775-9