Abstract
Purpose
To investigate the postoperative analgesic effect of subacromial patient-controlled analgesia (SA-PCA) with ropivacaine in comparison with intravenous patient-controlled analgesia (IV-PCA) after arthroscopic rotator cuff repair.
Methods
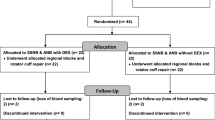
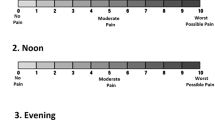
Sixty patients were prospectively randomized into one of the two types of analgesics for 48 h after the operation. In the SA-PCA group, patients received 0.5% ropivacaine at a rate of 2 ml/h with a patient-controlled bolus dose of 2 ml. In the IV-PCA group, patients received intravenous patient-controlled analgesia. Pain relief was regularly assessed using visual analog scale (VAS) for 48 h, and side effects were noted.
Results
The postoperative pain VAS at 1 h after the operation was lower for the SA-PCA group (4.3 ± 2.7) than for the IV-PCA group (6.3 ± 2.6, P = 0.009). The frequency of requested bolus doses by patients in the IV-PCA (19 ± 19) was higher than in the SA-PCA (7 ± 10, P = 0.04). Rescue opioid or NSAID requirements were not different. More patients in the IV-PCA (17/30) experienced nausea than in the SA-PCA (7/30, P = 0.03). Patient satisfaction was higher in the SA-PCA than in the IV-PCA [6.7 (3–10) vs. 5.6 (0–8), P = 0.04]. The mean total venous plasma concentration of ropivacaine at 8 and 24 h was below the maximum tolerated venous plasma concentration, and symptoms of systemic toxicity were not noted during 48 h in the SA-PCA.
Conclusions
The analgesic effect of subacromial patient-controlled analgesia with ropivacaine was better than intravenous analgesia during the immediate postoperative period with fewer side effects.
Level of evidence
Therapeutic study, Level I.

Similar content being viewed by others
References
Bang SR, Yu SK, Kim TH (2010) Can gabapentin help reduce postoperative pain in arthroscopic rotator cuff repair? A prospective, randomized, double-blind study. Arthroscopy 26(9 Suppl):S106–S111
Barber FA, Herbert MA (2002) The effectiveness of an anesthetic continuous-infusion device on postoperative pain control. Arthroscopy 18(1):76–81
Benumof JL (2000) Permanent loss of cervical spinal cord function associated with interscalene block performed under general anesthesia. Anesthesiology 93(6):1541–1544
Boss AP, Maurer T, Seiler S, Aeschbach A, Hintermann B, Strebel S (2004) Continuous subacromial bupivacaine infusion for postoperative analgesia after open acromioplasty and rotator cuff repair: preliminary results. J Should Elb Surg 13(6):630–634
Brown SL, Morrison AE (2004) Local anesthetic infusion pump systems adverse events reported to the Food and Drug Administration. Anesthesiology 100(5):1305–1307
Busfield BT, Romero DM (2009) Pain pump use after shoulder arthroscopy as a cause of glenohumeral chondrolysis. Arthroscopy 25(6):647–652
Childs SG (2002) Tension pneumothorax: a pulmonary complication secondary to regional anesthesia from brachial plexus interscalene nerve block. J Perianesth Nurs 17(6):404–410
Cho NS, Ha JH, Rhee YG (2007) Patient-controlled analgesia after arthroscopic rotator cuff repair: subacromial catheter versus intravenous injection. Am J Sports Med 35(1):75–79
Coghlan JA, Forbes A, Bell SN, Buchbinder R (2008) Efficacy and safety of a subacromial continuous ropivacaine infusion for post-operative pain management following arthroscopic rotator cuff surgery: a protocol for a randomised double-blind placebo-controlled trial. BMC Musculoskelet Disord 9:56
DeMarco JR, Componovo R, Barfield WR, Liles L, Nietert P (2011) Efficacy of augmenting a subacromial continuous-infusion pump with a preoperative interscalene block in outpatient arthroscopic shoulder surgery: a prospective, randomized, blinded, and placebo-controlled study. Arthroscopy 27(5):603–610
Dutton RP, Eckhardt WF 3rd, Sunder N (1994) Total spinal anesthesia after interscalene blockade of the brachial plexus. Anesthesiology 80(4):939–941
Eroglu A (2006) A comparison of patient-controlled subacromial and i.v. analgesia after open acromioplasty surgery. Br J Anaesth 96(4):497–501
Gomoll AH, Yanke AB, Kang RW, Chubinskaya S, Williams JM, Bach BR, Cole BJ (2009) Long-term effects of bupivacaine on cartilage in a rabbit shoulder model. Am J Sports Med 37(1):72–77
Hansen BP, Beck CL, Beck EP, Townsley RW (2007) Postarthroscopic glenohumeral chondrolysis. Am J Sports Med 35(10):1628–1634
Harvey GP, Chelly JE, AlSamsam T, Coupe K (2004) Patient-controlled ropivacaine analgesia after arthroscopic subacromial decompression. Arthroscopy 20(5):451–455
Irwin W, Fontaine E, Agnolucci L, Penzo D, Betto R, Bortolotto S, Reggiani C, Salviati G, Bernardi P (2002) Bupivacaine myotoxicity is mediated by mitochondria. J Biol Chem 277(14):12221–12227
Johnson SM, Saint John BE, Dine AP (2008) Local anesthetics as antimicrobial agents: a review. Surg Infect (Larchmt) 9(2):205–213
Knudsen K, Beckman Suurkula M, Blomberg S, Sjovall J, Edvardsson N (1997) Central nervous and cardiovascular effects of i.v. infusions of ropivacaine, bupivacaine and placebo in volunteers. Br J Anaesth 78(5):507–514
Laurila PA, Lopponen A, Kanga-Saarela T, Flinkkila T, Salomaki TE (2002) Interscalene brachial plexus block is superior to subacromial bursa block after arthroscopic shoulder surgery. Acta Anaesthesiol Scand 46(8):1031–1036
Lenters TR, Davies J, Matsen FA 3rd (2007) The types and severity of complications associated with interscalene brachial plexus block anesthesia: local and national evidence. J Should Elb Surg 16(4):379–387
Miller RD (2010) Miller’s Anesthesia, 7th edn. Churchill Livingstone, Philadelphia, pp 926–936
Nonaka I, Takagi A, Ishiura S, Nakase H, Sugita H (1983) Pathophysiology of muscle fiber necrosis induced by bupivacaine hydrochloride (Marcaine). Acta Neuropathol 60(3–4):167–174
Oh JH, Kim WS, Kim JY, Gong HS, Rhee KY (2007) Continuous intralesional infusion combined with interscalene block was effective for postoperative analgesia after arthroscopic shoulder surgery. J Should Elb Surg 16(3):295–299
Oh JH, Rhee KY, Kim SH, Lee PB, Lee JW, Lee SJ (2009) Comparison of analgesic efficacy between single interscalene block combined with a continuous intra-bursal infusion of ropivacaine and continuous interscalene block after arthroscopic rotator cuff repair. Clin Orthop Surg 1(1):48–53
Savoie FH, Field LD, Jenkins RN, Mallon WJ, Phelps RA 2nd (2000) The pain control infusion pump for postoperative pain control in shoulder surgery. Arthroscopy 16(4):339–342
Singelyn FJ, Lhotel L, Fabre B (2004) Pain relief after arthroscopic shoulder surgery: a comparison of intraarticular analgesia, suprascapular nerve block, and interscalene brachial plexus block. Anesth Analg 99(2):589–592
Webb ST, Ghosh S (2009) Intra-articular bupivacaine: potentially chondrotoxic? Br J Anaesth 102(4):439–441
Winkler T, Suda AJ, Dumitrescu RV, Pinggera O, Weber G, Loho G, Schneider B, Wurnig C (2009) Interscalene versus subacromial continuous infusion of ropivacaine after arthroscopic acromioplasty: a randomized controlled trial. J Should Elb Surg 18(4):566–572
Yang CW, Jung SM, Cho CK, Kwon HU, Kang PS, Lim YS, Oh JY, Yi JW (2010) Pleural effusion and atelectasis during continuous interscalene brachial plexus block -A case report. Korean J Anesthesiol 58(1):95–98
Yang CW, Jung SM, Kwon HU, Cho CK, Yi JW, Kim CW, Jung JK, An YM (2010) A clinical comparison of continuous interscalene brachial plexus block with different basal infusion rates of 0.2% ropivacaine for shoulder surgery. Korean J Anesthesiol 59(1):27–33
Yun MJ, Kim YH, Oh AY, Jeon YT, Kim YC (2009) Midazolam dose for loss of response to verbal stimulation during the unilateral or bilateral spinal anesthesia. Acta Anaesthesiol Scand 53(1):93–97
Zink W, Graf BM (2004) Local anesthetic myotoxicity. Reg Anesth Pain Med 29(4):333–340
Acknowledgments
The authors would like to thank Hye Ran Kim and Shang Mi Shim for their assistance with data collection.
Conflict of interest
This study is supported by grant to 04-2008-008 from the SNUBH Research Fund. There was no potential benefit to the company from this article. No product of the company was mentioned.
Ethical board review
All authors certifies that his or her institution has approved (This work was performed at Seoul National University College of medicine, Seoul National University Bundang hospital, IRB Number; B-1103/124-106) the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research.
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors, their immediate families, and any research foundations with which they are affiliated have not received any financial payments or other benefits from any commercial entity related to the subject of this article and have no potential conflicts of interest related to this manuscript.
Rights and permissions
About this article
Cite this article
Yun, M.J., Oh, J.H., Yoon, J.P. et al. Subacromial patient-controlled analgesia with ropivacaine provides effective pain control after arthroscopic rotator cuff repair. Knee Surg Sports Traumatol Arthrosc 20, 1971–1977 (2012). https://doi.org/10.1007/s00167-011-1841-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-011-1841-1