Abstract
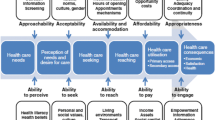
We draw upon a framework outlining household recognition and response to child illness proposed by Colvin et al. (Soc Sci Med 86:66–78, 2013) to examine factors predictive of treatment sought for a recent child illness. In particular, we model whether no treatment, middle layer treatment (traditional healer, pharmacy, community health worker, etc.), or biomedical treatment was sought for recent episodes of diarrhea, fever, or cough. Based on multinomial, multi-level analyses of Demographic and Health Surveys from 19 countries in sub-Saharan Africa, we determine that if women have no say in their own healthcare, they are unlikely to seek treatment in response to child illness. We find that women in sub-Saharan Africa need healthcare knowledge, the ability to make healthcare decisions, as well as resources to negotiate cost and travel, in order to access biomedical treatment. Past experience with medical services such as prenatal care and a skilled birth attendant also increases the odds that biomedical treatment for child illness is sought. We conclude that caregiver decision-making in response to child illness within households is critical to reducing child morbidity and mortality in sub-Saharan Africa.
Similar content being viewed by others
References
Abuya, B. A., Ciera, J., & Kimani-Murage, E. (2012). Effect of mother’s education on child’s nutritional status in the slums of Nairobi. BMC Pediatrics, 12, 80.
Adekanmbi, V. T., Kayode, G. A., & Uthman, O. A. (2011). Individual and contextual factors associated with childhood stunting in Nigeria: A multilevel analysis. Maternal & Child Nutrition, 9, 244–259.
Ahorlu, C. K., Koram, K. A., & Weiss, M. G. (2007). Children, pregnant women and the culture of malaria in two rural communities of Ghana. Anthropology and Medicine, 14, 167–181.
Alldendorf, K. (2010). The quality of family relationships and use of maternal health-care services in India. Studies in Family Planning, 41, 263–276.
Beiersmann, C., Sanou, A., Wladarsch, E., De Allegri, M., Kouyate, B., & Muller, O. (2007). Malaria in rural Burkina Faso: Local illness concepts, patterns of traditional treatment and influence on health-seeking behaviour. Malaria Journal, 6, 106.
Blum, L. S., Sharmin, T., & Ronsmans, C. (2006). Attending home vs. clinic-based deliveries: perspectives of skilled birth attendants in Matlab, Bangladesh. Reproductive Health Matters, 14, 51–60.
Chakraborty, P., & Anderson, A. K. (2011). Maternal autonomy and low birth weight in India. Journal of Women’s Health, 20, 1373–1382.
Chen, J., Xie, Z., & Liu, H. (2007). Son preference, use of maternal health care, and infant mortality in rural China, 1989–2000. Population Studies, 61, 161–183.
Cho, Y., Song, S., & Frisbie, W. P. (2005). Adverse birth outcomes among Korean Americans: The impact of nativity and social proximity to other Koreans. Population Research and Policy Review, 24, 263–282.
Chuma, J., Gilson, L., & Molyneux, C. (2007). Treatment-seeking behaviour, cost burdens and coping strategies among rural and urban households in Coastal Kenya: An equity analysis. Tropical Medicine & International Health, 12, 673–686.
Colvin, C. J., Smith, H. J., Swartz, A., Ahs, J. W., de Heer, J., Opiyo, N., et al. (2013). Understanding careseeking for child illness in sub-Saharan Africa: A systematic review and conceptual framework based on qualitative research of household recognition and response to child diarrhea, pneumonia and malaria. Social Science and Medicine, 86, 66–78.
Comoro, C., Nsimba, S. E., Warsame, M., & Tomson, G. (2003). Local understanding, perceptions and reported practices of mothers/guardians and health workers on childhood malaria in a Tanzanian district—implications for malaria control. Acta Tropica, 87, 305–313.
Deressa, W., Ali, A., & Hailemariam, D. (2008). Malaria-related health-seeking behaviour and challenges for care providers in rural Ethiopia: Implications for control. Journal of Biosocial Science, 40, 115–135.
Ellis, A. A., Winch, P., Daou, Z., Gilroy, K. E., & Swedberg, E. (2007). Home management of childhood diarrhoea in southern Mali—implications for the introduction of zinc treatment. Social Science and Medicine, 64, 701–712.
Falade, C. O., Ogundiran, M. O., Bolaji, M. O., Ajayi, I. O., Akinboye, D. O., Oladepo, O., & Adeniyi, J. D. (2005). The influence of cultural perception of causation, complications, and severity of childhood malaria on determinants of treatment and preventive pathways. International Quarterly of Community Health Education, 24, 347–363.
Finlay, J. E., Özaltin, E., & Canning, D. (2011). The association of maternal age with infant mortality, child anthropometric failure, diarrhea and anemia for first births: evidence from 55 low- and middle-income countries. BMJ Open, 2, e000226.
Frankenberg, E., Suriastini, W., & Thomas, D. (2005). Can expanding access to basic healthcare improve children’s health status? Lessons from Indonesia’s ‘Midwife in the Village’ Programme. Population Studies, 59, 5–19.
Friend-du Preez, N., Cameron, N., & Griffiths, P. (2009). Stuips, spuits and prophet ropes: The treatment of abantu childhood illnesses in urban South Africa. Social Science and Medicine, 68, 343–351.
Frost, M. B., Forste, R., & Haas, D. W. (2005). Maternal education and child nutritional status in Bolivia: Finding the links. Social Science and Medicine, 60, 395–407.
Gribble, J. N., Murray, N. J., & Menotti, E. P. (2009). Reconsidering childhood under nutrition: Can birth spacing make a difference. An analysis of the 2002–2003 El Salvador National Family Health Survey. Maternal and Child Nutrition, 5, 49–63.
Hayford, S. R. (2005). Conformity and change: Community effects on female genital cutting in Kenya. Journal of Health and Social Behavior, 46, 121–140.
Heuveline, P., & Goldman, N. (2000). A description of child illness and treatment behavior in Guatemala. Social Science and Medicine, 50, 345–364.
Hildenwall, H., Rutebemberwa, E., Nsabagasani, X., Pariyo, G., Tomson, G., & Peterson, S. (2007). Local illness concepts—implications for management of childhood pneumonia in eastern Uganda. Acta Tropica, 101, 217–224.
Kamat, V. R. (2006). “I thought it was only ordinary fever!” cultural knowledge and the micropolitics of therapy seeking for childhood febrile illness in Tanzania. Social Science and Medicine, 62, 2945–2959.
Kumar, A., & Mohanty, S. K. (2011). Socio-economic differentials in childhood immunization in India, 1992–2006. Journal of Population Research, 28, 301–324.
Malhotra, C., Malhotra, R., Østbye, T., & Subramanian, S. V. (2012). Maternal autonomy and child health care utilization in India: Results from the national family health survey. Asia-Pacific Journal of Public Health, 20, 1–13.
Martín, T. C., & Juárez, F. (1995). The impact of women’s Education on fertility in Latin America: Searching for explanations. International Family Planning Perspectives, 21(52–57), 80.
Measure DHS/ICF International. (2013). Standard Recode manual for DHS 6. Demographic and Health Surveys methodology. United States Agency for International Development (USAID).
Nsungwa-Sabiiti, J., Källander, K., Nsabagasani, X., Namusisi, K., Pariyo, G., Johansson, A., et al. (2004). Local fever illness classifications: Implications for home management of malaria strategies. Tropical Medicine & International Health, 9, 1191–1199.
Omariba, W. R., Beaujot, R., & Rajulton, F. (2007). Determinants of infant and child mortality in Kenya: An analysis controlling for frailty effects. Population Research and Policy Review, 26, 299–321.
Othero, D. M., Orago, A. S., Groenewegen, T., Kaseje, D. O., & Otengah, P. A. (2008). Home management of diarrhea among underfives in a rural community in Kenya: household perceptions and practices. East African Journal of Public Health, 5, 142–146.
Pilkington, H., Mayombo, J., Aubouy, N., & Deloron, P. (2004). Malaria, from natural to supernatural: A qualitative study of mothers’ reactions to fever (Dienga, Gabon). Journal of Epidemiology and Community Health, 58, 826–830.
Pokhrel, S. (2007). Determinants of parental reports of children’s illness: Empirical evidence from Nepal. Social Science and Medicine, 65, 1106–1117.
Sastry, N., & Burgard, S. (2011). Changes in diarrheal disease and treatment among Brazilian children from 1986 to 1996. Population Research and Policy Review, 30, 81–100.
Schellenberg, J. A., Victora, C. G., Mushi, A., de Savigny, D., Dachellenberg, D., Mshinda, H., & Bryce, J. (2003). Inequities among the very poor: Health care for children in rural southern Tanzania. Lancet, 361, 561–566.
Shah, B. D., & Dwivedi, L. K. (2011). Causes of neonatal deaths among tribal women in Gujarat, India. Population Research and Policy Review, 30, 517–536.
Sharkey, A. B., Chopra, M., Jackson, D., Winch, P. J., & Minkovitz, C. S. (2012). Pathways of care-seeking during fatal infant illnesses in under-resourced South African settings. Transactions of the Royal Society of Tropical Medicine and Hygiene, 106, 110–116.
Thind, A., & Andersen, R. (2003). Respiratory illness in the Dominical Republic: What are the predictors for health services utilization of young children? Social Science and Medicine, 56, 1173–1182.
Vikram, K., Vanneman, R., & Desai, S. (2012). Linkages between maternal education and childhood immunizations in India. Social Science and Medicine, 75, 331–339.
Westoff, C. F., & Koffman, D. A. (2011). The association of television and radio with reproductive behavior. Population and Development Review, 37, 749–759.
World Health Organization/United Nations Children’s Fund (WHO/UNICEF). (2010). Countdown to 2015 decade report (2000–2010): Taking stock of maternal, newborn and child survival. Geneva: World Health Organization.
World Health Organization/United Nations Children’s Fund (WHO/UNICEF). (2013). Ending preventable child deaths from pneumonia and diarrhoea by 2025: Executive summary. The Integrated Global Action Plan for the Prevention and Control of Pneumonia and Diarrhoea (GAPPD). Geneva: World Health Organization.
Author information
Authors and Affiliations
Corresponding author
Appendix
Rights and permissions
About this article
Cite this article
Pierce, H., Gibby, A.L. & Forste, R. Caregiver Decision-Making: Household Response to Child Illness in Sub-Saharan Africa. Popul Res Policy Rev 35, 581–597 (2016). https://doi.org/10.1007/s11113-016-9396-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11113-016-9396-y