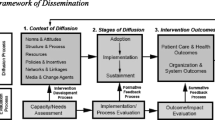
There is nothing more difficult to plan, more doubtful of success, nor more dangerous to manage than the creation of a new order of things. Machiavelli
Abstract
Listening Visits (LV), an empirically supported depression treatment delivered by non mental health specialists, were implemented into two distinctly structured programs. The relative importance of providers’ views and organizational context on implementation were examined. Thirty-seven home visitors completed pre- and post-LV training surveys assessing their views toward implementing LV. Implementation rates markedly differed in the two organizations (73.9% vs. 35.7%). Logistic regression results showed that when predicting the implementation rate, the impact of the organizational setting outweighed home visitors’ personal views. These results underscore the importance of organizational context in the implementation of empirically supported treatments.
Similar content being viewed by others
References
Beck, C. T. (1998). The effects of postpartum depression on child development: A meta-analysis. Archives of Psychiatric Nursing, 12, 12–20.
Beck, C. T. (1999). Maternal depression and child behavior problems: A meta-analysis. Journal of Advanced Nursing, 29, 623–629.
Bickman, L. (2008). Improving the effectiveness of mental health services. Administration and Policy in Mental Health and Mental Health Services Research, 35, 229.
Chabrol, H., Teissedre, F., Saint-Jean, M., Teisseyre, N., Roge, B., & Mullet, E. (2002). Prevention and treatment of post-partum depression: A controlled randomized study on women at risk. Psychological Medicine, 32, 1039–1047.
Cooper, P. J., Murray, L., Wilson, A., & Romaniuk, H. (2003). Controlled trial of the short-and long-term effect of psychological treatment of post-partum depression. I. Impact on maternal mood. British Journal of Psychiatry, 182, 412–419.
Dennis, C.-L., & Chung-Lee, L. (2006). Postpartum depression help-seeking barriers and maternal treatment preferences: A qualitative systematic review. Birth, 33, 323–331.
Durlak, J. A., & DuPre, E. P. (2008). Implementation matters: A review of research on the influence of implementation on program outcomes and the factors affecting implementation. American Journal of Community Psychology, 41, 327–350.
Field, T. (2010). Postpartum depression effects on early interactions, parenting, and safety practices: A review. Infant Behavior and Development, 33, 1–6.
Gavin, N. I., Gaynes, B. N., Lohr, K. N., Meltzer-Brody, S., Gartlehner, G., & Swinson, T. (2005). Perinatal depression: A systematic review of prevalence and incidence. Obstetrics and Gynecology, 106, 1071–1083.
Glaser, E. M. (1973). Knowledge transfer and institutional change. Professional Psychology, 4, 434–444.
Glisson, C. (2002). The organizational context of children’s mental health services. Clinical Child and Family Psychology Review, 5, 233–253.
Glisson, C., & Schoenwald, S. K. (2005). The ARC organizational and community intervention strategy for implementing evidence-based children’s mental health treatments. Mental Health Services Research, 7, 243–259.
Goodman, J. (2009). Women’s attitudes, preferences, and perceived barriers to treatment for perinatal depression. Birth, 36, 60–69.
Goodman, S. H., & Gotlib, I. H. (1999). Risk for psychopathology in the children of depressed mothers: A developmental model for understanding mechanisms of transmission. Psychological Review, 106, 458–490.
Gotham, H. J. (2004). Diffusion of mental health and substance abuse treatments: Development, dissemination, and implementation. Clinical Psychology: Science and Practice, 11, 160–176.
Grote, N. K., Bridge, J. A., Gavin, A. R., Melville, J. L., Iyengar, S., & Katon, W. J. (2010). A meta-analysis of depression during pregnancy and the risk of preterm birth, low birth weight, and intrauterine growth restriction. Archives of General Psychiatry, 67, 1012–1024.
Holden, J. M., Sagovsky, R., & Cox, J. L. (1989). Counselling in a general practice setting: Controlled study of health visitor intervention in treatment of postnatal depression. British Medical Journal, 298, 223–226.
Insel, T. (2008). National Institute of Mental Health: Strategic Plan. Retrieved January 12, 2010, from http://www.nimh.nih.gov/about/strategic-planning-reports/nimh-strategic-plan-2008.pdf.
Kelly, J. A., Somlai, A. M., DiFranceisco, W. J., Otto-Salaj, L. L., McAuliffe, T. L., Hackl, K. L., et al. (2000). Bridging the gap between the science and service of HIV prevention: Transferring effective research-based HIV prevention interventions to community AIDS service providers. American Journal of Public Health, 90, 1082–1088.
Kerner, J., Rimer, B., & Emmons, K. (2005). Dissemination research and research dissemination: How can we close the gap? Introduction to the Special Section on Dissemination. Health Psychology, 24, 443–446.
Landsverk, J., Brown, C. H., Reutz, J. R., Palinkas, L., & Horwitz, S. M. (2010). Design elements in implementation research: A structured review of child welfare and child mental health studies [Electronic Version]. Administration and Policy in Mental Health and Mental Health Services Research. Retrieved January 12, 2010, from http://www.springerlink.com/content/1g43632088524w02/fulltext.pdf.
Leis, J. A., Mendelson, T., Tandon, S. D., & Perry, D. F. (2009). A systematic review of home-based interventions to prevent and treat postpartum depression. Archives of Women’s Mental Health, 12, 3–13.
Levy, L. B., & O’Hara, M. W. (2010). Psychotherapeutic interventions for depressed, low-income women: A review of the literature [Electronic Version]. Clinical Psychology Review. doi:10.1016/j.cpr.2010.06.006.
Martins, C., & Gaffan, E. A. (2000). Effects of early maternal depression on patterns of infant-mother attachment: A meta-analytic investigation. Journal of Child Psychology and Psychiatry, 41, 737–746.
McCarthy, M., & McMahon, C. (2008). Acceptance and experience of treatment for postnatal depression in a community mental health setting. Health Care for Women International, 29, 618–637.
Mendel, P., Meredith, L. S., Schoenbaum, M., Sherbourne, C. D., & Wells, K. B. (2008). Interventions in organizational and community context: A framework for building evidence on dissemination and implementation in health services research. Administration and Policy in Mental Health and Mental Health Services Research, 35, 21–37.
Morrell, C. J., Slade, P., Warner, R., Paley, G., Dixon, S., Walters, S. J., et al. (2009). Clinical effectiveness of health visitor training in psychologically informed approaches for depression in postnatal women: Pragmatic cluster randomised trial in primary care [Electronic Version]. British Medical Journal, 338, a3045. doi:10.1136/bmj.a3045.
Murray, L., Sinclair, D., Cooper, P., Ducournau, P., Turner, P., & Stein, A. (1999). The socioemotional development of 5-year-old children of postnatally depressed mothers. Journal Child Psychology and Psychiatry, 40, 1259–1271.
Nadeem, E., Lange, J. M., Edge, D., Fongwa, M., Belin, T. D., & Miranda, J. (2007). Does stigma keep poor young immigrant and U.S.-born Black and Latina women from seeking mental health care? Psychiatric Services, 58, 1547–1554.
O’Hara, M. W., Stuart, S., Gorman, L. L., & Wenzel, A. (2000). Efficacy of Interpersonal Psychotherapy for postpartum depression. Archives of General Psychiatry, 57, 1039–1045.
Schoenwald, S. K. (2008). Toward evidence-based transport of evidenced-based treatments: MST as an example. Journal of Child and Adolescent Substance Abuse, 17, 69–91.
Schoenwald, S. K., Kelleher, K., Weisz, J. R., & The Research Network on Youth Mental Health. (2008). Building bridges to evidence-based practice: The MacArthur Foundation Child System and Treatment Enhancement Projects (Child STEPS). Administration and Policy in Mental Health and Mental Health Services Research, 35, 66–72.
Segre, L. S., O’Hara, M. W., Arndt, S., & Stuart, S. (2007). The prevalence of postpartum depression: The relative significance of three social status indices. Social Psychiatry and Psychiatric Epidemiology, 42, 316–321.
Segre, L. S., Stasik, S. M., O’Hara, M. W., & Arndt, S. (2010). Listening Visits: An evaluation of the effectiveness and acceptability of a home-based depression treatment. Psychotherapy Research, 20, 712–721.
Song, D., Sands, R. G., & Wong, Y.-L. I. (2004). Utilization of mental health services by low-income pregnant and postpartum women on medical assistance. Women and Health, 39, 1–24.
Sword, W., Busser, D., Ganann, R., McMillan, T., & Swinton, M. (2008). Women’s care-seeking experiences after referral for postpartum depression. Qualitative Health Research, 18, 1161–1173.
Watt, S., Sword, W., Krueger, P., & Sheehan, D. (2002). A cross-sectional study of early identification of postpartum depression: Implications for primary care providers from The Ontario Mother & Infant Survey [Electronic Version]. BMC Family Practice. doi:10.1186/1471-2296-3-5.
Wickberg, B., & Hwang, C. P. (1996). Counselling of postnatal depression: A controlled study on a population based Swedish sample. Journal of Affective Disorders, 39, 209–216.
Zazzali, J. L., Sherbourne, C., Hoagwoad, K. E., Greene, D., Bigley, M. F., & Sexton, T. L. (2008). The adoption and implementation of an evidenced based practice in child and family mental health services organizations: A pilot study of Functional Family Therapy in New York State. Administration and Policy in Mental Health and Mental Health Services Research, 35, 38–49.
Acknowledgments
The authors would like to acknowledge the contribution of the staff of Visiting Nurse Services in the conduct of this research, including the VNS Chief Executive Officer, Dr. Jennifer Van Liew, the directors of Healthy Start and Maternal Child Health, Ms. Darby Taylor and Ms. Cari Spear, as well as the home visitors from both programs.
Disclosure
No competing financial interests exist.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Segre, L.S., McCabe, J.E., Stasik, S.M. et al. Implementation of an Evidence-Based Depression Treatment Into Social Service Settings: The Relative Importance of Acceptability and Contextual Factors. Adm Policy Ment Health 39, 180–186 (2012). https://doi.org/10.1007/s10488-011-0345-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10488-011-0345-0