Abstract
Background
Sentinel node biopsy (SNB) for cN0 early squamous cell carcinoma (SCC) of the oral cavity has been validated by numerous studies. Around 30% of SNB will detect occult disease. Several clinical and morphological features of the primary tumor have been claimed to be predictive for occult metastasis in elective neck dissections. The aim of this study was to assess these factors in the context of SNB.
Methods
Seventy-eight patients undergoing SNB for T1/2 oral SCC from the years 2000 to 2007 were prospectively included. Primary tumors were reviewed for the following morphological and clinical parameters: grade of differentiation, tumor depth, tumor thickness, perineural invasion, lymphatic invasion, vascular invasion, muscle invasion, lymphoplasmacytic infiltration, and mode of invasion, age, gender, primary tumor site, tumor side, and cT category.
Results
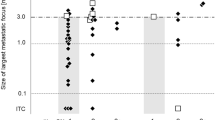
Statistical analysis revealed significance to predict occult metastasis in the SNB for grade of differentiation (P = 0.002), lymphatic invasion (P < 0.001), and mode of invasion (P < 0.001). None of the other factors reached significance. The mean tumor depth was 6.45 mm (range 0.72–15.15 mm) and the mean tumor thickness was 7.2 mm (range 0.72–15.15 mm). None of the cutoff values reached significance for predicting occult disease.
Conclusions
Tumor depth and tumor thickness failed to achieve statistical significance for prediction of occult metastases in the context of SNB. Patients with cN0 early squamous cell carcinoma of the oral cavity should be offered SNB regardless of their tumor depth and thickness. Poorly differentiated carcinomas, carcinomas with lymphangiosis, and carcinomas with a dissolute mode of invasion show a high probability of positive SNB.





Similar content being viewed by others
References
Kalnins IK, Leonard AG, Sako K, Razack MS, Shedd DP. Correlation between prognosis and degree of lymph node involvement in carcinoma of the oral cavity. Am J Surg. 1977;134(4):450–4.
Barrs DM, DeSanto LW, O’Fallon WM. Squamous cell carcinoma of the tonsil and tongue-base region. Arch Otolaryngol. 1979;105(8):479–85.
Callery CD, Spiro RH, Strong EW. Changing trends in the management of squamous carcinoma of the tongue. Am J Surg. 1984;148(4):449–54.
Grandi C, Alloisio M, Moglia D, Podrecca S, Sala L, Salvatori P, Molinari R. Prognostic significance of lymphatic spread in head and neck carcinomas: therapeutic implications. Head Neck Surg. 1985;8(2):67–73.
Byers RM, Wolf PF, Ballantyne AJ. Rationale for elective modified neck dissection. Head Neck Surg. 1988;10(3):160–7.
van den Brekel MW, van der Waal I, Meijer CJ, Freeman JL, Castelijns JA, Snow GB. The incidence of micrometastases in neck dissection specimens obtained from elective neck dissections. Laryngoscope. 1996;106(8):987–91.
Krag DN, Weaver DL, Alex JC, Fairbank JT. Surgical resection and radiolocalization of the sentinel lymph node in breast cancer using a gamma probe. Surg Oncol. 1993;2(6):335–9.
Morton DL, Wen DR, Wong JH, Economou JS, Cagle LA, Storm FK, et al. Technical details of intraoperative lymphatic mapping for early stage melanoma. Arch Surg. 1992;127(4):392–9.
Stoeckli SJ. Sentinel node biopsy for oral and oropharyngeal squamous cell carcinoma of the head and neck. Laryngoscope. 2007;117(9):1539–51.
Shoaib T, Soutar DS, Prosser JE, Dunaway DJ, Gray HW, McCurrach GM, et al. A suggested method for sentinel node biopsy in squamous cell carcinoma of the head and neck. Head Neck. 1999;21(8):728–33.
Ross GL, Shoaib T, Soutar DS, MacDonald DG, Camilleri IG, Bessent RG, et al. The First International Conference on Sentinel Node Biopsy in Mucosal Head and Neck Cancer and adoption of a multicenter trial protocol. Ann Surg Oncol. 2002;9(4):406–10.
Greene FL, Page DL, Fleming ID, Fritz AG, Balch CM, Haller DG, et al. AJCC cancer staging handbook, 6th ed. New York: Springer; 2002.
Stoeckli SJ, Steinert H, Pfaltz M, Schmid S. Sentinel lymph node evaluation in squamous cell carcinoma of the head and neck. Otolaryngol Head Neck Surg. 2001;125(3):221–6.
Ambrosch P, Kron M, Fischer G, Brinck U. Micrometastases in carcinoma of the upper aerodigestive tract: detection, risk of metastasizing, and prognostic value of depth of invasion. Head Neck. 1995;17(6):473–9.
Kane SV, Gupta M, Kakade AC, D’ Cruz A. Depth of invasion is the most significant histological predictor of subclinical cervical lymph node metastasis in early squamous carcinomas of the oral cavity. Eur J Surg Oncol. 2006;32(7):795–803.
Shingaki S, Suzuki I, Nakajima T, Kawasaki T. Evaluation of histopathologic parameters in predicting cervical lymph node metastasis of oral and oropharyngeal carcinomas. Oral Surg Oral Med Oral Pathol. 1988;66(6):683–8.
Pimenta Amaral TM, Da Silva Freire AR, Carvalho AL, Pinto CA, Kowalski LP. Predictive factors of occult metastasis and prognosis of clinical stages I and II squamous cell carcinoma of the tongue and floor of the mouth. Oral Oncol. 2004;40(8):780–6.
Brandwein-Gensler M, Teixeira MS, Lewis CM, Lee B, Rolnitzky L, Hille JJ, et al. Oral squamous cell carcinoma: histologic risk assessment, but not margin status, is strongly predictive of local disease-free and overall survival. Am J Surg Pathol. 2005;29(2):167–78.
Yamamoto E, Miyakawa A, Kohama G. Mode of invasion and lymph node metastasis in squamous cell carcinoma of the oral cavity. Head Neck Surg. 1984;6(5):938–47.
Kurokawa H, Zhang M, Matsumoto S, Yamashita Y, Tomoyose T, Tanaka T, et al. The high prognostic value of the histologic grade at the deep invasive front of tongue squamous cell carcinoma. J Oral Pathol Med. 2005;34(6):329–33.
Kurokawa H, Yamashita Y, Takeda S, Zhang M, Fukuyama H, Takahashi T. Risk factors for late cervical lymph node metastases in patients with stage I or II carcinoma of the tongue. Head Neck. 2002;24(8):731–6.
Woolgar JA, Scott J. Prediction of cervical lymph node metastasis in squamous cell carcinoma of the tongue/floor of mouth. Head Neck. 1995;17(6):463–72.
Lim SC, Zhang S, Ishii G, Endoh Y, Kodama K, Miyamoto S, et al. Predictive markers for late cervical metastasis in stage I and II invasive squamous cell carcinoma of the oral tongue. Clin Cancer Res. 2004;10(1 Pt 1):166–72.
Brown B, Barnes L, Mazariegos J, Taylor F, Johnson J, Wagner RL. Prognostic factors in mobile tongue and floor of mouth carcinoma. Cancer. 1989;64(6):1195–202.
Fukano H, Matsuura H, Hasegawa Y, Nakamura S. Depth of invasion as a predictive factor for cervical lymph node metastasis in tongue carcinoma. Head Neck. 1997;19(3):205–10.
Okamoto M, Nishimine M, Kishi M, Kirita T, Sugimura M, Nakamura M, et al. Prediction of delayed neck metastasis in patients with stage I/II squamous cell carcinoma of the tongue. J Oral Pathol Med. 2002;31(4):227–33.
Po Wing Yuen A, Lam KY, Lam LK, Ho CM, Wong A, Chow TL, et al. Prognostic factors of clinically stage I and II oral tongue carcinoma-A comparative study of stage, thickness, shape, growth pattern, invasive front malignancy grading, Martinez-Gimeno score, and pathologic features. Head Neck. 2002;24(6):513–20.
Mohit-Tabatabai MA, Sobel HJ, Rush BF, Mashberg A. Relation of thickness of floor of mouth stage I and II cancers to regional metastasis. Am J Surg. 1986;152(4):351–3.
Sparano A, Weinstein G, Chalian A, Yodul M, Weber R. Multivariate predictors of occult neck metastasis in early oral tongue cancer. Otolaryngol Head Neck Surg. 2004;131(4):472–6.
Warburton G, Nikitakis NG, Roberson P, Marinos NJ, Wu T, Sauk JJ Jr, et al. Histopathological and lymphangiogenic parameters in relation to lymph node metastasis in early stage oral squamous cell carcinoma. J Oral Maxillofac Surg. 2007;65(3):475–84.
Asakage T, Yokose T, Mukai K, Tsugane S, Tsubono Y, Asai M, Ebihara S. Tumor thickness predicts cervical metastasis in patients with stage I/II carcinoma of the tongue. Cancer. 1998;82(8):1443–8.
Spiro RH, Huvos AG, Wong GY, Spiro JD, Gnecco CA, Strong EW. Predictive value of tumor thickness in squamous carcinoma confined to the tongue and floor of the mouth. Am J Surg. 1986;152(4):345–50.
Martínez-Gimeno C, Rodríguez EM, Vila CN, Varela CL. Squamous cell carcinoma of the oral cavity: a clinicopathologic scoring system for evaluating risk of cervical lymph node metastasis. Laryngoscope. 1995;105(71):728–33.
Wenzel S, Sagowski C, Kehrl W, Metternich FU. Retrospective analysis of the prognostic significance of depth of invasion of advanced oral and oropharyngeal squamous cell carcinomas with lymph node metastases. HNO. 2004;52(7):604–10.
Morton RP, Ferguson CM, Lambie NK, Whitlock RM. Tumor thickness in early tongue cancer. Arch Otolaryngol Head Neck Surg. 1994;120(7):717–20.
Lopes MA, Nikitakis NG, Reynolds MA, Ord RA, Sauk J Jr. Biomarkers predictive of lymph node metastases in oral squamous cell carcinoma. J Oral Maxillofac Surg. 2002;60(2):142–7.
Byers RM, El-Naggar AK, Lee YY, Rao B, Fornage B, Terry NH, et al. Can we detect or predict the presence of occult nodal metastases in patients with squamous carcinoma of the oral tongue? Head Neck. 1998;20(2):138–44.
Chen RB, Suzuki K, Nomura T, Nakajima T. Flow cytometric analysis of squamous cell carcinomas of the oral cavity in relation to lymph node metastasis. J Oral Maxillofac Surg. 1993;51(4):397–401.
Osaki T, Hirota J, Yoneda K, Yamamoto T, Ueta E. Clinical and histopathologic characteristics of tongue and gingiva carcinomas with occult and clinically evident cervical lymph-node metastasis. Int J Oral Maxillofac Surg. 1996;25(4):274–8.
Nagata T, Schmelzeisen R, Mattern D, Schwarzer G, Ohishi M. Application of fuzzy inference to European patients to predict cervical lymph node metastasis in carcinoma of the tongue. Int J Oral Maxillofac Surg. 2005;34(2):138–42.
Okamoto M, Ozeki S, Watanabe T, Iida Y, Tashiro H. Cervical lymph node metastasis in carcinoma of the tongue Correlation between clinical and histopathological findings and metastasis. J Craniomaxillofac Surg. 1988;16(1):31–4.
Kowalski LP, Bagietto R, Lara JR, Santos RL, Tagawa EK, Santos IR. Factors influencing contralateral lymph node metastasis from oral carcinoma. Head Neck. 1999;21(2):104–10.
Odell EW, Jani P, Sherriff M, Ahluwalia SM, Hibbert J, Levison DA, et al. The prognostic value of individual histologic grading parameters in small lingual squamous cell carcinomas. The importance of the pattern of invasion. Cancer. 1994;74(3):789–94.
Noone RB, Bonner H Jr, Raymond S, Brown AS, Graham WP III, Lehr HB. Lymph node metastases in oral carcinoma. A correlation of histopathology with survival. Plast Reconstr Surg. 1974;53(2):158–66.
Ambrosch P, Brinck U. Detection of nodal micrometastases in head and neck cancer by serial sectioning and immunostaining. Oncology (Williston Park). 1996;10(8):1221–6.
Hermanek P, Hutter RV, Sobin LH, Wittekind C. International Union Against Cancer Classification of isolated tumor cells and micrometastasis. Cancer. 1999;86(12):2668–73.
Bilde A, von Buchwald C, Therkildsen MH, Mortensen J, Kirkegaard J, Charabi B, et al. Need for intensive histopathologic analysis to determine lymph node metastases when using sentinel node biopsy in oral cancer. Laryngoscope. 2008;118(3):408–14.
Alkureishi LW, Ross GL, Shoaib T, Soutar DS, Robertson AG, Sorensen JA, et al. Does tumor depth affect nodal upstaging in squamous cell carcinoma of the head and neck? Laryngoscope. 2008;118(4):629–34.
Acknowledgment
We are grateful to Norbert Wey for technical support and to Marianne Tinguely, MD for the review of the histological specimens.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Goerkem, M., Braun, J. & Stoeckli, S.J. Evaluation of Clinical and Histomorphological Parameters as Potential Predictors of Occult Metastases in Sentinel Lymph Nodes of Early Squamous Cell Carcinoma of the Oral Cavity. Ann Surg Oncol 17, 527–535 (2010). https://doi.org/10.1245/s10434-009-0755-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-009-0755-3