Abstract
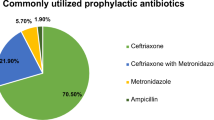
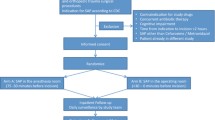
Objective:a prospective multicentre study was conducted to assess major aspects of surgical prophylaxis and to determine whether inappropriate antimicrobial prophylaxis was a factor associated (risk or protective factor) with surgical site infection (SSI). Method: surgical prophylaxis practices were assessed by analysing four variables: indication, antimicrobial agent, timing and duration. Univariate and multivariate analyses were carried out to identify predictors of SSI among patient-specific, operation-specific and antimicrobial prophylaxis-specific factors.Results: The frequency of SSI was 2.7% (13 SSI in 474 observations). Total compliance of the prescription with guidelines was observed in 41.1% of cases (195 prescriptions). Of the 139 patients who received an inappropriate drug, 126 (90.6%) received a drug with a broader spectrum than the recommended drug. Prophylaxis was prolonged in 71 (87.7%) of the 81 patients who received prophylaxis for inappropriate lengths of time and 43 (61.4%) of the 70 patients who did not receive prophylaxis at the optimal moment were treated too late. Multivariate analysis clearly demonstrated that SSI was associated with multiple procedures (relative risk 8.5), short duration of prophylaxis (relative risk 12.7) and long-term therapy with antimicrobial agents during the previous year (relative risk 8.8).Conclusions: the ecological risk of the emergence of resistance associated with the frequent use of broad-spectrum antibiotics and prophylaxis for longer periods was not offset by individual benefit to the patients who received inappropriate prophylaxis.
Similar content being viewed by others
References
Haley RW, Culver DH, White JW, Emori TG. The national nosocomial infection rate. A new need for vital statistics. Am J Epidemiol 1985,121:159–67
Pittet D, Ducel G. Infectious risk factors related to operating rooms. Infect Control Hosp Epidemiol 1994,15:456–62
McGowan JE Jr. Cost and benefit of perioperative antimicrobial prophylaxis: methods for economic analysis. Rev Infect Dis 1991,13(suppl 10):S879–S889
Arjona MF, Cabrera RH, Gomez-Sancha F, Nieto S, Calero JR. Economical saving due to prophylaxis in the prevention of surgical wound infection. Eur J Epidemiol 1996,12:455–9.
Kernodle DS, Kaiser AB. Postoperative infections and antimicrobial prophylaxis. In: Mandell GL, Bennett JE, Dolin R, eds. Principles and practice of infectious diseases. 4th ed. New York, NY: Churchill Livingstone, 1995,2742–56
Burke JF. The effective period of preventive antibiotic action in experimental incisions and dermal lesions. Surgery 1961,50:161–8
Martin C, Pourriat JL. Quality of postoperative antibiotic administration by French anaesthetists. J Hosp Infect 1998,40:47–53
Keat AS. The ASA classification of physical status: a recapitulation. Anesthesiology 1978,49:233–6
Haley RW, Culver DH, Morgan WM, White JW, Emori TG, Hooton TM. Identifying patients at high risk of surgical wound infection. A simple multivariate index of patient susceptibility and wound contamination. Am J Epidemiol 1985,121:206–15.
Culver DH, Horan TC, Gaynes RP, Martone WJ, Jarvis WR, Emori TG et al. Surgical wound infection rates by wound class, operative procedure, and patient risk index. National Nosocomial Infections Surveillance System. Am J Med 1991,91 (Suppl 3B):152S–7S.
Horan TC, Gaynes RP, Martone WJ, Jarvis WR, Emori TG. Centers for Diseases Control (CDC) definitions for nosocomial surgical site infections, 1992: a modification of CDC definitions of surgical wound infections. Infect Control Hosp Epidemiol 1992,13:606–8.
Martin C. Antimicrobial prophylaxis in surgery: general concepts and clinical guidelines. Infect Control Hosp Epidemiol 1994,15:463–71.
Gorbach SL, Condon RE, Conte JE, Kaiser AB, Ledger WJ, Nichols RL. Evaluation of new anti-infective drugs for prophylaxis of surgical infections. Clin Infect Dis 1992,15 (Suppl. 1): S313–S338.
Finkelstein R, Reinhertz G, Embom A. Surveillance of the use of antibiotic prophylaxis in surgery. Isr J Med Sci 1996,32:1093–97.
Kager L, Ljungdahl I, Malmborg AS, Nord CE, Pieper R, Dahlgren P. Antibiotic prophylaxis with cefoxitin in colorectal surgery: effect on the colon micriflora and septic complications-a clinical model for prediction of the benefit and risks in using a new antibiotic in prophylaxis. Ann Surg 1981,193:277–82.
Maki DG, Bohn MJ, Stolz SM, Kroncke GM, Archer CW, Myerowitz PD. Comparative study of cefazolin, cefamandole, and vancomycin for surgical prophylaxis in cardiac and vascular operations. A double-blind randomised trial. J Thorac Cardiovasc Surg 1992,104:1423–34.
Archer GL, Armstrong BC. Alteration of staphylococcal flora in cardiac surgery patients receiving antibiotic prophylaxis. J Infect Dis 1983,147:642–9.
Kernodle DS, Barg NL, Kaiser AB. Low-level colonization of hospitalized patients with methicillin-resistant coagulasenegative staphylococci and emergence of the organisms during surgical antimicrobial prophylaxis. Antimicrob Agents Chemother 1988,32:202–8.
Ignelzi RJ, Vanderark GD. Analysis of the treatment of basilar skull fractures with and without antibiotics. J Neurosurg 1975,43:721–6.
Fukatsu K, Saito H, Matsuda T, Ikeda S, Furukawa S, Muto T. Influences of type and duration of antimicrobial prophylaxis on an outbreak of methicillin-resistant Staphylococcus aureus and on the incidence of wound infection. Arch Surg 1997,132:1320–5.
Vaisbrud V, Raveh D, Schlesinger Y, Yinnon A. Surveillance of antimicrobial prophylaxis for surgical procedures. Infect Control Hosp Epidemiol 1999,20:610–3.
Ehrenkranz NJ. Antimicrobial prophylaxis in surgery: mechanisms, misconceptions, and mischief. Infect Control Hosp Epidemiol 1993,14:99–106.
Maki DG, Schuna AA. A study of antimicrobial misuse in a university hospital. Am J Med Sci 1978,275:271–82.
Montravers P. The economic impact of inadequate prescriptions. Ann Fr Anesth Reanim 2000,19:388–94.
Parret T, Schneider R, Rime B, Saghafi L, Pannatier A, Francioli P. Evaluation of antibiotic use: a prospective study in a university hospital center. Schweiz Med Wochenschr 1993,123:402–13.
Dellinger EP, Gross PA, Barrett TL, Krause PJ, Martone WJ, McGowan JE Jr, et al. Quality standard for antimicrobial prophylaxis in surgical procedures. Clin Infect Dis 1994,18:422–7.
Martin C, Bruguerolle B, Mallet MN, Condomines M, Sastre P, Gouin F. Pharmacokinetics and tissue penetration of a single dose of ornidazole (1000 mg) for antibiotic prophylaxis in colo-rectal surgery. Antimicrob Agents Chemother 1990,34:1921–4.
Dipiro JT, Cheung RPF, Bowden TA Jr, Mansberger JA. Single dose systemic antibiotic prophylaxis of surgical wound infections. Am J Surg 1986,152:552–9.
Taylor G, Blondel-Hill E, Kibsey P. Containing cefoxitin costs through a program to curtail use in surgical prophylaxis. Can J Infect Dis 1993,4:275–8.
Crossley K, Gardner LC. Antimicrobial prophylaxis in surgical patients. J Am Med Assoc 1981,245:722–6.
Griffiths LR, Bartzokas CA, Hampson JP, Ghose AR. Antibiotic costs and prescribing patterns in a recently commissioned Liverpool Teaching hospital. Part II: antimicrobial prophylaxis. J Hosp Infect 1986,8:168–77.
Classen DC, Evans RS, Pestotnik SL, Horn SD, Menlove RL, Burke JP. The timing of prophylactic administration of antibiotics and the risk of surgical wound infection. N Engl J Med 1992,326:281–6.
Coignard B, Siegel JD, Weinstein RA, Sohn AH, Sinkowitz-Cochran RL, Jarvis WR. Reality check: how should we control antimicrobial use? Current practices and controversies. Infect Control Hosp Epidemiol 2000,21:792–5.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Lallemand, S., Thouverez, M., Bailly, P. et al. Non-observance of guidelines for surgical antimicrobial prophylaxis and surgical-site infections. Pharm World Sci 24, 95–99 (2002). https://doi.org/10.1023/A:1016122202439
Issue Date:
DOI: https://doi.org/10.1023/A:1016122202439