Abstract
Objectives
We used quality improvement methods to implement a care bundle for children presenting to a pediatric emergency department (ED) with mental health concerns. A bundle novelty was that it included an option for assessment in a partnered clinic, not in the ED, to families of children assessed as having no medical or safety concerns. The primary aim of this study was to establish successful implementation of the bundle prior to studying its impact.
Methods
The bundle included the Ask Suicide-Screening Questions to standardize risk assessment at triage, the HEADS-ED (Home, Education, Activities/Peers, Drug/Alcohol, Suicidality, Emotions/Behavior, Discharge Resources) tool for brief, scored mental health assessments, and offering an urgent appointment within 96 h for low-risk children as an alternative to ED-based assessment or as a follow-up option for patients assessed in the ED. We developed aims, driver diagrams, and outcome measures for each bundle element. Each element was introduced with small tests of change using iterative plan-do-study-act cycles. Run charts were used to determine successful completion of aims.
Results
Rules for special cause were met through detection of shifts in performance 5 months after bundle implementation for the Ask Suicide-Screening Questions and HEADS-ED. These bundle elements were consistently used with ≥ 80% of eligible patients, representing aim achievement. During the 6 months of providing urgent appointments, 89.3% of 159 referred families received an appointment within 96 h.
Conclusions
Using quality improvement methods, we were able to successfully ensure reliable implementation of a new care bundle for pediatric patients presenting to the ED with mental health concerns and allow eligible low-risk patients to receive full assessments in a partnered clinic instead of the ED.
Résumé
Objectifs
Nous avons utilisé des méthodes d'amélioration de la qualité pour mettre en œuvre un ensemble de soins (bundle) pour les enfants qui se présentent à un service d'urgence pédiatrique avec des problèmes de santé mentale. Une nouveauté de ce bundle était qu'il comprenait une option d'évaluation dans une clinique partenaire, et non au service des urgences, pour les familles d'enfants évalués comme n'ayant aucun problème médical ou de sécurité. L'objectif premier de cette étude était d'assurer la réussite de la mise en œuvre du bundle avant d'en étudier l'impact.
Méthodes
Le bundle comprenait le questionnaire Ask Suicide-Screening Questions pour normaliser l'évaluation du risque au triage, l'outil HEADS-ED (Home, Education, Activities/Peers, Drug/Alcohol, Suicidality, Emotions/Behavior, Discharge Resources) pour des évaluations brèves et notées de la santé mentale, et l'offre d'un rendez-vous urgent dans les 96 heures pour les enfants à faible risque comme alternative à l'évaluation à l'urgence ou comme option de suivi pour les patients évalués à l'urgence. Nous avons élaboré des objectifs, des diagrammes de pilotage et des mesures de résultats pour chaque élément du bundle. Chaque élément a été introduit avec de petits tests de changement en utilisant des cycles itératifs planifier-faire-étudier-agir. Des diagrammes de progression ont été utilisés pour déterminer la réussite des objectifs.
Résultats
Les règles relatives à la cause spéciale ont été respectées grâce à la détection de changements dans les performances 5 mois après la mise en œuvre de bundle pour les questions de dépistage du suicide et HEADS-ED. Ces bundles ont été systématiquement utilisés avec plus de 80 % des patients éligibles, ce qui représente un objectif atteint. Au cours des six mois pendant lesquels des rendez-vous urgents ont été proposés, 89,3 % des 159 familles référées ont obtenu un rendez-vous dans les 96 heures.
Conclusions
En utilisant des méthodes d'amélioration de la qualité, nous avons réussi à assurer une mise en œuvre fiable d'un nouveau bundle de soin pour les patients pédiatriques se présentant aux urgences avec des problèmes de santé mentale et à permettre aux patients à faible risque éligibles de recevoir des évaluations complètes dans une clinique partenaire plutôt qu'aux urgences.
Similar content being viewed by others
What is known about the topic? |
Validated pediatric-specific tools to guide care of patients with mental health emergencies are underutilized. |
What did this study ask? |
Can a care bundle with pediatric-specific mental health tools and a referral from triage option be reliably implemented? |
What did this study find? |
Care bundle elements were implemented with high fidelity, and eligible low-risk patients were assessed in a partnered clinic outside the emergency department. |
Why does this study matter to clinicians? |
It presents an innovative model for pediatric mental health emergencies and the use of quality improvement methods to support implementation. |
Introduction
Children often access the emergency department (ED) for mental health concerns [1, 2]. During the visit, risks are identified, concerns assessed, and disposition decided. Despite the best efforts of healthcare providers, care is often inefficient, inaccessible, and not patient-centered [3]. While some EDs use pediatric-specific mental health tools to guide care, this practice is not widespread [1, 4,5,6]. Local feedback from patients and parents in Alberta suggested the need to refine mental health care to improve care efficiency, timeliness, and access to mental health providers in the ED and following discharge [7]. We designed a prospective implementation study of a mental health care bundle to improve suicide risk screening at triage, to standardized needs assessment, to provide timely follow-up visits, and to offer an option for low-risk patients to choose a scheduled appointment over remaining in the ED. For the bundle to improve patient care, ED flow, and outcomes, all bundle elements needed to be reliably implemented. Therefore, embedded in the study, was a quality improvement (QI) initiative to test and fully implement each bundle element.
The project aims were that within 6 months of bundle introduction, 80% of eligible patients would receive suicide risk screening, 80% would receive a needs assessment score, and 100% of eligible discharged patients would be offered a follow-up appointment within 96 h.
Methods
Context
The initiative took place from February to October 2021 in the Stollery Children’s Hospital, a tertiary care pediatric ED in Edmonton, Alberta, Canada with ~ 50,000 annual pediatric visits including ~ 2300 annual visits for mental health. Prior to the initiative, mental health visits began with an assessment by a triage nurse who would classify urgency into one of five acuity levels using the Canadian Triage and Acuity Scale (CTAS) score; however, score determination lacked standardized, validated questions to identify suicide risk [8]. Following triage, children were assessed by an ED mental health nurse who would provide a summary to the ED physician, who would decide on the need for a psychiatrist consultation and determine disposition. During this process, a standardized tool was not used to guide assessments and narrative summaries did not consistently assist physician decision-making. Most discharge instructions required families to organize their child’s follow-up care.
Intervention
The care bundle (Fig. 1) was developed with patient and parent partners. It includes three elements that have a strong evidence base and reflect recommendations from the American Academy of Pediatrics (AAP) and American College of Emergency Physicians [1]. Elements were introduced sequentially in 2-week intervals to allow the project team to give each change appropriate attention and give staff time to adapt. Impact on patient outcomes will be evaluated once patient-reported follow-up data have been collected (study registration # NCT04292379) [9].
Suicide risk assessment at triage
Nurses utilized the Ask Suicide-Screening Questions at triage with children ≥ 8 years presenting with one of the following chief complaints [10, 11]: anxiety, depression/suicidal, deliberate self-harm, hallucinations/delusions, homicidal behavior, ingestion, pediatric disruptive behavior, situational crisis, or violent behavior. The tool is highly sensitive for detecting immediate suicide risk in this age group [12,13,14]. If a child answered ‘yes’ to at least one of four questions about suicidality, a fifth question was asked about acuity.
Children were admitted to the ED if they answered ‘yes’ to any question or were unable/refused to answer. Families of patients who answered ‘no’ to the first four questions (negative screen), and did not have other medical or safety concerns, were met by an ED mental health nurse to discuss whether they would prefer to schedule an urgent appointment in a mental health clinic in lieu of waiting to be seen in the ED. This approach ensured that low-acuity patients would have an expedited path to assessment and avoid a lengthy ED wait.
Focused mental health assessments
We introduced the HEADS-ED tool for use by ED mental health nurses who assessed patients prior to ED physicians. The tool facilitated focused assessments with patients and guided nurse/physician decision-making for psychiatrist consultation and discharge planning [2]. The tool has excellent inter-rater agreement [16] and was originally developed to aid physician assessment [15, 16].
The tool has seven domains for assessment: Home, Education, Activities/Peers, Drug/Alcohol, Suicidality, Emotions and Behavior, Discharge Resources. Nurses assigned a score to each domain to indicate an impairment/action level: 0 (no/minimal functional impairment; no action needed), 1 (moderate functional impairment; needs action but not immediate), or 2 (severe functional impairment; needs immediate action) [17]. Total scores ≥ 8 (reflecting moderate-to-severe impairments across several domains) or a suicidality domain score of 2 (at-risk for immediate harm) were used to identify children potentially in need of psychiatry consultation. ED physicians could consult psychiatry regardless of score if deemed clinically important. Children with lower scores were deemed suitable for ED discharge with an urgent appointment offered to those without a mental health provider.
Urgent appointments
We introduced an urgent appointment within 96 h that was booked prior to the family leaving the ED. For low-risk children whose families chose an appointment over an ED visit, the appointment occurred at a mental health clinic located within the children’s hospital. For children discharged from the ED with an appointment, it occurred at the hospital-based clinic or one of two community-based clinics. Partnerships with community-based clinics were created to provide appointments and additional funding was obtained to support the hospital-based clinic.
The appointment was modeled after the Choice and Partnership Approach to care, a shared decision-making framework that focuses on prioritizing the needs and preferences of children and their caregivers [18]. Per the framework, mental health providers generated a case formulation with the child/caregiver and concluded the appointment with a joint decision on what resources/services best matched needs and goals [19].
Implementing and supporting practices
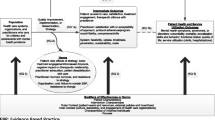
We created clinical workflows for each bundle element. Healthcare providers received element-specific training by a nurse educator and/or QI nurse. The QI nurse also used change management strategies, based on the Prosci ADKAR® model [20], including providing just-in-time, one-on-one support, and group communications (emails, posters, huddles) (Fig. 2). We developed aims (Table 1) and key driver diagrams for each bundle element [21]. We conducted a value stream mapping exercise to verify the bundle’s potential to increase efficiency, despite addition of new tools, by supporting more focused assessments and standardizing flow. Feedback was collected from healthcare providers to inform necessary modifications.
Plan-do-study-act cycles
We tested bundle implementation using iterative plan-do-study-act cycles. Initial tests of change were small (e.g. testing a change with one provider, one patient, or during one ED shift) to learn quickly if a component could be used as planned or required adjustments. Tests of change became larger in scale as learning accrued from previous cycles [22].
Measures and data collection
Outcome measures are identified in Table 1 alongside each aim. For measures related to Ask Suicide-Screening Questions and HEADS-ED, an aim of 80% of all patients with an eligible chief complaint was selected to allow for cases in which the use of the tools would not be possible (e.g. refusal, intoxication, developmental age < 8 years). Clinical data were collected from the patient’s electronic medical records.
Analysis
We used weekly run charts to determine if change was resulting in improvement. Run charts were developed according to established standards [22], and chosen over statistical process control P-charts because we preferred a simple tool that uses a median as the center line (an advantage for mitigating the effect of outliers), could detect a specific special cause (shift), and did not require special software so it could be maintained by ED staff. Since none of the bundle elements were used prior to implementation, we did not analyze pre-implementation data. The baseline median represented the initial use of the tools upon introduction and was established using the first ten data points. Non-random signals of change were identified by a shift (≥ 6 consecutive points above/below the median) [22]. Other outcome data were analyzed using descriptive statistics.
Ethical considerations
The plan-do-act cycles undertaken for this initiative were deemed QI per the University of Alberta’s Guidelines for Differentiating among Research, Program Evaluation and Quality Improvement [24]. REB approval was obtained for the implementation study.
Results
Suicide risk assessments at triage
Tests of change with individual providers began February 1, 2021 with full use of the Ask Suicide-Screening Questions beginning April 2021. A shift occurred in September 2021 with tool use occurring with 93% of eligible patients (Fig. 3). From April to October 2021, 80.3% of 1251 total mental health presentations were screened with tool. Among patients who screened negative, 20 (61.0%) of 36 families were offered an urgent appointment, with 95.0% of appointments scheduled within 96 h. Two families (9.0%) offered appointments declined and remained in the ED for an assessment. The opportunity to offer an urgent appointment was missed with 14 families (39.0%). The median time to an appointment was 11.3 h. (IQR 13.4–23.3 h.). All families attended their appointment, and no patients were redirected to the ED with safety concerns.
Focused mental health assessments
Small tests of change began in February 2021 with full HEADS-ED use beginning April 2021. A shift was noted in August 2021 with scores generated for 87% of patients (Fig. 4). From April to October 2021, 80.8% of 795 patients had scores generated on the HEADS-ED with 39.9% of 642 having a HEADS-ED score ≥ 8 (n = 152) or suicidality score of 2 (n = 104). Of these, 52.3% of the 256 received a psychiatric consultation and 47.7% received a comprehensive assessment from the nurse. Of the 386 patients with a HEADS-ED score ≤ 7 and suicidality score of 0 or 1, 21.0% received a psychiatric consultation.
Urgent appointments were offered to all (100%) 159 patients at ED discharge who did not already have a mental health provider. Of these appointments, 89.3% were booked within 96 h of the ED visit. Reasons for appointments outside of the target timeframe were family choice (n = 3) and holiday between ED visit and next appointment (n = 9); reasons were unclear for five appointments. Of the 159 appointments, 8.2% were not attended (no-show), 6.9% were canceled, and 1.9% were redirected back to the ED during their appointment due to newly emerged safety concerns (suicidal ideation with plan, unable to safety plan, agitation).
Urgent appointments
Tests of change began April 2021. Case formulations were completed for 98.5% of 132 eligible appointments, with 2 not completed due to lack of child/caregiver engagement. At appointment conclusion, 76 families expressed an interest in ongoing treatment, and all were referred.
Discussion
Interpretation
In this initiative, we used a novel approach of embedding QI methods in an implementation study to support the introduction of changes. Aims were met in the implementation of two ED-based tools, the Ask Suicide-Screening Questions and HEADS-ED. We did not achieve our aim to offer urgent appointments to all eligible low-risk patients at triage, but met our aim of offering appointments to all eligible patients at ED discharge, with almost all occurring within the 96-h target.
Previous studies
To our knowledge there are no published ED clinical pathways that combine standardized risk screening at triage with a preference-based choice for care if immediate risks are not identified. The Ask Suicide-Screening Questions has been successfully used in other EDs [25,26,27], but our use to introduce care choices to families is unique. Offering select adult medical patients a clinic visit instead of remaining in the ED has been described as safe and effective [28, 29]. The use of HEADS-ED to guide assessments and decision-making has also been studied in other EDs [16, 30, 31]. We introduced it to also support interprofessional communication between ED physicians, mental health nurses, and psychiatrists. Finally, our provision of urgent appointments allowed families to be directly connected to mental health services. Current practices in discharge of pediatric mental health patients have not been published. A study of academic EDs in the United States showed that 72% reported making appointments for patients to support discharge planning, but it was not reported how often this approach was used [32]. Modeling our urgent appointment after the Choice and Partnership Approach [18] was also unique. To date, appointments using a ‘choice approach’ have only occurred within mental health care settings [33]. Our use of this approach after the ED visit removed the burden on families to arrange care and ensured access to services.
Strengths and limitations
A key strength of this initiative was the novel use of QI to augment an implementation study. Meaningful assessment of implementation outcomes requires that the intervention be successfully adopted. Typically, implementation study interventions are fully designed prior to introduction, whereas QI begins with small tests of change with an intervention modified as learning accrues [34]. While our bundle elements were predetermined, each element was introduced with small tests of change. We believe implementing with plan-do-study-act cycles increased acceptability to staff and ensured sufficient adoption, while analyzing run charts ensured progress toward aims.
Our initiative was limited by logistical challenges. Not all eligible patients were offered a choice for care following triage. One potential reason for this may have been the infrequency of negative Ask Suicide-Screening Questions screens. As only 7% of patients (1–2 per week) screened negative, some triage nurses may have forgotten to use the option. In addition, the COVID-19 pandemic presented staffing challenges with a higher than usual proportion of casual staff present during implementation. As casual staff may be less aware of current initiatives, this may have lowered use of bundle elements. Finally, we cannot comment on bundle impact on patient-reported outcomes as this project was not designed to measure bundle effectiveness.
Clinical implications
During bundle design, reducing long ED waits was a parent partner priority. It was important to our team that urgent appointments were offered to low-risk families from triage as an alternative to remaining in the ED so families could choose what they believed to be in their child’s best interest. While this option was not utilized as frequently as anticipated, there were no adverse events associated with this aspect of the bundle, and we believe that its availability enhances family-centered care and may help alleviate ED crowding.
Research and QI implications
Bundle impact on patient-reported outcomes will be addressed in the ongoing prospective implementation study [9]. There are very few published reports on patient/family experiences with ED mental health visits and outcomes following discharge; this will be an area of immense importance in planning future improvement initiatives.
Using QI methods was an effective strategy to ensure reliable implementation of the bundle. Frequent interactions with staff, follow-up on pathway use, and ongoing education supported early success. Additionally, the use of run charts throughout implementation allowed our team to adjust strategies when initial approaches were not resulting in reaching our implementation aims.
Conclusions
Using a multi-disciplinary approach supported by QI methods, we ensured that a mental health bundle to improve screening, risk assessment, and follow-up was reliably delivered to patients presenting to the ED with mental health concerns. Pediatric-specific mental health assessment tools can be used to assess risk and offer an alternative to full ED evaluation to appropriate low-risk patients.
Data availability
Data can be made available upon reasonable request once appropriate ethics and data sharing permissions are established.
References
American Academy of Pediatrics, Committee on Pediatric Emergency Medicine; American College of Emergency Physicians, Pediatric Committee; Emergency Nurses Association Pediatric Committee. Joint policy statement-guidelines for care of children in the emergency department. Pediatrics. 2009;124(4):1233–43.
Newton AS, Hartling L, Soleimani A, Kirkland S, Dyson MP, Cappelli M. A systematic review of management strategies for children’s mental health care in the emergency department: update on evidence and recommendations for clinical practice and research. Emerg Med J. 2017;34(6):376–84.
Sheridan JS, Sheridan DC, Johnson KP, Marshall RD. Can’t we just get some help? Providing innovative care to children in acute psychiatric crisis. Health Soc Work. 2017;42(3):177–82. https://doi.org/10.1093/hsw/hlx025.
US Department of Health and Human Services, Health Resources and Services Administration, Maternal and Child Health Bureau. Critical crossroads: pediatric mental health care in the emergency department. A care pathway resource toolkit. 2019.
Leon SL, Cappelli M, Ali S, et al. The current state of mental health services in Canada’s paediatric emergency departments. Paediatr Child Health. 2013;18(2):81–5.
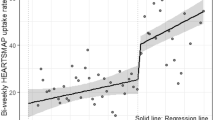
Gill C, Arnold B, Nugent S, Rajwani A, Xu M, Black T, Doan Q. Reliability of HEARTSMAP as a tool for evaluating psychosocial assessment documentation practices in emergency departments for pediatric mental health complaints. Acad Emerg Med. 2018;25(12):1375–84. https://doi.org/10.1111/acem.13506. (Epub 2018 Aug 16).
Suen V. Helping Kids & Youth in Times of Emotional Crisis: Phase 1 Final Report. Edmonton, AB: Addiction and Mental Health Strategic Clinical Network™ and Emergency Strategic Clinical Network™, Alberta Health Services, 2018. https://www.albertahealthservices.ca/assets/about/scn/ahs-scn-amh-helping-kids-and-youth-in-times-of-emotional-crisis-phase-1.pdf. Accessed Sep 12, 2022.
Bullard MJ, Unger B, Spence J, Grafstein E, CTAS National Working Group. Revisions to the Canadian Emergency Department Triage and Acuity Scale (CTAS) adult guidelines. CJEM. 2008;10(2):136–51. https://doi.org/10.1017/s1481803500009854. (English, French. Erratum in: CJEM. 2008 Jul;10(4):330).
Freedman S, Thull-Freedman J, Lightbody T, et al. Introducing an innovative model of acute paediatric mental health and addictions care to paediatric emergency departments: a protocol for a multicentre prospective cohort study. BMJ Open Quality. 2020;9: e001106. https://doi.org/10.1136/bmjoq-2020-001106.
Freedman SB, Newton AS. Screening for suicide risk—The need, the possibilities, and a call for resources. CJEM. 2020;22(3):269–70.
Grafstein E, Unger B, Bullard M, Innes G. Canadian Emergency Department Information System (CEDIS) presenting complaint list (Version 1.0). Canadian J Emerg Med. 2003;5(1):27–34. https://doi.org/10.1017/S1481803500008071.
Horowitz LM, Bridge JA, Teach SJ, Ballard E, Klima J, Rosenstein DL, et al. Ask suicide-screening questions (ASQ): a Brief instrument for the pediatric emergency department. Arch Pediatr Adolesc Med. 2012;166(12):1170–6.
Newton AS, Soleimani A, Kirkland SW, et al. A systematic review of instruments to identify mental health and substance use problems among children in the emergency department. Acad Emerg Med. 2017;24:552–68.
Horowitz LM, Wharff EA, Mournet AM, Ross AM, McBee-Strayer S, He J, et al. Validation and feasibility of the Ask Suicide-Screening Questions (ASQ) among pediatric medical/surgical inpatients. Hosp Pediatr. 2020;10(9):750–7.
Cappelli M, Gray CE, Zemek RL, et al. The HEADS-ED: a rapid mental health screening tool for pediatric patients in the emergency department. Pediatrics. 2012;130(2):e321–7.
Cappelli M, Zemek R, Polihronis C, et al. The HEADS-ED: evaluating the clinical use of a brief, action-oriented, pediatric mental health screening tool. Pediatr Emerg Care. 2020;36:9–15.
Cappelli M. HEADS-ED: Mental health screening tool for children and young people. https://www.heads-ed.com/en/content?id=4. Accessed Jan 26, 2021.
York C, Kingsbury S. The choice and partnership approach: a service transformation model. London: CAMHS Network; 2009.
Clark S. Improving access to child and adolescent mental health care: the Choice and Partnership approach. J Can Acad Child Adolesc Psychiatry. 2018;27(1):5–14.
Prosci Inc. The prosci ADKAR model. https://www.prosci.com/adkar. Accessed Jan 17, 2022.
Institute for Healthcare Improvement. Tools. Boston, MA: Institute for Healthcare Improvement, 2020. http://www.ihi.org/resources/Pages/Tools/Driver-Diagram.aspx. Accessed Jan 28, 2022.
Provost LP, Murray SK. The health care data guide: learning from data for improvement. San Francisco: Jossey-Bass; 2011.
Accreditation Canada. Emergency department. Ottawa: Health Standards Organization; 2018.
University of Alberta. Guidelines for differentiating among research, program evaluation and quality improvement. Edmonton: University of Alberta; 2020.
Cwik M, Jay S, Ryan TC, DeVylder J, Edwards S, Wilson ME, Virden J, Goldstein M, Wilcox HC. Lowering the age limit in suicide risk screening: clinical differences and screening form predictive ability. J Am Acad Child Adolesc Psychiatry. 2021;60(5):537–40.
DeVylder JE, Ryan TC, Cwik M, Wilson ME, Jay S, Nedstadt PS, Goldstein M, Wilcox HC. Assessment of selective and universal screening for suicide risk in a pediatric emergency department. JAMA Netw Open. 2019;2(10): e1914070.
Brahmbhatt K, Kurtz BP, Afzal KI, Giles LL, Kowal ED, Johnson KP, Lanzillo E, Pao M, Plioplys S, Horowitz LM, PaCC Workgroup. Suicide risk screening in pediatric hospitals: clinical pathways to address a global health crisis. Psychosomatics. 2019;60(1):1–9.
van der Straten LM, van Stel HF, Spee FJ, Vreeburg ME, Schrijvers AJ, Sturms LM. Safety and efficiency of triaging low urgent self-referred patients to a general practitioner at an acute care post: an observational study. Emerg Med J. 2012;29(11):877–81. https://doi.org/10.1136/emermed-2011-200539. (Epub 2011 Dec 8).
Morreel S, Philips H, De Graeve D, Monsieurs KG, Kampen JK, Meysman J, Lefevre E, Verhoeven V. Triaging and referring in adjacent general and emergency departments (the TRIAGE trial): a cluster randomised controlled trial. PLoS ONE. 2021;16(11): e0258561. https://doi.org/10.1371/journal.pone.0258561.
Clark SE, Cloutier P, Polihronis C, Cappelli M. Evaluating the HEADS-ED screening tool in a hospital-based mental health and addictions central referral intake system: a prospective cohort study. Hosp Pediatr. 2019;9(2):107–14.
MacWilliams K, Curran J, Racek J, Cloutier P, Cappelli M. Barriers and facilitators to implementing the HEADS-ED: a rapid screening tool for pediatric patients in emergency departments. Pediatr Emerg Care. 2017;33(12):774–80.
Boudreaux ED, Niro K, Sullivan A, Rosenbaum CD, Allen M, Camargo CA Jr. Current practices for mental health follow-up after psychiatric emergency department/psychiatric emergency service visits: a national survey of academic emergency departments. Gen Hosp Psychiatry. 2011;33(6):631–3.
Pajer K, Pastrana C, Gardner W, Sivakumar A, York A. A scoping review of the Choice and Partnership Approach in child and adolescent mental health services. J Child Health Care. 2022. https://doi.org/10.1177/13674935221076215. (Epub ahead of print).
Ogrinc G, Dolansky M, Berman AJ, Chambers DA, Davies L. Different approaches to making and testing change in healthcare. BMJ. 2021;374:n1010. https://doi.org/10.1136/bmj.n1010.
Acknowledgements
We would like to acknowledge Kaitlyn Hill, Care Manager, Stollery Emergency Department, for her involvement in this initiative.
Funding
This project was supported Alberta Innovates and Alberta Health Services through joint contribution to the PRIHS (Partnership for Research and Innovation in the Health System) Program (Grant PRIHS 4). Dr. Lightbody’s fellowship was funded by the generosity of the Stollery Children’s Hospital Foundation through the Women and Children’s Health Research Institute (Edmonton, Alberta). Dr. Freedman is supported by the Alberta Children’s Hospital Foundation Professorship in Child Health and Wellness. The funders have no role in the study or dissemination of results.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no confict of interest.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lightbody, T., Thull-Freedman, J., Freedman, S.B. et al. Use of quality improvement methods to enhance implementation of a mental health care bundle in a pediatric emergency department. Can J Emerg Med 25, 326–334 (2023). https://doi.org/10.1007/s43678-023-00476-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43678-023-00476-4