Abstract
Background
Rural-dwelling hemodialysis patients have less frequent contact with nephrologists than urban-dwelling patients, and are known to have higher mortality. We hypothesized that rural-dwelling hemodialysis patients would have more evidence of poorly controlled extracellular fluid volume (ECVF) than otherwise similar urban-dwellers.
Methods
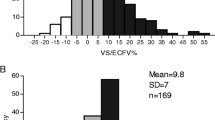
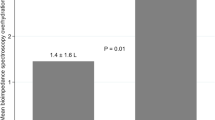
We studied prevalent hemodialysis patients within a single renal program in Alberta, Canada and assessed ECFV using bioimpedance spectroscopy (BIS). Our primary outcome was impedance vector length (ohm/m) as assessed by BIS using the Xitron Hydra 4200 device, where shorter vector length indicated poorer ECFV control. Because poor ECFV control can lead to hypertension, we also assessed pre- and post-dialysis blood pressure. We measured outcomes at baseline.
Results
We studied 228 hemodialysis patients, of whom 115 (50.4 %) and 113 (49.6 %) were urban- and rural-dwelling, respectively. There were no differences in volume control in urban versus rural participants; odds ratio (OR) for vector length in the lowest sex-specific quartile of vector length was 0.93 (95 % CI 0.54, 1.59) after adjusting for age, sex, diabetic status, years since dialysis initiation and phase angle. The odds of very poor blood pressure control (pre-dialysis blood pressure ≥180/100) did not differ between urban and rural participants [fully adjusted OR 0.96 (0.36, 2.60)].
Conclusions
Differences in ECFV control do not appear to explain higher mortality among remote- and rural- dwelling hemodialysis patients, compared to urban-dwellers.

Similar content being viewed by others
References
Tonelli M, Manns B, Culleton B et al (2007) Association between proximity to the attending nephrologist and mortality among patients receiving hemodialysis. CMAJ 177(9):1039–1044
Ho LT, Kushner RF, Schoeller DA, Gudivaka R, Spiegel DM (1994) Bioimpedance analysis of total body water in hemodialysis patients. Kidney Int 46(5):1438–1442
Jaffrin MY, Fenech M, de Fremont JF, Tolani M (2002) Continuous monitoring of plasma, interstitial, and intracellular fluid volumes in dialyzed patients by bioimpedance and hematocrit measurements. ASAIO J 48(3):326–333
Matthie J, Zarowitz B, De Lorenzo A et al (1998) Analytic assessment of the various bioimpedance methods used to estimate body water. J Appl Physiol (1985) 84(5):1801–1816
Basile C, Vernaglione L, Di Iorio B et al (2007) Development and validation of bioimpedance analysis prediction equations for dry weight in hemodialysis patients. Clin J Am Soc Nephrol 2(4):675–680
Fagugli RM, Pasini P, Quintaliani G et al (2003) Association between extracellular water, left ventricular mass and hypertension in haemodialysis patients. Nephrol Dial Transplant 18(11):2332–2338
Fisch BJ, Spiegel DM (1996) Assessment of excess fluid distribution in chronic hemodialysis patients using bioimpedance spectroscopy. Kidney Int 49(4):1105–1109
Katzarski K, Charra B, Laurent G et al (1996) Multifrequency bioimpedance in assessment of dry weight in haemodialysis. Nephrol Dial Transplant 11(Suppl 2):20–23
Katzarski KS, Charra B, Luik AJ et al (1999) Fluid state and blood pressure control in patients treated with long and short haemodialysis. Nephrol Dial Transplant 14(2):369–375
Kraemer M, Rode C, Wizemann V (2006) Detection limit of methods to assess fluid status changes in dialysis patients. Kidney Int 69(9):1609–1620
Lin YP, Yu WC, Hsu TL, Ding PY, Yang WC, Chen CH (2003) The extracellular fluid-to-intracellular fluid volume ratio is associated with large-artery structure and function in hemodialysis patients. Am J Kidney Dis 42(5):990–999
Schneditz D (2006) The arrow of bioimpedance. Kidney Int 69:1492–1493
Zhu F, Sarkar S, Kaitwatcharachai C, Greenwood R, Ronco C, Levin NW (2003) Methods and reproducibility of measurement of resistivity in the calf using regional bioimpedance analysis. Blood Purif 21(1):131–136
De Lorenzo A, Andreoli A, Matthie J, Withers P (1997) Predicting body cell mass with bioimpedance by using theoretical methods: a technological review. J Appl Physiol (1985) 82(5):1542–1558
Di Iorio B, Bellizzi V (2000) Association of mortality and morbidity with bioimpedance analysis. Kidney Int 58(1):464–465
Maggiore Q, Nigrelli S, Ciccarelli C, Grimaldi C, Rossi GA, Michelassi C (1996) Nutritional and prognostic correlates of bioimpedance indexes in hemodialysis patients. Kidney Int 50(6):2103–2108
Pillon L, Piccoli A, Lowrie EG, Lazarus JM, Chertow GM (2004) Vector length as a proxy for the adequacy of ultrafiltration in hemodialysis. Kidney Int 66(3):1266–1271
Piccoli A (1998) Identification of operational clues to dry weight prescription in hemodialysis using bioimpedance vector analysis. The Italian Hemodialysis-Bioelectrical Impedance Analysis (HD-BIA) Study Group. Kidney Int 53(4):1036–1043
Piccoli A, Pillon L, Tabbi MG (1999) Major confounders for reactance as a marker of malnutrition in hemodialysis patients. Kidney Int 56(6):2311–2312
Chamney PW, Kramer M, Rode C, Kleinekofort W, Wizemann V (2002) A new technique for establishing dry weight in hemodialysis patients via whole body bioimpedance. Kidney Int 61(6):2250–2258
De Vries JP, Bogaard HJ, Kouw PM, Oe LP, Stevens P, De Vries PM (1993) The adjustment of post dialytic dry weight based on non-invasive measurement of extracellular fluid and blood volumes. ASAIO J 39(3):M368–M372
Zhu F, Kuhlmann MK, Sarkar S et al (2004) Adjustment of dry weight in hemodialysis patients using intradialytic continuous multifrequency bioimpedance of the calf. Int J Artif Organs 27(2):104–109
Jindal K, Chan CT, Deziel C et al (2006) Hemodialysis clinical practice guidelines for the Canadian Society of Nephrology. J Am Soc Nephrol 17(3 Suppl 1):S1–S27
Veugelers PJ, Yip AM (2003) Socioeconomic disparities in health care use: does universal coverage reduce inequalities in health? J Epidemiol Community Health 57(6):424–428
Permaul-Woods JA, Carroll JC, Reid AJ et al (1999) Going the distance: the influence of practice location on the Ontario Maternal Serum Screening Program. CMAJ 161(4):381–385
Seidel JE, Ghali WA, Faris PD et al (2004) Geographical location of residence and uniformity of access to cardiac revascularization services after catheterization. Can J Cardiol 20(5):517–523
Charra B, Chazot C (2003) Volume control, blood pressure and cardiovascular function. Lessons from hemodialysis treatment. Nephron Physiol 93(4):p94–p101
Charra B, Terrat JC, Vanel T et al (2004) Long thrice weekly hemodialysis: the Tassin experience. Int J Artif Organs 27(4):265–283
Chazot C, Charra B, Van Vo C et al (1999) The Janus-faced aspect of ‘dry weight’. Nephrol Dial Transplant 14(1):121–124
Fagugli RM, Pasini P, Pasticci F, Ciao G, Cicconi B, Buoncristiani U (2006) Effects of short daily hemodialysis and extended standard hemodialysis on blood pressure and cardiac hypertrophy: a comparative study. J Nephrol 19(1):77–83
Gunal AI, Karaca I, Aygen B, Yavuzkir M, Dogukan A, Celiker H (2004) Strict fluid volume control and left ventricular hypertrophy in hypertensive patients on chronic haemodialysis: a cross-sectional study. J Int Med Res 32(1):70–77
Ozkahya M, Ok E, Cirit M et al (1998) Regression of left ventricular hypertrophy in haemodialysis patients by ultrafiltration and reduced salt intake without antihypertensive drugs. Nephrol Dial Transplant 13(6):1489–1493
Ozkahya M, Toz H, Qzerkan F et al (2002) Impact of volume control on left ventricular hypertrophy in dialysis patients. J Nephrol 15(6):655–660
Toprak A, Koc M, Tezcan H, Ozener IC, Akoglu E, Oktay A (2003) Inferior vena cava diameter determines left ventricular geometry in continuous ambulatory peritoneal dialysis patients: an echocardiographic study. Nephrol Dial Transplant 18(10):2128–2133
Agarwal R (2005) Hypertension and survival in chronic hemodialysis patients–past lessons and future opportunities. Kidney Int 67(1):1–13
Cannella G, Paoletti E, Ravera G et al (2000) Inadequate diagnosis and therapy of arterial hypertension as causes of left ventricular hypertrophy in uremic dialysis patients. Kidney Int 58(1):260–268
Charra B, Calemard E, Ruffet M et al (1992) Survival as an index of adequacy of dialysis. Kidney Int 41(5):1286–1291
Foley RN, Parfrey PS, Harnett JD, Kent GM, Murray DC, Barre PE (1996) Impact of hypertension on cardiomyopathy, morbidity and mortality in end-stage renal disease. Kidney Int 49(5):1379–1385
Mazzuchi N, Carbonell E, Fernandez-Cean J (2000) Importance of blood pressure control in hemodialysis patient survival. Kidney Int 58(5):2147–2154
Ritz E, Strumpf C, Katz F, Wing AJ, Quellhorst E (1985) Hypertension and cardiovascular risk factors in hemodialyzed diabetic patients. Hypertension. 7(6 Pt 2):118–124 (II)
Tomita J, Kimura G, Inoue T et al (1995) Role of systolic blood pressure in determining prognosis of hemodialyzed patients. Am J Kidney Dis 25(3):405–412
Agarwal R, Satyan S, Alborzi P et al (2009) Home blood pressure measurements for managing hypertension in hemodialysis patients. Am J Nephrol 30(2):126–134
Acknowledgments
The authors of this report are grateful to the study coordinators: Nancy Ruholl, Nasreen Ahmad and Lori Piquette; research assistants Yuanchen Liu, Lois Hannam, Brian Nadler, Tim Chan, Evelyn Chan, and Somaya Zahran; and to all of the participants in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by the Canadian Institutes of Health Research.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Tonelli, M., Lloyd, A., Pannu, N. et al. Extracellular fluid management and hypertension in urban dwelling versus rural dwelling hemodialysis patients. J Nephrol 31, 103–110 (2018). https://doi.org/10.1007/s40620-016-0337-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-016-0337-y