Abstract
Background
Although dietary components may play a role in the development of chronic kidney disease (CKD), data on this topic are scarce. The objective of this study was to investigate the association between macronutrient intakes and CKD in a large non-diabetic adult population-based study.
Methods
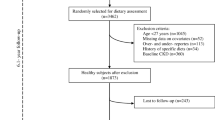
This cross-sectional study recruited 5,316 participants aged ≥27 years without diabetes within the framework of the Tehran lipid and glucose study. Dietary intake was collected using a validated food-frequency questionnaire. Macronutrients intake including total-, animal-, and plant-protein, carbohydrate, simple sugar, fructose, total fat, saturated fatty acids, poly- and monounsaturated-fatty acids (PUFA and MUFA), and n-3 and n-6 fatty acids was categorized into quartiles. Anthropometrics, blood pressure, serum creatinine, and fasting plasma glucose and lipids were measured. Estimated glomerular filtration rate (eGFR) was calculated using the Modification of Diet in Renal Disease Study equation. CKD was defined as eGFR <60 ml/min/1.73 m2.
Result
Mean age of participants was 45.0 ± 12.2 years. Mean eGFR was 71.9 ± 11.1 ml/min/1.73 m2, and 13 % had CKD. After adjustment for serum triglycerides and cholesterol, body mass index, and hypertension, the risk of CKD decreased in the highest quartile compared to lowest quartile of plant protein (OR, 95 % CI) (0.70, 0.51–0.97), PUFA (0.73, 0.55–0.99), and n-6 fatty acids (0.75, 0.57–0.97). However, the risk of CKD increased in the highest quartile of animal protein (1.37, 1.05–1.79) compared to the lowest.
Conclusion
Plant protein, PUFA, and n-6 fatty acids are associated with a lower risk of CKD, independently of hypertension and diabetic mellitus, while animal protein may be a risk factor for CKD in adults.
Similar content being viewed by others
References
National Kidney Foundation (2002) K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Am J Kidney Dis 39:S1–S266
Imai E, Horio M, Yamagata K et al (2008) Slower decline of glomerular filtration rate in the Japanese general population: a longitudinal 10-year follow-up study. Hypertens Res 31:433–441
Xu R, Zhang L, Zhang P et al (2009) Comparison of the prevalence of chronic kidney disease among different ethnicities: Beijing CKD survey and American NHANES. Nephrol Dial Transplant 24:1220–1226
Lin J, Fung TT, Hu FB et al (2011) Association of dietary patterns with albuminuria and kidney function decline in older white women: a subgroup analysis from the Nurses’ Health Study. Am J Kidney Dis 57:245–254
Chrysohoou C, Panagiotakos DB, Pitsavos C et al (2010) Adherence to the Mediterranean diet is associated with renal function among healthy adults: the ATTICA study. J Ren Nutr 20:176–184
Daviglus ML, Greenland P, Stamler J et al (2005) Relation of nutrient intake to microalbuminuria in nondiabetic middle-aged men and women: International Population Study on macronutrients and blood pressure (INTERMAP). Am J Kidney Dis 45:256–266
Higashiyama A, Watanabe M, Kokubo Y et al (2010) Relationships between protein intake and renal function in a Japanese general population: NIPPON DATA90. J Epidemiol 20(Suppl 3):S537–S543
Knight EL, Stampfer MJ, Hankinson SE et al (2003) The impact of protein intake on renal function decline in women with normal renal function or mild renal insufficiency. Ann Intern Med 138:460–467
Diaz-Lopez A, Bullo M, Basora J et al (2013) Cross-sectional associations between macronutrient intake and chronic kidney disease in a population at high cardiovascular risk. Clin Nutr 32:606–612
Pedrini MT, Levey AS, Lau J et al (1996) The effect of dietary protein restriction on the progression of diabetic and nondiabetic renal diseases: a meta-analysis. Ann Intern Med 124:627–632
Walrand S, Short KR, Bigelow ML et al (2008) Functional impact of high protein intake on healthy elderly people. Am J Physiol Endocrinol Metab 295:E921–E928
Frank H, Graf J, Amann-Gassner U et al (2009) Effect of short-term high-protein compared with normal-protein diets on renal hemodynamics and associated variables in healthy young men. Am J Clin Nutr 90:1509–1516
Gopinath B, Harris DC, Flood VM et al (2011) Consumption of long-chain n-3 PUFA, alpha-linolenic acid and fish is associated with the prevalence of chronic kidney disease. Br J Nutr 105:1361–1368
Gopinath B, Harris DC, Flood VM et al (2011) Carbohydrate nutrition is associated with the 5-year incidence of chronic kidney disease. J Nutr 141:433–439
Azizi F, Rahmani M, Emami H et al (2002) Cardiovascular risk factors in an Iranian urban population: Tehran lipid and glucose study (phase 1). Soz Praventivmed 47:408–426
Azizi F, Ghanbarian A, Momenan AA et al (2009) Prevention of non-communicable disease in a population in nutrition transition: Tehran lipid and glucose study phase II. Trials 10:5
Hosseini-Esfahani F, Jessri M, Mirmiran P et al (2010) Adherence to dietary recommendations and risk of metabolic syndrome: Tehran lipid and glucose study. Metabolism 59:1833–1842
Mirmiran P, Esfahani FH, Mehrabi Y et al (2010) Reliability and relative validity of an FFQ for nutrients in the Tehran lipid and glucose study. Public Health Nutr 13:654–662
Asghari G, Rezazadeh A, Hosseini-Esfahani F et al (2012) Reliability, comparative validity and stability of dietary patterns derived from an FFQ in the Tehran lipid and glucose study. Br J Nutr 108:1109–1117
The Nutrient Data Laboratory (2009) Food Composition Table (FCT) FaNIC, United States Department of Agriculture (USDA). Available from URL: http://www.nal.usda.gov/fnic/foodcomp. Accessed date 2009
Azar MSE (1980) Food Composition Table of Iran. National Nutrition and Food Research Institute. Shahid Beheshti University Press, Tehran
Mancia G, De Backer G, Dominiczak A et al (2007) 2007 guidelines for the management of arterial hypertension: the task force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens 25:1105–1187
Levey AS, Bosch JP, Lewis JB et al (1999) A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Modification of Diet in Renal Disease Study Group. Ann Intern Med 130:461–470
Lin J, Hu FB, Curhan GC (2010) Associations of diet with albuminuria and kidney function decline. Clin J Am Soc Nephrol 5:836–843
Barbosa AC, Lajolo FM, Genovese MI (2011) Effect of free or protein-associated soy isoflavones on the antioxidant status in rats. J Sci Food Agric 91:721–731
Braun P, Aubourg S, Van Leene J et al (2013) Plant protein interactomes. Annu Rev Plant Biol 64:161–187
Curhan GC, Willett WC, Rimm EB et al (1993) A prospective study of dietary calcium and other nutrients and the risk of symptomatic kidney stones. N Engl J Med 328:833–838
Breslau NA, Brinkley L, Hill KD et al (1988) Relationship of animal protein-rich diet to kidney stone formation and calcium metabolism. J Clin Endocrinol Metab 66:140–146
Coe FL, Moran E, Kavalich AG (1976) The contribution of dietary purine over-consumption to hyperuricosuria in calcium oxalate stone formers. J Chronic Dis 29:793–800
Alexander RT, Hemmelgarn BR, Wiebe N et al (2012) Kidney stones and kidney function loss: a cohort study. BMJ 345:e5287
Shcherbak AV, Kozlovskaia LV, Bobkova IN et al (2013) Hyperuricemia and the problem of chronic kidney disease. Ter Arkh 85:100–104
Sun SZ, Flickinger BD, Williamson-Hughes PS et al (2010) Lack of association between dietary fructose and hyperuricemia risk in adults. Nutr Metab (Lond) 7:16
Lau C, Faerch K, Glumer C et al (2005) Dietary glycemic index, glycemic load, fiber, simple sugars, and insulin resistance: the Inter99 study. Diabetes Care 28:1397–1403
Chen S, Chen Y, Liu X et al (2013) Association of insulin resistance with chronic kidney disease in non-diabetic subjects with normal weight. PLoS One 8:e74058
Chandalia M, Garg A, Lutjohann D et al (2000) Beneficial effects of high dietary fiber intake in patients with type 2 diabetes mellitus. N Engl J Med 342:1392–1398
Krishnamurthy VM, Wei G, Baird BC et al (2012) High dietary fiber intake is associated with decreased inflammation and all-cause mortality in patients with chronic kidney disease. Kidney Int 81:300–306
Palafox-Carlos H, Ayala-Zavala JF, Gonzalez-Aguilar GA (2011) The role of dietary fiber in the bioaccessibility and bioavailability of fruit and vegetable antioxidants. J Food Sci 76:R6–R15
Chen H, Chen D, Michiels J et al (2013) Dietary fiber affects intestinal mucosal barrier function by regulating intestinal bacteria in weaning piglets. Commun Agric Appl Biol Sci 78:71–78
Taylor EN, Curhan GC (2008) Fructose consumption and the risk of kidney stones. Kidney Int 73:207–212
Milne DB, Nielsen FH (2000) The interaction between dietary fructose and magnesium adversely affects macromineral homeostasis in men. J Am Coll Nutr 19:31–37
Nguyen NU, Dumoulin G, Henriet MT et al (1995) Increase in urinary calcium and oxalate after fructose infusion. Horm Metab Res 27:155–158
Curhan GC, Taylor EN (2008) 24-h uric acid excretion and the risk of kidney stones. Kidney Int 73:489–496
Hosseini-Esfahani F, Bahadoran Z, Mirmiran P et al (2011) Dietary fructose and risk of metabolic syndrome in adults: Tehran lipid and glucose study. Nutr Metab (Lond) 8:50
Ha V, Sievenpiper JL, de Souza RJ et al (2012) Effect of fructose on blood pressure: a systematic review and meta-analysis of controlled feeding trials. Hypertension 59:787–795
Bray GA (2012) Fructose and risk of cardiometabolic disease. Curr Atheroscler Rep 14:570–578
Ruan X, Guan Y (2009) Metabolic syndrome and chronic kidney disease. J Diabetes 1:236–245
Lin J, Judd S, Le A et al (2010) Associations of dietary fat with albuminuria and kidney dysfunction. Am J Clin Nutr 92:897–904
Kshirsagar AV, Bomback AS, Bang H et al (2008) Association of C-reactive protein and microalbuminuria (from the National Health and Nutrition Examination Surveys, 1999 to 2004). Am J Cardiol 101:401–406
Ma Y, Griffith JA, Chasan-Taber L et al (2006) Association between dietary fiber and serum C-reactive protein. Am J Clin Nutr 83:760–766
Masson CJ, Mensink RP (2011) Exchanging saturated fatty acids for (n-6) polyunsaturated fatty acids in a mixed meal may decrease postprandial lipemia and markers of inflammation and endothelial activity in overweight men. J Nutr 141:816–821
Esmaillzadeh A, Kimiagar M, Mehrabi Y et al (2007) Dietary patterns and markers of systemic inflammation among Iranian women. J Nutr 137:992–998
Lopez-Garcia E, Schulze MB, Fung TT et al (2004) Major dietary patterns are related to plasma concentrations of markers of inflammation and endothelial dysfunction. Am J Clin Nutr 80:1029–1035
Acknowledgments
This work was funded by a grant from the Research Institute for Endocrine Sciences, Shadid Beheshti University of Medical Sciences, Tehran, Iran. All authors read and approved the final manuscript. The authors express appreciation to the participants in the Tehran Lipid and Glucose Study for their enthusiastic support, and the staff of the Tehran Lipid and Glucose Study Unit of the Research Institute for Endocrine Sciences, for their valuable help. We would like to acknowledge Ms. N. Shiva for critical edition of English grammar and syntax of the manuscript.
Conflict of interest
None of the authors had any personal or financial conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yuzbashian, E., Asghari, G., Mirmiran, P. et al. Associations of dietary macronutrients with glomerular filtration rate and kidney dysfunction: Tehran lipid and glucose study. J Nephrol 28, 173–180 (2015). https://doi.org/10.1007/s40620-014-0095-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-014-0095-7