Abstract
Objective
The aim of this study was to evaluate the relationships between the serum levels of adiponectin and systemic oxidative stress exerted on lipids, proteins, as well as endothelial function and cardiovascular diseases (CVD) risk markers, in elderly subjects with metabolic syndrome (MS).
Methods
The serum advanced glycation and oxidation protein products, low-density lipoprotein susceptibility to oxidation (oxLDL), nitric oxide metabolic pathway products (NOx), serum lipid peroxidation, as well as total antioxidant/oxidative capacity (TAC/TOC), were analyzed in elderly subjects with MS (n = 44), compared to aged-matched control (n = 39).
Results
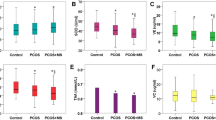
We pointed out significantly lower levels of adiponectin in elderly MS subjects concomitantly with significantly higher levels of oxidative stress and CVD risk markers. Significant positive correlations were found between serum adiponectin levels and HDL-cholesterol (p < 0.05) and the total cholesterol/LDL-cholesterol ratio (p < 0.01). Additionally, adiponectin levels were significantly inversely associated with insulin resistance index (HOMA-IR, r = −0.348; p < 0.05) and serum lipid peroxidation (r = −0.337; p < 0.05), and significantly positively with the antioxidant capacity (TAC, r = 0.339; p < 0.05). Conversely, adiponectin levels were significantly negatively (r = −0.310; p < 0.05) associated with serum uric acid concentration.
Conclusions
The major protective role of adiponectin versus stress related to an impaired glucose and lipid metabolism suggests that adiponectin plays a critical role in adiposity-related metabolic stress and redox homeostasis.

Similar content being viewed by others
References
Lanske B, Razzaque MS (2007) Vitamin D and aging: old concepts and new insights. J Nutr Biochem 18:771–777
Tchkonia T, Morbeck DE, Von Zglinicki T et al (2010) Fat tissue, aging, and cellular senescence. Aging Cell 9:667–684
Nigro E, Scudiero O, Monaco ML et al (2014) New insight into adiponectin role in obesity and obesity-related diseases. Biomed Res Int 2014:658913
Coimbra S, Brandão Proença J, Santos-Silva A et al (2014) Adiponectin, leptin, and chemerin in elderly patients with type 2 diabetes mellitus: a close linkage with obesity and length of the disease. BioMed Res Int 2014:701915
Kizer JR (2013) Adiponectin, cardiovascular disease, and mortality: parsing the dual prognostic implications of a complex adipokine. Metabolism 63:1079–1083
Mascarenhas-Melo F, Palavra F, Marado D et al (2013) Emergent biomarkers of residual cardiovascular risk in patients with low HDL-c and/or high triglycerides and average LDL-c concentrations: focus on HDL subpopulations. Oxidized LDL, adiponectin, and uric acid. Sci World J 2013:387849
Weyer C, Funahashi T, Tanaka S et al (2001) Hypoadiponectinemia in obesity and type 2 diabetes: close association with insulin resistance and hyperinsulinemia. J Clin Endocrinol Metab 86:1930–1935
Hulthe J, Hulten LM, Fagerberg B (2003) Low adipocyte-derived plasma protein adiponectin concentrations are associated with the metabolic syndrome and small dense low-density lipoprotein particles: atherosclerosis and insulin resistance study. Metabolism 52:1612–1614
Cruz M, Garcia-Macedo R, Garcia-Valerio Y et al (2004) Low adiponectin levels predict type 2 diabetes in Mexican children. Diabetes Care 27:1451–1453
Cheung CY, Hui EY, Cheung BM et al (2014) Adiponectin gene variants and the risk of coronary heart disease: a 16-year longitudinal study. Eur J Endocrinol 171:107–115
Keaney JF Jr, Larson MG, Vasan RS et al (2003) Obesity and systemic oxidative stress: clinical correlates of oxidative stress in the Framingham Study. Arterioscler Thromb Vasc Biol 23:434–439
Furukawa S, Fujita T, Shimabukuro M et al (2004) Increased oxidative stress in obesity and its impact on metabolic syndrome. J Clin Invest 114:1752–1761
Fujita K, Nishizawa H, Funahashi T et al (2006) Systemic oxidative stress is associated with visceral fat accumulation and the metabolic syndrome. Circ J 70:1437–1442
Vincent HK, Taylor AG (2006) Biomarkers and potential mechanisms of obesity-induced oxidant stress in humans. Int J Obes 30:400–418
Chen SJ, Yen CH, Huang YC et al (2012) Relationships between inflammation, adiponectin, and oxidative stress in metabolic syndrome. PLoS ONE 7:e45693
Nakanishi S, Yamane K, Kamei N et al (2005) A protective effect of adiponectin against oxidative stress in Japanese Americans: the association between adiponectin or leptin and urinary isoprostane. Metabolism 54:194–199
Lautamäki R, Rönnemaa T, Huupponen R et al (2007) Low serum adiponectin is associated with high circulating oxidized low-density lipoprotein in patients with type 2 diabetes mellitus and coronary artery disease. Metabolism 56:881–886
Gustafsson S, Lind L, Söderberg S et al (2013) Oxidative stress and inflammatory markers in relation to circulating levels of adiponectin. Obesity (Silver Spring) 21:1467–1473
Al-Attas OS, Al-Daghri NM, Alokail MS et al (2010) Adiposity and insulin resistance correlate with telomere length in middle-aged Arabs: the influence of circulating adiponectin. Eur J Endocrinol 163:601–607
Liu JB, Li WJ, Fu FM et al (2015) Inverse correlation between serum adiponectin and 8-iso-prostaglandin F2α in newly diagnosed type 2 diabetes patients. Int J Clin Exp Med 8:6085–6090
Schautz B, Later W, Heller M et al (2012) Impact of age on leptin and adiponectin independent of adiposity. Br J Nutr 108:363–370
Cicero AF, Magni P, Moré M et al (2012) Metabolic syndrome, adipokines and hormonal factors in pharmacologically untreated adult elderly subjects from the Brisighella Heart Study historical cohort. Obes Facts 5:319–326
Graessler J, Gruber M, Radke RB et al (2011) Type 2 diabetes in octogenarians is associated with decreased low molecular weight adiponectin. Gerontology 57:316–326
Zamboni M, Mazzali G, Zoico E et al (2005) Health consequences of obesity in the elderly: a review of four unresolved questions. Int J Obes 29:1011–1029
Kassi E, Pervanidou P, Kaltsas G et al (2011) Metabolic syndrome: definitions and controversies. BMC Med 2011:9
Grundy SM, Brewer B, Cleeman JI et al (2004) Definition of metabolic syndrome: report of the National Heart, Lung, and Blood Institute/American Heart Association conference on scientific issues related to definition. Circulation 109:433–438
Grundy SM, Cleeman JI, Daniels SR et al (2005) Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation 112:2735–2752
Matthews DR, Hosker JP, Rudenski AS et al (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28:412–419
Scoccia AE, Molinuevo MS, McCarthy AD et al (2001) A simple method to assess the oxidative susceptibility of low density lipoproteins. BMC Clin Pathol 1:1. doi:10.1186/1472-6890-1-1
Kalousová M, Škrha J, Zima T (2002) Advanced glycation end-products and advanced oxidation protein products in patients with diabetes mellitus. Physiol Res 51:597–604
Bartling B, Hofmann HS, Sohst A et al (2011) Prognostic potential and tumor growth-inhibiting effect of plasma advanced glycation end products in non-small cell lung carcinoma. Mol Med 17:980–989
Margina D, Gradinaru D, Manda G et al (2013) Membranar effects exerted in vitro by polyphenols -quercetin, epigallocatechin gallate and curcumin- on HUVEC and Jurkat cells, relevant for diabetes mellitus. Food Chem Toxicol 61:86–93
Gubandru M, Margina D, Tsitsimpikou C et al (2013) Alzheimer’s disease treated patients showed different patterns for oxidative stress and inflammation markers. Food Chem Toxicol 61:209–214
Dobiasova M, Frohlich J (2001) The plasma parameter log (TG/HDL-C) as an atherogenic index: correlation with lipoprotein particle size and esterification rate in apoB-lipoprotein-depleted plasma (FER(HDL)). Clin Biochem 34:583–588
Guarner V, Rubio-Ruiz ME (2012) Aging, metabolic syndrome and the heart. Aging Dis 3:269–279
Tormos KV, Anso E, Hamanaka RB et al (2011) Mitochondrial complex III ROS regulate adipocyte differentiation. Cell Metab 14:537–544
Hirose H, Takayama M, Iwao Y et al (2016) Effects of aging on visceral and subcutaneous fat areas and on homeostasis model assessment of insulin resistance and insulin secretion capacity in a comprehensive health checkup. J Atheroscler Thromb 23:207–215
Tsunekawa T, Hayashi T, Suzuki Y et al (2003) Plasma adiponectin plays an important role in improving insulin resistance with glimepiride in elderly type 2 diabetic subjects. Diabetes Care 26:285–589
Pischon T, Girman CJ, Hotamisligil GS et al (2004) Plasma adiponectin levels and risk of myocardial infarction in men. JAMA 291:1730–1737
Margina D, Gradinaru D, Panaite C et al (2011) The association of adipose tissue markers for redox imbalance and the cardio-vascular risk in obese patients. HealthMED J 5:194–199
Gradinaru D, Borsa C, Ionescu C et al (2013) Advanced oxidative and glycoxidative protein damage markers in the elderly with type 2 diabetes. J Proteomics 92:313–322
Gradinaru D, Borsa C, Ionescu C et al (2013) Vitamin D status and oxidative stress markers in the elderly with impaired fasting glucose and type 2 diabetes mellitus. Aging Clin Exp Res 24:595–602
Chiou WK, Huang DH, Wang MH et al (2012) Significance and association of serum uric acid (UA) levels with components of metabolic syndrome (MS) in the elderly. Arch Gerontol Geriatr 55:724–728
Osgood K, Krakoff J, Thearle M (2013) Serum uric acid predicts both current and future components of the metabolic syndrome. Metab Syndr Relat Disord 11:157–162
Zurlo A, Veronese N, Giantin V et al (2015) High serum uric acid levels increase the risk of metabolic syndrome in elderly women: the PRO.V.A study. Nutr Metab Cardiovasc Dis 15:S0939–S4753
Bochud M, Marques-Vidal PM, Vollenweider P et al (2008) Blood pressure modifies the association between serum adiponectin and uric acid, in a sex-dependent manner. In: 40th Annual meeting Swiss society of nephrology, St. Gallen, December 3–5, 2008. Swiss Med Weekly 138:10S
Tsioufis C, Kyvelou S, Dimitriadis K et al (2011) The diverse associations of uric acid with low-grade inflammation, adiponectin and arterial stiffness in never-treated hypertensives. J Hum Hypertens 25:554–559
Park JS, Kang S, Ahn CW et al (2012) Relationships between serum uric acid, adiponectin and arterial stiffness in postmenopausal women. Maturitas 73:344–348
Acknowledgments
The authors are grateful for the support consisting in the opportunity to make use of the equipment obtained under the framework of the EU-FP7 Project “MARK-AGE, European Study to Establish Biomarkers of Human Ageing.” Daniela Gradinaru and Anca Dinischiotu acknowledge the scientific support of the EU-COST Actions on Lipid Peroxidation Associated Disorders (B35 Action) and on Chemistry of Non-Enzymatic Protein Modifications (CM1001 Action).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was reviewed and approved by the Ethics Committee of the Ana Aslan—National Institute of Gerontology and Geriatrics (Approval Number 14203/14.09.2015).
Statement of human and animal rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Gradinaru, D., Margina, D., Borsa, C. et al. Adiponectin: possible link between metabolic stress and oxidative stress in the elderly. Aging Clin Exp Res 29, 621–629 (2017). https://doi.org/10.1007/s40520-016-0629-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-016-0629-z