Abstract
Background
Researches seek to understand the links between adverse health outcomes and cortisol concentrations. However, the relationship between depressive symptomatology and cortisol concentrations is controversial in the literature.
Aim
To analyze the relationship between the depressive symptomatology and the cortisol concentrations in elderly community residents in the Brazilian Northeast.
Methods
Cross-sectional study is composed of 256 elderly (≥65 years). Depressive symptomatology was evaluated by the Center for Epidemiologic Studies-Depression Scale and cortisol concentrations by salivary collection (upon waking, 30 and 60 min after waking, at 3 pm and before bed), in addition to composite measurements. Sociodemographic and health conditions were evaluated. For analysis of the cortisol measurements in relation to depressive symptomatology, and between genders, the Student’s t test was used. For cortisol measurements in every curve, analysis of variance for repeated measurements with Bonferroni post hoc test was used.
Results
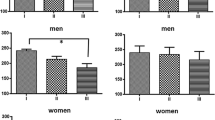
There were significant salivary cortisol differences upon awakening, among elderly with and without depressive symptomatology (p = 0.04). There was no significance in relation to gender. Between measurements of each curve, elderly with depressive symptomatology showed no significant difference between the 1st measure in relation to the 2nd and 3rd, and also between the 4th and 5th, demonstrating higher cortisol night levels in elderly with depressive symptomatology, without decline, with curve plane aspect.
Conclusion
The relationship between depressive symptomatology and hypocortisolism throughout the day seems to exist. However, in Brazil, adverse life conditions can lead to chronic stress and be sufficient factors to superpose biggest differences that could exist in relation to the presence of depressive symptomatology.


Similar content being viewed by others
References
Karatsoreos IN, Karatoreos IN, McEwen BS (2013) Annual Research Review: The neurobiology and physiology of resilience and adaptation across the life course. J Child Psychol Psychiatry 54:337–347. doi:10.1111/jcpp.12054
Heaney JL, Phillips AC, Carroll D (2010) Ageing, depression, anxiety, social support and the diurnal rhythm and awakening response of salivary cortisol. Int J Psychophysiol 78:201–208. doi:10.1016/j.ijpsycho.2010.07.009
Dowd JB, Simanek AM, Aiello AE (2009) Socio-economic status, cortisol and allostatic load: a review of the literature. Int J Epidemiol 38:1297–1309. doi:10.1093/ije/dyp277
Fries E, Hesse J, Hellhammer J et al (2005) A new view on hypocortisolism. Psychoneuroendocrinology 30:1010–1016. doi:10.1016/j.psyneuen.2005.04.006
Chida Y, Steptoe A (2009) Cortisol awakening response and psychosocial factors: a systematic review and meta-analysis. Biol Psychol 80:265–278. doi:10.1016/j.biopsycho.2008.10.004
Hinkelmann K, Moritz S, Botzenhardt J et al (2009) Cognitive impairment in major depression: association with salivary cortisol. Biol Psychiatry 66:879–885. doi:10.1016/j.biopsych.2009.06.023
Oliveira DAAP, Gomes L, Oliveira RF (2006) Prevalência de depressão em idosos que freqüentam centros de convivência. Rev Saúde Pública 40:734–736. doi:10.1590/S0034-89102006000500026
Gillespie CF, Nemeroff CB (2005) Hypercortisolemia and depression. Psychosom Med 67(Suppl 1):S26–S28. doi:10.1097/01.psy.0000163456.22154.d2
Hartaigh BO, Loerbroks A, Thomas GN et al (2012) Age-dependent and -independent associations between depression, anxiety, DHEAS, and cortisol: from the MIPH Industrial Cohort Studies (MICS). Psychoneuroendocrinology 37:929–936. doi:10.1016/j.psyneuen.2011.10.009
Otte C, Hart S, Neylan TC et al (2005) A meta-analysis of cortisol response to challenge in human aging: importance of gender. Psychoneuroendocrinology 30:80–91. doi:10.1016/j.psyneuen.2004.06.002
Caldas VV, Zunzunegui MV, Freire AN et al (2012) Translation, cultural adaptation and psychometric evaluation of the Leganes cognitive test in a low educated elderly Brazilian population. Arq Neuropsiquiatr 70:22–27. doi:10.1590/S0004-282X2012000100006
Zunzunegui MV, Cuadra PG, Beland F et al (2000) Development of simple cognitive function measures in a community dwelling population of elderly in Spain. Int J Geriatr Psychiatry 15:130–140. doi:10.1002/(SICI)1099-1166(200002)15:23.3.CO;2-3
Batistoni SST, Neri AL, Cupertino APFB (2007) Validade da escala de depressão do Center for Epidemiological Studies entre idosos brasileiros. Rev Saúde Pública 41:598–605. doi:10.1590/S1413-82712010000100003
Radloff LS (1977) The CES-D Scale: a self-report depression scale for research in the general population. Appl Psychol Meas 1:385–401. doi:10.1177/014662167700100306
Pruessner M, Hellhammer DH, Pruessner JC et al (2003) Self-reported depressive symptoms and stress levels in healthy young men: associations with the cortisol response to awakening. Psychosom Med 65:92–99. doi:10.1097/01.PSY.0000040950.22044.10
Alvarado BE, Zunzunegui MV, Beland F et al (2007) Social and gender inequalities in depressive symptoms among urban older adults of latin America and the Caribbean. J Gerontol B Psychol Sci Soc Sci 62:S226–S236. doi:10.1093/geronb/62.4.S226
Mechakra-Tahiri S, Zunzunegui MV, Préville M et al (2009) Social relationships and depression among people 65 years and over living in rural and urban areas of Quebec. Int J Geriatr Psychiatry 24:1226–1236. doi:10.1002/gps.2250
Maciel ÁCC, Guerra RO (2006) Prevalence and associated factors of depressive simptomatology in elderly residents in the Northeast of Brazil. J Bras Psiquiatr 55:26–33. doi:10.1590/S0047-20852006000100004
Penninx BW, Beekman AT, Bandinelli S et al (2007) Late-life depressive symptoms are associated with both hyperactivity and hypoactivity of the hypothalamo-pituitary-adrenal axis. Am J Geriatr Psychiatry 15:522–529. doi:10.1097/JGP.0b013e318033ed80
Borges LJ, Benedetti TRB, Mazo GZ (2007) Rastreamento cognitivo e sintomas depressivos em idosos iniciantes em programa de exercício físico. J Bras Psiquiatr 56:273–279. doi:10.1590/S0047-20852007000400006
Okamoto K, Momose Y, Fujino A et al (2008) Gender differences in the relationship between self-rated health (SRH) and 6-year mortality risks among the elderly in Japan. Arch Gerontol Geriatr 47:311–317. doi:10.1016/j.archger.2007.08.013
Gardner MP, Lightman S, Sayer AA et al (2013) Dysregulation of the hypothalamic pituitary adrenal (HPA) axis and physical performance at older ages: an individual participant meta-analysis. Psychoneuroendocrinology 38:40–49. doi:10.1016/j.psyneuen.2012.04.016
Peeters GMEE, van Schoor NM, van Rossum EFC et al (2008) The relationship between cortisol, muscle mass and muscle strength in older persons and the role of genetic variations in the glucocorticoid receptor. Clin Endocrinol (Oxf) 69:673–682. doi:10.1111/j.1365-2265.2008.03212.x
Balardin JB, Vedana G, Luz C et al (2010) Subjective mild depressive symptoms are associated with abnormal diurnal cycle of salivary cortisol in older adults. J Geriatr Psychiatry Neurol 24:19–22. doi:10.1177/0891988710373599
Burke HM, Davis MC, Otte C et al (2005) Depression and cortisol responses to psychological stress: a meta-analysis. Psychoneuroendocrinology 30:846–856. doi:10.1016/j.psyneuen.2005.02.010
Tu MT, Zunzunegui MV, Guerra RO et al (2013) Cortisol profile and depressive symptoms in older adults residing in Brazil and in Canada. Aging Clin Exp Res. doi:10.1007/s40520-013-0111-0
Vreeburg SA, Hoogendijk WJ, DeRijk RH et al (2012) Salivary cortisol levels and the 2-year course of depressive and anxiety disorders. Psychoneuroendocrinology 38:1494–1502. doi:10.1016/j.psyneuen.2012.12.017
Knorr U, Vinberg M, Kessing LV et al (2010) Salivary cortisol in depressed patients versus control persons: a systematic review and meta-analysis. Psychoneuroendocrinology 35:1275–1286. doi:10.1016/j.psyneuen.2010.04.001
Phillips AC, Batty GD, Gale CR et al (2011) Major depressive disorder, generalised anxiety disorder, and their comorbidity: associations with cortisol in the Vietnam Experience Study. Psychoneuroendocrinology 36:682–690. doi:10.1016/j.psyneuen.2010.09.011
Goldman-Mellor S, Hamer M, Steptoe A (2012) Early-life stress and recurrent psychological distress over the lifecourse predict divergent cortisol reactivity patterns in adulthood. Psychoneuroendocrinology 37:1755–1768. doi:10.1016/j.psyneuen.2012.03.010
Acknowledgments
We thank all the participants of this research and the physiotherapists who worked as interviewers during data collection. This work has been funded by the National Council for Scientific and Technological Development (Conselho Nacional de Desenvolvimento Científico e Tecnológico—CNPq) as project 474728/2009-9.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the Research Ethics Committee of the Universidade Federal do Rio Grande do Norte, as part of a larger study called “Functional performance, load allostatic and biomarkers stress in the elderly residents in the community” (CEP/HUOL 481/10), in accordance with resolution 466/12 National Health Council and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Additional informed consent was obtained from all individual participants for whom identifying information is included in this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Moreira, M.A., Guerra, R.O., do Nascimento Falcão Freire, A. et al. Depressive symptomatology and cortisol concentrations in elderly community residents: a cross-sectional study. Aging Clin Exp Res 28, 131–137 (2016). https://doi.org/10.1007/s40520-015-0374-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-015-0374-8