Abstract
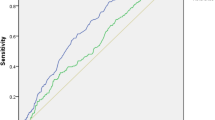
Metabolic syndrome (MetS) has been shown to be associated with inflammation. However, in diabetic patients with MetS, its relationship with the neutrophil to lymphocyte ratio (NLR) as a novel inflammation marker is unclear. The aim of the study was to investigate the association between NLR and MetS in patients with type 2 diabetes mellitus. It was a cross-sectional study which included 261 consecutive patients (mean age 56.7 ± 10.5 years, 56.7% female) with type 2 diabetes. NLR and other clinical and laboratory parameters of patients with and without MetS were evaluated. The prevalence of MetS was 85.8%. The NLR was higher in patients with MetS than without MetS (p = 0.001). There was a significant correlation between the NLR and the number of MetS components (r = 0.147, p = 0.017). Logistic regression analysis showed that an elevated NLR value was an independent predictor of MetS. The receiver operating curve analysis suggested that the optimum NLR cut-off point for MetS was 1.50 with a sensitivity of 74.6% and specificity of 52%. There is a significant relationship between NLR and MetS prevalence in patients with type 2 diabetes mellitus. NLR seems as an independent predictor of MetS in diabetic patients.



Similar content being viewed by others
References
Eckel RH, Grundy SM, Zimmet PZ. The metabolic syndrome. Lancet. 2005;365:1415–28.
Grundy SM, Cleeman JI, Daniels SR, Donato KA, Eckel RH, Franklin BA, Gordon DJ, Krauss RM, Savage PJ, Smith Jr SC, et al. Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute scientific statement. Circulation. 2005;112:2735–52.
Wilson PW, D’Agostino RB, Parise H, Sullivan L, Meigs JB. Metabolic syndrome as a precursor of cardiovascular disease and type 2 diabetes mellitus. Circulation. 2005;112:3066–72.
Marsland AL, McCaffery JM, Muldoon MF, Manuck SB. Systemic inflammation and the metabolic syndrome among middle-aged community volunteers. Metabolism. 2010;59:1801–8.
Kirilmaz B, Asgun F, Alioglu E, Ercan E, Tengiz I, Turk U, Saygi S, Ozerkan F. High inflammatory activity related to the number of metabolic syndrome components. J Clin Hypertens (Greenwich). 2010;12:136–44.
Hotamisligil GS, Shargill NS, Spiegelman BM. Adipose expression of tumor necrosis factor-alfa: direct role in obesity-linked insulin resistance. Science. 1993;259:87–91.
Balta S, Celik T, Mikhailidis DP, Ozturk C, Demirkol S, Aparci M, Iyisoy A. The relation between atherosclerosis and the neutrophil-lymphocyte ratio. Clin Appl Thromb Hemost. 2015; doi:10.1177/1076029615569568.
Gul M, Uyarel H, Ergelen M, Ugur M, Isik T, Ayhan E, Turkkan C, Aksu HU, Akgul O, Uslu N. Predictive value of neutrophil to lymphocyte ratio in clinical outcomes of non-ST elevation myocardial infarction and unstable angina pectoris: a3-year-follow-up. Clin Appl Thromb Hemost. 2014;20:378–84.
Arbel Y, Finkelstein A, Halkin A, Birati EY, Revivo M, Zuzut M, Shevach A, Berliner S, Herz I, Keren G, et al. Neutrophil/lymphocyte ratio is related to the severity of coronary artery disease and clinical outcome in patients undergoing angiography. Atherosclerosis. 2012;225:456–60.
Horne BD, Anderson JL, John JM, Weaver A, Bair TL, Jensen KR, Renlund DG, Muhlestein JB; intermountain heart collaborative study group. Which white blood cell subtypes predict increased cardiovascular risk? J Am Coll Cardiol 2005;45:1638–1643.
Buyukkaya E, Karakas MF, Karakas E, Akçay AB, Tanboga IH, Kurt M, Sen N. Correlation of neutrophil to lymphocyte ratio with the presence and severity of metabolic syndrome. Clin Appl Thromb Hemost. 2014;20:159–63.
Alberti KG, Zimmet PZ. Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med. 1998;15:539–53.
Fröhlich M, Imhof A, Berg G, Hutchinson WL, Pepys MB, Boeing H, Muche R, Brenner H, Koenig W. Association between C-reactive protein and features of the metabolic syndrome: a population-based study. Diabetes Care. 2000;23:1835–9.
Tsai JC, Sheu SH, Chiu HC, Chung FM, Chang DM, Chen MP, Shin SJ, Lee YJ. Association of peripheral total and differential leukocyte counts with metabolic syndrome and risk of ischemic cardiovascular diseases in patients with type 2 diabetes mellitus. Diabetes Metab Res Rev. 2007;23:111–8.
Festa A, D'Agostino Jr R, Tracy RP, Haffner SM. Elevated levels of acute-phase proteins and plasminogen activator inhibitor-1 predict the development of type 2 diabetes: the insulin resistance atherosclerosis study. Diabetes. 2002;51:1131–7.
Cull CA, Jensen CC, Retnakaran R, Holman RR. Impact of the metabolic syndrome on macrovascular and microvascular outcomes in type2 diabetes mellitus: United Kingdom prospective diabetes study 78. Circulation. 2007;116:2119–26.
Libby P, Ridker PM, Hansson GK. Leducq transatlantic network on atherothrombosis. Inflammation in atherosclerosis: from pathophysiology to practice. J Am Coll Cardiol. 2009;54:2129–38.
Wheeler JG, Mussolino ME, Gillum RF, Danesh J. Associations between differential leucocyte count and incident coronary heart disease: 1764 incident cases from seven prospective studies of 30 374 individuals. Eur Heart J. 2004;25:1287–92.
Kalay N, Dogdu O, Koc F, Yarlioglues M, Ardic I, Akpek M, Cicek D, Oguzhan A, Ergin A, Kaya MG. Hematologic parameters and angiographic progression of coronary atherosclerosis. Angiology. 2011;63:213–7.
Wang X, Zhang G, Jiang X, Zhu H, Lu Z, Xu L. Neutrophil to lymphocyte ratio in relation to risk of all-cause mortality and cardiovascular events among patients undergoing angiography or cardiac revascularization: a meta-analysis of observational studies. Atherosclerosis. 2014;234:206–13.
Sefil F, Ulutas KT, Dokuyucu R, Sumbul AT, Yengil E, Yagiz AE, Yula E, Ustun I, Gokce C. Investigation of neutrophil lymphocyte ratio and blood glucose regulation in patients with type 2 diabetes mellitus. J Int Med Res. 2014;42(2):581–8.
Shiny A, Bibin YS, Shanthirani CS, Regin BS, Anjana RM, Balasubramanyam M, Jebarani S, Mohan V. Association of neutrophil-lymphocyte ratio with glucose intolerance: an indicator of systemic inflammation in patients with type 2 diabetes. Diabetes Technol Ther. 2014;16(8):524–30.
Surendar J, Indulekha K, Mohan V, Pradeepa R. Association of neutrophil-lymphocyte ratio with metabolic syndrome and its components in Asian Indians (CURES-143). J Diabetes Complicat. 2016;30(8):1525–9.
Nagasawa N, Tamakoshi K, Yatsuya H, Hori Y, Ishikawa M, Murata C, Zhang H, Wada K, Otsuka R, Mabuchi T, et al. Association of white blood cell count and clustered components of metabolic syndrome in Japanese men. Circ J. 2004;68:892–7.
Shim WS, Kim HJ, Kang ES, Ahn CW, Lim SK, Lee HC, Cha BS. The association of total and differential white blood cell count with metabolic syndrome in type 2 diabetic patients. Diabetes Res Clin Pract. 2006;73:284–91.
Vishram JK, Borglykke A, Andreasen AH, Jeppesen J, Ibsen H, Jørgensen T, Palmieri L, Giampaoli S, Donfrancesco C, Kee F, et al. Impact of age and gender on the prevalence and prognostic importance of the metabolic syndrome and its components in Europeans. The MORGAM Prospective Cohort Project PLoS One. 2014;9:e107294. doi:10.1371/journal.pone.0107294.
Varol E, Bas HA, Aksoy F, Ari H, Ozaydin M. Relationship between neutrophil–lymphocyte ratio and isolated low highdensity lipoprotein cholesterol. Angiology. 2013;65:630–3.
Toth PP, Davidson MH. High-density lipoproteins: marker of cardiovascular risk and therapeutic target. J Clin Lipidol. 2010;4:359–64.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kaya, T., Solak, Y., Akçay, E.Ü. et al. The relationship between neutrophil to lymphocyte ratio and metabolic syndrome in patients with type 2 diabetes. Int J Diabetes Dev Ctries 37, 215–220 (2017). https://doi.org/10.1007/s13410-017-0550-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13410-017-0550-9