Abstract
Peptide-based vaccine delivery can be hampered by rapid peptidase activity and poor inherent immunogenicity. The self-adjuvanting lipid core peptide system (LCP) has been shown to confer improved stability and immunogenicity on peptide epitopes of group A Streptococcus, Chlamydia, hookworm, and malaria pathogens. However, various diseases, including cancer, still require targeted delivery of their vaccine candidates. For this reason, we have selected two model peptides (ovalbumin CD4+ and/or CD8+ T cell epitopes), and incorporated two or four copies of either epitope into our LCP vaccine. Optimised glycosylation of ovalbumin peptides yielded 46 % when microwave-assisted double coupling with 2 eq of carbohydrate derivative, activated by N,N-diisopropylethylamine and (O-benzotriazol-1-yl)-N,N,N′,N′-tetramethyluronium hexafluorophosphate, was performed. All ovalbumin peptides were successfully synthesised and purified in 11–55 % yields by Fmoc- or Boc-chemistry using solid-phase peptide synthesis. The mannosylated ovalbumin peptides were nontoxic to human erythrocytes in haemolytic assay (<2 % haemolysis) and showed increased (up to 20-fold) stability in plasma.
Similar content being viewed by others
Introduction
A large number of potent and highly specific therapeutic peptides and proteins have been found that have the potential to cure or prevent a variety of diseases [1–3]. Synthetic subunit peptide vaccines are popular due to their safety, ease of large-scale production, purity and lack of side effects when compared to whole-organism vaccines. However, peptide antigens are generally unstable in vivo and have limited immunogenicity because they do not stimulate an innate immune response. The immunostimulatory properties of peptide vaccines can be improved by co-administration with an adjuvant, and/or incorporation into a self-adjuvanting delivery system. Many strong adjuvants are used in animal models, but are too toxic for use in humans. Aluminium-based adjuvants are one of the few adjuvants licensed for human application, though they are quite weak and unstable [4]. Recently, other adjuvants, such as MF59, ASO4 and virosomes, have also been used in vaccine delivery [5].
The lipid core peptide (LCP) system was designed to be a self-adjuvanting delivery system, avoiding the need for a conventional adjuvant. The LCP system is composed of lipoamino acids (α-amino acids with long alkyl side chains) and a polylysine, or carbohydrate core, providing branching for attachment of multiple copies of peptide antigens [6]. LCP vaccines can be readily synthesised by solid-phase peptide synthesis (SPPS), a common technique for peptide production. The efficacy of the LCP system has previously been demonstrated in animal models against Chlamydia [7], group A Streptococcus [8], hookworm [9], and malaria [10]. While many advantages have been described about the lipidation of peptides, increased lipophilicity leads to poor water solubility, an important factor in vaccine delivery [6]. Glycosylation of peptides has been reported to improve their stability and uptake, as well as enhance water solubility, transport across biological barriers [11] and allow targeting to specific sites [12–15].
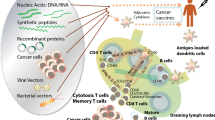
The delivery of compounds to antigen presenting cells within distinct tissues is highly desirable. The synthesised compounds were designed to target dendritic cells (DCs), which are important antigen presenting cells, with key roles in the initiation and regulation of immune responses [16]. They have the ability to capture and present pathogen and tumour antigens to CD4+ and CD8+ T cells [17]. In addition, the LCP motif on our compounds acts as toll-like receptor 2 ligand, which helps DCs to optimise antigen presentation to T cells [18]. It was demonstrated that glycosylated compounds can target DCs in vitro, using mannose receptors located on the DCs [19, 20]. Immune responses were reported to be higher when nanogel particles, carrying an ovalbumin (OVA) vaccine cargo, were decorated with the mannose-targeting ligand [21].
OVA peptides have been used as model peptides in a wide range of studies [21–24]. Vaccines are often designed to include a CD4+ T cell helper epitope, as they are known to improve or be necessary for optimal CD8+ T cell activity [25]. It has been demonstrated that a class I major histocompatibility complex (MHC) bound OVA257-264 peptide can induce a strong cytolytic CD8+ T cell response [26]. OVA323–339 has been used extensively to study the nature of class II MHC–peptide binding and T cell activation [27, 28]. Therefore, we selected both ovalbumin peptides (OVA257–264 and OVA323–339) for our study, and combined them with the self-adjuvanting LCP core and a mannose receptor-targeting unit.
Materials and methods
Materials
Peptide synthesis solvents, dimethylformamide (DMF), dichloromethane (DCM), methanol and reagents, trifluoroacetic acid (TFA), N,N-diisopropylethylamine (DIPEA), hydroxybenzotriazole (HOBt) and 1-hydroxy-7-azabenzotriazole (HOAt) were purchased from Auspep (Melbourne, VIC, Australia). (O-Benzotriazol-1-yl)-N,N,N′,N′-tetramethyluronium hexafluorophosphate (HBTU), O-(7-azabenzotriazol-1-yl)-N,N,N′,N′-tetramethyluronium hexafluorophosphate (HATU) and di-tert-butyl dicarbonate (Boc2O) were obtained from GL Biochem Ltd (Shanghai, China). N α-tert-Butyloxycarbonyl (Boc)-protected and 9-fluorenylmethoxycarbonyl (Fmoc)-protected amino acids, 4-methyl benzhydrylamine (pMBHA) and Rink amide MBHA resins were supplied by Novabiochem (Läufelfingen, Switzerland). Palladium (10 % wt on carbon) was purchased from Lancaster Synthesis (Lancashire, England). Sodium dodecyl sulfate (SDS), diisopropylcarbodiimide (DIC) and dicyclohexanecarbodiimide (DCC) were purchased from Sigma-Aldrich (St. Louis, USA). Ninety-six well plates were obtained from Corning® Costar® (Tewksbury, Massachusetts, USA) in sterile condition. Ultra-pure gases (N2, H2, Ar) were supplied by BOC Gases (Brisbane, QLD, Australia). Silica for flash chromatography (Silica gel 60, 230–400 mesh) was obtained from Lomb Scientific (Taren Point, NSW, Australia). Deuterated solvents (d 1-CDCl3 and DMSO-d 6) were manufactured by Cambridge Isotope Laboratories Inc. (Andover, MA, USA). All other reagents were purchased in analytical grade or higher purity from Sigma-Aldrich (Castle Hill, VIC, Australia) or Merck Pty (Kilsyth, VIC, Australia). Solvents were freshly distilled and dried prior to use, and all moisture-sensitive reactions were carried out under inert atmosphere (N2/Ar) using oven-dried glassware.
General methods
Electrospray ionisation mass spectra (ESI-MS) were obtained from a triple-quadrupole electrospray instrument (PerkinElmer Sciex API 3000) in positive ion mode using Analyst 1.4 software (Applied Biosystems/MDS Sciex, Toronto, Canada). NMR spectra were recorded on a Bruker AM 300 MHz instrument, using CDCl3 as a deuterated solvent, with tetramethylsilane as an internal standard, at 297 K. Coupling constants are given in hertz (Hz). Analytical reverse phase high-pressure liquid chromatography (RP-HPLC) was performed on a Shimadzu instrument (Kyoto, Japan; LC-10AT liquid chromatograph, SCL-10A system controller, SPD-6A UV detector, SIL-6B auto injector with a SCL-6B system controller; LabSolutions software), and C18 and C4 Grace Vydac® columns (Columbia, Maryland, USA; 10 μm, 4.6 mm internal diameter (i.d.) × 250 mm) using a linear gradient of 0–100 % of CH3CN/10 % water/0.1 % TFA (solvent B) and water/0.1 % TFA (solvent A) for 30 min, with a 1 mL/min flow rate and detection at 214 nm, unless otherwise stated. Semi-preparative RP-HPLC was performed using a Waters Delta 600 system (Milford, Massachusetts, USA; model 600 controller, 490E UV detector). Purifications were performed on Vydac® C4 or C18 preparative columns (10 μm, 22 mm i.d. × 250 mm) using a gradient of solvent B as listed below with 10 mL/min flow rate, and detection at 230 nm. Fractions containing pure compound were pooled and lyophilised overnight.
Synthesis
Solid-phase peptide synthesis
SPPS was assisted by a microwave peptide synthesiser (Discover Solid-Phase Synthesis, CEM A.I. Scientific) at 70 °C, 20 W and/or manual shaker (Shaker WS/180°, Glas-Col). In the case of the HAAH peptide sequence, manual shaking at room temperature for 1 h was performed to avoid racemisation.
For Fmoc-chemistry (OVA peptides), Rink amide MBHA resin (substitution ratio: 0.60 mmol/g) was swelled in DMF for 90 min. Each amino acid coupling consisted of microwave-assisted Fmoc-deprotection with piperidine (20 % in DMF) (2 × 5 min), 1 min DMF flow wash, followed by 10 min microwave-assisted coupling of pre-activated amino acid.
For Boc-chemistry (LCP peptides), pMBHA resin (substitution ratio: 0.45 mmol/g) was swelled in DMF for 90 min. Each amino acid coupling cycle consisted of Boc-deprotection with neat TFA (2 × 1 min), a 1 min DMF flow wash, followed by 10 min microwave-assisted coupling of pre-activated amino acid.
An activated mixture consisted of Boc- or Fmoc-amino acid (4.2 eq per mol amino-group), HBTU (4.0 eq) and DIPEA (6.2 eq). Upon completion of synthesis and removal of the terminal Boc or Fmoc groups (and acetylation of N-terminal amine group in cases where no other couplings were to be performed), the resin was washed with DMF, CH2Cl2 and MeOH, and dried in vacuo.
The crude peptides prepared by Fmoc-chemistry were cleaved from the resin using a 3-h incubation with TFA/triisopropyl silane: H2O (95:2.5:2.5). The crude peptides prepared by Boc-chemistry were cleaved from the resin using hydrofluoric acid at −10 to −5 °C, with p-cresol as scavenger. All cleaved peptides were precipitated, filtered and washed thoroughly with ice-cold diethyl ether. The precipitated compounds were dissolved in CH3CN/water/TFA and lyophilised overnight to give amorphous powders. All crude peptides (Table 1) were analysed and purified by RP-HPLC as described above.
Carbohydrate coupling to peptidyl resin
4-Oxo-4-[(2,3,4,6-tetra-O-acetyl-β-D-glucopyranosyl)-amino]-butanoic acid (2 eq in 1 mL DMF) was activated with one of the coupling reagents, HBTU, DIC, DIC and HOBt, DIC and HOAt, HATU, cyanuric chloride, 2,4-dimethoxy-6-(N-ethyl-morpholine)-triazene, or DCC and pentafluorophenol (1.9 eq in 1 mL DMF), and DIPEA (2.1 eq). The entire mixture was added to a microwave vessel containing resin-bound peptide with the terminal amine deprotected, and reacted in the microwave-assisted synthesiser for 15 min at 70 °C.
For screening of coupling conditions, only HBTU was used as the coupling reagent. Mechanism of coupling glucose succinate to deprotected OVA323–339-resin is shown in Scheme 1. The equivalents of the carbohydrate for each experiment were varied from 1.1 to 3 eq, and the equivalents of HBTU and DIPEA were determined based on that of the carbohydrate (eq of HBTU = 0.95 × eq of sugar; eq of DIPEA = 1.05 × eq of sugar). All manual couplings were carried out at room temperature, while all microwave-assisted couplings were performed at 70 °C, and coupling times ranged from 15 min to 16 h. Deacetylation of the products was achieved by shaking the product resin (2 × 30 min) with 75 % hydrazine hydrate in methanol or by Zemplen deacetylation using 1 M sodium methoxide in methanol. Once optimised with a glucose derivative, 4-oxo-4-[(2,3,4,6-tetra-O-acetyl-β-D-mannopyranosyl)-amino]-butanoic acid was used to prepare the mannosylated ovalbumin peptides. The resin was washed consecutively with DMF, DCM and MeOH and left to dry under vacuum overnight. The glycopeptides (Table 1) were cleaved from the resin, analysed, and purified according to the protocol above.
In vitro assays
Haemolytic assay
A haemolytic assay was used to quantify the membrane-damaging properties of the synthesised peptides. The blood was collected from healthy adult volunteers and treated with heparin. Human erythrocytes were isolated by centrifugation at 3,000 rpm for 15 min (Sigma 2–5 centrifuge, Sigma Laborzentrifugen GmbH, Osterode am Harz, Germany). The pellet was washed four times with an isotonic phosphate-buffered saline (PBS), pH 7.4 (Gibco-BRL, Grand Island, NY, USA), centrifuged at 3,000 rpm for 15 min and re-suspended in the same buffer. The erythrocyte pellet was diluted in PBS to a final concentration of 4 % (v/v) erythrocytes. This stock solution was always freshly prepared and used within 24 h.
Three concentrations (10, 50 and 100 μM) of the test compounds (100 μL) were transferred into the 96-well flat-bottom microtiter plates (TPP, Zurich, Switzerland) and incubated at 37 °C for 1 h on a Titramax 1000 vibrating shaker (Heidolph, Schwabach, Germany). The red blood cell (erythrocyte) suspensions (100 μL) were added to each well on the plate and incubated for 1 h at 37 °C with constant shaking. The plates were centrifuged at 2,400 rpm for 15 min to separate the red blood cells from the supernatant. The supernatant (75 μL) was transferred into a new 96-well plate, and the absorbance of each sample was recorded at 540 nm using a SpectraMax 250-microplate reader (Molecular Devices, Sunnyvale, CA, US) to determine the release of haemoglobin. Each experiment was performed in triplicate. SDS (10 mM) in PBS, and PBS alone, were used as positive and negative controls, respectively.
Haemolytic assays were performed with the approval of the University of Queensland Ethics Committee (no. 2009000661), and all procedures were performed using a Biological Safety cabinet (Nuaire) in sterile conditions.
Plasma stability assay
The plasma stability assay was performed using fresh blood taken from a healthy human volunteer and collected in 2 × 10 mL Li-heparin tubes (anticoagulant). The collected blood was spun several times using Sigma centrifuge (2,400 rpm, 15 min) with PBS. After washing, the plasma was transferred to a new tube and the red blood cell suspension was discarded. A solution of a test compound (1 mg/mL in PBS, 300 μL) was mixed with plasma (300 μL) at 37 °C, and the mixture was incubated at 37 °C for 120 min. At pre-determined time intervals (0, 5, 10, 15, 20, 30, 60 and 120 min), 50 μL of plasma solution was removed and placed on ice. Cold acetonitrile (75 μL) was added to precipitate the plasma proteins. All experiments were performed in triplicate. After centrifugation (10,000 rpm, 10 min), 100 μL of supernatant was collected and analysed via analytical RP-HPLC. The degradation profiles of the compounds were obtained by plotting the percentage of peptide remaining in solution over time. The plasma stability assays were performed with the approval of The University of Queensland Ethics Committee (no. 2009000661).
Results and discussion
Design and synthesis
To synthesise a vaccine candidate with a built-in adjuvant and a targeting unit, two/four copies of the ovalbumin peptide OVA257–264 and/or OVA323–339 epitopes were coupled to the LCP system, with the mannose derivative attached at the N-terminus of the peptide sequences (Table 1). The lipidic adjuvanting moiety of the vaccine candidates, consisting of three synthetic lipoamino acids with two glycine spacers, was synthesised by stepwise SPPS using Boc-chemistry and pMBHA resin. The lipoamino acid, Boc-C16 (2-(t-butoxycarbonylamino)-D,L-octadecanoic acid), was prepared from diethylacetamido malonate, bromotetradecane and di-tert-butyldicarbonate [29]. To investigate the activation of different T cell subsets, the LCP compounds contained both OVA257–264 (SIINFEKL) and OVA323–339 (ISQAVHAAHAEINEAGR) peptide epitopes and the lipid moiety incorporated into one compound.
Glycosylated ovalbumin lipopeptide constructs (Table 1) were designed to target mannose receptors on DCs. This is a well-validated approach for delivering vaccines to DCs [20], and was successfully employed in the past [19]. Carbohydrate derivatives were synthesised starting from glycosyl azides, which were converted into amines and coupled to succinic acid. In order to optimise the coupling of the sugar moiety to the peptide, per-acetylated glucose succinate was prepared according to Kellam et al. [30]. Per-acetylated mannose succinate was synthesised similarly [19] and used for glycosylation of the N-terminus of the ovalbumin peptides and LCPs.
Control peptides, OVA257–264 and OVA323–339, were synthesised by microwave-assisted SPPS on Rink amide MBHA resin. Couplings were performed with Fmoc-protected amino acids activated with DIPEA and HBTU. Manual coupling at room temperature (no microwave) was used in the case of OVA323–339 for the HAAH sequence to avoid racemisation of histidine [31]. For the synthesis of compounds containing both epitopes, Boc/Fmoc-Lys strategy was applied. Two copies of OVA257–264 were first attached to LCP, or Lys3, followed by acetylation at their N-termini. Subsequently, after Boc-deprotection of the branching lysine residue, two copies of OVA323–339 were synthesised and mannose succinate was attached to their N-termini (Table 1).
All crude compounds, obtained after hydrofluoric acid (LCPs made by Boc-chemistry) or TFA (peptides made by Fmoc-chemistry) cleavage, were purified by RP-HPLC using C-18 or C-4 column. The lyophilised peptides were obtained in 11–55 % yields, characterised by ESI-MS and their purity confirmed by RP-HPLC (Table 2).
Optimisation of coupling carbohydrate to a peptide and subsequent deacetylation
Previous studies have shown that N-terminal glycosylation of peptides can proceed in low yield [32]. In order to improve the glycosylation yields, coupling of the carbohydrate to the peptide was optimised using glucose succinate and OVA323–339 (Scheme 1). Glucose succinate was co-evaporated three times with toluene in order to remove the excess of acetic acid present from the previous purification. Omission of the co-evaporation step resulted in formation of an acetylated OVA323–339 peptide (tR 16.34 min; C18 column, 0–100 %), thus termination of glycosylation. For glycosylation optimisation, the coupling conditions were kept the same (2 eq glucose succinate, 1.9 eq coupling reagent, 2.1 eq DIPEA, microwave-assisted, 15 min, 70 °C), while a range of coupling reagents were screened (Table 3). HBTU emerged as the coupling reagent of choice because it resulted in the greatest amount (29 % yield) of the coupled product, GlcOVA323–339. Using HBTU, the glycosylation yield was more than 1.5 times higher than the next best coupling reagent, HATU, which gave only 18 %.
Having determined the most efficient coupling reagent (HBTU), the conditions employed were varied so that the most efficient coupling conditions could be established. Both manual and microwave-assisted couplings were carried out, with various reaction times (15 min–16 h). The equivalents of the sugar (glucose succinate) were varied (1.1–3), and double and triple couplings were performed (Fig. 1).
Different reaction conditions for glucose succinate coupling to OVA323–339 and their influence on the product formation (yield); this graph also demonstrates the amount of impurities present in the reaction mixtures based on HPLC chromatograms after GlcOVA323–339 cleavage from the resin. Coupling reagent: HBTU (eq = 0.95 × eq of sugar), DIPEA (eq = 1.05 × eq of sugar); manual couplings were performed at room temperature; microwave-assisted (MW) couplings performed at 70 °C
After manual coupling for 6 h (conditions 1), 12 % of the product was obtained, with 24 % of starting material remaining. When the duration of coupling was extended to 16 h (conditions 2), little of the starting material remained. However, this did not result in a large increase in the amount of desired product present (19 %). Microwave-assisted coupling gave cleaner conversion to the desired product. However, when coupling times were increased from 15 to 30 min, to 1 h, both the amount of starting material and product decreased sequentially (conditions 3, 4 and 5), which may be attributed to their decomposition. This trend was also observed with the analogous double-coupling experiments (conditions 8, 9 and 10). Carrying out the coupling reaction three times (conditions 11) gave the highest quantity (46 %) of the desired GlcOVA323–339, but this was not significantly better than the analogous double coupling (conditions 8; 45 %). Therefore, in cases where the sugar moiety is of high value, double coupling may be the appropriate option.
While the glycopeptide was attached to the resin, hydrazine hydrate in methanol was used to perform the final deacetylation step for the mannose moiety of the glycosylated peptides [33]. Alternatively, deacetylation could be performed in solution after cleavage of the glycosylated peptides from the resin by Zemplen transesterification method, using sodium methoxide in methanol. We compared both methods, and, in agreement with Liu et al. [34], we found the hydrazine hydrate deacetylation of our resin-bound glycopeptide (GlcOVA323–339) to be better, since it gave fewer by-products (data not shown).
In vitro assays
Toxicity evaluation
A haemolytic assay was performed using a human erythrocyte model (a commonly used model for investigating membrane interactions) to investigate and quantify the effect of the ovalbumin peptides on the cell membrane. The release of haemoglobin is easily measured by absorbance reading at 540 nm after exposure of the erythrocytes to the compound of interest. Haemolytic lysis of human red blood cells was measured after the cells were incubated at 37 °C for 1 h with three different concentrations of the test compounds. Erythrocytes treated with PBS and SDS were used as negative and positive controls (0 and 100 % of lysis, respectively). The maximum haemolysis (<2 %) was detected at 100 μM, the standard concentration used in vaccine delivery (Fig. 2). According to Amin and Dannenfelser, these values are considered to be non-haemolytic [35].
Human plasma stability of ovalbumin peptides
Incubation of ovalbumin peptides with human plasma revealed improved stability of modified ovalbumins, ManOVA323–339 and (OVA257–264)2(ManOVA323–339)2Lys3. The OVA323–339 degraded rapidly (t1/2 = 1.2 min), whereas its glycosylated form, ManOVA323–339, showed almost a 20-fold improvement in stability, with a half-life of 23.2 min (Fig. 3). Even though the stability of the branched (OVA257–264)2(ManOVA323–339)2Lys3 was the highest (61 %) compared to ManOVA323–339 (41 %) and OVA323–339 (11 %) at 120 min, its half-life was t1/2 = 13.3 min. The shorter half-life might be attributed to the second peptide epitope OVA257–264 and the charged Lys3 moiety. The half-life of the (OVA257–264)2(ManOVA323–339)2Lys3 peptide represents an 11-fold stability enhancement compared to the parent peptide. In order to properly evaluate the stability of the tested compounds, we used a peptide concentration of 1 mg/mL in PBS, so as to reach a sufficient absorbance on RP-HPLC at 214 nm. However, this concentration was too high for the LCP compounds to be dissolved.
Conclusion
A series of ovalbumin peptides was successfully synthesised by Fmoc- and Boc-chemistry and SPPS in 11–55 % yields. Based on the data obtained from the sugar coupling optimisation, we recommend using 2 × 2 eq carbohydrate coupling steps, 1.9 eq HBTU, 2.1 eq DIPEA and 15 min microwave-assisted coupling to an ovalbumin peptide. This condition provided high yield of glycosylated product, and can be applied to glycosylation of other peptides, with a variety of carbohydrates. The mannosylated ovalbumin peptides did not lyse human erythrocytes when tested in vitro using haemolytic assay and showed an increased stability in plasma. This approach is likely to offer a new strategy to target vaccines and drugs to immune cells. Glycosylated and lipidated ovalbumin peptides were designed and synthesised in order to study the specific targeting towards mannose receptors on dendritic cells. An extended study will be performed to examine the delivery of these compounds to dendritic cells in vivo. The use of the carbohydrate-modified LCP delivery system could be applied to target different cells and deliver a variety of peptides.
References
Goodwin D, Simerska P, Toth I. Peptides as therapeutics with enhanced bioactivity. Curr Med Chem. 2012;19(26):4451–61.
Steinberg M. Degarelix: a gonadotropin-releasing hormone antagonist for the management of prostate cancer. Clin Ther. 2009;31:2312–31. doi:10.1016/J.Clinthera.2009.11.009.
Bray BL. Large-scale manufacture of peptide therapeutics by chemical synthesis. Nat Rev Drug Discov. 2003;2(7):587–93. doi:10.1038/nrd1133.
Peek LJ, Middaugh CR, Berkland C. Nanotechnology in vaccine delivery. Adv Drug Deliv Rev. 2008;60(8):915–28. doi:10.1016/J.Addr.2007.05.017.
Leroux-Roels G. Unmet needs in modern vaccinology: adjuvants to improve the immune response. Vaccine. 2010;28 Suppl 3:C25–36. doi:10.1016/j.vaccine.2010.07.021.
Simerska P, Moyle PM, Toth I. Modern lipid-, carbohydrate-, and peptide-based delivery systems for peptide, vaccine, and gene products. Med Res Rev. 2011;31(4):520–47. doi:10.1002/med.20191.
Zhong G, Toth I, Reid R, Brunham RC. Immunogenicity evaluation of a lipidic amino acid-based synthetic peptide vaccine for Chlamydia trachomatis. J Immunol. 1993;151(7):3728–36.
Simerska P, Abdel-Aal AB, Fujita Y, Batzloff MR, Good MF, Toth I. Synthesis and in vivo studies of carbohydrate-based vaccines against group A Streptococcus. Biopolymers. 2008;90(5):611–6.
Skwarczynski M, Dougall AM, Khoshnejad M, Chandrudu S, Pearson MS, Loukas A, et al. Peptide-based subunit vaccine against hookworm infection. Plos One. 2012;7(10):e46870. doi:10.1371/journal.pone.0046870.
Apte SH, Groves PL, Skwarczynski M, Fujita Y, Chang CH, Toth I et al. Vaccination with lipid core peptides fails to induce epitope-specific T cell responses but confers non-specific protective immunity in a malaria model. Plos One. 2012;7(8). doi: ARTN e40928 doi 10.1371/journal.pone.0040928.
Ross BP, Braddy AC, McGeary RP, Blanchfield JT, Prokai L, Toth I. Micellar aggregation and membrane partitioning of bile salts, fatty acids, sodium dodecyl sulphate, and sugar-conjugated fatty acids: correlation with haemolytic potency and implications for drug delivery. Mol Pharm. 2004;1(3):233–45.
Nomoto M, Yamada K, Haga M, Hayashi M. Improvement of intestinal absorption of peptide drugs by glycosylation: transport of tetrapeptide by the sodium ion-dependent D-glucose transporter. J Pharm Sci. 1998;87(3):326–32.
Drouillat B, Hillery AM, Dekany G, Falconer R, Wright K, Toth I. Novel liposaccharide conjugates for drug and peptide delivery. J Pharm Sci. 1998;87(1):25–30.
Koda Y, Del Borgo M, Wessling ST, Lazarus LH, Okada Y, Toth I, et al. Synthesis and in vitro evaluation of a library of modified endomorphin 1 peptides. Bioorg Med Chem. 2008;16(11):6286–96. doi:10.1016/j.bmc.2008.04.020.
Keler T, Ramakrishna V, Fanger MW. Mannose receptor-targeted vaccines. Expert Opin Biol Ther. 2004;4(12):1953–62. doi:10.1517/14712598.4.12.1953.
Platt CD, Ma JK, Chalouni C, Ebersold M, Bou-Reslan H, Carano RA, et al. Mature dendritic cells use endocytic receptors to capture and present antigens. Proc Natl Acad Sci U S A. 2010;107(9):4287–92. doi:10.1073/pnas.0910609107.
Banchereau J, Briere F, Caux C, Davoust J, Lebecque S, Liu YT, et al. Immunobiology of dendritic cells. Annu Rev Immunol. 2000;18:767–811.
Phillipps KSM, Wykes MN, Liu XQ, Brown M, Blanchfield JT, Toth I. A novel synthetic adjuvant enhances dendritic cell function. Immunology. 2009;128(1pt2):e582–8. doi:10.1111/j.1365-2567.2008.03038.x.
Moyle PM, Olive C, Ho MF, Pandey M, Dyer J, Suhrbier A, et al. Toward the development of prophylactic and therapeutic human papillomavirus type-16 lipopeptide vaccines. J Med Chem. 2007;50(19):4721–7.
Irache JM, Salman HH, Gamazo C, Espuelas S. Mannose-targeted systems for the delivery of therapeutics. Expert Opin Drug Deliv. 2008;5(6):703–24. doi:10.1517/17425240802168025.
Thomann-Harwood LJ, Kaeuper P, Rossi N, Milona P, Herrmann B, McCullough KC. Nanogel vaccines targeting dendritic cells: contributions of the surface decoration and vaccine cargo on cell targeting and activation. J Control Release. 2013;166(2):95–105. doi:10.1016/j.jconrel.2012.11.015.
Sun LZ, Elsayed S, Aasen TB, Van Do T, Aardal NP, Florvaag E, et al. Comparison between ovalbumin and ovalbumin peptide 323–339 responses in allergic mice: humoral and cellular aspects. Scand J Immunol. 2010;71(5):329–35. doi:10.1111/J.1365-3083.2010.02382.X.
Yuba E, Harada A, Sakanishi Y, Watarai S, Kono K. A liposome-based antigen delivery system using pH-sensitive fusogenic polymers for cancer immunotherapy. Biomaterials. 2013;34(12):3042–52. doi:10.1016/j.biomaterials.2012.12.031.
Burgdorf S, Kautz A, Bohnert V, Knolle PA, Kurts C. Distinct pathways of antigen uptake and intracellular routing in CD4 and CD8 T cell activation. Science. 2007;316(5824):612–6. doi:10.1126/Science.1137971.
Bourgeois C, Tanchot C. CD4 T cells are required for CD8 T cell memory generation. Eur J Immunol. 2003;33(12):3225–31. doi:10.1002/Eji.200324576.
Lipford GB, Hoffman M, Wagner H, Heeg K. Primary in vivo responses to ovalbumin: probing the predictive value of the Kb binding motif. J Immunol. 1993;150(4):1212–22.
Bickert T, Wohlleben G, Brinkman M, Trujillo-Vargas CM, Ruehland C, Reiser COA, et al. Murine polyomavirus-like particles induce maturation of bone marrow-derived dendritic cells and proliferation of T cells. Med Microbiol Immunol. 2007;196(1):31–9. doi:10.1007/S00430-006-0026-X.
Szymczak-Workman AL, Workman CJ, Vignali DAA. Cutting edge: regulatory T cells do not require stimulation through their TCR to suppress. J Immunol. 2009;182(9):5188–92. doi:10.4049/Jimmunol.0903123.
Gibbons WA, Hughes RA, Charalambous M, Christodoulou M, Szeto A, Aulabaugh AE, et al. Lipidic peptides I. Synthesis, resolution and structural elucidation of lipidic amino acids and their homo- and hetero-oligomers. Liebigs Ann Chem. 1990;12:1175–83.
Kellam B, Drouillat B, Dekany G, Starr MS, Toth I. Synthesis and in vitro evaluation of lipoamino acid and carbohydrate-modified enkephalins as potential antinociceptive agents. Int J Pharm. 1998;161(1):55–64.
Collins JM, Leadbeater NE. Microwave energy: a versatile tool for the biosciences. Org Biomol Chem. 2007;5(8):1141–50. doi:10.1039/b617084f.
Varamini P, Mansfeld FM, Blanchfield JT, Wyse BD, Smith MT, Toth I. Synthesis and biological evaluation of an orally active glycosylated endomorphin-1. J Med Chem. 2012;55(12):5859–67. doi:10.1021/Jm300418d.
Bardaji E, Torres JL, Clapes P, Albericio F, Barany G, Rodriguez RE, et al. Synthesis and biological activity of O-glycosylated morphiceptin analogues. J Chem Soc Perkin Trans 1. 1991;0(7):1755–9.
Liu M, Barany G, Live D. Parallel solid-phase synthesis of mucin-like glycopeptides. Carbohydr Res. 2005;240(13):2111–22.
Amin K, Dannenfelser RM. In vitro hemolysis: guidance for the pharmaceutical scientist. J Pharm Sci. 2006;95(6):1173–6. doi:10.1002/jps.20627.
Acknowledgments
We acknowledge the Australian Research Council for their support of this work with the Discovery Project grant DP1092829, Professorial Research Fellowship to I.T. (DP110100212), and an Australian Postdoctoral Fellowship to P.S. (DP1092829). The sugar coupling optimisation protocol was supported by the National Health and Medicinal Research Council APP1026488. We thank Angeline Chan, Emma Sierecki and Tittaya Suksamran for their help with preparation of some peptide constructs and to Abdul Kader Shabbir for help with in vitro assays. Pavla Simerska, Zyta Ziora, Vincent Fagan, Daryn Goodwin, Farrah Edrous and Istvan Toth declare that they have no conflict of interest.
All institutional and national guidelines for the care and use of laboratory animals were followed. The haemolytic assays and plasma stability assays were performed with the approval of The University of Queensland Ethics Committee (no. 2009000661).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Simerska, P., Ziora, Z.M., Fagan, V. et al. Design, synthesis and characterisation of mannosylated ovalbumin lipid core peptide self-adjuvanting vaccine delivery system. Drug Deliv. and Transl. Res. 4, 246–255 (2014). https://doi.org/10.1007/s13346-013-0173-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-013-0173-8