Abstract
Background
Iron deficiency anemia (IDA) is a common complication of inflammatory bowel disease (IBD). Oral ferric maltol improves and normalizes hemoglobin (Hb) in patients with IBD.
Aim
This open-label, randomized Phase 1 study evaluated the pharmacokinetics of ferric maltol and its effect on iron indices in IBD patients with iron deficiency (with or without anemia).
Methods
Iron deficient adult IBD patients received ferric maltol 30, 60, or 90 mg twice daily during an 8-day period. Pharmacokinetics and iron uptake were assessed on days 1 and 8.
Results
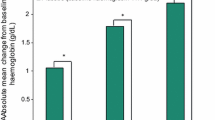
Twenty-four patients were included: 13 with Crohn’s disease and 11 with ulcerative colitis (mean age 39 years; 67 % female, mean Hb 13.0 g/dL; mean reticulocyte Hb content (CHr) 31.9 pg; mean ferritin 13.9 µg/L). Plasma maltol and maltol glucuronide increased rapidly at all doses, reaching maximum plasma concentration (C max) 1.0–1.5 h post-dose and declining to baseline after 3–6 h. Maltol and maltol glucuronide exposure (area under the concentration–time curve; AUC) appeared dose proportional with twice-daily dosing, with higher exposure to maltol glucuronide vs. maltol. Mean day 8/day 1 ratios for C max and AUC0–t indicated no accumulation after 7 days of twice-daily dosing. Serum iron and transferrin saturation (TSAT) increased with all doses (maximum values at 1.5–3.0 h post-dose). Serum ferritin and CHr increased by day 8, with greater improvements with 60 and 90 mg twice-daily doses than with 30 mg twice-daily doses.
Conclusions
The key constituents of ferric maltol showed predictable pharmacokinetics, with no accumulation over 7 days and increased iron uptake and storage over time at 30–90 mg twice-daily doses.




Similar content being viewed by others
References
Goldberg ND. Iron deficiency anemia in patients with inflammatory bowel disease. Clin Exp Gastroenterol. 2013;6:61–70.
Kulnigg S, Gasche C. Systematic review: managing anaemia in Crohn’s disease. Aliment Pharmacol Ther. 2006;24(11–12):1507–23.
Gasche C, Lomer MC, Cavill I, Weiss G. Iron, anaemia, and inflammatory bowel diseases. Gut. 2004;53(8):1190–7.
Bergamaschi G, Di Sabatino A, Albertini R, Ardizzone S, Biancheri P, Bonetti E, et al. Prevalence and pathogenesis of anemia in inflammatory bowel disease. Influence of anti-tumor necrosis factor-alpha treatment. Haematologica. 2010;95(2):199–205.
Wiesenthal M, Dignass A, Hartmann F, Iqbal T, Stein J. Serum hepcidin levels predict intestinal iron absorption in IBD patients. Poster presentation P.139. European Crohn’s & Colitis Organisation (ECCO). 2014. https://www.ecco-ibd.eu/index.php/publications/congress-abstract-s/abstracts-2014/item/p139-serum-hepcidin-levels-predict-intestinal-iron-absorption-in-ibd-patients.html. Accessed 7 July 2015.
Wilson A, Reyes E, Ofman J. Prevalence and outcomes of anemia in inflammatory bowel disease: a systematic review of the literature. Am J Med. 2004;116(Suppl 7A):44S–9S.
Stein J, Dignass AU. Management of iron deficiency anemia in inflammatory bowel disease—a practical approach. Ann Gastroenterol. 2013;26(2):104–13.
de Silva AD, Tsironi E, Feakins RM, Rampton DS. Efficacy and tolerability of oral iron therapy in inflammatory bowel disease: a prospective, comparative trial. Aliment Pharmacol Ther. 2005;22(11–12):1097–105.
Erichsen K, Hausken T, Ulvik RJ, Svardal A, Berstad A, Berge RK. Ferrous fumarate deteriorated plasma antioxidant status in patients with Crohn disease. Scand J Gastroenterol. 2003;38(5):543–8.
Kawai M, Sumimoto S, Kasajima Y, Hamamoto T. A case of ulcerative colitis induced by oral ferrous sulfate. Acta Paediatr Jpn. 1992;34(4):476–8.
Zhu A, Kaneshiro M, Kaunitz JD. Evaluation and treatment of iron deficiency anemia: a gastroenterological perspective. Digest Dis Sci. 2010;55(3):548–59.
Van Assche G, Dignass A, Bokemeyer B, Danese S, Gionchetti P, Moser G, et al. Second European evidence-based consensus on the diagnosis and management of ulcerative colitis part 3: special situations. J Crohn’s Colitis. 2013;7(1):1–33.
Lund EK, Wharf SG, Fairweather-Tait SJ, Johnson IT. Oral ferrous sulfate supplements increase the free radical-generating capacity of feces from healthy volunteers. Am J Clin Nutr. 1999;69(2):250–5.
Keating GM. Ferric carboxymaltose: a review of its use in iron deficiency. Drugs. 2014;75(1):101–27.
Gasche C, Ahmad T, Tulassay Z, Baumgart DC, Bokemeyer B, Buning C, et al. Ferric maltol is effective in correcting iron deficiency anemia in patients with inflammatory bowel disease: results from a phase-3 clinical trial program. Inflamm Bowel Dis. 2015;21(3):579–88.
Levey JA, Barrand MA, Callingham BA, Hider RC. Characteristics of iron(III) uptake by isolated fragments of rat small intestine in the presence of the hydroxypyrones, maltol and ethyl maltol. Biochem Pharmacol. 1988;37(10):2051–7.
Barrand MA, Callingham BA, Dobbin P, Hider RC. Dissociation of a ferric maltol complex and its subsequent metabolism during absorption across the small intestine of the rat. Br J Pharmacol. 1991;102(3):723–9.
Barrand MA, Callingham BA. Evidence for regulatory control of iron uptake from ferric maltol across the small intestine of the rat. Br J Pharmacol. 1991;102(2):408–14.
Kelsey SM, Hider RC, Bloor JR, Blake DR, Gutteridge CN, Newland AC. Absorption of low and therapeutic doses of ferric maltol, a novel ferric iron compound, in iron deficient subjects using a single dose iron absorption test. J Clin Pharm Ther. 1991;16(2):117–22.
Kelsey SM, Blake DR, Hider RC, Gutteridge CN, Newland AC. Absorption of ferric maltol, a novel ferric iron compound, in iron-deficient subjects. Clin Lab Haematol. 1989;11(3):287–8.
Barrand MA, Callingham BA, Hider RC. Effects of the pyrones, maltol and ethyl maltol, on iron absorption from the rat small intestine. J Pharm Pharmacol. 1987;39(3):203–11.
Harvey RS, Reffitt DM, Doig LA, Meenan J, Ellis RD, Thompson RP, et al. Ferric trimaltol corrects iron deficiency anaemia in patients intolerant of iron. Aliment Pharmacol Ther. 1998;12(9):845–8.
Reffitt DM, Burden TJ, Seed PT, Wood J, Thompson RP, Powell JJ. Assessment of iron absorption from ferric trimaltol. Ann Clin Biochem. 2000;37(Pt 4):457–66.
Breuer W, Hershko C, Cabantchik ZI. The importance of non-transferrin bound iron in disorders of iron metabolism. Transfus Sci. 2000;23(3):185–92.
Acknowledgments
Matthew Reilly, PhD, at InTouch Medical Ltd provided editorial support in the preparation of this manuscript, paid for by Shield TX (UK) Limited, and had access to all study data.
Author contributions
As principal investigator, BB oversaw the clinical research, helped collect the data and acted as guarantor for the manuscript. AK, CM, SH and MM contributed clinical data and provided critical input on the manuscript. NM helped design the study, oversaw clinical data management and analysis, and contributed critical input to the manuscript. All authors had access to the study data and approved the final version of the manuscript prior to submission.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This research was funded in full by Iron Therapeutics Ltd, UK.
Conflict of interest
BB has received consultancy fees from Abbvie, MSD, Shire, Ferring, UCB, Hospira, Takeda, Movetis and Shield TX (UK) Limited, speaker honoraria from Abbvie, Ferring, MSD, Merckle, Falk, HLR and UCB, and research funding from Abbvie, Ferring and UCB. NM is an employee of Shield TX (UK) Limited. SH has received consulting fees and travel expenses from Shield TX (UK) Limited. AK, CM and MM have no conflicts of interest to declare.
Ethical approval
The study protocol was approved by the responsible independent ethics committees, and all procedures were conducted according to the Declaration of Helsinki, the International Conference on Harmonization guidelines on Good Clinical Practice and applicable national and regional laws and regulations.
Informed consent
Written informed consent was obtained from each patient prior to participation.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Bokemeyer, B., Krummenerl, A., Maaser, C. et al. Randomized Open-Label Phase 1 Study of the Pharmacokinetics of Ferric Maltol in Inflammatory Bowel Disease Patients with Iron Deficiency. Eur J Drug Metab Pharmacokinet 42, 229–238 (2017). https://doi.org/10.1007/s13318-016-0334-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13318-016-0334-5