Abstract
Objective
To assess the validity of modified Centor Score in predicting streptococcal pharyngitis, and describe the antibiotic sensitivity of streptococcal strains.
Methods
A crosssectional study of 120 children (age 1–18 y) with signs and symptoms of pharyngitis was undertaken in the pediatric department of a tertiary care teaching hospital in Chennai from July 2015 to April 2016. Modified Centor score was calculated for all children, and streptococcal sore throat was confirmed by throat swab culture. Predictive validity of Centor score was assessed by Receiver Operating Curve (ROC) analysis.
Results
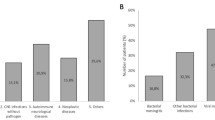
Streptococcal culture positivity was 35%. The Area Under the Curve (AUC) value for modified Centor score was 0.589 (95% CI 0.481 to 0.697, P=0.11) in predicting streptococcal pharyngitis. Cough had the highest sensitivity (63.4%), but poor specificity (36.7%) for streptococcal pharyngitis confirmed by culture. The specificity was 100% for palatine petechiae, followed by palatine exudates (97.5%) and tender anterior cervical nodes (88.6%) to diagnose streptococcal pharyngitis. The proportion of antibiotic resistance was highest for cotrimoxazole (16.7%).
Conclusions
Predictive validity of modified Centor score was not satisfactory, and resistance to cotrimoxazole, fluoroquinolones and macrolides was high among S. pyogenes strains.
Similar content being viewed by others
References
Gerber MA. Group A Streptococcus. Nelson Textbook of Pediatrics: Elsevier; 2011. p. 914–25. e1.
Ayanruoh S, Waseem M, Quee F, Humphrey A, Reynolds T. Impact of rapid streptococcal test on antibiotic use in a pediatric emergency department. Pediatr Emerg Care. 2009;25:748–50.
Centor RM, Witherspoon JM, Dalton HP, Brody CE, Link K. The diagnosis of strep throat in adults in the emergency room. Med Decis Making. 1981;1:239–46.
McIsaac WJ, White D, Tannenbaum D, Low DE. A clinical score to reduce unnecessary antibiotic use in patients with sore throat. CMAJ. 1998;158:75–83.
Kundu R. Rapid diagnostic tests in childhood infections. Indian Pediatr. 2018;55:233–7.
Fine AM, Nizet V, Mandl KD. Large-scale validation of the Centor and McIsaac scores to predict group A streptococcal pharyngitis. Arch Intern Med. 2012;172:847–52.
Atlas SJ, McDermott SM, Mannone C, Barry MJ. The role of point of care testing for patients with acute pharyngitis. J Gen Intern Med. 2005;20:759–61.
Orda U, Mitra B, Orda S, Fitzgerald M, Gunnarsson R, Rofe G, et al. Point of care testing for group A streptococci in patients presenting with pharyngitis will improve appropriate antibiotic prescription. Emerg Med Australas. 2016;28:199–204.
Palla AH, Khan RA, Gilani AH, Marra F. Over prescription of antibiotics for adult pharyngitis is prevalent in developing countries but can be reduced using McIsaac modification of Centor scores: a cross-sectional study. BMC Pulm Med. 2012;12:70.
Regoli M, Chiappini E, Bonsignori F, Galli L, de Martino M. Update on the management of acute pharyngitis in children. Ital J Pediatr. 2011;37:10.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vasudevan, J., Mannu, A. & Ganavi, G. McIsaac Modification of Centor Score in Diagnosis of Streptococcal Pharyngitis and Antibiotic Sensitivity Pattern of Beta-hemolytic Streptococci in Chennai, India. Indian Pediatr 56, 49–52 (2019). https://doi.org/10.1007/s13312-019-1467-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-019-1467-9