Abstract
Objective
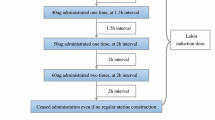
To compare the efficacy and safety profile of two methods of labor induction i.e., intracervical dinoprostone gel (0.5 mg 8 h) and misoprostol (50 μg 4 h) for induction of labor in women with a poor Bishop’s score.
Design
Observational study.
Study Period
January 1st, 2009 to December 31st, 2010.
Population
A total of 329 women with unfavorable cervices induced at or near term.
Methods
Two cervical ripening agent study arms were used: dinoprostone gel (193 women) and misoprostol (137 women).
Main Outcome Measures
Induction to delivery interval, cesarean section, incidence of meconium stained liquor, FHR pattern, incidence of uterine hyperstimulation, and neonatal outcomes.
Results
The induction to delivery interval was significantly shorter in the misoprostol group as compared to the dinoprostone group (p < 0.001). There was no difference in cesarean section rates between the two groups (dinoprostone gel 43 %; misoprostol 33 %; p = 0.144). The incidence of non-reassuring fetal heart rate pattern, meconium stained liquor, and uterine hyperstimulation were equivalent in both the groups (p = 0.529; 0.733; and 0.321, respectively). The neonatal outcomes in both the groups were comparable in terms of Apgar scores at birth (p = 0.160) and NICU admissions (p = 0.951).
Conclusions
Labor induction in women with unfavorable cervices results in high caesarean section rates. However, the use of misoprostol significantly reduces the induction to delivery interval, without adversely affecting the caesarean section rates and neonatal outcomes. Hence it may become a cost-effective alternative to dinoprostone gel in resource-poor settings like India.
Similar content being viewed by others
References
ACOG (1999) Induction of labour. ACOG practice bulletin number 10. Washington, DC, USA: The American College of Obstetricians and Gynecologists.
Wing DA, Jones MM, Rahall A, et al. A comparison of misoprostol and prostaglandin E2 gel for preinduction cervical ripening and labor induction. Am J Obstet Gynecol. 1995;172:1804–10.
Wing DA, Rahall A, Jones MM, et al. Misoprostol: an effective agent for cervical ripening and labor induction. Am J Obstet Gynecol. 1995;172:1811–6.
Chuck FJ, Huffaker BJ. Labor induction with intravaginal misoprostol versus intracervical prostaglandin E2 gel (prepidil gel): randomized comparison. Am J Obstet Gynecol. 1995;173:1137–42.
Varaklis K, Gumina R, Stubblefield PG. Randomized controlled trial of vaginal misoprostol and intracervical prostaglandin E2 gel for induction of labor at term. Obstet Gynecol. 1995;86:541–4.
Mundle WR, Young DC. Vaginal misoprostol for induction of labor: a randomized controlled trial. Obstet Gynecol. 1996;88:521–5.
Gottschall DS, Borgida AF, Mihalek JJ, et al. A randomised clinical trial comparing misoprostol with prostaglandin E2 gel for preinduction cervical ripening. Am J Obstet Gynecol. 1997;177:1067–70.
Buser D, Mora G, Arias F. A randomised comparison between misoprostol and dinoprostone for cervical ripening and labor induction in patients with unfavorable cervices. Obstet Gynecol. 1997;89:581–5.
Sanchez-Ramos L, Peterson DE, Delke I, et al. Induction with prostaglandin E1 misoprostol compared with dinoprostone vaginal insert: a randomised trial. Obstet Gynecol. 1998;91:401–5.
Kolderup L, McLean L, Grullon K, et al. Misoprostol is more efficacious for labor induction than prostaglandin E2, but is it associated with more risk? Am J Obstet Gynecol. 1999;180:1543–5150.
Danielian P, Porter B, Ferri N, et al. Misoprostol for induction of labor at term: a more effective agent than dinoprostone vaginal gel. Br J Obstet Gynaecol. 1999;106:793–7.
Nunes F, Rodrigues R, Meirinho M. Randomized comparison between intravaginal misoprostol and dinoprostone for cervical ripening and induction of labor. Am J Obstet Gynecol. 1999;181:626–9.
Fletcher H, Mitchell S, Frederick J, et al. Intravaginal misoprostol versus dinoprostone as cervical ripening and labor-inducing agents. Obstet Gynecol. 1994;83:244–7.
Surbek DV, Boesiger H, Hoesli I, et al. A double-blind comparison of the safety and efficacy of intravaginal misoprostol and prostaglandin E2 to induce labor. Am J Obstet Gynecol. 1997;177:1018–23.
Wing DA, Ortiz-Omphroy G, Paul RH. A comparison of intermittent vaginal administration of misoprostol with continuous dinoprostone for cervical ripening and labor induction. Am J Obstet Gynecol. 1997;177:612–8.
Sanchez-Ramos L, Kaunitz AM, Wears RL, et al. Misoprostol for cervical ripening and labor induction: a metaanalysis. Obstet Gynecol. 1997;89:633–42.
American College of Obstetricians and Gynecologists (1999) Induction of labor with misoprostol. ACOG committee opinion no. 228. Washington, DC 7: American College of Obstetricians and Gynecologists.
Sanchez-Ramos L. Induction of labor. Obstet Gynecol Clin N Am. 2005;32:181–200.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sareen, S., Chawla, I. & Singh, P. Labor Induction with 50 μg Vaginal Misoprostol: Can We Reduce Induction-Delivery Intervals Safely?. J Obstet Gynecol India 64, 270–273 (2014). https://doi.org/10.1007/s13224-014-0521-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13224-014-0521-8