Abstract
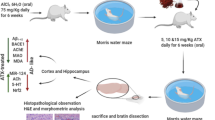
Alzheimer’s disease (AD) is a progressive degenerative disorder characterized by the presence of amyloid deposits, neurofibrillary tangles and neuron loss. Emerging evidence indicates that antioxidants could be useful either for the prevention or treatment of AD. Tacrine and melatonin are well-known drugs which act as an acetylcholinesterase inhibitor and a free radical scavenger, respectively. In this study, we evaluated the effects of a new tacrine–melatonin hybrid on behavior and the biochemical and neuropathologic changes observed in amyloid precursor protein/presenilin 1 (APP/Ps1) transgenic mice. Our findings showed that direct intracerebral administration of this hybrid decreased amyloid β peptide (Aβ)-induced cell death and amyloid burden in the brain parenchyma of APP/Ps1 mice. This reduction in Aβ pathology was accompanied by a recovery in cognitive function. Since this tacrine–melatonin hybrid apparently reduces brain Aβ and behavioral deficits, we believe this drug has remarkable and significant neuroprotective effects and might be considered a potential therapeutic strategy in AD.





Similar content being viewed by others
References
Acuña-Castroviejo D, Escames G, Rodríguez MI, López LC (2007) Melatonin role in the mitochondrial function. Front Biosci 12:947–963
Carro E, Trejo JL, Gomez-Isla T, LeRoith D, Torres-Aleman I (2002) Serum insulin-like growth factor I regulates brain amyloid-beta levels. Nat Med 8:1390–1397
Christensen DZ, Kraus SL, Flohr A, Cotel MC, Wirths O, Bayer TA (2008) Transient intraneuronal A beta rather than extracellular plaque pathology correlates with neuron loss in the frontal cortex of APP/PS1KI mice. Acta Neuropathol 116:647–655
Chung JA, Cummings JL (2000) Neurobehavioral and neuropsychiatric symptoms in Alzheimer’s disease: characteristics and treatment. Neurol Clin 18:829–846
Dietrich MO, Spuch C, Antequera D, Rodal I, de Yebenes JG, Molina JA, Bermejo F, Carro E (2008) Megalin mediates the transport of leptin across the blood-CSF barrier. Neurobiol Aging 29:902–912
Engelhart MJ, Geerlings MI, Ruitenberg A, van Swieten JC, Hofman A, Witteman JC, Breteler MM (2002) Dietary intake of antioxidants and risk of Alzheimer disease. JAMA 287:3223–3229
Feng Z, Chang Y, Cheng Y, Zhang BL, Qu ZW, Qin C, Zhang JT (2004) Melatonin alleviates behavioral deficits associated with apoptosis and cholinergic system dysfunction in the APP 695 transgenic mouse model of Alzheimer’s disease. J Pineal Res 37:129–136
Feng Z, Qin C, Chang Y, Zhang JT (2006) Early melatonin supplementation alleviates oxidative stress in a transgenic mouse model of Alzheimer’s disease. Free Radic Biol Med 40:101–109
Fernández-Bachiller MI, Pérez C, Campillo NE, Páez JA, González-Muñoz GC, Usán P, García-Palomero E, López MG, Villarroya M, García AG, Martínez A, Rodríguez-Franco MI (2009) Tacrine–melatonin hybrids as multifunctional agents for Alzheimer’s disease, with cholinergic, antioxidant, and neuroprotective properties. Chem Med Chem 4:828–841
Frisoni GB, Rozzini L, Gozzetti A, Binetti G, Zanetti O, Bianchetti A, Trabucchi M, Cummings JL (1999) Behavioral syndromes in Alzheimer’s disease: description and correlates. Dement Geriatr Cogn Disord 10:130–138
Fu H, Li W, Lao Y, Luo J, Lee NT, Kan KK, Tsang HW, Tsim KW, Pang Y, Li Z, Chang DC, Li M, Han Y (2006) Bis (7)-tacrine attenuates beta amyloid-induced neuronal apoptosis by regulating L-type calcium channels. J Neurochem 98:1400–1410
Fu H, Li W, Luo J, Lee NT, Li M, Tsim KW, Pang Y, Youdim MB, Han Y (2008) Promising anti-Alzheimer’s dimer bis(7)-tacrine reduces beta-amyloid generation by directly inhibiting BACE-1 activity. Biochem Biophys Res Commun 366:631–636
García-Palomero E, Muñoz P, Usan P, Garcia P, Delgado E, De Austria C, Valenzuela R, Rubio L, Medina M, Martínez A (2008) Potent beta-amyloid modulators. Neurodegener Dis 5:153–156
Germano C, Kinsella GJ (2005) Working memory and learning in early Alzheimer’s disease. Neuropsychol Rev 15:1–10
Geula C, Nagykery N, Nicholas A, Wu CK (2008) Cholinergic neuronal and axonal abnormalities are present early in aging and in Alzheimer disease. J Neuropathol Exp Neurol 67:309–318
Gonzalez de la Vega A, Buño W, Pons S, Garcia-Calderat MS, Garcia-Galloway E, Torres-Aleman I (2001) Insulin-like growth factor I potentiates kainate receptors through a phosphatidylinositol 3-kinase dependent pathway. Neuroreport 12:1293–1296
Gorfine T, Yeshurun Y, Zisapel N (2007) Nap and melatonin-induced changes in hippocampal activation and their role in verbal memory consolidation. J Pineal Res 43:336–342
Gutierrez-Cuesta J, Tajes M, Jiménez A, Coto-Montes A, Camins A, Pallàs M (2008) Evaluation of potential pro-survival pathways regulated by melatonin in a murine senescence model. J Pineal Res 45:497–505
Hager K, Kenklies M, McAfoose J, Engel J, Münch G (2007) Alpha-lipoic acid as a new treatment option for Alzheimer’s disease—a 48 months follow-up analysis. J Neural Transm Suppl 72:189–193
Holzgrabe U, Kapková P, Alptüzün V, Scheiber J, Kugelmann E (2007) Targeting acetylcholinesterase to treat neurodegeneration. Expert Opin Ther Targets 11:161–179
Huang HM, Zhang H, Ou HC, Chen HL, Gibson GE (2004) Alpha-keto-beta-methyl-n-valeric acid diminishes reactive oxygen species and alters endoplasmic reticulum Ca(2+) stores. Free Radic Biol Med 37:1779–1789
Krishnan KR, Charles HC, Doraiswamy PM, Mintzer J, Weisler R, Yu X, Perdomo C, Ieni JR, Rogers S (2003) Randomized, placebo-controlled trial of the effects of donepezil on neuronal markers and hippocampal volumes in Alzheimer’s disease. Am J Psychiatry 160:2003–2011
Lahiri DK (1999) Melatonin affects the metabolism of the beta-amyloid precursor protein in different cell types. J Pineal Res 26:137–146
Lalonde R, Kim HD, Fukuchi K (2004) Exploratory activity, anxiety, and motor coordination in bigenic APPswe + PS1/DeltaE9 mice. Neurosci Lett 369:156–161
Liu RY, Zhou JN, van Heerikhuize J, Hofman MA, Swaab DF (1999) Decreased melatonin levels in postmortem cerebrospinal fluid in relation to aging, Alzheimer’s disease, and apolipoprotein E-epsilon4/4 genotype. J Clin Endocrinol Metab 84:323–327
Luchsinger JA, Tang MX, Shea S, Mayeux R (2003) Antioxidant vitamin intake and risk of Alzheimer disease. Arch Neurol 60:203–208
Martinez A, Fernández E, Castro A, Conde S, Rodríguez-Franco MI, Baños JE, Badia A (2000) N-Benzylpiperidine derivatives of 1,2,4-thiadiazolidinone as new acetylcholinesterase inhibitors. Eur J Med Chem 35:913–922
Masilamoni JG, Jesudason EP, Dhandayuthapani S, Ashok BS, Vignesh S, Jebaraj WC, Paul SF, Jayakumar R (2008) The neuroprotective role of melatonin against amyloid beta peptide injected mice. Free Radic Res 42:661–673
Matsubara E, Bryant-Thomas T, Pacheco Quinto J, Henry TL, Poeggeler B, Herbert D, Cruz-Sanchez F, Chyan YJ, Smith MA, Perry G, Shoji M, Abe K, Leone A, Grundke-Ikbal I, Wilson GL, Ghiso J, Williams C, Refolo LM, Pappolla MA, Chain DG, Neria E (2003) Melatonin increases survival and inhibits oxidative and amyloid pathology in a transgenic model of Alzheimer’s disease. J Neurochem 85:1101–1108
Modrego PJ (2006) The effect of drugs for Alzheimer disease assessed by means of neuroradiological techniques. Curr Med Chem 13:3417–3424
Moreira PI, Santos MS, Oliveira CR, Shenk JC, Nunomura A, Smith MA, Zhu X, Perry G (2008) Alzheimer disease and the role of free radicals in the pathogenesis of the disease. CNS Neurol Disord Drug Targets 7:3–10
Nuñez A, Buño W (1999) In vitro electrophysiological properties of rat dorsal column nuclei neurons. Eur J Neurosci 11:1865–1876
Polidori MC (2004) Oxidative stress and risk factors for Alzheimer’s disease: clues to prevention and therapy. J Alzheimers Dis 6:185–191
Pons S, Torres-Aleman I (2000) Insulin-like growth factor-I stimulates dephosphorylation of ikappa B through the serine phosphatase calcineurin (protein phosphatase 2B). J Biol Chem 275:38620–38625
Quinn J, Suh J, Moore MM, Kaye J, Frei B (2003) Antioxidants in Alzheimer’s disease-vitamin C delivery to a demanding brain. J Alzheimer Dis 5:309–313
Raina P, Santaguida P, Ismaila A, Patterson C, Cowan D, Levine M, Booker L, Oremus M (2008) Effectiveness of cholinesterase inhibitors and memantine for treating dementia: evidence review for a clinical practice guideline. Ann Intern Med 148:379–397
Raschetti R, Albanese E, Vanacore N, Maggini M (2007) Cholinesterase inhibitors in mild cognitive impairment: a systematic review of randomised trials. PLoS Med 4:338
Rodríguez-Franco MI, Fernández-Bachiller MI (2002) 1-Benzyl-4-chloromethylpiperidine: a building block in the synthesis of compounds of pharmacological interest. Synthesis 911–915
Rodríguez-Franco MI, Dorronsoro I, Martínez A (2001) O-Pyrazolylpropynyl-hydroxylamines as versatile intermediates in the synthesis of compounds of pharmacological interest. Synthesis 1711–1775
Rodríguez-Franco MI, Fernández-Bachiller MI, Pérez C, Castro A, Martínez A (2005) Design and synthesis of N-benzylpiperidine–purine derivatives as new dual inhibitors of acetyl- and butyrylcholinesterase. Biorg Med Chem 13:6795–6802
Rodríguez-Franco MI, Fernández-Bachiller MI, Pérez C, Hernández-Ledesma B, Bartolomé B (2006) Novel tacrine–melatonin hybrids as dual–acting drugs for Alzheimer disease, with improved acetylcholinesterase inhibitory and antioxidant properties. J Med Chem 49:459–462
Samuel W, Terry RD, DeTeresa R, Butters N, Masliah E (1994) Clinical correlates of cortical and nucleus basalis pathology in Alzheimer dementia. Arch Neurol 51:772–778
Scheff SW, DeKosky ST, Price DA (1990) Quantitative assessment of cortical synaptic density in Alzheimer’s disease. Neurobiol Aging 11:29–37
Song W, Lahiri DK (1997) Melatonin alters the metabolism of the beta-amyloid precursor protein in the neuroendocrine cell line PC12. J Mol Neurosci 9:75–92
Srinivasan V, Pandi-Perumal SR, Maestroni GJ, Esquifino AI, Hardeland R, Cardinali DP (2005) Role of melatonin in neurodegenerative diseases. Neurotox Res 7:293–318
Tiraboschi P, Hansen LA, Alford M, Masliah E, Thal LJ, Corey-Bloom J (2000) The decline in synapses and cholinergic activity is asynchronous in Alzheimer’s disease. Neurology 55:1278–1283
Vargas T, Ugalde C, Spuch C, Antequera D, Morán MJ, Martín MA, Ferrer I, Bermejo F, Carro E (2008) A beta accumulation in choroid plexus is associated with mitochondrial-induced apoptosis. Neurobiol Aging
Wu CK, Thal L, Pizzo D, Hansen L, Masliah E, Geula C (2005) Apoptotic signals within the basal forebrain cholinergic neurons in Alzheimer’s disease. Exp Neurol 195:484–496
Yao M, Nguyen T-VV, Pike CJ (2005) b-Amyloid-induced neuronal apoptosis involves c-Jun N-terminal kinase-dependent downregulation of Bcl-w. J Neurosci 25:1149–1158
Zhang HY, Yang DP, Tang GY (2006) Multipotent antioxidants: from screening to design. Drug Discov Today 11:749–754
Zhu X, Su B, Wang X, Smith MA, Perry G (2007) Causes of oxidative stress in Alzheimer disease. Cell Mol Life Sci 64:2202–2210
Acknowledgments
There is no conflict of interest with other people or organizations. This work was supported by grants from Fondo de Investigación Sanitaria (FIS) (CP04/00179, PI060155), Fundación Investigación Médica Mutua Madrileña (2006.125), CIBERNED, and Ministerio de Educación y Ciencia (BFU2006-07430/BFI and SAF2006-01249). We thank Dr. Washington Buño and Dr. David Fernandez de Sevilla for expert help in brain organotypic culture. We thank Dr. Ximena Alvira-Botero for editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Spuch, C., Antequera, D., Isabel Fernandez-Bachiller, M. et al. A New Tacrine–Melatonin Hybrid Reduces Amyloid Burden and Behavioral Deficits in a Mouse Model of Alzheimer’s Disease. Neurotox Res 17, 421–431 (2010). https://doi.org/10.1007/s12640-009-9121-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12640-009-9121-2