Abstract
Objectives
The present study examined whether the combination of self-reported mobility decline (SR-MD) and cognitive decline (SR-CD) was associated with mortality and new long-term care insurance (LTCI) service certifications based on sex and age.
Design
A prospective cohort study.
Setting and Participants
We analyzed cohort data from a sample of older adult residents in Kami Town, Japan. The response rate was 94.3%, and we followed 5,094 older adults for 3 years. Full analyses were conducted on 5,076 participants.
Measures
A total of four groups were determined through self-reported responses on the Kihon Checklist for SR-MD (a score of 3 or more on 5 items) and SR-CD (a score of 1 or more on 3 items): non-SR-cognitive frailty, non-SR-MD & SR-CD, SR-MD & non-SR-CD, and SR-cognitive frailty.
Results
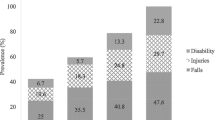
Main outcomes included mortality (n = 262) or new certifications for LTCI services (n = 708) during the 3-year period. Excluding overlapping, this included 845 older adults (16.6%). Among men, prevalence of non-SR-cognitive frailty, non-SR-MD & SR-CD, SR-MD & non-SR-CD, and SR-cognitive frailty (SR-MD & SR-CD) was 48.2%, 26.4%, 11.5%, and 13.8%, respectively. Respective rates for women were 45.7%, 15.5%, 23.1%, and 15.7%. Multivariate analyses revealed that for men, SR-MD & non-SR-CD significantly affected adverse health outcomes, leading to earlier negative outcomes relative to the non-SR-MD & SR-CD group. For women, non-SR-MD & SR-CD and SR-MD & non-SR-CD had similar slopes.
Conclusions
The impact of SR-MD or SR-CD on adverse health outcomes differed as a function of age and sex. Thus, we need to consider preventive approaches according to these specific target group features.
Similar content being viewed by others
References
Minister of Health, Labour and Welfare. A Basic-direction for Comprehensive Implementation of National Health Promotion. Ministerial Notification No. 430 of the Ministry of Health, Labour and Welfare. July 10, 2012. http://www.mhlw.go.jp/file/06-Seisakujouhou-10900000-Kenkoukyoku/0000047330.pdf Accessed 8 June 2018.
Ensrud KE, Lui LY, Paudel ML, Schousboe JT, Kats AM, Cauley JA, McCulloch CE, Yaffe K, Cawthon PM, Hillier TA, Taylor BC; Study of Osteoporotic Fractures (SOF). Effects of mobility and cognition on risk of mortality in women in late life: a prospective study. J Gerontol A Biol Sci Med Sci 2016;71(6):759–765. doi: https://doi.org/10.1093/gerona/glv220.
Avila-Funes JA, Amieva H, Barberger-Gateau P, Le Goff M, Raoux N, Ritchie K, Carrière I, Tavernier B, Tzourio C, Gutiérrez-Robledo Dartigues JF. Cognitive impairment improves the predictive validity of the phenotype of frailty for adverse health outcomes: the three-city study. J Am Geriatr Soc 2009;57(3):453–461. doi: https://doi.org/10.1111/j.1532-5415.2008.02136.x.
Tomata Y, Hozawa A, Ohmori-Matsuda K, Nagai M, Sugawara Y, Nitta A, Kuriyama S, Tsuji I. Validation of the Kihon Checklist for predicting the risk of 1-year incident long-term care insurance certification: the Ohsaki Cohort 2006 Study. Nihon Koshu Eisei Zasshi 2011;58(1):3–13. (in Japanese)
Zunzuneguia MV, Alvaradob BE, Guerrac R, Gómezd JF, Ylli A, Guralnik JM; Imias Research Group. The mobility gap between older men and women: the embodiment of gender. Arch Gerontol Geriatr 2015;61(2):140–148. doi: https://doi.org/10.1016/j.archger.2015.06.005.
Lang PO, Michel JP, Zekry D. Frailty syndrome: a transitional state in a dynamic process. Gerontology 2009;55(5):539–549. doi: https://doi.org/10.1159/000211949.
Abellan van Kan G, Rolland Y, Andrieu S, Bauer J, Beauchet O, Bonnefoy M, Cesari M, Donini LM, Gillette Guyonnet S, Inzitari M, Nourhashemi F, Onder G, Ritz P, Salva A, Visser M, Vellas B. Gait speed at usual pace as a predictor of adverse outcomes in community-dwelling older people an International Academy on Nutrition and Aging (IANA) Task Force. J Nutr Health Aging 2009;13(10):881–889.
Reed-Jones RJ, Solis GR, Lawson KA, Loya AM, Cude-Islas D, Berger CS. Vision and falls: a multidisciplinary review of the contributions of visual impairment to falls among older adults. Maturitas 2013;75(1):22–28. doi: https://doi.org/10.1016/j.maturitas.2013.01.019.
Visschedijk J, Achterberg W, Van Balen R, Hertogh C. (2010) Fear of falling after hip fracture: a systematic review of measurement instruments, prevalence, interventions, and related factors. J Am Geriatr Soc 2010;58(9):1739–1748. doi: https://doi.org/10.1111/j.1532-5415.2010.03036.x.
Cheng MH, Chang SF. Frailty as a risk factor for falls among community dwelling people: evidence from a meta-analysis. J Nurs Scholarsh 2017;49(5):529–536. doi: https://doi.org/10.1111/jnu.12322.
Buchman AS, Wilson RS, Leurgans SE, Bennett DA, Barnes LL. Change in motor function and adverse health outcomes in older African-Americans. Exp Gerontol. 2015;70:71–7. doi: https://doi.org/10.1016/j.exger.2015.07.009.
Polis S, Fernandez R. Impact of physical and psychological factors on health-related quality of life in adult patients with liver cirrhosis: a systematic review protocol. JBI Database System Rev Implement Rep 2015;13(1):39–51. doi: https://doi.org/10.11124/jbisrir-2015-1987.
Pratali L, Mastorci F, Vitiello N, Sironi A, Gastaldelli A, Gemignani A. Motor activity in aging: an integrated approach for better quality of life. Int Sch Res Notices 2014;24: 257248. doi: https://doi.org/10.1155/2014/257248.
Kojima G, Iliffe S, Jivraj S, Walters K. Association between frailty and quality of life among community-dwelling older people: a systematic review and meta-analysis. J Epidemiol Community Health 2016;70(7):716–721. doi: https://doi.org/10.1136/jech-2015-206717.
Botoseneanu A, Allore HG, Mendes de Leon CF, Gahbauer EA, Gill TM. Sex differences in concomitant trajectories of self-reported disability and measured physical capacity in older adults. J Gerontol A Biol Sci Med Sci 2016;71(8):1056–1062. doi: https://doi.org/10.1093/gerona/glw038.
Davis DH, Rockwood MR, Mitnitski AB, Rockwood K. Impairments in mobility and balance in relation to frailty. Arch Gerontol Geriatr 2011;53(1):79–83. doi: https://doi.org/10.1016/j.archger.2010.06.013.
Veronese N, Stubbs B, Fontana L, Trevisan C, Bolzetta F, Rui M, Sartori L, Musacchio E, Zambon S, Maggi S, Perissinotto E, Corti MC, Crepaldi G, Manzato E, Sergi G. A comparison of objective physical performance tests and future mortality in the elderly people. J Gerontol A Biol Sci Med Sci 2017;72(3):362–368. doi: https://doi.org/10.1093/gerona/glw139.
Hubbard RE, O’Mahony MS, Woodhouse KW. Medication prescribing in frail older people. Eur J Clin Pharmacol 2013;69(3):319–326. doi: https://doi.org/10.1007/s00228-012-1387-1392.
Villacampa-Fernández P, Navarro-Pardo E, Tarin JJ, Cano A. Frailty and multimorbidity: Two related yet different concepts. Maturitas. 2016;95:31–35. doi: https://doi.org/10.1016/j.maturitas.2016.10.008.
Boeckxstaens P, Vaes B, Legrand D, Dalleur O, De Sutter A, Degryse JM. The relationship of multimorbidity with disability and frailty in the oldest patients: a cross-sectional analysis of three measures of multimorbidity in the BELFRAIL cohort. Eur J Gen Pract. 2015;21(1):39–44. doi: https://doi.org/10.3109/13814788.2014.914167.
Shimada H, Makizako H, Doi T, Yoshida D, Tsutsumimoto K, Anan Y, Uemura K, Ito T, Lee S, Park H, Suzuki T. Combined prevalence of frailty and mild cognitive impairment in a population of elderly Japanese people. J Am Med Dir Assoc 2013;14(7):518–524. doi: https://doi.org/10.1016/j.jaSR-MDa.2013.03.010.
Shimada H, Makizako H, Lee S, Doi T, Lee S, Tsutsumimoto K, Harada K, Hotta R, Bae S, Nakakubo S, Harada K, Suzuki T. Impact of cognitive frailty on daily Activities in older persons. J Nutr Health Aging. 2016;20(7):729–235. doi: https://doi.org/10.1007/s12603-016-0685-2.
Albala C, Lera L, Sanchez H, Angel B, Márquez C, Arroyo P, Fuentes P. Frequency of frailty and its association with cognitive status and survival in older Chileans. Clin Interv Aging 2017;12:995–1001. doi: https://doi.org/10.2147/CIA.S136906.
Su X, Shang L, Xu Q, Li N, Chen J, Zhang L, Zhang L, Hua Q. Prevalence and predictors of mild cognitive impairment in Xi’an: a community-based study among the elders. PLoS One 2014;9(1):e83217. doi: https://doi.org/10.1371/journal.pone.0083217.
Cooper C, Sommerlad A, Lyketsos CG, Livingston G. Modifiable predictors of dementia in mild cognitive impairment: a systematic review and meta-analysis. Am J Psychiatry 2015;172(4):323–334. doi: https://doi.org/10.1176/appi.ajp.2014.14070878.
Lindbergh CA, Dishman RK, Miller LS. Functional disability in mild cognitive impairment: a systematic review and meta-analysis. Neuropsychol Rev 2016;26(2):129–159. doi: https://doi.org/10.1007/s11065-016-9321-5.
Lipardo DS, Aseron AMC, Kwan MM, Tsang WW. Effect of exercise and cognitive training on falls and fall-related factors in older adults with mild cognitive impairment: a systematic review. Arch Phys Med Rehabil 2017;98(10):2079–2096. doi: https://doi.org/10.1016/j.apmr.2017.04.021.
Canevelli M, Grande G, Lacorte E, Quarchioni E, Cesari M, Mariani C, Bruno G, Vanacore N. Spontaneous reversion of mild cognitive impairment to normal cognition: A systematic review of literature and meta-analysis. J Am Med Dir Assoc 2016;17(10):943–938. doi: https://doi.org/10.1016/j.jaSR-MDa.2016.06.020.
Malek-Ahmadi M. Reversion from mild cognitive impairment to normal cognition: a meta-analysis. Alzheimer Dis AssoSR-CDisord 2016;30(4):324–330.
Kelaiditi E, Cesari M, Canevelli M, van Kan GA, Ousset PJ, Gillette-Guyonnet S, Ritz P, Duveau F, Soto ME, Provencher V, Nourhashemi F, Salvà A, Robert P, Andrieu S, Rolland Y, Touchon J, Fitten JL, Vellas B; IANA/IAGG. Cognitive frailty: rational and definition from an (I.A.N.A./I.A.G.G.) international consensus group. J Nutr Health Aging. 2013;17(9):726–734. doi: https://doi.org/10.1007/s12603-013-0367-2.
Arai H, Satake S, Kozaki K. Cognitive frailty in geriatrics. Clin Geriatr Med. 2018 34(4):667–675. doi: https://doi.org/10.1016/j.cger.2018.06.011.
Roppolo M, Mulasso A, Rabaglietti E. Cognitive frailty in Italian community-dwelling older adults: Prevalence rate and its association with disability. J Nutr Health Aging. 2017;21(6):631–636. doi: https://doi.org/10.1007/s12603-016-0828-5.
Delrieu J, Andrieu S, Pahor M, Cantet C, Cesari M, Ousset PJ, Voisin T, Fougère B, Gillette S, Carrie I, Vellas B. Neuropsychological profile of “cognitive frailty” subjects in MAPT Study. J Prev Alzheimers Dis. 2016;3(3):151–159.
Shimada H, Doi T, Lee S, Makizako H, Chen LK, Arai H. Cognitive frailty predicts incident dementia among community-dwelling older people. J Clin Med. 2018;7(9). pii: E250. doi: https://doi.org/10.3390/jcm7090250.
Fougère B, Delrieu J, Del Campo N, Soriano G, Sourdet S, Vellas B. Cognitive frailty: Mechanisms, tools to measure, prevention and controversy. Clin Geriatr Med. 2017;33(3):339–355. doi: https://doi.org/10.1016/j.cger.2017.03.001.
Montero-Odasso MM, Barnes B, Speechley M, Muir Hunter SW, Doherty TJ, Duque G, Gopaul K, Sposato LA, Casas-Herrero A, Borrie MJ, Camicioli R, Wells JL. Disentangling cognitive-frailty: Results from the gait and brain study. J Gerontol A Biol Sci Med Sci. 2016;71(11):1476–1482.
Feng L, Zin Nyunt MS, Gao Q, Feng L, Yap KB, Ng TP. Cognitive frailty and adverse health outcomes: Findings from the Singapore Longitudinal Ageing Studies (SLAS). J Am Med Dir Assoc. 2017;18(3):252–258. doi: https://doi.org/10.1016/j.jamda.2016.09.015.
Solfrizzi V, Scafato E, Lozupone M, Seripa D, Giannini M, Sardone R, Bonfiglio C, Abbrescia DI, Galluzzo L, Gandin C, Baldereschi M, Di Carlo A, Inzitari D, Daniele A, Sabbà C, Logroscino G, Panza F, Italian Longitudinal Study on Aging Working Group. Additive role of a potentially reversible cognitive frailty model and inflammatory state on the risk of disability: The Italian Longitudinal Study on Aging. Am J Geriatr Psychiatry. 2017;25(11):1236–1248. doi: https://doi.org/10.1016/j.jagp.2017.05.018.
Solfrizzi V, Scafato E, Seripa D, Lozupone M, Imbimbo BP, D’Amato A, Tortelli R, Schilardi A, Galluzzo L, Gandin C, Baldereschi M, Di Carlo A, Inzitari D, Daniele A, Sabbà C1, Logroscino G, Panza F, Italian Longitudinal Study on Aging Working Group. Reversible cognitive frailty, dementia, and all-cause mortality. The Italian Longitudinal Study on Aging. J Am Med Dir Assoc. 2017;18(1):89.e1–89.e8. doi: https://doi.org/10.1016/j.jamda.2016.10.012.
Shimada H, Makizako H, Tsutsumimoto K, Doi T, Lee S, Suzuki T. Cognitive frailty and incidence of dementia in older persons. J Prev Alzheimers Dis. 2018;5(1):42–48. doi: https://doi.org/10.14283/jpad.2017.29.
Satake S, Senda K, Hong YJ, Miura H, Endo H, Sakurai T, Kondo I, Toba K. (2016) Validity of the Kihon Checklist for assessing frailty status. Geriatr Gerontol Int 2016;16(6):709–715. doi: https://doi.org/10.1111/ggi.12543.
Morley JE, Arai H, Cao L, Dong B, Merchant RA, Vellas B, Visvanathan R, Woo J. Integrated care: enhancing the role of the primary health care professional in preventing functional decline: a systematic review. J Am Med Dir Assoc 2017;18(6):489–494. doi: https://doi.org/10.1016/j.jaSR-MDa.2017.03.015.
Ambagtsheer RC, Thompson MQ, Archibald MM, Casey MG, Schultz TJ. Diagnostic test accuracy of self-reported frailty screening instruments in identifying community-dwelling older people at risk of frailty and pre-frailty: a systematic review protocol. JBI Database System Rev Implement Rep 2017;15(10):2464–2468. doi: https://doi.org/10.11124/JBISRIR-2017-003363.
Kojima G, Taniguchi Y, Kitamura A, Shinkai S. Are the Kihon Checklist and the Kaigo-Yobo Checklist compatible with the frailty index? J Am Med Dir Assoc 2018;19(9):797–800.e2. doi: https://doi.org/10.1016/j.jaSR-MDa.2018.05.012.
Fukutomi E, Okumiya K, Wada T, Sakamoto R, et al. Importance of cognitive assessment as part of the “Kihon Checklist” developed by the Japanese Ministry of Health, Labor and Welfare for prediction of frailty at a 2-year follow up. Geriatr Gerontol Int 2013;13(3):6546–62. doi: https://doi.org/10.1111/j.1447-0594.2012.00959.x.
Fukutomi E, Okumiya K, Wada T, Sakamoto R, Ishimoto Y, Kimura Y, Kasahara Y, Chen WL, Imai H, Fujisawa M, Otuka K, Matsubayashi K. Relationships between each category of 25-item frailty risk assessment (Kihon Checklist) and newly certified older adults under Long-Term Care Insurance: a 24-month follow-up study in a rural community in Japan. Geriatr Gerontol Int 2015;15(7):864–871. doi: https://doi.org/10.1111/ggi.12360.
Tomata Y, Sugiyama K, Kaiho Y, Sugawara Y, Hozawa A, Tsuji I. Predictive ability of a simple subjective memory complaints scale for incident dementia: Evaluation of Japan’s national checklist, the “Kihon Checklist”. Geriatr Gerontol Int 2017;17(9):1300–1305. doi: https://doi.org/10.1111/ggi.12864.
Theou O, O’Connell SR-MD, King-Kallimanis BL, O’Halloran AM, Rockwood K, Kenny RA. Measuring frailty using self-report and test-based health measures. Age Ageing 2015;44(3):471–477. doi: 10.1093/ageing/afv010.
Kusumastuti S, Gerds TA, Lund R, Mortensen EL, Westendorp RGJ. Discrimination ability of comorbidity, frailty, and subjective health to predict mortality in community-dwelling older people: population based prospective cohort study. Eur J Intern Med 2017;42:29–38. doi: https://doi.org/10.1016/j.ejim.2017.05.016.
Snitz BE, Unverzagt FW, Chang CC, Bilt JV, Gao S, Saxton J, Hall KS, Ganguli M. Effects of age, gender, education and race on two tests of language ability in community-based older adults. Int Psychogeriatr 2009;21(6):1051–1062. doi: https://doi.org/10.1017/S1041610209990214.
Apóstolo J, Cooke R, Bobrowicz-Campos E, Santana S, Marcucci M, Cano A, Vollenbroek-Hutten M, Germini F, D’Avanzo B, Gwyther H, Holland C. Effectiveness of interventions to prevent pre-frailty and frailty progression in older adults: a systematic review. JBI Database System Rev Implement Rep 2018;16(1):140–232. doi: https://doi.org/10.11124/JBISRIR-2017-003382.
Potter R, Ellard D, Rees K, Thorogood M. A systematic review of the effects of physical activity on physical functioning, quality of life and depression in older people with dementia. Int J Geriatr Psychiatry 2011;26(10):1000–11. doi: https://doi.org/10.1002/gps.2641.
Huang CQ, Wang ZR, Li YH, Xie YZ, Liu QX. Cognitive function and risk for depression in old age: a meta-analysis of published literature. Int Psychogeriatr 2011;23(4):516–525. doi: https://doi.org/10.1017/S1041610210000049.
Shinsho F. New strategy for better geriatric oral health in Japan: 80/20 movement and Healthy Japan 21. Int Dent 2001;J51(3 Suppl):200–206.
Wright J, Baldwin C. Oral nutritional support with or without exercise in the management of malnutrition in nutritionally vulnerable older people: a systematic review and meta-analysis. Clin Nutr pii: 2017;S0261–5614(17)30319–9. doi: https://doi.org/10.1016/j.clnu.2017.09.004.
Iecovich E, Biderman A. Attendance in adult day care centers and its relation to loneliness among frail older adults. Int Psychogeriatr 2012;24(3):439–448. doi: https://doi.org/10.1017/S1041610211001840.
Okura M, Ogita M, Yamamoto M, Nakai T, Numata T, Arai H. The relationship of community activities with cognitive impairment and depressive mood independent of mobility disorder in Japanese older adults. Arch Gerontol Geriatr 2017;70:54–61. doi: https://doi.org/10.1016/j.archger.2016.12.010.
Okura M, Ogita M, Yamamoto M, Nakai T, Numata T, Arai H. Community activities predict disability and mortality in community-dwelling older adults. Geriatr Gerontol Int 2018;18(7):1114–1124. doi: https://doi.org/10.1111/ggi.13315.
Minister of Health, Labour and Welfare. Long-term care insurance latest information Vol. 181: About implementation method of secondary preventive project. March 11, 2011. https://www.wam.go.jp/gyoseiShiryou-files/resources/bc344f83-6255-4263-90b0-2e3d99f0209e/%E4%BB%8B%E8%AD%B7%E4%BF%9D%E9%99%BA%E6%9C%80%E6%96%B0%E6%83%85%E5%A0%B1vol.181.pdf Accessed 1 March 2019.
Nakash RA, Hutton JL, Jørstad-Stein EC, Gates S, Lamb SE. Maximising response to postal questionnaires—a systematic review of randomised trials in health research. BMC Med Res Methodol. 2006;6:5.
Edwards P, Roberts I, Clarke M, DiGuiseppi C, Pratap S, Wentz R, Kwan I, Cooper R. Methods to increase response rates to postal questionnaires. Cochrane Database Syst Rev. 2007;2:MR000008.
Edelman LS, Yang R, Guymon M, Olson LM. Survey methods and response rates among rural community dwelling older adults. Nurs Res. 2013;62(4):286–291. doi: https://doi.org/10.1097/NNR.0b013e3182987b32.
Wright J, Baldwin C. Oral nutritional support with or without exercise in the management of malnutrition in nutritionally vulnerable older people: a systematic review and meta-analysis. Clin Nutr pii: 2017;S0261–5614(17)30319–9. doi: https://doi.org/10.1016/j.clnu.2017.09.004.
Okamoto K, Ohsuka K, Shiraishi T, Hukazawa E, Wakasugi S, Furuta K. Comparability of epidemiological information between self- and interviewer-administered questionnaires. J Clin Epidemiol 2002;55(5):505–511.
Pike CJ. Sex and the development of Alzheimer’s disease. J Neurosci Res 2017;95(1–2):671–680. doi: https://doi.org/10.1002/jnr.23827.
Hirvensalo M, Rantanen T, Heikkinen E. Mobility difficulties and physical activity as predictors of mortality and loss of independence in the community-living older population. J Am Geriatr Soc 2000;48(5):493–498.
Strobl R, Maier W, Ludyga A, Mielck A, Grill E. Relevance of community structures and neighbourhood characteristics for participation of older adults: a qualitative study. Qual Life Res. 2016;25(1):143–152. doi: https://doi.org/10.1007/s11136-015-1049-9.
Acknowledgements
We are extremely grateful to all the study participants and staff from the Kami Town Hall, who assisted with this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Okura, M., Ogita, M. & Arai, H. Self-Reported Cognitive Frailty Predicts Adverse Health Outcomes for Community-Dwelling Older Adults Based on an Analysis of Sex and Age. J Nutr Health Aging 23, 654–664 (2019). https://doi.org/10.1007/s12603-019-1217-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-019-1217-7