Abstract
Objectives
To examine the independent and combined effects of inflammation and endocrine dysregulation on (i) baseline frailty status and (ii) frailty progression at one year, among cognitively impaired community dwelling older adults.
Design
Prospective cohort study.
Setting
Tertiary Memory Clinic.
Methods
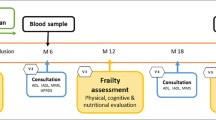
We recruited patients with mild cognitive impairment and mild-moderate Alzheimer’s disease. Physical frailty status was assessed at baseline and 1-year. Blood biomarkers of systemic inflammation [interleukin-6 (IL-6), tumour necrosis factor-α (TNF-α)] and anabolic hormones [insulin-like growth factor-1 (IGF-1), dehydroepiandrosterone sulphate (DHEAS)] were measured at baseline and examined in relation to physical frailty status at baseline and progression at 1-year. Each subject was categorized as (i) neither pro-inflammatory nor endocrine deficient, (ii) pro-inflammatory (IL-6 or TNF-α, or both, being in highest quartile) but not endocrine deficient, (iii) endocrine deficient (IGF-1 or DHEAS, or both, being in lowest quartile) but not pro-inflammatory and (iv) both pro-inflammatory and endocrine deficient.
Results
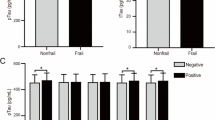
Twenty (20.2%) of 99 subjects were physically frail at baseline. There was no association between severity of cognitive impairment and baseline frailty status, but the frail group had significantly greater hippocampal atrophy (median MTA: 2 (2–3) vs 1 (1–2), p=0.010). TNF-α was significantly higher in subjects who were physically frail at baseline (median TNF-α: 1.30 (0.60–1.40) vs 0.60 (0.50–1.30) pg/mL, p=0.035). In multiple logistic regression adjusted for age and gender, a pro-inflammatory state in the absence of concomitant endocrine deficiency was significantly associated with physical frailty at baseline (OR=4.99, 95% C.I 1.25–19.88, p=0.023); this was no longer significant when MTA score was included in the model. Isolated pro-inflammatory state (without endocrine deficiency) significantly increased the odds of frailty progression (OR=4.06, 95% CI 1.09–15.10, p=0.037) at 1-year. The combination pro-inflammatory and endocrine deficient state was not significantly associated with either baseline or progressive physical frailty.
Conclusion
A pro-inflammatory state exerts differential effects on physical frailty, contributing to the increased risk of baseline and progressive frailty only in the absence of a concomitant endocrine deficient state, with potential mediation via neurodegeneration.
Similar content being viewed by others
References
Buchman AS, Boyle PA, Wilson RS et al. Frailty is associated with incident Alzheimer’s disease and cognitive decline in the elderly. Psychomatic Medicine 2007;69: 483–489
Claudia B, Luigi B, Paola N et al. Frailty syndrome diagnosed according to the Study of Osteoporotic Fractures criteria and mortality in older outpatients suffering from Alzheimer’s disease: A one-year prospective cohort study. Aging & Mental Health 2012;16(3): 273–280
Fang X, Shi J, Song X et al. Frailty in relation to the risk of falls, fractures, and mortality in older Chinese adults: results from the Beijing Longitudinal Study of Aging. J Nutri Health &Aging 2012;16:903–907
Ensrud KE, Ewing SK, Tayloe BC et al. Frailty and risk of falls, fracture, and mortality in older women: The Study of Osteoporotic Fractures. J Gerontol A Biol Med Sci 2007;62A(7):744–751
Fried LP, Ferruci L, Darer J et al. Untangling the concepts of disability, frailty and co-morbidity: implications for improved targeting and care. J Gerontol A Biol Med Sci 2004;59:255–63
Robertson DA, Savva GM, Kenny RA. Frailty and cognitive impairment- A review of the evidence and causal mechanisms. Ageing Res Reviews 2013;12:840–851
Ni Mhaolain AM, Gallagher D, Crosby L et al. Frailty and quality of life for people with Alzheimer’s dementia and mild cognitive impairment. Am J of Alzheimer’s Dis and Other Demen 2012;27(1):48–54
Ni Mhaolain AM, Gallagher D, Crosby L, Ryan D et al. Correlates of frailty in Alzheimer’s disease and mild cognitive impairment. Age Ageing 2011;630–633
Thomas MG, Evelyne AG, Heather GA et al. Transitions between frailty states among community-living older persons. Arch Intern Med 2006;166:418–423
Nader F, Arnold M, Samuel DS et al. Transitions in frailty status in older adults in relation to mobility: A multi-state modeling approach employing a deficit count. J Am Geriatr Soc 2011;59(3): 524–529
Oosterveld SM, Kessels RP, Ramakers RH et al. The influence of co-morbidity and frailty on clinical manifestation of patients with Alzheimer’s disease. J Alzheimer’s Dis Jun 2 (Epub ahead of print), 2014
Chong MS, Tay L, Chan M et al. Stage-specific relationship between frailty and cognitive impairment in a specialist Memory Clinic setting. The Journal of Frailty and Ageing 2014;3(2):113–119
Buchman AS, Schneider JA, Leurgans S et al. Physical frailty in older persons is associated with Alzheimer pathology. Neurology 2008;71(7);499–504
Holmes C, Cunningham C, Zotova E, et al. Systemic inflammation and disease progression in Alzheimer disease. Neurology 2009;73:768–774
Watson J, McBurnie MA, Newman A et al. Frailty and activation of the inflammation and coagulation systems with and without clinical comorbidities. Results from the cardiovascular health study. Arch Intern Med 2002;162:2333–2341
Cappola AR, Xue QL, Fried L. Multiple hormonal deficiencies in anabolic hormones are found in frail older women: The Women’s Health and Aging studies. J Gerontol A Biol Med Sci 2009;64:243–248
Maggio M, Dall’ Aglio E, Lauretani F et al. The hormonal pathway to cognitive impairment in older men. J Nutr Health Aging 2012;16(1): 40–54
Singh-Manoux A, Dugravot A, Brunner E et al. Interleukin-6 and C-reactive protein as predictors of cognitive decline in late midlife. Neurology 2014;83(6):486–493
Afilalo J, Karunananthan S, Eisenberg MJ et al. Role of frailty in patients with cardiovascular disease. Am J Cardiol 2009;103:1616–1621
Luchsinger J, Mayeux R. Cardiovascular risk factors and Alzheimer’s disease. Curr Atheroscler Rep Jul; 2004;6(4):261–266
Buchman AS, Yu L, Wilson RS et al. Brain pathology contributes to simultaneous change in physical frailty and cognition in old age. J Gerontol A Biol Sci Med Sci 2014;69(12):1536–1544
Kelaiditi E, Cesari M, Canevelli M et al. Cognitive frailty: rational and definition from an (I.A.N.A/ I.A.G.G) international consensus group. J Nutr Health Aging 2013;17(9): 726–34
Halil M, Kilizarslanogul M. C, Kuyumcu M. E, Yesil Y, Jentoft AJ C. Cognitive aspects of frailty: mechanisms behind the link between frailty and cognitive impairment. J Nutr Health Aging 2015;19(3): 276–83
Darvin K, Randolph A, Ovalles S et al. Plasma protein biomarkers of the geriatric syndrome. J Gerontol A Biol Sci Med Sci 2014;69(2):182–186
Collerton J, Martin-Ruiz C, Davies K et al. Frailty and the role of inflammation, immunosenescence and cellular ageing in the very old: cross-sectional findings from the Newcastle 85+ study. Mech Ageing Dev 2012;133(6):456–466
Perry RT, Collins JS, Wiener H et al. The role of TNF and its receptors in Alzheimer’s disease. Neurobiol Aging 2001;22(6):873–883
Yeap BB, Paul Chubb SA, Lopez D et al. Associations of insulin-like growth factor-1 and its binding proteins and testosterone with frailty in older men. Clinical Endocrinology 2013;78: 752–759
Mustafa A, Lannfelt L, Lilius L et al. Decreased plasma insulin-like growth factor-1 level in familial Alzheimer’s disease patients carrying the Swedish APP 670/671 mutation. Dement Geriatr Cogn Disord 1999;10:446–451
Watanabe T, Miyazaki A, Katagiri T et al. Relationship between serum insulin-like growth factor-1 levels and Alzheimer’s disease and vascular dementia. J Am Geriatr Soc 2005;53: 1748–1753
Cappola AR, Xue QL, Ferrucci L et al. Insulin-like growth factor 1 and interleukin-6 contribute synergistically to disability and mortality in older women. J Clin Endocrinol Metab 2008;88:2019–2025
De Benedetti F, Alonzi T, Moretta A et al. Interleukin 6 causes growth impairment in transgenic mice through a decrease in insulin-like growth factor-I. A model for stunted growth in children with chronic inflammation. J Clin Invest Feb 1997;15;99(4):643–50
Lelbach A, Scharf JG, Ramadori G. Regulation of insulin-like growth factor-I and of insulin- like growth factor binding protein-1, -3 and -4 in cocultures of rat hepatocytes and Kupffer cells by interleukin-6. J Hepatol Nov; 2001;35(5):558–67
Suzuki T, Suzuki N, Daynes RA et al. Dehydroepiandrosterone enhances IL2 production and cytotoxic effector function of human T cells. Clin Immunol Immunopathol 1991;61:202–11
Morris JC. The Clinical Dementia Rating (CDR): current version and scoring rules. Neurology 1993;43:2412–2414
Sahadevan S, Lim JP, Tan NJ, Chan SP. Psychometric identification of early Alzheimer disease in an elderly Chinese population with differing educational levels. Alzheimer Dis Assoc Disord 2002;16:65–72.
Sahadevan S, Lim PP, Tan NJ, Chan SP. Diagnostic performance of two mental status tests in the older Chinese: influence of education and age on cut-off values. Int J Geriatr Psychiatry 2000;15:234–41
McKhann G, Drachmann DA, Folstein M, Katzman R, Price DL, Stadlan EM. Clinical diagnosis of Alzheimer’s disease–report to the NINCDS-ADRDA workgroup under the auspices of Department of Health and Human Services Task Force on Alzheimer’s disease. Neurology 1984;34:939–44.
Lim WS, Chin JJ, Lam CK, Lim PP, Sahadevan S. Clinical dementia rating: experience of a multi-racial Asian population. Alzheimer Dis Assoc Disord 2005;19:135–42.
Chong MS, Sahadevan S. An Evidence-based Clinical Approach to the Diagnosis of Dementia. Ann Acad Med Singapore 2003;23:740–9.
Williams, M. M., Storandt, M., Roe, C. M. and Morris JC. Progression of Alzheimer’s disease as measured by Clinical Dementia Rating Sum of Boxes scores. Alzheimer’s and Dementia 2013;S39–S44
Wolf PA, D Agostino RB, Belanger AJ et al. Probability of stroke: a risk profile from the Framingham study. Stroke 1991;22(3): 312–318
Mahoney FI, Barthel D. Functional evaluation: the Barthel Index. Maryland State Medical Journal1 1965;4:56–61.
Barberger-Gateau P, Commenges D, Gagnon M, Letenneur L, Sauvel C, Dartigues JF. Instrumental activities of daily living as a screening tool for cognitive impairment and dementia in elderly community dwellers. J American Geriatr Soc 1992;40:1129–1134
Guralnik JM, Simonsick EM, Ferruci L et al. A short physical performance battery assessing lower extremity function: Association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol 1994;49(2):M85–94
Wade DT, Legh-Smith J, Langton Hewer R. Social activities after stroke: measurement and natural history using the Frenchay Activities Index. Int Rehabil Med 1985;7(4):176–81
Chan M, Lim YP, Ernest A, Tan TL. Nutritional assessment in an Asian nursing home and its association with mortality. J Nutr Health Aging. Jan;2010;14(1):23–8
Wahlund LO, Barkhof F, Fazekas F et al. A new rating scale for age-related white matter changes applicable to MRI and CT. Stroke. 2001;32:1318–22. 23.
Wahlund LO, Julin P, Johansson SE, Scheltens P. Visual rating and volumetry of the medial temporal lobe on magnetic resonance imaging in dementia: a comparative study. J Neurol Neurosurg Psychiatry 2000;69:630–5.
Metti AL, Yaffe K, Boudreau RM et al. Change in inflammatory markers and cognitive status in the oldest-old women from the Study of Osteoporotic Fractures. J Am Geriatr Soc 2014;62:662–666
Leng SX, Hung W, Cappola AR et al. White blood cell counts, insulin-like growth factor-1 levels, and frailty in community-dwelling older women. J Gerontol A Biol Sci Med Sci 2009;64A(4): 499–502
Andreassen M, Raymond I, Hillbrandt P et al. Associations between plasma insulin-like growth factor-1 and the markers of inflammation interleukin-6, c-reactive protein and YKL-40 in an elderly background population. Inflamm Res 2010;59(7): 503–10
Andreassen M, Raymond I, Kristorp C et al. IGF1 as a predictor of all-cause mortality and cardiovascular disease in an elderly population. Eur J Endocrinol 2009;160(1): 25–31
Naylor JC, Hulette CM, Steffens DC et al. Cerebrospinal fluid dehydroepiandrosterone levels are correlated with brain dehydroepiandrosterone levels, elevated in Alzheimer’s disease, and related with neuropathological disease stage. J Clin Endocrinol Metab 2008;93:3178–3178
Valenti G, Ferrucci L, Lauretani F et al. Dehydroepiandrosterone sulfate and cognitive function in the elderly: The InCHIANTI Study. J Endocrinol Invest 2009;32:766–72
Satizabal CL, Zhu YC, Mazoyer B et al. Circulating IL-6 and CRP are associated with MRI findings in the elderly. The 3C-Dijon study. Neurology 2012;78: 720–727
Morley JE, Vellas B, van Kan GA et al. Frailty consensus: a call to action. J Am Med Dir Assoc 2013;14(6): 392–7
Mijnarends DM, Schols JM, Meijers JM et al. Instruments to assess sarcopenia and physical frailty in older people living in a community (care) setting: similarities and discrepancies. J Am Med Dir Assoc 2015;16(4): 301–8
Nishiguchi S, Yamada M, Fukutani N et al. Differential association of frailty with cognitive decline and sarcopenia in community-dwelling older adults. J Am Med Dir Assoc 2015;16(2): 120–4
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tay, L., Lim, W.S., Chan, M. et al. The independent role of inflammation in physical frailty among older adults with mild cognitive impairment and mild-to-moderate Alzheimer’s disease. J Nutr Health Aging 20, 288–299 (2016). https://doi.org/10.1007/s12603-015-0617-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-015-0617-6