Abstract
Objective
This study examines whether risk factors for poor nutrition are associated with global cognitive function three years after confirmed Parkinson’s disease (PD) diagnosis.
Design
The follow-up investigations for this prospective community-based study were conducted three years after PD diagnosis.
Setting
The study participants lived in Västerbotten County, a region in northern Sweden with 142,000 inhabitants.
Participants
This study population consisted of 118 PD outpatients from the study of Newly Diagnosed PD in Umeå (NYPUM).
Measurements
Global cognition was assessed with the Mini Mental State Examination (MMSE) at baseline and at follow-up. Anthropometry, nutrition (Mini Nutritional Assessment, MNA, 3-day food registration, 3-FDR), olfactory function (Brief Smell Identification Test, B-SIT), and swallowing, cutting food, and salivation (single questions from the Unified Parkinson’s Disease Rating Scale, UPDRS) were used as markers for nutritional status.
Results
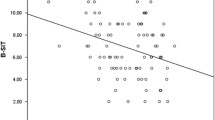
The MMSE score decreased over three years (–1.06±3.38, p=0.001). Olfactory function at baseline was associated to MMSE at three years (B=0.365, p=0.004). Changes in waist/hip ratio (B=113.29, p=0.017), swallowing (B=1.18, P=0.033), and cutting food (B=-1.80, p=0.000) were associated with MMSE at follow-up.
Conclusion
This study indicates that olfactory function, cutting food, swallowing, and visceral obesity are associated with MMSE three years after PD diagnosis.
Similar content being viewed by others
References
Barichella M, Cereda E, Madio C, Iorio L, Pusani C, Cancello R, et al. Nutritional risk and gastrointestinal dysautonomia symptoms in Parkinson’s disease outpatients hospitalised on a scheduled basis. Br J Nutr. 2013; 110: 347–53.
Heetun ZS, Quigley EM. Gastroparesis and Parkinson’s disease: A systematic review Parkinsonism Relat Disord. 2012; 18:433–40.
Martinez-Martin P, Falup Pecurariu C, Odin P, van Hilten JJ, Antonini A, Rojo-Abuin JM, et al. Gender-related differences in the burden of non-motor symptoms in Parkinson’s disease. J Neurol. 2012; 259:1639–47.
Elgh E, Domellöf M, Linder J, Edström M, Stenlund H, Forsgren L. Cognitive function in early Parkinson’s disease: a population-based study. Eur J Neurol. 2009; 16:1278–84.
Muslimovic D, Post B, Speelman JD, Schmand B. Cognitive profile of patients with newly diagnosed Parkinson disease. Neurology 2005; 25:1239–45.
Foltynie T, Brayne CE, Robbins TW, Barker RA. The cognitive ability of an incident cohort of Parkinsons patients in the UK. Brain. 2004; 127: 550–60.
Aarsland D, Brønnick K, Larsen JP, Tysnes OB, Alves G. Cognitive impairment in incident, untreated Parkinson disease: the Norwegian ParkWest study. Neurology 2009; 72:1121–6.
Sheard JM, Ash S, Mellick GD, Silburn PA, Kerr G K. Malnutrition in a sample of community-dwelling people with Parkinson’s disease. PLoS One. 2013; 8:e53290.
Sheard JM, Ash S, Silburn PA, Kerr GK. Nutritional status in Parkinson’s disease patients undergoing deep brain stimulation surgery: a pilot study. J Nutr Health Aging 2013; 17: 148–51.
Morley JE. Cognition and nutrition. Curr Opin Clin Nutr Metab Care. 2014; 17:1–4.
Andersson I, Sidenvall B. Case studies of food shopping, cooking and eating habits in older women with Parkinson’s disease. J Adv Nurs. 2001; 35:69–78.
Ådén E, Carlsson M, Poortvliet E, Stenlund H, Linder J, Edström M, et al. Dietary intake and olfactory function in patients with newly diagnosed Parkinson’s disease: a case-control study. Nutr Neurosci 2011; 14: 25–31.
Schubert CR, Carmichael LL, Murphy C, Klein BEK, Klein R, Cruickshanks KJ. Olfaction and the 5-year incidence of cognitive impairment in an epidemiologic study of older adults. J Am Geriatr Soc 2008; 56: 1517–21.
Strupeit S, Meyer S, Buss A, Gräske J, Worch A, Wolf-Ostermann K. Influence of living situation on vulnerable elderly: focus on nutritional status. J Nutr Health Aging 2014; 18: 787–91.
Sheard JM, Ash S, Mellick GD, Silburn PA, Kerr GK. Markers of disease severity are associated with malnutrition in Parkinson’s disease. PLoS One 2013; 8: e57986.
Linder J, Stenlund H, Forsgren L. Incidence of Parkinson’s disease and Parkinsonism in northern Sweden: a population-based study. Mov Disord 2010; 25: 341–8.
Fahn S, Elton RL, the UPDRS Development Committee. Unified Parkinson’s disease rating scale. In: Fahn S, Marsden CD, Calne D, Goldstein M, Eds. Recent developments in Parkinson’s disease. Florham Park, NJ: Macmillan Healthcare Information; 1987: 153–64.
Gibb WR, Lees AJ. The relevance of the Lewy body to the pathogenesis of idiopathic Parkinson’s disease. J Neurol Neurosurg Psychiatry 1988; 51: 745–52.
Hoehn MM, Yahr MD. Parkinsonism: onset, progression and mortality. Neurology 1967; 17: 427–42.
Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 1975; 12: 189–98.
Doty RL, Marcus A, Lee WW. Development of the 12-item Cross-Cultural Smell Identification Test (CC-SIT). Laryngoscope. 1996; 106(3 Pt 1): 353–6. (B-SIT)
Vikdahl M, Carlsson M, Linder J, Forsberg L, Håglin L. Wei ght gain and increased central obesity in the early phase of Parkinson’s disease. Clin Nutr. doi: 10.1016/j.clnu.2013.12.012.
Nicaretta H D, Rosso A L, de Mattos J P, Maliska C, Costa M B M. Dysphagia and sialorrhea: the relationship to Parkinson’s disease. Arq Gastroenterol. 2013; 50:42–9.
van Steijn J, van Harten B, Flapper E, Droogsma E, van Walderveen, Blaauw M, et al. The nutritional status of Dutch elderly patients with Parkinson’s disease. J Nutr Health Aging. 2014; 18:601–7.
Khoo TK, Yarnall AJ, Duncan GW, Coleman S, O’Brien JT, Brooks DJ, et al. The spectrum of nonmotor symptoms in early Parkinson Disease. Neurology. 2013; 80:276–81.
Karpa MJ, Gopinath B, Rochtchina E, Wang JJ, Gumming R G, Sue C M, et al. Prevalence and neurodegenerative or other associations with olfactory impairment in an older community. J Aging Health. 2010; 22; 154–68.
Lee JE, Cho KH, Ham JH, Song SK, Sohn YH, Lee PH. Olfactory performance acts as a cognitive reserve in non-demented patients with Parkinson’s disease. Parkinsonism Relat Disord. 2014; 20:186–91.
Coin A, Veronese N, De Rui M, Mosele M, Bolzetta F, Girardi A, et al. Nutritional predictors of cognitive impairment severity in demented elderly patients: the key role of BMI. J Nutr Health Aging. 2012; 16:553–6.
Kurth F, Levitt JG, Philips OR, Luders E, Woods RP, Mazziotta JC, et al. Relationships between gray matter, body mass index and waist circumference in healthy adults. Hum Brain Mapp. 2013; 34:1737–46.
Cereda E, Sansone V, Meola G, Malavazos AE. Increased visceral adipose tissue rather than BMI as a risk factor for dementia. Age Ageing 2007; 36:488–91.
Wirth R, Smoliner C, Sieber CC, Volkert D. Cognitive function is associated with body composition and nutritional risk of geriatric patients. J Nutr Health Aging 2011; 15:706–10.
Heller J, Dogan I, Schulz JB, Reetz K. Evidence for gender differences in cognition, emotion and quality of life in Parkinson’s disease. Aging and Disease 2014; 1: 63–75.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vikdahl, M., Domellöf, M.E., Forsgren, L. et al. Olfactory function, eating ability, and visceral obesity associated with MMSE three years after Parkinson’s disease diagnosis. J Nutr Health Aging 19, 894–900 (2015). https://doi.org/10.1007/s12603-015-0573-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-015-0573-1