Abstract
Background
Neonates with ABO hemolytic disease are at greater risk for developing significant hyperbilirubinemia. We aimed to determine whether sixth hour transcutaneous bilirubin (TcB) could predict such a risk.
Methods
TcB measurements were obtained at the 6th hour of life in blood group A or B neonates born to blood group O, rhesus factor compatible mothers. Subsequent hyperbilirubinemia was monitored and considered significant if a neonate required phototherapy/exchange transfusion. The predictive role of sixth hour TcB was estimated.
Results
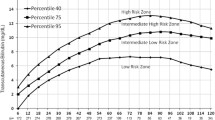
Of 144 ABO incompatible neonates, 41(OA, 24; O-B, 17) had significant hyperbilirubinemia. Mean sixth hour TcB was significantly higher among neonates who developed significant hyperbilirubinemia than those who did not (5.83±1.35 mg/dL vs. 3.65±0.96 mg/dL, P<0.001). Sixth hour TcB value >4 mg/dL had the highest sensitivity of 93.5% and >6 mg/dL had the highest specificity of 99%. Area under receiver operating characteristic curve was 0.898.
Conclusion
Sixth hour TcB predicts subsequent significant hyperbilirubinemia in ABO incompatible neonates.
Similar content being viewed by others
References
Maisels MJ, Kring E. Length of stay, jaundice, and hospital readmission. Pediatrics 1998;101:995–998.
Bhutani VK, Johnson LH, Keren R. Diagnosis and management of hyperbilirubinemia in the term neonate: for a safer first week. Pediatr Clin North Am 2004;51:843–861, vii.
Madam A, MacMonon JR, Stevenson DK. Neonatal Hyperbilirubinemia. In: Taeusch HW, Ballard RA, Gleason CA, eds. Avery’s Disease of the Newborn, 8th ed. Philadelphia: Saunders, 2005: 1226–1250.
Sarici SU, Yurdakök M, Serdar MA, Oran O, Erdem G, Tekinalp G, et al. An early (sixth-hour) serum bilirubin measurement is useful in predicting the development of significant hyperbilirubinemia and severe ABO hemolytic disease in a selective high-risk population of newborns with ABO incompatibility. Pediatrics 2002;109:e53.
Quinn MW, Weindling AM, Davidson DC. Does ABO incompatibility matter? Arch Dis Child 1988;63:1258–1260.
Whyte J, Graham H. Prediction of the severity of ABO haemolytic disease of the newborn by cord blood tests. Acta Paediatr Scand 1981;70:217–222.
Brouwers HA, Overbeeke MA, van Ertbruggen I, Schaasberg W, Alsbach GP, van der Heiden C, et al. What is the best predictor of the severity of ABO-haemolytic disease of the newborn? Lancet 1988;2:641–644.
Han P, Kiruba R, Ong R, Joseph R, Tan KL, Wong HB. Haematolytic disease due to ABO incompatibility: incidence and value of screening in an Asian population.. Aust Paediatr J 1988;24:35–38.
Levine DH, Meyer HB. Newborn screening for ABO hemolytic disease. Clin Pediatr (Phila) 1985;24:391–394.
Bhutani VK, Johnson L, Sivieri EM. Predictive ability of a predischarge hour-specific serum bilirubin for subsequent significant hyperbilirubinemia in healthy term and near-term newborns. Pediatrics 1999;103:6–14
Bhat YR, Rao A. Transcutaneous bilirubin in predicting hyperbilirubinemia in term neonates. Indian J Pediatr 2008;75:119–123.
Speck WT. A guide to the use of phototherapy in the management of neonatal hyperbilirubinemia. Commentary. J Pediatr 1979;95:285–287.
Maisels MJ. Neonatal hyperbilirubinemia and kernicterus — not gone but sometimes forgotten. Early Hum Dev 2009;85:727–732.
Bhutani VK, Vilms RJ, Hamerman-Johnson L. Universal bilirubin screening for severe neonatal hyperbilirubinemia. J Perinatol 2010;30Suppl:S6–15.
Maisels MJ. Screening and early postnatal management strategies to prevent hazardous hyperbilirubinemia in newborns of 35 or more weeks of gestation. Semin Fetal Neonatal Med 2010;15:129–135.
Randev S, Grover N. Predicting neonatal hyperbilirubinemia using first day serum bilirubin levels. Indian J Pediatr 2010;77:147–150.
Osborn LM, Lenarsky C, Oakes RC, Reiff MI. Phototherapy in full-term infants with hemolytic disease secondary to ABO incompatibility. Pediatrics 1984;74:371–374.
Alpay F, Sarici SU, Tosuncuk HD, Serdar MA, Inanç N, Gökçay E. The value of first-day bilirubin measurement in predicting the development of significant hyperbilirubinemia in healthy term newborns. Pediatrics 2000;106:E16.
Lucas GN. Neonatal jaundice due to ABO incompatibility in Sri Lankan. Indian J Pediatr 1996;63:381–384.
Watchko JF. Identification of neonates at risk for hazardous hyperbilirubinemia: emerging clinical insights. Pediatr Clin North Am 2009;56:671–687.
Bucher KA, Patterson AM Jr, Elston RC, Jones CA, Kirkman HN Jr. Racial difference in incidence of ABO hemolytic disease. Am J Public Health 1976;66:854–858.
Kaplan M, Hammerman C, Vreman HJ, Wong RJ, Stevenson DK. Hemolysis and hyperbilirubinemia in antiglobulin positive, direct ABO blood group heterospecific neonates. J Pediatr 2010;157:772–777.
Schutzman DL, Sekhon R, Hundalani S. Hour-specific bilirubin nomogram in infants with ABO incompatibility and direct Coombs-positive results. Arch Pediatr Adolesc Med 2010;164:1158–1164.
Lease M, Whalen B. Assessing jaundice in infants of 35-week gestation and greater. Curr Opin Pediatr 2010;22:352–365.
Stoniene D, Buinauskiene J, Markūniene E. The value of transcutaneous method of bilirubin measurement in newborn population with the risk of ABO hemolytic disease. Medicina (Kaunas) 2009;45:792–797.
American Academy of Pediatrics, Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics 2004;114:297–316.
Trikalinos TA, Chung M, Lau J, Ip S. Systematic review of screening for bilirubin encephalopathy in neonates. Pediatrics 2009;124:1162–1171.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bhat, R.Y., Kumar, P.C.G. Sixth hour transcutaneous bilirubin predicting significant hyperbilirubinemia in ABO incompatible neonates. World J Pediatr 10, 182–185 (2014). https://doi.org/10.1007/s12519-013-0421-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-013-0421-5