Abstract
Background
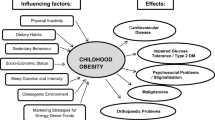
Childhood obesity is associated with adverse changes in cardiometabolic risk factors. A family-oriented group program stressing a health-promoting lifestyle has been more effective than routine counselling in the treatment of obesity in school children. The aim of the present study was to compare the impact of group program and routine councelling on body composition and metabolic profile, and to evaluate the associations of changes in adiposity with levels of cardiometabolic risk factors.
Methods
Seventy obese prepubertal children were randomized into family-oriented group program (15 sessions for parents and children) and routine counselling (2 appointments for children). Body mass index (BMI), body composition and different metabolic risk factors were assessed before and after the 6-month intervention.
Results
Waist/height decreased more in the children attending the group treatment, but there were no significant differences between treatment arms in the changes of metabolic risk factors. When the arms were analyzed as combined, serum triglycerides decreased significantly if BMI standard deviation score (BMI-SDS) decreased ≥0.5. Serum fasting insulin decreased if BMISDS decreased ≥0.25.
Conclusions
Obesity-related metabolic risk factors reduced in prepubertal children if BMI-SDS decreased substantially. This result was not dependent on which intervention, family-oriented group program or routine counselling, was used.
Similar content being viewed by others
References
Reilly JJ, Methven E, McDowell ZC, Hacking B, Alexander D, Stewart L, et al. Health consequences of obesity. Arch Dis Child 2003;88:748–752.
Garcés C, Gutierrez-Guisado J, Benavente M, Cano B, Viturro E, Ortega H, et al. Obesity in Spanish schoolchildren: relationship with lipid profile and insulin resistance. Obes Res 2005;13:959–963.
Zimmet P, Alberti G, Kaufman F, Tajima N, Silink M, Arslanian S, et al. The metabolic syndrome in children and adolescents. Lancet 2007;369:2059–2061.
Baker JL, Olsen LW, Sorensen TI. Childhood body-mass index and the risk of coronary heart disease in adulthood. N Engl J Med 2007;357:2329–2337.
Jiang JX, Xia XL, Greiner T, Lian GL, Rosenqvist U. A two year family based behaviour treatment for obese children. Arch Dis Child 2005;90:1235–1238.
Nemet D, Barkan S, Epstein Y, Friedland O, Kowen G, Eliakim A. Short- and long-term beneficial effects of a combined dietary-behavioral-physical activity intervention for the treatment of childhood obesity. Pediatrics 2005;115:e443–e449.
Golley RK, Magarey AM, Baur LA, Steinbeck KS, Daniels LA. Twelve-month effectiveness of a parent-led, family-focused weight-management program for prepubertal children: a randomized, controlled trial. Pediatrics 2007;119:517–525.
Savoye M, Shaw M, Dziura J, Tamborlane WV, Rose P, Guandalini C, et al. Effects of a weight management program on body composition and metabolic parameters in overweight children: a randomized controlled trial. JAMA 2007;297:2697–2704.
Reinehr T, Andler W. Changes in the atherogenic risk factor profile according to degree of weight loss. Arch Dis Child 2004;89:419–422.
Reinehr T, Kiess W, Kapellen T, Andler W. Insulin sensitivity among obese children and adolescents, according to degree of weight loss. Pediatrics 2004;114:1569–1573.
Kalavainen MP, Korppi MO, Nuutinen OM. Clinical efficacy of group-based treatment for childhood obesity compared with routinely given individual counselling. Int J Obes (Lond) 2007;31:1500–1508.
Kalavainen M, Karjalainen S, Martikainen J, Korppi M, Linnosmaa I, Nuutinen O. Cost-effectiveness of routine and group programs for treatment of obese children. Pediatr Int 2009;51:606–611.
Tilator Oy Ltd. Pediator software for growth data [computer program]. Version Release 6.7.4. Säkylä, Finland, 2004.
Pere A. Comparison of two methods for transforming height and weight to normality. Ann Hum Biol 2000;27:35–45.
Sorva R, Lankinen S, Tolppanen EM, Perheentupa J. Variation of growth in height and weight of children. II. After infancy. Acta Paediatr Scand 1990;79:498–506.
Northwest Institute for Bio-Health Informatics: child obesity calculator using British 1990 growth reference data. http://www.phsim.man.ac.uk/ (accessed January 18, 2007).
Cole TJ, Freeman JV, Preece MA. Body mass index reference curves for the UK, 1990. Arch Dis Child 1995;73:25–29.
Freeman JV, Cole TJ, Chinn S, Jones PR, White EM, Preece MA. Cross-sectional stature and weight reference curves for the UK, 1990. Arch Dis Child 1995;73:17–24.
Cole TJ, Freeman JV, Preece MA. British 1990 growth reference centiles for weight, height, body mass index and head circumference fitted by maximum penalized likelihood. Stat Med 1998;17:407–429.
Cole TJ. The LMS method for constructing normalized growth standards. Eur J Clin Nutr 1990;44:45–60.
McCarthy HD, Ashwell M. A study of central fatness using waist-to-height ratios in UK children and adolescents over two decades supports the simple message—’keep your waist circumference to less than half your height’. Int J Obes (Lond) 2006;30:988–992.
Bedogni G, Malavolti M, Severi S, Poli M, Mussi C, Fantuzzi AL, et al. Accuracy of an eight-point tactile-electrode impedance method in the assessment of total body water. Eur J Clin Nutr 2002;56:1143–1148.
Tanner JM, Whitehouse RH. Clinical longitudinal standards for height, weight, height velocity, weight velocity, and stages of puberty. Arch Dis Child 1976;51:170–179.
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 1985;28:412–419.
Utriainen P, Voutilainen R, Jaaskelainen J. Continuum of phenotypes and sympathoadrenal function in premature adrenarche. Eur J Endocrinol 2009;160:657–665.
Schwandt P, Kelishadi R, Haas GM. First reference curves of waist circumference for German children in comparison to international values: the PEP family heart study. World J Pediatr 2008;4:259–266.
Jackson LV, Thalange NK, Cole TJ. Blood pressure centiles for Great Britain. Arch Dis Child 2007;92:298–303.
Ford AL, Hunt LP, Cooper A, Shield JP. What reduction in BMI SDS is required in obese adolescents to improve body composition and cardiometabolic health? Arch Dis Child 2010;95:256–261.
Tuomilehto J, Lindström J, Eriksson JG, Valle TT, Hämäläinen H, Ilanne-Parikka P, et al. Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N Engl J Med 2001;344:1343–1350.
Wunsch R, de Sousa G, Toschke AM, Reinehr T. Intimamedia thickness in obese children before and after weight loss. Pediatrics 2006;118:2334–2340.
Schiel R, Beltschikow W, Radon S, Kramer G, Perenthaler T, Stein G. Increased carotid intima-media thickness and associations with cardiovascular risk factors in obese and overweight children and adolescents. Eur J Med Res 2007;12:503–508.
Pinhas-Hamiel O, Lerner-Geva L, Copperman NM, Jacobson MS. Lipid and insulin levels in obese children: changes with age and puberty. Obesity (Silver Spring) 2007;15:2825–2831.
Kyle UG, Bosaeus I, De Lorenzo AD, Deurenberg P, Elia M, Manuel Gómez J, et al. Bioelectrical impedance analysis-part II: utilization in clinical practice. Clin Nutr 2004;23:1430–1453.
Kalavainen M, Korppi M, Nuutinen O. Long-term efficacy of group-based treatment for childhood obesity compared with routinely given individual counselling. Int J Obes (London) 2011;35:530–533.
Schiel R, Beltschikow W, Radón S, Kramer G, Schmiedel R, Berndt RD, et al. Long-term treatment of obese children and adoloscents using a telemedicine support programme. J Telemed Telecare 2008;14:13–16.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kalavainen, M., Utriainen, P., Vanninen, E. et al. Impact of childhood obesity treatment on body composition and metabolic profile. World J Pediatr 8, 31–37 (2012). https://doi.org/10.1007/s12519-011-0324-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-011-0324-2