Abstract
Background
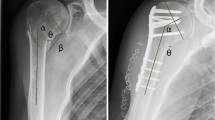
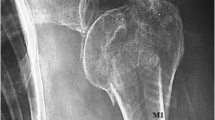
The risk of post-traumatic humeral head avascular necrosis (AVN), regardless of the treatment, has a high reported incidence. In 2004, Hertel et al. stated that the most relevant predictors of ischemia after intracapsular fracture treated with osteosynthesis are the calcar length, medial hinge integrity and some specific fracture types. Based on Hertel’s model, the purpose of this study is to evaluate both its reliability and weaknesses in our series of 267 fractures, assessing how the anatomical configuration of fracture, the quality of reduction and its maintenance were predictive of osteonecrosis development, and so to suggest a treatment choice algorithm.
Materials and methods
A retrospective study, level of evidence IV, was conducted to duly assess the radiographic features of 267 fractures treated from 2004 to 2010 following Hertel’s criteria treated with open reduction and internal fixation by angular stability plates and screws. The average age was 65.2 years. The average follow-up was 28.3 ± 17.0 months. The percentage of AVN, the quality and maintenance of reduction obtained during surgery were evaluated.
Results
The AVN incidence was 3.7 %. No significant correlation with gender, age and fracture type was found. At the last follow-up X-ray, only 30 % presented all Hertel’s good predictors in the AVN group, 4.7 % in the non-AVN group (p < 0.05). About quality of reduction in the AVN group, it was poor in 50 %; while in the non-AVN group, it was poor in 3.4 % (p < 0.05). Four patients with AVN were symptomatic, and three needed a second surgery.
Conclusions
Hertel’s criteria are important in the surgical planning, but they are not sufficient: an accurate evaluation of the calcar area fracture in three planes is required. All fractures involving calcar area should be studied with CT.
Level of evidence
IV.



Similar content being viewed by others
References
Bastian JD, Hertel R (2008) Initial post-fracture humeral head ischemia does not predict development of necrosis. J Shoulder Elbow Surg 17:2–8. doi:10.1016/j.jse.2007.03.026
Brunner F, Sommer C, Bahrs C, Heuwinkel R, Hafner C, Rillmann P et al (2009) Open reduction and internal fixation of proximal humerus fractures using a proximal humeral locked plate: a prospective multicenter analysis. J Orthop Trauma 23:163–172. doi:10.1097/BOT.0b013e3181920e5b
Clavert P, Adam P, Bevort A, Bonnomet F, Kempf J-F (2010) Pitfalls and complications with locking plate for proximal humerus fracture. J Shoulder Elbow Surg 19:489–494. doi:10.1016/j.jse.2009.09.005 Epub 2009 Dec 7
Cruess RL (1978) Experience with steroid-induced avascular necrosi of the shoulder and etiologic considerations regarding osteonecrosis of the hip. Clin Orthop Relat Res 130:86–93
Ficat P, Arlet J (1973) Pre-radiologic stage of femur head osteonecrosis: diagnostic and therapeutic possibilities. Rev Chir Orthop Reparatrice Appar Mot 59(Suppl 1):26–38
Gerber C, Schneeberger AG, Vinh TS (1990) The arterial vascularization of the humeral head. An anatomical study. J Bone Joint Surg Am 72:1486–1494
Gerber C, Werner CM, Vienne P (2004) Internal fixation of complex fractures of the proximal humerus. J Bone Joint Surg Br 86:848–855. doi:10.1302/0301-620X.86B6
Gregory TM, Vandenbussche E, Augereau B (2013) Surgical treatment of three and four-part proximal humeral fractures. Orthop Traumatol: Surg Res 99S:S197–S207. doi:10.1016/j.otsr.2012.12.006
Greiner S, Kaab MJ, Haas NP, Bail HJ (2009) Humeral head necrosis rate at mid-term follow-up after open reduction and angular stable plate fixation for proximal humeral fractures. Injury 40:186–191. doi:10.1016/j.injury.2008.05.030
Hardeman F, Bollars P, Donnelly M, Bellemans J, Nijs S (2012) Predictive factors for functional outcome and failure in angular stable osteosynthesis of the proximal humerus. Inj Int J Care Inj 43:153–158. doi:10.1016/j.injury.2011.04.003
Hente R, Kampshoff J, Kinner B et al (2004) Treatment of dislocated 3- and 4-part fractures of the proximal humerus with an angle-stabilizing fixation plate. Unfallchirurg 107:769–782. doi:10.1007/s00113-004-0818-7
Hertel R, Hempfing A, Stiehler M, Leunig M (2004) Predictors of humeral head ischemia after intracapsular fracture of the proximal humerus. J Shoulder Elbow Surg 13:427–433. doi:10.1016/j.jse.2004.01.034
Hessmann M, Baumgaertel F, Gehling H, Klingelhoeffer I, Gotzen L (1999) Plate fixation of proximal humeral fractures with indirect reduction: surgical technique and results utilizing three shoulder scores. Injury 30:453–462. doi:10.1016/S0020-1383(99)00111-4
Hettrich CM, Boraiah S, Dyke JP, Neviaser A, Helfet DL, Lorich DG (2010) Quantitative assessment of the vascularity of the proximal part of the humerus. J Bone Joint Surg Am 92:943–948. doi:10.2106/JBJS.H.01144
Hirschmann MT, Quarz V, Audigé L (2007) Internal fixation of unstable proximal humerus fractures with an anatomically preshaped interlocking plate: a clinical and radiologic evaluation. J Trauma 63:1314–1323. doi:10.1097/01.ta.0000240457.64628.38
Jost B, Spross C, Grehn H, Gerber C (2013) Locking plate fixation of fractures of the proximal humerus: analysis of complications, revision strategies and outcome. J Shoulder Elbow Surg 22(4):542–549. doi:10.1016/j.jse.2012.06.008
Jung WB, Moon ES, Kim SK, Kovacevic D, Kim MS (2013) Does medial support decrease major complications of unstable proximal humerus fractures treated with locking plate? BMC Musculoskelet Disord 14:102. doi:10.1186/1471-2474-14-102
L’Insalata JC, Pagnani MJ, Warren RF, Dines DM (1996) Humeral head osteonecrosis: clinical course and radiographic predictors of outcome. J Shoulder Elbow Surg 5:355–361
Plecko M, Kraus A (2005) Internal fixation of proximal humerus fractures using the locking proximal humerus plate. Oper Orthop Traumatol 17:25–50
Reineck JR, Krishnan SG, Burkhead WZ (2007) Four-part proximal humerus fractures: evaluation and treatment. Hand Clin 23:415–424. doi:10.1016/j.hcl.2007.09.006
Russo R, Cautiero F, Della Rotonda G (2012) The classification of complex 4-part humeral fractures revisited: the missing fifth fragment and indications for surgery. Musculoskelet Surg 96(Suppl 1):S13–S19. doi:10.1007/s12306-012-0195-2
Soliman OA, Koptan WMT (2013) Four-part fracture dislocations of the proximal humerus in young adults: results of fixation. Inj Int J Care Inj 44:442–447. doi:10.1016/j.injury.2012.09.005
Sproul RC, Iyengar JJ, Devcic Z, Feeley BT (2011) A systematic review of locking plate fixation of proximal humerus fractures. Inj Int J Care Inj 42:408–413. doi:10.1016/j.injury.2010.11.058
Widnall JC, Dheerendra SK, Malal JJ, Waseem M (2013) Proximal humeral fractures: a review of current concepts. Open Orthop J 7(Suppl 3: M12):361–365. doi:10.2174/1874325001307010361
Wijgman AJ, Roolker W, Patt TW (2002) Open reduction and internal fixation of three and four-part fractures of the proximal part of the humerus. J Bone Joint Surg Am 84A:1919–1925
Informed consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000 (5). All patients provided written informed consent for enrollment in the study and for the inclusion in this article of information that could potentially lead to their identification.
Human and animal rights
The study was conducted in accordance with all institutional and national guidelines for the care and use of laboratory animals.
Conflict of interest
Campochiaro Gabriele, Rebuzzi Manuela, Baudi Paolo, Catani Fabio declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Campochiaro, G., Rebuzzi, M., Baudi, P. et al. Complex proximal humerus fractures: Hertel’s criteria reliability to predict head necrosis. Musculoskelet Surg 99 (Suppl 1), 9–15 (2015). https://doi.org/10.1007/s12306-015-0358-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-015-0358-z