Abstract
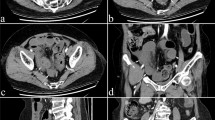
Early intestinal obstruction is easily misdiagnosed. Many physicians consider terminal bouton if computed tomography (CT) scan is done. However, different examinations provide diverse information and significance. This retrospective, randomized, clinical study investigated the diagnostic value of three imaging modalities for intestinal obstruction, supine and upright (or decubitus) plain abdominal radiography, contrast radiography using Gastrografin, and 64 multi-slice spiral CT (MSCT). A total 142 patients with intestinal obstruction were examined. The diagnostic accuracy of plain radiography, contrast radiography, and MSCT for detecting small bowel obstruction was 62.5, 85, and 77.5 %, for localizing the obstruction was 0, 90, and 78.75 %, and for determining the cause of obstruction was 0, 71, and 65 %, respectively. The diagnostic accuracy for detecting large bowel obstruction was 53.23, 73.17, and 92 %, and for localizing the obstruction was 38.17, 60.98, and 98 %, respectively. The diagnostic accuracy of MSCT in determining the cause of obstruction was 91 %. None of the patients administered Gastrografin experienced any adverse effects. In conclusion, MSCT has great diagnostic value in identifying the site and cause of intestinal obstruction, especially in cases of large bowel obstruction. Contrast radiography using Gastrografin was effective in diagnosing and treating small bowel obstruction, making it a beneficial adjunct to MSCT.
Similar content being viewed by others
References
Cooper JM, Thirlby RC (2002) Small bowel obstruction. Curr Treat Options Gastroenterol 5:3–8
Thompson WM, Kilani RK, Smith BB, Thomas J, Jaffe TA, Delong DM et al (2007) Accuracy of abdominal radiography in acute small-bowel obstruction: does reviewer experience matter? Am J Roentgenol 188:233–238
Megibow AJ, Balthazar EJ, Cho KC, Medwid SW, Birnbaum BA, Noz ME (1991) Bowel obstruction: evaluation with CT. Radiology 180:313–318
Suri RR, Vora P, Kirby JM, Ruo L (2014) Computed tomography features associated with operative management for nonstrangulating small bowel obstruction. Can J Surg 57:254–259
Antonsen J, Tilma J (2014) Images in clinical medicine. Mechanical small-bowel obstruction. N Engl J Med 28:371–379
Menzies D (1992) Peritoneal adhesions. Incidence, cause, and prevention. Surg Annu 24:27–45
Luijendijk RW, de Lange DC, Wauters CC, Hop WC, Duron JJ, Pailler JL (1996) Foreign material in postoperative adhesions. Ann Surg 223:242–248
Parker MC, Ellis H, Moran BJ, Thompson JN, Wilson MS, Menzies D et al (2001) Postoperative adhesions: ten-year follow-up of 12,584 patients undergoing lower abdominal surgery. Dis Colon Rectum 44:822–829
Ellis H (1998) The magnitude of adhesion related problems. Ann Chir Gynaecol 87:9–11
Zhang Y, Gao Y, Ma Q, Dang C, Wei W, De Antoni F et al (2006) Randomised clinical trial investigating the effects of combined administration of octreotide and methylglucamine diatrizoate in the older persons with adhesive small bowel obstruction. Dig Liver Dis 38:188–194
Umman P, Adiyodi V, Narayan C (2013) Small bowel adenocarcinoma—report of two cases and review of literature. Indian J Surg 75:123–127
Coleman G, McLain AD, Moran BJ (2000) Impact of previous surgery on time taken for incision and division of adhesions during laparotomy. Dis Colon Rectum 43:1297–1299
Van Der Krabben AA, Dijkstra FR, Nieuwenhuijzen M, Reijnen MM, Schaapveld M, Van Goor H (2000) Morbidity and mortality of inadvertent enterotomy during adhesiotomy. Br J Surg 87:467–471
Menzies D (1993) Postoperative adhesions: their treatment and relevance in clinical practice. Ann R Coll Surg Engl 75:147–153
Galardi N, Collins J, Friend K (2013) Use of early gastrografin small bowel follow-through in small bowel obstruction management. Am Surg 79:794–796
Assalia A, Schein M, Kopelman D, Hirshberg A, Hashmonai M (1994) Therapeutic effect of oral Gastrografin in adhesive, partial small bowel obstruction: a prospective randomized trial. Surgery 115:433–437
Choi HK, Law WL, Ho JW, Chu KW (2005) Value of Gastrografin in adhesive small bowel obstruction after unsuccessful conservative treatment: a prospective evaluation. World J Gastroenterol 11:3742–3745
Chen SC, Lin FY, Lee PH, Yu SC, Wang SM, Chang KJ (1998) Watersoluble contrast study predicts the need for early surgery in adhesive small bowel obstruction. Br J Surg 85:1692–1694
Stordahl A, Laerum F, Gjolberg T, Enge I (1988) Water-soluble contrast-media in adiography of small bowel obstruction—comparison of ionic and non-ionic contrast-media. Acta Radiol 29:53–56
Branco BC, Barmparas G, Schnuriger B, Inaba K, Chan LS, Demetriades D (2010) Systematic review and meta-analysis of the diagnostic and therapeutic role of water-soluble contrast agent in adhesive small bowel obstruction. Br J Surg 97:470–478
Rahmani N, Mohammadpour RA, Khoshnood P, Ahmadi A, Assadpour S (2013) Prospective evaluation of oral gastrografin® in the management of postoperative adhesive small bowel obstruction. Indian J Surg 75:195–199
Sawai RS (2012) Management of colonic obstruction: a review. Clin Colon Rectal Surg 25:200–203
Hayakawa K, Tanikake M, Yoshida S, Yamamoto A, Yamamoto E, Morimoto T (2013) CT findings of small bowel strangulation: the importance of contrast enhancement. Emerg Radiol 20:3–9
Compliance with Ethical Standards
The authors declare that they have no conflicts of interest. This study was approved by the ethics committee of Xuanwu Hospital, Capital University of Medicine Sciences. All patients provided informed, written consent prior to study enrolment.
Conflict of interest
We declare that we have no conflict of interests. We have no financial and personal relationships with other people or organizations that can inappropriately influence our work.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jun, L., ChangYi, S. Diagnostic Value of Plain and Contrast Radiography, and Multi-slice Computed Tomography in Diagnosing Intestinal Obstruction in Different Locations. Indian J Surg 77 (Suppl 3), 1248–1251 (2015). https://doi.org/10.1007/s12262-015-1269-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-015-1269-9