Abstract
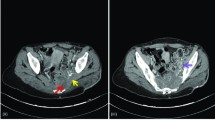
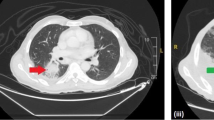
Malakoplakia is a rare inflammatory condition that typically occurs in the urinary tract. The cutaneous form is less prevalent, and most commonly occurs in the perianal or genital regions. Here we present a 61 year old lady with cutaneous malakoplakia of the neck, which was successfully treated with surgical excision and a prolonged course of ciprofloxacin. We follow our case report with a discussion and literature review of all seventeen previously reported cutaneous head and neck malakoplakia cases from the literature. A diagnosis of cutaneous malakoplakia should be considered in nodular, ulcerated or discharging lesions that are refractory to treatment. Histology is essential, not only to diagnose malakoplakia, but also to exclude other important differential diagnoses, such as malignancy. Combined surgical excision and prolonged antibiotic courses appear to have the highest success rate. Antibiotics should be culture specific, but quinolones appear to be the best empirical choice.



Similar content being viewed by others
References
Rubinson R, Mendes VS, Sanchez G, Costantini S. Malakoplakia. Pediatr Dermatol. 2012;29(4):541–3.
Garg M, Eley KA, Bond SE, Shah KA, Browning L, Watt-Smith SR. Malakoplakia presenting as an enlarging neck mass: case presentation and review of the literature. Head Neck. 2010;32(9):1269–72.
Coombes DM, Norris PM, Barrett AW, Brown AE. Malakoplakia of the face: a rare but important diagnosis. Br J Oral Maxillofac Surg. 2010;48(1):55–7.
Akkuzu G, Aydin E, Bilezikçi B, Akkuzu B, Ozluoglu LN. Malakoplakia in nasal vestibule. Otolaryngol Head Neck Surg. 2006;135(4):636–7.
Toubes-Klingler E, Prabhu VC, Bernal K, Poage D, Swindells S. Malacoplakia of the cranium and cerebrum in a human immunodeficiency virus-infected man: case report. J Neurosurg. 2006;104(3):432–5.
Kumar Vinod, Coady MSE. Malakoplakia of the neck in an immunosuppressed patient. Plast Reconstr Surg. 2005;116(6):125e–7e.
Pang LC. Malacoplakia manifesting as a chronic inflammatorymass at the site of a nonhealing surgical wound. Ear Nose Throat J. 2003;82:876–80.
Schmerber S, Lantuejoul S, Lavieille JP, Reyt E. Malakoplakia of the neck. Arch Otolaryngol Head Neck Surgery. 2003;129(11):1240–2.
Enjolras O, Guillemette J, Carlotti A, Plantier F, Jubert C, Escande JP. Cutaneous malacoplakia: a pediatric case. Annales de dermatologie et de venereologie. 1998;125(8):522–4.
Feldmann R, Breier F, Duschet P, Löw-Weiser H, Gschnait F. Cutaneous malakoplakia on the forehead. Dermatology. 1997;194(4):358–60.
Douglas-Jones AG, Rodd C, James EMV, Mills RGS. Prediagnostic malakoplakia presenting as a chronic inflammatory mass in the soft tissues of the neck. J Laryngol Otol. 1992;106(02):173–7.
Nayar RC, Garg I, Alapatt JJ. Malakoplakia of the temporal bone in a nine-month-old infant. J Laryngol Otol. 1991;105(07):568–70.
Lowitt MH, et al. Cutaneous malacoplakia: a report of two cases and review of the literature. J Am Acad Dermatol. 1996;34(2):325–32.
Kumar PV, Tabei SZ. Cutaneous malakoplakia diagnosed by scraping cytology. Acta Cytol. 1988;32:125–7.
Font Ramon L, Bersani Thomas A, Eagle Ralph C. Malakoplakia of the eyelid: clinical, histopathologic, and ultrastructural characteristics. Ophthalmology. 1988;95(1):61–8.
Addison DJ. Malakoplakia of the eyelid. Ophthalmology. 1986;93(8):1064–7.
Chaudhry AP, Satchidanand SK, Anthone R, Baumler RA, Gaeta JF. An unusual case of supraclavicular and colonic malakoplakia—a light and ultrastructural study. J Pathol. 1980;131(3):193–208.
Afonso JPJM, Ando PN, Padilha MHVDQ, Michalany NS, Porro AM. Cutaneous malakoplakia: case report and review. Anais brasileiros de dermatologia. 2013;88(3):432–7.
Kohl Shane K, Hans Christine P. Cutaneous malakoplakia. Arch Pathol Lab Med. 2008;132(1):113.
Remond B, Dompmartin A, Moreau A, Esnault P, Thomas A, Mandard JC, Leroy D. Cutaneous malacoplakia. Int J Dermatol. 1994;33(8):538–42.
McClure John. Malakoplakia. J Pathol. 1983;140(4):275–330.
Michaelis L, Gutmann C. ÜberEinschlüsse in blasentumoren. Z Klin Med. 1902;47:208–15.
Stanton MJ, Maxted W. Malacoplakia: a study of the literature and current concepts of pathogenesis, diagnosis and treatment. J urolo. 1981;125(2):139.
Lou TY, Teplitz C. Malakoplakia: pathogenesis and ultrastructural morphogenesis: a problem of altered macrophage (phagolysosomal) response. Hum Pathol. 1974;5:191–207.
Abdou NI, NaPombejara C, Sagawa A, Ragland C, Stechschulte DJ, Nilsson U, Sooley B. Malakoplakia: evidence for monocyte lysosomal abnormality correctable by cholinergic agonist in vitro and in vivo. N Engl J Med. 1977;297(26):1413–9.
van der Voort PH, ten Velden JJ, Wassenaar RP, Silberbusch J. Malacoplakia: two case reports and a comparison of treatment modalities based on a literature review. Arch Intern Med. 1996;156(5):577–83.
Acknowledgments
Mr. Martin Heaton, Consultant Plastic Surgeon at the Norfolk and Norwich University Hospital UK, for all his help with this patient’s surgical reconstructive work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None.
Rights and permissions
About this article
Cite this article
Coates, M., Del Pero, M.M. & Nassif, R. A Case of Cutaneous Malakoplakia in the Head and Neck Region and Review of the Literature. Head and Neck Pathol 10, 444–450 (2016). https://doi.org/10.1007/s12105-016-0721-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12105-016-0721-x