Abstract
Background and Purpose
Prophylactic anticonvulsants are routinely prescribed in the acute setting for intracerebral hemorrhage (ICH) patients, but some studies have reported an association with worse outcomes. We sought to characterize the prevalence and predictors of prophylactic anticonvulsant administration after ICH as well as guideline adherence. We also sought to determine whether prophylactic anticonvulsants were independently associated with poor outcome.
Methods
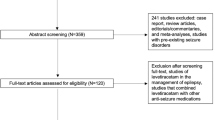
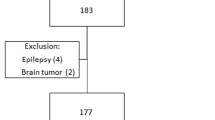
We performed a retrospective study of primary ICH in our two academic centers. We used a propensity matching approach to make treated and non-treated groups comparable. We conducted multiple logistic regression analysis to identify independent predictors of prophylactic anticonvulsant initiation and its association with poor outcome as measured by modified Rankin score.
Results
We identified 610 patients with primary ICH, of whom 98 were started on prophylactic anticonvulsants. Levetiracetam (97%) was most commonly prescribed. Age (OR 0.97, 95% CI 0.95–0.99, p < .001), lobar location (OR 2.94, 95% CI 1.76–4.91, p < .001), higher initial National Institutes of Health Stroke Scale (NIHSS) score (OR 2.31, 95% CI 1.40–3.79, p = .001), craniotomy (OR 3.06, 95% CI 1.51–6.20, p = .002), and prior ICH (OR 2.36, 95% CI 1.10–5.07, p = .028) were independently associated with prophylactic anticonvulsant initiation. Prophylactic anticonvulsant use was not associated with worse functional outcome [modified Rankin score (mRS) 4–6] at hospital discharge or with increased case-fatality. There was no difference in prescribing patterns after 2010 guideline publication.
Discussion
Levetiracetam was routinely prescribed following ICH and was not associated with worse outcomes. Future investigations should examine the effect of prophylactic levetiracetam on cost and neuropsychological outcomes as well as the role of continuous EEG in identifying subclinical seizures.
Similar content being viewed by others
References
van Asch CJ, Luitse MJ, Rinkel GJ, van der Tweel I, Algra A, Klijn CJ. Incidence, case fatality, and functional outcome of intracerebral haemorrhage over time, according to age, sex, and ethnic origin: a systematic review and meta-analysis. Lancet Neurol. 2010;9:167–76.
Szaflarski JP, Rackley AY, Kleindorfer DO, Khoury J, Woo D, Miller R, et al. Incidence of seizures in the acute phase of stroke: a population-based study. Epilepsia. 2008;49:974–81.
Messé SR, Sansing LH, Cucchiara BL, Herman ST, Lyden PD, Kasner SE, et al. Prophylactic antiepileptic drug use is associated with poor outcome following ich. Neurocrit Care. 2009;11:38–44.
Morgenstern LB, Hemphill JC, Anderson C, Becker K, Broderick JP, Connolly ES, et al. Guidelines for the management of spontaneous intracerebral hemorrhage. Stroke. 2010;41:2108–29.
Hemphill JC, Greenberg SM, Anderson CS, Becker K, Bendok BR, Cushman M, et al. Guidelines for the management of spontaneous intracerebral hemorrhage: a guideline for healthcare professionals from the american heart association/american stroke association. Stroke. 2015.
Naidech AM, Garg RK, Liebling S, Levasseur K, Macken MP, Schuele SU, et al. Anticonvulsant use and outcomes after intracerebral hemorrhage. Stroke. 2009;40:3810–5.
Battey TW, Falcone GJ, Ayres AM, Schwab K, Viswanathan A, McNamara KA, et al. Confounding by indication in retrospective studies of intracerebral hemorrhage: Antiepileptic treatment and mortality. Neurocrit Care. 2012;17:361–6.
Sheth KN, Martini SR, Moomaw CJ, Koch S, Elkind MS, Sung G, et al. Prophylactic antiepileptic drug use and outcome in the ethnic/racial variations of intracerebral hemorrhage study. Stroke. 2015:3532–3535.
Gilmore EJ, Maciel CB, Hirsch LJ, Sheth KN. Review of the utility of prophylactic anticonvulsant use in critically ill patients with intracerebral hemorrhage. Stroke. 2016;47:2666–72.
McDonald CJ, Overhage JM, Barnes M, Schadow G, Blevins L, Dexter PR, et al. The indiana network for patient care: a working local health information infrastructure. Health Aff. 2005;24:1214–20.
Alwell K, Khoury J, Moomaw C, Kleindorfer D, Woo D, Flaherty M, et al. Icd-9 codes positive predictive value for stroke subtypes in a population-based epidemiology study. Stroke. 2009;40:e183.
Williams LS, Yilmaz EY, Lopez-Yunez AM. Retrospective assessment of initial stroke severity with the NIH stroke scale. Stroke. 2000;31:858–62.
Kothari RU, Brott T, Broderick JP, Barsan WG, Sauerbeck LR, Zuccarello M, et al. The abcs of measuring intracerebral hemorrhage volumes. Stroke. 1996;27:1304–5.
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (redcap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42:377–81.
Rosenbaum PR, Rubin DB. Constructing a control group using multivariate matched sampling methods that incorporate the propensity score. Am Stat. 1985;39:33–8.
Reddig RT, Nixdorf KE, Jensen MB. The prophylactic use of an antiepileptic drug in intracerebral hemorrhage. Clin Neurol Neurosurg. 2011;113:895–7.
Naidech AM, Beaumont J, Jahromi B, Prabhakaran S, Kho A, Holl JL. Evolving use of seizure medications after intracerebral hemorrhage: a multicenter study. Neurology. 2017;88:52–6.
Taylor S, Heinrichs RJ, Janzen JM, Ehtisham A. Levetiracetam is associated with improved cognitive outcome for patients with intracranial hemorrhage. Neurocrit Care. 2011;15:80–4.
Szaflarski JP, Sangha KS, Lindsell CJ, Shutter LA. Prospective, randomized, single-blinded comparative trial of intravenous levetiracetam versus phenytoin for seizure prophylaxis. Neurocrit Care. 2010;12:165–72.
Brophy GM, Human T, Shutter L. Emergency neurological life support: Pharmacotherapy. Neurocrit Care. 2015;23(Suppl 2):S48–68.
Funding
This work was supported by awards from the IU Health Values Fund (IUH VFR365), the IU CTSI PDT (ICTSI NIH/NCRR RR025761), the IUH/IUSM Strategic Research Initiative, and an IU CTSI KL2 award (NIH, UL1TR001108, Shekhar PI).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Mackey is funded by Research Grant; Significant; IUH-VFR-365, IUH/IUSM Strategic Research Initiative, and CTSI PDT; NIH LRP recipient; Indiana University CTSI KL2 award recipient. A.D. Blatsioris, E.A.S. Moser, R.J.L. Carter, C. Saha, A. Stevenson, and A.L. Hulin are funded by Research Grant; Significant; IUH-VFR-365, IUH/IUSM Strategic Research Initiative. Drs. O’Neill, Cohen-Gadol, Leipzig, and Williams report no disclosures.
Rights and permissions
About this article
Cite this article
Mackey, J., Blatsioris, A.D., Moser, E.A.S. et al. Prophylactic Anticonvulsants in Intracerebral Hemorrhage. Neurocrit Care 27, 220–228 (2017). https://doi.org/10.1007/s12028-017-0385-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-017-0385-8