Abstract
Background
To determine the prevalence, type, and significance of brain damage in critically ill patients with a primary non-neurological diagnosis developing acute brain dysfunction.
Methods
This retrospective cohort study was performed at the Johns Hopkins University School of Medicine, an academic tertiary care hospital. Medical records were reviewed of 479 consecutive ICU patients who underwent brain magnetic resonance imaging (MRI) over a 2-year period. Patients were selected for analysis if MRI was obtained to evaluate an acute onset of brain dysfunction (altered mental status, seizures, and/or focal neurological deficit). Subjects with a history of a central nervous system disorder were excluded. The principal clinical endpoint was Glasgow Outcome Scale (GOS) assessed at discharge. MRI-defined brain abnormalities were classified according to type and location. Factors associated with MRI-defined abnormalities were assessed in uni- and multivariable models.
Results
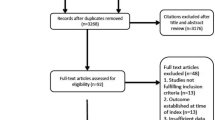
146 patients met inclusion criteria (mean age 54 ± 7 years). Brain damage was detected in 130 patients (89 %). The most prevalent lesions were white matter hyperintensities (104/146, 71 %) and acute cerebral infarcts (59/146, 40 %). In a multivariable model, lesions on brain MRI were independently associated with unfavorable outcome (GOS1-3 in 71 % of patients with lesions vs. 44 % in those without, p = 0.007). No adverse events occurred in relation to transport and MRI scanning.
Conclusions
In critically ill patients without known neurological disease who have acute brain dysfunction, MRI reveals an unexpectedly high burden of underlying brain damage, which is associated with unfavorable outcome. The results indicate that brain damage could be an important and under-recognized factor contributing to critical illness brain dysfunction.


Similar content being viewed by others
References
Teres D, Brown RB, Lemeshow S. Predicting mortality of intensive care unit patients. The importance of coma. Crit Care Med. 1982;10:86–95.
Ely EW, Shintani A, Truman B, Speroff T, Gordon SM, Harrell FE Jr, et al. Delirium as a predictor of mortality in mechanically ventilated patients in the intensive care unit. JAMA. 2004;291:1753–62.
Girard TD, Jackson JC, Pandharipande PP, Pun BT, Thompson JL, Shintani AK, et al. Delirium as a predictor of long-term cognitive impairment in survivors of critical illness. Crit Care Med. 2010;38:1513–20.
Iwashyna TJ, Ely EW, Smith DM, Langa KM. Long-term cognitive impairment and functional disability among survivors of severe sepsis. J Am Med Assoc. 2010;304:1787–94.
Hopkins RO, Weaver LK, Collingridge D, Parkinson RB, Chan KJ, Orme JF Jr. Two-year cognitive, emotional, and quality-of-life outcomes in acute respiratory distress syndrome. Am J Respir Crit Care Med. 2005;171:340–7.
Gofton TE, Young GB. Sepsis-associated encephalopathy. Nat Rev Neurol. 2012;8:557–66.
Sharshar T, Annane D, de la Grandmaison GL, Brouland JP, Hopkinson NS, Francoise G. The neuropathology of septic shock. Brain Pathol. 2004;14:21–33.
Wijman CA, Mlynash M, Caulfield AF, Hsia AW, Eyngorn I, Bammer R, et al. Prognostic value of brain diffusion-weighted imaging after cardiac arrest. Ann Neurol. 2009;65:394–402.
Wu O, Sorensen AG, Benner T, Singhal AB, Furie KL, Greer DM. Comatose patients with cardiac arrest: predicting clinical outcome with diffusion-weighted MR imaging. Radiology. 2009;252:173–81.
Sharshar T, Carlier R, Bernard F, Guidoux C, Brouland JP, Nardi O, et al. Brain lesions in septic shock: a magnetic resonance imaging study. Intensiv Care Med. 2007;33:798–806.
Dsm-Iv American Psychiatric Association. Task force. Diagnostic and statistical manual of mental disorders: DSM-IV-TR: American Psychiatric Publication; 2000.
Posner JB, Saper CB, Schiff ND, Plum F. Examination of the comatose patient. In: Plum and Posner’s diagnosis of stupor and coma. 4 ed. Oxford: Oxford University Press; 2007:38–7.
Fisher RS, van Emde BW, Blume W, Elger C, Genton P, Lee P, et al. Epileptic seizures and epilepsy: definitions proposed by the International League against Epilepsy (ILAE) and the International Bureau for Epilepsy (IBE). Epilepsia. 2005;46:470–2.
The Acute Respiratory Distress Syndrome Network. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. 2000;342:1301–8.
Bernard GR, Artigas A, Brigham KL, Carlet J, Falke K, Hudson L, et al. Report of the American-European consensus conference on ARDS: definitions, mechanisms, relevant outcomes and clinical trial coordination. The Consensus Committee. Intensiv Care Med. 1994;20:225–32.
Levy MM, Fink MP, Marshall JC, Abraham E, Angus D, Cook D, et al. 2001 SCCM/ESICM/ACCP/ATS/SIS International Sepsis Definitions Conference. Intensiv Care Med. 2003;29:530–8.
Levy MM, Fink MP, Marshall JC, Abraham E, Angus D, Cook D, et al. 2001 SCCM/ESICM/ACCP/ATS/SIS International Sepsis Definitions Conference. Crit Care Med. 2003;31:1250–6.
Sener RN. Diffusion MRI: apparent diffusion coefficient (ADC) values in the normal brain and a classification of brain disorders based on ADC values. Comput Med Imaging Graph. 2001;25:299–326.
Hinchey J, Chaves C, Appignani B, Breen J, Pao L, Wang A, et al. A reversible posterior leukoencephalopathy syndrome. N Engl J Med. 1996;334:494–500.
Schmidt R, Fazekas F, Kleinert G, Offenbacher H, Gindl K, Payer F, et al. Magnetic resonance imaging signal hyperintensities in the deep and subcortical white matter. A comparative study between stroke patients and normal volunteers. Arch Neurol. 1992;49:825–7.
Bartynski WS, Boardman JF, Zeigler ZR, Shadduck RK, Lister J. Posterior reversible encephalopathy syndrome in infection, sepsis, and shock. AJNR Am J Neuroradiol. 2006;27:2179–90.
Piazza O, Cotena S, De Robertis E, Caranci F, Tufano R. Sepsis associated encephalopathy studied by MRI and cerebral spinal fluid S100B measurement. Neurochem Res. 2009;34:1289–92.
Finelli PF, Uphoff DF. Magnetic resonance imaging abnormalities with septic encephalopathy. J Neurol Neurosurg Psychiatry. 2004;75:1189–91.
Hollinger P, Zurcher R, Schroth G, Mattle HP. Diffusion magnetic resonance imaging findings in cerebritis and brain abscesses in a patient with septic encephalopathy. J Neurol. 2000;247:232–4.
Morandi A, Rogers BP, Gunther ML, Merkle K, Pandharipande P, Girard TD, et al. The relationship between delirium duration, white matter integrity, and cognitive impairment in intensive care unit survivors as determined by diffusion tensor imaging: the VISIONS prospective cohort magnetic resonance imaging study*. Crit Care Med. 2012;40:2182–9.
Witlox J, Eurelings LSM, de Jonghe JFM, Kalisvaart KJ, Eikelenboom P, van Gool WA. Delirium in elderly patients and the risk of postdischarge mortality, institutionalization, and dementia: a meta-analysis. J Am Med Assoc. 2010;304:443–51.
Hachinski VC, Potter P, Merskey H. Leuko-araiosis. Arch Neurol. 1987;44:21–3.
Awad IA, Johnson PC, Spetzler RF, Hodak JA. Incidental subcortical lesions identified on magnetic resonance imaging in the elderly II. Postmortem pathological correlations. Stroke. 1986;17:1090–7.
Awad IA, Spetzler RF, Hodak JA, Awad CA, Carey R. Incidental subcortical lesions identified on magnetic resonance imaging in the elderly. I. Correlation with age and cerebrovascular risk factors. Stroke. 1986;17:1084–9.
Fernando MS, O’Brien JT, Perry RH, English P, Forster G, McMeekin W, et al. Comparison of the pathology of cerebral white matter with post-mortem magnetic resonance imaging (MRI) in the elderly brain. Neuropathol Appl Neurobiol. 2004;30:385–95.
Debette S, Markus HS. The clinical importance of white matter hyperintensities on brain magnetic resonance imaging: systematic review and meta-analysis. BMJ. 2010;341:c3666.
Young VG, Halliday GM, Kril JJ. Neuropathologic correlates of white matter hyperintensities. Neurology. 2008;71:804–11.
Pantoni L, Garcia JH. Pathogenesis of leukoaraiosis: a review. Stroke. 1997;28:652–9.
Murray AD, Staff RT, McNeil CJ, Salarirad S, Ahearn TS, Mustafa N, et al. The balance between cognitive reserve and brain imaging biomarkers of cerebrovascular and Alzheimer’s diseases. Brain. 2011;134:3687–96.
Wijdicks EF, Scott JP. Stroke in the medical intensive-care unit. Mayo Clin Proc. 1998;73:642–6.
Walkey AJ, Wiener RS, Ghobrial JM, Curtis LH, Benjamin EJ. Incident stroke and mortality associated with new-onset atrial fibrillation in patients hospitalized with severe sepsis. JAMA. 2011;306:2248–54.
Beckmann U, Gillies DM, Berenholtz SM, Wu AW, Pronovost P. Incidents relating to the intra-hospital transfer of critically ill patients. An analysis of the reports submitted to the Australian Incident Monitoring Study in Intensive Care. Intensiv Care Med. 2004;30:1579–85.
Acknowledgement
We would like to acknowledge Dr. Lucas Restrepo from the Department of Neurology, University of California, Los Angeles for his careful review and insightful comments on this manuscript. We confirm that all persons, who contributed significantly to the study, are listed as authors. Raoul Sutter is supported by the Research Fund of the University Basel, the Scientific Society Basel, and the Gottfried Julia Bangerter-Rhyner Foundation.
Conflict of interest
Dr. Robert D Stevens, Dr. Julio A Chalela, Dr. Richard Leigh, Dr. Tamer Abdelhak, Dr. Peter W Kaplan, Dr. Gayane Yenokyan, and Dr. Tarek Sharshar have no disclosures.
Ethical Standard
This study was approved by the institutional review board (Johns Hopkins Medicine Institutional Review Board).
Funding
There was no funding received for this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sutter, R., Chalela, J.A., Leigh, R. et al. Significance of Parenchymal Brain Damage in Patients with Critical Illness. Neurocrit Care 23, 243–252 (2015). https://doi.org/10.1007/s12028-015-0110-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-015-0110-4