Abstract
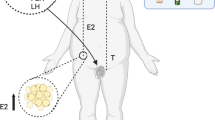
Maternal obesity during pregnancy has been related with several pathological states in offspring. However, the impact of maternal obesity on reproductive system on the progeny is beginning to be elucidated. In this work, we characterize the effect of maternal obesity on puberty onset and follicular development in adult offspring in rats. We also propose that alterations in ovarian physiology observed in offspring of obese mothers are due to increased levels of estradiol during early development. Offspring of control dams and offspring of dams exposed to a high-fat diet (HF) were studied at postnatal days (PND) 1, 7, 14, 30, 60, and 120. Body weight and onset of puberty were measured. Counting of ovarian follicles was performed at PND 60 and 120. Serum estradiol, estriol, androstenedione, FSH, LH, and insulin levels were measured by ELISA. Hepatic CYP3A2 expression was determined by Western blot. HF rats had a higher weight than controls at all ages and they also had a precocious puberty. Estradiol levels were increased while CYP3A2 expression was reduced from PND 1 until PND 60 in HF rats compared to controls. Estriol was decreased at PND60 in HF rats. Ovaries from HF rats had a decrease in antral follicles at PND60 and PND120 and an increase in follicular cysts at PND60 and PND120. In this work, we demonstrated that maternal obesity in rats alters follicular development and induces follicular cysts generation in the adult offspring. We observed that maternal obesity produces an endocrine disruption through increasing endogenous estradiol in early life. A programmed failure in hepatic metabolism of estradiol is probably the cause of its increase.







Similar content being viewed by others
References
E.S. Jungheim, J.L. Travieso, K.R. Carson, K.H. Moley, Obesity and reproductive function. Obstet. Gynecol. Clin. North Am. 39(4), 479–493 (2012). doi:10.1016/j.ogc.2012.09.002
C.J. Lavie, P.A. McAuley, T.S. Church, R.V. Milani, S.N. Blair, Obesity and cardiovascular diseases: implications regarding fitness, fatness, and severity in the obesity paradox. J. Am. Coll. Cardiol. 63(14), 1345–1354 (2014). doi:10.1016/j.jacc.2014.01.022
K. Ghoshal, M. Bhattacharyya, Adiponectin: probe of the molecular paradigm associating diabetes and obesity. World J Diabetes 6(1), 151–166 (2015). doi:10.4239/wjd.v6.i1.151
C.P. Rodrigo, Current mapping of obesity. Nutr. Hosp. 28(Suppl 5), 21–31 (2013). doi:10.3305/nh.2013.28.sup5.6915
V.H. Roberts, A.E. Frias, K.L. Grove, Impact of maternal obesity on fetal programming of cardiovascular disease. Physiology 30(3), 224–231 (2015). doi:10.1152/physiol.00021.2014
O. Paliy, C.J. Piyathilake, A. Kozyrskyj, G. Celep, F. Marotta, R. Rastmanesh, Excess body weight during pregnancy and offspring obesity: potential mechanisms. Nutrition 30(3), 245–251 (2014). doi:10.1016/j.nut.2013.05.011
C.E. McCurdy, J.M. Bishop, S.M. Williams, B.E. Grayson, M.S. Smith, J.E. Friedman, K.L. Grove, Maternal high-fat diet triggers lipotoxicity in the fetal livers of nonhuman primates. J. Clin. Investig. 119(2), 323–335 (2009). doi:10.1172/JCI32661
A. Mouralidarane, J. Soeda, C. Visconti-Pugmire, A.M. Samuelsson, J. Pombo, X. Maragkoudaki, A. Butt, R. Saraswati, M. Novelli, G. Fusai, L. Poston, P.D. Taylor, J.A. Oben, Maternal obesity programs offspring nonalcoholic fatty liver disease by innate immune dysfunction in mice. Hepatology 58(1), 128–138 (2013). doi:10.1002/hep.26248
T.J. Pereira, M.A. Fonseca, K.E. Campbell, B.L. Moyce, L.K. Cole, G.M. Hatch, C.A. Doucette, J. Klein, M. Aliani, V.W. Dolinsky, Maternal obesity characterized by gestational diabetes increases the susceptibility of rat offspring to hepatic steatosis via a disrupted liver metabolome. J Physiol (2015). doi:10.1113/JP270429
P. Catalano, S.H. deMouzon, Maternal obesity and metabolic risk to the offspring: why lifestyle interventions may have not achieved the desired outcomes. Int J Obes 39(4), 642–649 (2015). doi:10.1038/ijo.2015.15
P.D. Taylor, A.M. Samuelsson, L. Poston, Maternal obesity and the developmental programming of hypertension: a role for leptin. Acta Physiol. 210(3), 508–523 (2014). doi:10.1111/apha.12223
Y. Cheong, K.H. Sadek, K.D. Bruce, N. Macklon, F.R. Cagampang, Diet-induced maternal obesity alters ovarian morphology and gene expression in the adult mouse offspring. Fertil. Steril. 102(3), 899–907 (2014). doi:10.1016/j.fertnstert.2014.06.015
K.L. Connor, M.H. Vickers, J. Beltrand, M.J. Meaney, D.M. Sloboda, Nature, nurture or nutrition? Impact of maternal nutrition on maternal care, offspring development and reproductive function. J Physiol 590(Pt 9), 2167–2180 (2012). doi:10.1113/jphysiol.2011.223305
D.M. Sloboda, G.J. Howie, A. Pleasants, P.D. Gluckman, M.H. Vickers, Pre- and postnatal nutritional histories influence reproductive maturation and ovarian function in the rat. PLoS One 4(8), e6744 (2009). doi:10.1371/journal.pone.0006744
S.A. Keim, A.M. Branum, M.A. Klebanoff, B.S. Zemel, Maternal body mass index and daughters’ age at menarche. Epidemiology 20(5), 677–681 (2009). doi:10.1097/EDE.0b013e3181b093ce
G.C. Windham, L. Zhang, M.P. Longnecker, M. Klebanoff, Maternal smoking, demographic and lifestyle factors in relation to daughter’s age at menarche. Paediatr. Perinat. Epidemiol. 22(6), 551–561 (2008). doi:10.1111/j.1365-3016.2008.00948.x
L. Hilakivi-Clarke, R. Clarke, I. Onojafe, M. Raygada, E. Cho, M. Lippman, A maternal diet high in n-6 polyunsaturated fats alters mammary gland development, puberty onset, and breast cancer risk among female rat offspring. Proc. Natl. Acad. Sci. USA 94(17), 9372–9377 (1997)
G. Cruz, R. Barra, D. Gonzalez, R. Sotomayor-Zarate, H.E. Lara, Temporal window in which exposure to estradiol permanently modifies ovarian function causing polycystic ovary morphology in rats. Fertil. Steril. 98(5), 1283–1290 (2012). doi:10.1016/j.fertnstert.2012.07.1060
W.H. Nah, M.J. Park, M.C. Gye, Effects of early prepubertal exposure to bisphenol A on the onset of puberty, ovarian weights, and estrous cycle in female mice. Clin Exp Reprod Med 38(2), 75–81 (2011). doi:10.5653/cerm.2011.38.2.75
Y. Li, W. Zhang, J. Liu, W. Wang, H. Li, J. Zhu, S. Weng, S. Xiao, T. Wu, Prepubertal bisphenol A exposure interferes with ovarian follicle development and its relevant gene expression. Reprod. Toxicol. 44, 33–40 (2014). doi:10.1016/j.reprotox.2013.09.002
R. Sotomayor-Zarate, M. Tiszavari, G. Cruz, H.E. Lara, Neonatal exposure to single doses of estradiol or testosterone programs ovarian follicular development-modified hypothalamic neurotransmitters and causes polycystic ovary during adulthood in the rat. Fertil. Steril. 96(6), 1490–1496 (2011). doi:10.1016/j.fertnstert.2011.09.011
S. de Assis, A. Warri, M.I. Cruz, O. Laja, Y. Tian, B. Zhang, Y. Wang, T.H. Huang, L. Hilakivi-Clarke, High-fat or ethinyl-oestradiol intake during pregnancy increases mammary cancer risk in several generations of offspring. Nat Commun 3, 1053 (2012). doi:10.1038/ncomms2058
J. Wojcikowski, A. Haduch, W.A. Daniel, Effect of classic and atypical neuroleptics on cytochrome P450 3A (CYP3A) in rat liver. Pharmacol Rep: PR 64(6), 1411–1418 (2012)
H. Yamazaki, P.M. Shaw, F.P. Guengerich, T. Shimada, Roles of cytochromes P450 1A2 and 3A4 in the oxidation of estradiol and estrone in human liver microsomes. Chem. Res. Toxicol. 11(6), 659–665 (1998). doi:10.1021/tx970217f
M. Tajima, N. Ikarashi, Y. Imahori, T. Okaniwa, K. Saruta, M. Ishii, Y. Kusunoki, R. Kon, T. Toda, W. Ochiai, H. Yamada, K. Sugiyama, Consumption of a high-fat diet during pregnancy decreases the activity of cytochrome P450 3a in the livers of offspring. Eur J Pharm Sci 47(1), 108–116 (2012). doi:10.1016/j.ejps.2012.05.008
L.L. Moltke, D.J. Greenblatt, J. Schmider, J.S. Harmatz, R.I. Shader, Metabolism of drugs by cytochrome P450 3A isoforms implications for drug interactions in psychopharmacology. Clin Pharmacokinet 29(Suppl 1), 33–43 (1995). (discussion 43–34)
G.M. Centola, Surface features of exfoliated vaginal epithelial cells during the oestrous cycle of the rat examined by scanning electron microscopy. J. Anat. 127(Pt 3), 553–561 (1978)
A. Barria, V. Leyton, S.R. Ojeda, H.E. Lara, Ovarian steroidal response to gonadotropins and beta-adrenergic stimulation is enhanced in polycystic ovary syndrome: role of sympathetic innervation. Endocrinology 133(6), 2696–2703 (1993). doi:10.1210/endo.133.6.8243293
E.G. Bligh, W.J. Dyer, A rapid method of total lipid extraction and purification. Can J Biochem Physiol 37(8), 911–917 (1959)
V.D. Ramirez, C.H. Sawyer, Advancement of puberty in the female rat by estrogen. Endocrinology 76, 1158–1168 (1965). doi:10.1210/endo-76-6-1158
V. Matagne, G. Rasier, M.C. Lebrethon, A. Gerard, J.P. Bourguignon, Estradiol stimulation of pulsatile gonadotropin-releasing hormone secretion in vitro: correlation with perinatal exposure to sex steroids and induction of sexual precocity in vivo. Endocrinology 145(6), 2775–2783 (2004). doi:10.1210/en.2003-1259
S.M. Losa-Ward, K.L. Todd, K.A. McCaffrey, K. Tsutsui, H.B. Patisaul, Disrupted organization of RFamide pathways in the hypothalamus is associated with advanced puberty in female rats neonatally exposed to bisphenol A. Biol. Reprod. 87(2), 28 (2012). doi:10.1095/biolreprod.112.100826
T. Yum, S. Lee, Y. Kim, Association between precocious puberty and some endocrine disruptors in human plasma. J Environ Sci Health Part A, Toxic/Hazard Subst Environ Eng 48(8), 912–917 (2013). doi:10.1080/10934529.2013.762734
T.J. Key, N.E. Allen, E.A. Spencer, R.C. Travis, Nutrition and breast cancer. Breast 12(6), 412–416 (2003)
R.C. Travis, T.J. Key, Oestrogen exposure and breast cancer risk. Breast Cancer Res: BCR 5(5), 239–247 (2003). doi:10.1186/bcr628
G. Cruz, W. Foster, A. Paredes, K.D. Yi, M. Uzumcu, Long-term effects of early-life exposure to environmental oestrogens on ovarian function: role of epigenetics. J. Neuroendocrinol. 26(9), 613–624 (2014). doi:10.1111/jne.12181
C.D. Fisher, A.J. Lickteig, L.M. Augustine, J. Ranger-Moore, J.P. Jackson, S.S. Ferguson, N.J. Cherrington, Hepatic cytochrome P450 enzyme alterations in humans with progressive stages of nonalcoholic fatty liver disease. Drug Metab Dispos Biol Fate Chem 37(10), 2087–2094 (2009). doi:10.1124/dmd.109.027466
D. Kolwankar, R. Vuppalanchi, B. Ethell, D.R. Jones, S.A. Wrighton, S.D. Hall, N. Chalasani, Association between nonalcoholic hepatic steatosis and hepatic cytochrome P-450 3A activity. Clin Gastroenterol Hepatol 5(3), 388–393 (2007). doi:10.1016/j.cgh.2006.12.021
S.J. Woolsey, S.E. Mansell, R.B. Kim, R.G. Tirona, M.D. Beaton, CYP3A activity and expression in nonalcoholic fatty liver disease. Drug Metab Dispos 43(10), 1484–1490 (2015). doi:10.1124/dmd.115.065979
S.A. Bayol, B.H. Simbi, R.C. Fowkes, N.C. Stickland, A maternal “junk food” diet in pregnancy and lactation promotes nonalcoholic Fatty liver disease in rat offspring. Endocrinology 151(4), 1451–1461 (2010). doi:10.1210/en.2009-1192
M. Mukai, K. Ozasa, K. Hayashi, K. Kawai, Various S-GOT/S-GPT ratios in nonviral liver disorders and related physical conditions and life-style. Dig. Dis. Sci. 47(3), 549–555 (2002)
Z. Abdel-Razzak, P. Loyer, A. Fautrel, J.C. Gautier, L. Corcos, B. Turlin, P. Beaune, A. Guillouzo, Cytokines down-regulate expression of major cytochrome P-450 enzymes in adult human hepatocytes in primary culture. Mol. Pharmacol. 44(4), 707–715 (1993)
T. Zhou, S. Cong, S. Sun, H. Sun, R. Zou, S. Wang, C. Wang, J. Jiao, K. Goto, H. Nawata, T. Yanase, Y. Zhao, Identification of endocrine disrupting chemicals activating SXR-mediated transactivation of CYP3A and CYP7A1. Mol. Cell. Endocrinol. 365(1), 36–43 (2013). doi:10.1016/j.mce.2012.09.001
S.Y. Choi, K.H. Koh, H. Jeong, Isoform-specific regulation of cytochromes P450 expression by estradiol and progesterone. Drug metabolism and disposition: the biological fate of chemicals 41(2), 263–269 (2013). doi:10.1124/dmd.112.046276
R. Sotomayor-Zarate, M. Dorfman, A. Paredes, H.E. Lara, Neonatal exposure to estradiol valerate programs ovarian sympathetic innervation and follicular development in the adult rat. Biol. Reprod. 78(4), 673–680 (2008). doi:10.1095/biolreprod.107.063974
G. Cruz, R. Riquelme, P. Espinosa, P. Jara, A. Dagnino-Subiabre, G.M. Renard, R. Sotomayor-Zarate, Neonatal exposure to estradiol valerate increases dopamine content in nigrostriatal pathway during adulthood in the rat. Horm Metab Res 46(5), 322–327 (2014). doi:10.1055/s-0033-1361159
M.K. Moon, I.K. Jeong, T.J. Oh, H.Y. Ahn, H.H. Kim, Y.J. Park, H.C. Jang, K.S. Park, Long-term oral exposure to bisphenol A induces glucose intolerance and insulin resistance. J Endocrinol (2015). doi:10.1530/JOE-14-0714
C. Alexanderson, E. Eriksson, E. Stener-Victorin, M. Lonn, A. Holmang, Early postnatal oestradiol exposure causes insulin resistance and signs of inflammation in circulation and skeletal muscle. J Endocrinol 201(1), 49–58 (2009). doi:10.1677/JOE-08-0534
A.M. Zama, M. Uzumcu, Targeted genome-wide methylation and gene expression analyses reveal signaling pathways involved in ovarian dysfunction after developmental EDC exposure in rats. Biol. Reprod. 88(2), 52 (2013). doi:10.1095/biolreprod.112.104802
A.E. Armenti, A.M. Zama, L. Passantino, M. Uzumcu, Developmental methoxychlor exposure affects multiple reproductive parameters and ovarian folliculogenesis and gene expression in adult rats. Toxicol. Appl. Pharmacol. 233(2), 286–296 (2008). doi:10.1016/j.taap.2008.09.010
D.H. Abbott, D.A. Dumesic, S. Franks, Developmental origin of polycystic ovary syndrome—a hypothesis. J Endocrinol 174(1), 1–5 (2002)
V. Padmanabhan, A. Veiga-Lopez, Developmental origin of reproductive and metabolic dysfunctions: androgenic versus estrogenic reprogramming. Sem Reprod Med 29(3), 173–186 (2011). doi:10.1055/s-0031-1275519
H. Li, Y. Chen, L.Y. Yan, J. Qiao, Increased expression of P450scc and CYP17 in development of endogenous hyperandrogenism in a rat model of PCOS. Endocrine 43(1), 184–190 (2013). doi:10.1007/s12020-012-9739-3
A.D. Genazzani, F. Ricchieri, C. Lanzoni, Use of metformin in the treatment of polycystic ovary syndrome. Women’s Health 6(4), 577–593 (2010). doi:10.2217/whe.10.43
N.P. Johnson, Metformin use in women with polycystic ovary syndrome. Ann Transl Med 2(6), 56 (2014). doi:10.3978/j.issn.2305-5839.2014.04.15
G.L. Rodriguez-Gonzalez, C.C. Vega, L. Boeck, M. Vazquez, C.J. Bautista, L.A. Reyes-Castro, O. Saldana, D. Lovera, P.W. Nathanielsz, E. Zambrano, Maternal obesity and overnutrition increase oxidative stress in male rat offspring reproductive system and decrease fertility. Int J Obes 39(4), 549–556 (2015). doi:10.1038/ijo.2014.209
H.M. Rivera, K.J. Christiansen, E.L. Sullivan, The role of maternal obesity in the risk of neuropsychiatric disorders. Front Neurosci 9, 194 (2015). doi:10.3389/fnins.2015.00194
L. Fan, S.R. Lindsley, S.M. Comstock, D.L. Takahashi, A.E. Evans, G.W. He, K.L. Thornburg, K.L. Grove, Maternal high-fat diet impacts endothelial function in nonhuman primate offspring. Int J Obes 37(2), 254–262 (2013). doi:10.1038/ijo.2012.42
A.M. Samuelsson, A. Morris, N. Igosheva, S.L. Kirk, J.M. Pombo, C.W. Coen, L. Poston, P.D. Taylor, Evidence for sympathetic origins of hypertension in juvenile offspring of obese rats. Hypertension 55(1), 76–82 (2010). doi:10.1161/HYPERTENSIONAHA.109.139402
Acknowledgments
This work was supported by Fondecyt Initiation Grant 11130707-CONICYT. Additional funds were provided by Center for Neurobiology and Cerebral Plasticity (CNPC)—Universidad de Valparaíso. We thank Dr. Gladys Tapia from University of Chile for helping with hepatic studies and Dr. Alfonso Paredes from University of Chile for kindly providing LH and FSH kits. We thank to Ms. Tania Cerda from University of Valparaíso for technical support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Valery Ambrosetti and Marcelo Guerra have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Ambrosetti, V., Guerra, M., Ramírez, L.A. et al. Increase in endogenous estradiol in the progeny of obese rats is associated with precocious puberty and altered follicular development in adulthood. Endocrine 53, 258–270 (2016). https://doi.org/10.1007/s12020-016-0858-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-016-0858-0