Abstract
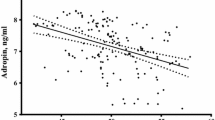
The aims of the study were to evaluate whether adiposity was among the determinants of circulating prolactin levels and to determine whether serum prolactin independently predicted metabolic abnormalities in patients with polycystic ovary syndrome (PCOS). A total of 322 PCOS patients with normal serum prolactin levels were recruited between January 2007 and January 2014. Anthropometric, metabolic, and hormonal parameters were measured in all of the patients. HOMA-IR was calculated as an index of insulin resistance. Serum prolactin was negatively correlated with age (p < 0.0001), all the adiposity indices [body mass index p < 0.0001; waist circumference p < 0.0001; waist-hip ratio (WHR) p < 0.0001], visceral adiposity index (VAI, p = 0.043), fasting insulinemia (p = 0.002), and HOMA-IR (p = 0.002), and was positively correlated with serum adiponectin (p = 0.034), but not with circulating androgens or serum leptin levels. Serum adiponectin, but not HOMA-IR or fasting insulinemia, was independently associated with serum prolactin after adjustment for age, leptin, and anthropometrical adiposity parameters. Of the adiposity parameters, only WHR and VAI were independent predictors of serum prolactin after adjustment for adiponectin. Circulating prolactin was also negatively correlated with fasting glycemia (only in patients with normal glucose metabolism, p = 0.037) and was inversely correlated with the presence of metabolic syndrome (p < 0.001), but this association was not maintained after adjustment for possible confounders. In PCOS patients, serum prolactin level was related to adipose tissue quantity and function, and adiponectin was a possible mediator of this relationship. Low serum prolactin levels were associated with an unfavorable metabolic profile, but this association seemed to be due to the complex interplay among prolactin, adiposity, and insulin resistance rather than to a direct metabolic effect of prolactin.

Similar content being viewed by others
References
L. Balbach, H. Wallaschofski, H. Völzke, M. Nauck, M. Dörr, R. Haring, Serum prolactin concentrations as risk factor of metabolic syndrome or type 2 diabetes? BMC Endocr. Disord. 13, 12 (2013). doi:10.1186/1472-6823-13-12
V. Chirico, S. Cannavò, A. Lacquaniti, V. Salpietro, M. Mandolfino, P.D. Romeo, O. Cotta, C. Munafò, G. Giorgianni, C. Salpietro, T. Arrigo, Prolactin in obese children: a bridge between inflammation and metabolic-endocrine dysfunction. Clin. Endocrinol. (Oxf). 79, 537–544 (2013)
G. Corona, E. Mannucci, E.A. Jannini, F. Lotti, V. Ricca, M. Monami, V. Boddi, E. Bandini, G. Balercia, G. Forti, M. Maggi, Hypoprolactinemia: a new clinical syndrome in patients with sexual dysfunction. J. Sex Med. 6, 1457–1466 (2009)
G. Corona, G. Rastrelli, V. Boddi, M. Monami, C. Melani, D. Balzi, A. Sforza, G. Forti, E. Mannucci, M. Maggi, Prolactin levels independently predict major cardiovascular events in patients with erectile dysfunction. Int. J. Androl. 34, 217–224 (2011)
R. Haring, N. Friedrich, H. Volzke, R.S. Vasan, S.B. Felix, M. Dorr, H. Meyer zu Schwabedissen, M. Nauck, H. EWallaschofski, Positive association of serum prolactin concentrations with all-cause and cardiovascular mortality. Eur. Heart J. 35, 1215–1221 (2012)
M. Freemark, I. Avril, D. Fleenor, P. Driscoll, A. Petro, E. Opara, W. Kendall, J. Oden, S. Bridges, N. Binart, B. Breant, P.A. Kelly, Targeted deletion of the PRL receptor: effects on islet development, insulin production, and glucose tolerance. Endocrinology 143, 1378–1385 (2002)
M.C. Barber, R.A. Clegg, E. Finley, R.G. Vernon, D.J. Flint, The role of growth hormone, prolactin and insulin-like growth factors in the regulation of rat mammary gland and adipose tissue metabolism during lactation. J. Endocrinol. 135, 195–202 (1992)
E.R. Hugo, D.C. Borcherding, K.S. Gersin, J. Loftus, N. Ben-Jonathan, Prolactin release by adipose explants, primary adipocytes, and LS14 adipocytes. J. Clin. Endocrinol. Metab. 93, 4006–4012 (2008)
R.J. Norman, D. Dewailly, R.S. Legro, T.E. Hickey, Polycystic ovary syndrome. Lancet 370, 685–697 (2007)
L.J. Moran, M.L. Misso, R.A. Wild, R.J. Norman, Impaired glucose tolerance, type 2 diabetes and metabolic syndrome in polycystic ovary syndrome: a systematic review and meta-analysis. Hum. Reprod. Update 16, 347–363 (2010)
A. Dunaif, K.R. Segal, W. Futterweit, A. Dobrjansky, Profound peripheral insulin resistance, independent of obesity, in polycystic ovary syndrome. Diabetes 38, 1165–1174 (1989)
H.F. Escobar-Morreale, J.L. San Millán, Abdominal adiposity and the polycystic ovary syndrome. Trends Endocrinol. Metab. 18, 266–272 (2007)
K.A. Toulis, D.G. Goulis, D. Farmakiotis, N.A. Georgopoulos, I. Katsikis, B.C. Tarlatzis, I. Papadimas, D. Panidis, Adiponectin levels in women with polycystic ovary syndrome: a systematic review and a meta-analysis. Hum. Reprod. Update. 15, 297–307 (2009)
Rotterdam ESHRE/ASRM-Sponsored Consensus Workshop Group, Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome (PCOS). Hum. Reprod. 19, 41–47 (2004)
A. Albu, S. Radian, S. Fica, C.G. Barbu, Biochemical hyperandrogenism is associated with metabolic syndrome independently of adiposity and insulin resistance in Romanian polycystic ovary syndrome patients. Endocrine (2014). doi:10.1007/s12020-014-0340-9
W. Kühnel, IMMULITE® and IMMULITE® 2000 Reference Range Compendium. Page 44 [Internet]. http://diagnostics.cwp.co.kr/html/Support/DatDwn.asp?id=1&nm=Reference%20range.PDF
Expert panel on detection evaluation, and treatment of high blood cholesterol in adults, Executive summary of the third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III). JAMA 285, 2486–2497 (2001)
American Diabetes Association: Standards of Care for Diabetes, Brief summary of screening and diagnosis of type 2 diabetes and its complications. Diabetes Care 36, S11–S61 (2013)
M.C. Amato, C. Giordano, Visceral adiposity index: an indicator of adipose tissue dysfunction. Int. J. Endocrinol (2014). doi:10.1155/2014/730827
D.J. Flint, R.A. Clegg, R.G. Vernon, Prolactin and the regulation of adipose-tissue metabolism during lactation in rats. Mol. Cell. Endocrinol. 22, 265–275 (1981)
C.M. Oller do Nascimento, V. Ilic, D.H. Williamson, Re-examination of the putative roles of insulin and prolactin in the regulation of lipid deposition and lipogenesis in vivo in mammary gland and white and brown adipose tissue of lactating rats and litter-removed rats. Biochem. J. 258, 273–278 (1989)
J. Auffret, S. Viengchareun, N. Carré, R.G.P. Denis, C. Magnan, P.Y. Marie, A. Muscat, B. Fève, M. Lombès, N. Binart, Beige differentiation of adipose depots in mice lacking prolactin receptor protects against high-fat-diet-induced obesity. FASEB J. 26, 3728–3737 (2012)
N. Carré, N. Binart, Prolactin and adipose tissue. Biochimie 97, 16–21 (2013)
N. Ben-Jonathan, E.R. Hugo, T.D. Brandebourg, C.R. LaPensee, Focus on prolactin as a metabolic hormone. Trends Endocrinol. Metab. 17, 110–116 (2006)
F. Roelfsema, H. Pijl, D.M. Keenan, J.D. Veldhuis, Prolactin secretion in healthy adults is determined by gender, age and body mass index. PLoS ONE 7, e31305 (2012)
B. Ernst, M. Thurnheer, B. Schultes, Basal serum prolactin levels in obesity–unrelated to parameters of the metabolic syndrome and unchanged after massive weight loss. Obes. Surg. 19, 1159–1162 (2009)
P. Kok, F. Roelfsema, M. Frölich, A.E. Meinders, H. Pijl, Prolactin release is enhanced in proportion to excess visceral fat in obese women. J. Clin. Endocrinol. Metab. 89, 4445–4449 (2004)
J.Y. Oh, Y.A. Sung, H.J. Lee, The visceral adiposity index as a predictor of insulin resistance in young women with polycystic ovary syndrome. Obesity. 21(8), 1690–1694 (2013)
I. Ek, P. Arner, A. Bergqvist, K. Carlström, H. Wahrenberg, Impaired adipocyte lipolysis in nonobese women with the polycystic ovary syndrome: a possible link to insulin resistance? J. Clin. Endocrinol. Metab. 82, 1147–1153 (1997)
L. Mannerås-Holm, H. Leonhardt, J. Kullberg, E. Jennische, A. Odén, G. Holm, M. Hellström, L. Lönn, G. Olivecrona, E. Stener-Victorin, M. Lönn, Adipose tissue has aberrant morphology and function in PCOS: enlarged adipocytes and low serum adiponectin, but not circulating sex steroids, are strongly associated with insulin resistance. J. Clin. Endocrinol. Metab. 96, E304–E311 (2011)
T.P. Combs, U.B. Pajvani, A.H. Berg, Y. Lin, L.A. Jelicks, M. Laplante, A.R. Nawrocki, M.W. Rajala, A.F. Parlow, L. Cheeseboro, Y.Y. Ding, R.G. Russell, D. Lindemann, A. Hartley, G.R. Baker, S. Obici, Y. Deshaies, M. Ludgate, L. Rossetti, P.E. Scherer, A transgenic mouse with a deletion in the collagenous domain of adiponectin displays elevated circulating adiponectin and improved insulin sensitivity. Endocrinology 145, 367–383 (2004)
F. Rodriguez-Pacheco, A.J. Martinez-Fuentes, S. Tovar, L. Pinilla, M. Tena-Sempere, C. Dieguez, J.P. Castaño, M.M. Malagon, Regulation of pituitary cell function by adiponectin. Endocrinology 148, 401–410 (2007)
J.C. Seidell, L. Perusse, J.P. Despres, C. Bouchard, Waist and hip circumferences have independent and opposite effects on cardiovascular disease risk factors: the Quebec family study. Am. J. Clin. Nutr. 74, 315–321 (2001)
L. Lissner, C. Bjorkelund, B.L. Heitmann, J.C. Seidell, C. Bengtsson, Larger hip circumference independently predicts health and longevity in a Swedish female cohort. Obes. Res. 9, 644–646 (2001)
Y. Yildiz, G. Ozaksit, B. Serdar Unlu, E. Ozgu, H. Energin, M. Kaba, M. Ugur, Serum adiponectin level and clinical, metabolic, and hormonal markers in patients with polycystic ovary syndrome. Int. J. Fertil. Steril. 7, 331–336 (2014)
T.D. Brandebourg, J.L. Bown, B.J. Nira, Prolactin upregulates its receptors and inhibits lipolysis and leptin release in male rat adipose tissue. Biochem. Biophys. Res Commun. 357, 408–413 (2007)
O. Gualillo, F. Lago, M. García, C. Menéndez, R. Señarís, F.F. Casanueva, C. Diéguez, Prolactin stimulates leptin secretion by rat white adipose tissue. Endocrinology 140, 5149–5153 (1999)
J.A. Parsons, T.C. Brelje, R.L. Sorenson, Adaptation of islets of Langerhans to pregnancy: increased islet cell proliferation and insulin secretion correlates with the onset of placental lactogen secretion. Endocrinology 130, 1459–1466 (1992)
R.L. Sorenson, T.C. Brelje, Adaptation of islets of Langerhans to pregnancy: beta-cell growth, enhanced insulin secretion and the role of lactogenic hormones. Horm. Metab. Res. 29, 301–307 (1997)
S. Park, S. Kang, H.W. Lee, B.S. Ko, Central prolactin modulates insulin sensitivity and insulin secretion in diabetic rats. Neuroendocrinology 95, 332–343 (2012)
S. Park, S. da Kim, J.W. Daily, S.H. Kim, Serum prolactin concentrations determine whether they improve or impair β-cell function and insulin sensitivity in diabetic rats. Diabetes Metab. Res. Rev. 27, 564–574 (2011)
T. Bouckenooghe, G. Sisino, S. Aurientis, G. Chinetti-Gbaguidi, J. Kerr-Conte, B. Staels, P. Fontaine, L. Storme, F. Pattou, A. Vambergue, Adipose tissue macrophages (ATM) of obese patients are releasing increased levels of prolactin during an inflammatory challenge: a role for prolactin in diabesity? Biochim. Biophys. Acta 1842(4), 584–593 (2014). doi:10.1016/j.bbadis.2013.12.005.
Acknowledgments
We are grateful to all of the staff for helping with the data collection and for the technical assistance.
Conflict of interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Albu, A., Florea, S. & Fica, S. Is prolactin the missing link in adipose tissue dysfunction of polycystic ovary syndrome patients?. Endocrine 51, 163–173 (2016). https://doi.org/10.1007/s12020-015-0655-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-015-0655-1