Abstract
Background
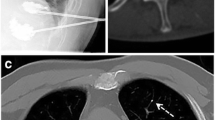
Percutaneous vertebroplasty is currently an alternative for treating vertebral fractures of the thoracic and lumbar spine, providing both pain control and vertebral stabilization. In the cervical spine, however, percutaneous vertebroplasty is technically challenging because of the complex anatomy of this region.
Questions/purposes
We evaluated the technical feasibility, complication rate, and ability of percutaneous vertebroplasty to provide pain relief in patients with painful metastatic cervical fractures.
Methods
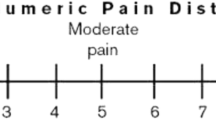
We retrospectively reviewed 62 patients (24 men) who, between May 2005 and May 2009, underwent vertebroplasty to treat painful metastatic cervical fractures. Each patient was evaluated by a visual analog scale for pain, number of pain analgesics, and CT and MRI before, the day after, and at 3 months after the procedure.
Results
Two of the 62 patients had asymptomatic cement leakage in the soft tissues. We observed no delayed complications. Mean pretreatment and 24-hour posttreatment visual analog scale pain scores were 7.9 ± 1.7 and 1.5 ± 2, respectively. Immediately after surgery, the pain completely disappeared in 25 (40%) patients. Administration of analgesics was suspended in 34 (55%) patients whereas in 27 (39%) patients the median analgesics use decreased from two pills per day (range, 0–3) to 0 (range, 0–3). In two (3%) patients, analgesics administration was continued due to the persistence of pain. At 3 months, the patients reported a mean visual analog scale pain score of 1.7 ± 2.
Conclusions
Our data suggest, in selected patients, percutaneous vertebroplasty may be performed with a high technical success rate combined with a low complication rate, providing immediate pain relief lasting at least 3 months and a reduction in the use of analgesic drugs.
Level of Evidence
Level IV, therapeutic study. See Guidelines for Authors for a complete description of levels of evidence.





Similar content being viewed by others
References
Barr JD, Barr MS, Lemley TJ, McCann RM. Percutaneous vertebroplasty for pain relief and spinal stabilization. Spine (Phila Pa 1976). 2000;25:923–928.
Barragán-Campos HM, Vallée JN, Lo D, Cormier E, Jean B, Rose M, Astagneau P, Chiras J. Percutaneous vertebroplasty for spinal metastases: complications. Radiology. 2006;238:354–362.
Böhm P, Huber J. The surgical treatment of bony metastases of spine and limbs. J Bone Joint Surg Br. 2002;84:521–529.
Calmels V, Vallée JN, Rose M, Chiras J. Osteoblastic and mixed spinal metastases: evaluation of the analgesic efficacy of percutaneous vertebroplasty. AJNR Am J Neuroradiol. 2007;28:570–574.
Chapman CR, Casey KL, Dubner R, Foley KM, Gracely RH, Reading AE. Pain measurement: an overview. Pain. 1985;22:1–31.
Chiras J, Depriester C, Weill A, Sola-Martinez MT, Deramond H. [Percutaneous vertebral surgery: technics and indications] [in French]. J Neuroradiol. 1997;24:45–59.
Cortet B, Cotten A, Boutry N, Dewatre F, Flipo RM, Duquesnoy B, Chastanet P, Delcambre B. Percutaneous vertebroplasty in patients with osteolytic metastases or multiple myeloma. Rev Rhum Engl Ed. 1997;64:177–183.
Cotten A, Dewatre F, Cortet B, Assaker R, Leblond D, Duquesnoy B, Chastanet P, Clarisse J. Percutaneous vertebroplasty for osteolytic metastases and myeloma: effects of the percentage of lesion filling and the leakage of methylmethacrylate at clinical follow-up. Radiology. 1996;200:525–530.
Deramond H, Deprestire C, Galibert P, Le Gars D. Percutaneous vertebroplasty with polymethylmethacrylate: technique, indications and results. Radiol Clin North Am. 1998;36:533–546.
Feydy A, Cognard C, Miaux Y, Sola Martínez MT, Weill A, Rose M, Chiras J. Acrylic vertebroplasty in symptomatic cervical vertebral haemangiomas: report of 2 cases. Neuroradiology. 1996;38:389–391.
Fung KY, Law SW. Management of malignant atlanto-axial tumours. J Orthop Surg (Hong Kong). 2005;13:232–239.
Gailloud P, Martin JB, Olivi A, Rüfenacht DA, Murphy KJ. Transoral vertebroplasty for a fractured C2 aneurysmal bone cyst. J Vasc Interv Radiol. 2002;13:340–341.
Gerszten PC, Welch WC. Current surgical management of metastatic spinal disease. Oncology. 2000;14:1013–1024.
Gupta S, Henningsen JA, Wallace MJ, Madoff DC, Morello FA Jr, Ahrar K, Murthy R, Hicks ME. Percutaneous biopsy of head and neck lesions with CT guidance: various approaches and relevant anatomic and technical considerations. Radiographics. 2007;27:371–390.
Hage WD, Aboulafia AJ, Aboulafia DM. Incidence, location, and diagnostic evaluation of metastatic bone disease. Orthop Clin North Am. 2000;31:515–528.
Harrington K. Metastatic tumors of the spine: diagnosis and treatment. J Am Acad Orthop Surg. 1993;1:76–86.
Janjan N. Bone metastases: approaches and management. Semin Oncol. 2001;28:28–34.
Jónsson B, Jónsson H Jr, Karlström G, Sjöström L. Surgery of cervical spine metastases: a retrospective study. Eur Spine J. 1994;3:76–83.
Levine SA, Perin LA, Hayes D, Hayes WS. An evidence-based evaluation of percutaneous vertebroplasty. Manag Care. 2000;9:56–60, 63.
Klimo P Jr, Schimdt MH. Surgical management of spinal metastases. Oncologist. 2004;9:188–196.
Martin JB, Gailloud P, Dietrich PY, Luciani ME, Somon T, Sappino PA, Rüfenach DA. Direct transoral approach to C2 percutaneous vertebroplasty. Cardiovasc Intervent Radiol. 2002;25:517–519.
Masala S, Mammucari M, Angelopoulos G, Fiori R, Massari F, Faria S, Simonetti G. Percutaneous vertebroplasty in the management of vertebral osteoporotic fractures: short-term, mid-term and long-term follow-up of 285 patients. Skeletal Radiol. 2009;38:863–869.
Masala S, Massari F, Fiori R, Mammucari M, Bartolucci DA, Simonetti G. Future directions in percutaneous vertebroplasty. Radiol Med. 2009;114:976–983.
Mercadante S. Malignant bone pain: pathophysiology and treatment. Pain. 1997;69:1–18.
Perrin RG, McBroom RJ, Perrin RG. Metastatic tumors of the cervical spine. Clin Neurosurg. 1991;37:740–755.
Pilitsis JG, Rengachary SS. The role of vertebroplasty in metastatic spinal disease. Neurosurg Focus. 2001;11:1–4.
Saarto T, Janes R, Tenhunen M, Kouri M. Palliative radiotherapy in the treatment of skeletal metastasis. Eur J Pain. 1989;6:323–330.
Sachs DC, Inamasu J, Mendel EE, Guiot BH. Transoral vertebroplasty for renal metastasis involving the axis. Spine (Phila Pa 1976). 2006;31:E925–E928.
Schachar NS. An update on the nonoperative treatment of patients with metastatic bone disease. Clin Orthop Relat Res. 2001;328:75–81.
Tong FC, Cloft HJ, Joseph GJ, Rodts GR, Dion JE. Transoral approach to cervical vertebroplasty for multiple myeloma. AJR Am J Roentgenol. 2000;175:1322–1324.
Weill A, Chiras J, Simon JM, Rose M, Sola-Martinez T, Enkaoua E. Spinal metastases: indications for and results of percutaneous injection of acrylic surgical cement. Radiology. 1996;199:241–247.
Author information
Authors and Affiliations
Corresponding author
Additional information
Each author certifies that he or she has no commercial associations (eg, consultancies, stock ownership, equity interest, patent/licensing arrangements, etc) that might pose a conflict of interest in connection with the submitted article.
Each author certifies that his or her institution approved the human protocol for this investigation and that all investigations were conducted in conformity with ethical principles of research, and that informed consent for participation in the study was obtained.
The work was performed at University of Rome “Tor Vergata”, at the Institute for Cancer Research and Treatment, and at Cardarelli Hospital.
About this article
Cite this article
Masala, S., Anselmetti, G.C., Muto, M. et al. Percutaneous Vertebroplasty Relieves Pain in Metastatic Cervical Fractures. Clin Orthop Relat Res 469, 715–722 (2011). https://doi.org/10.1007/s11999-010-1550-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-010-1550-y