Abstract
Introduction
Nutritional risk impacts outcome in developmental delay. The main objectives were to identify the incidence and factors contributing to growth faltering.
Methods
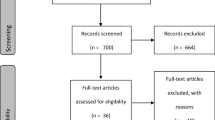
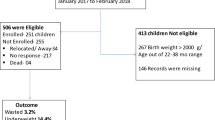
Clinical data review was completed for 500 patients with developmental delay accepted to an Early Intervention service. Data was collected using the standardised parent nutrition screening checklist prior to and at time of initial dietary assessment. Data was compared to nutritional assessment data, GOSH and FSAI dietary guidelines. Weight category was determined using RCPCH growth and BMI charts. Statistical analysis was conducted using Statistical Package for the Social Sciences version 20 (IBM Statistics 20.0).
Results
Nutritional risk was identified in 48.6 %. Weight categories were growth faltering (13.5 %), underweight (7.7 %), overweight (8.4 %) and obesity (4.3 %) at initial assessment. Growth faltering was correlated with age <1 year (p = 0.000) and with gestational age (p = 0.017) with highest rates identified in those born 32–36 weeks (3.6 %). Weight category was associated with introduction of solids pre 17 weeks recommendation (10.1 %), ANOVA demonstrating significance (P = 0.013). There was poor parental recognition of nutritional risk in 22.7 % of those assessed. Nutritional difficulties were common: 4.2 % were enterally fed, 7.7 % were on prescribed nutritional supplements, 29.1 % (n = 121) had feeding difficulties and 13.9 % (n = 58) had behavioural feeding difficulties. Iron intake did not meet the recommended intake in 20.9 % (n = 87), calcium in 4.5 % (n = 19). The prevalence of constipation was 21.6, 11.8 % of whom required medical management.
Conclusions
Developmental delay predisposes to nutritional deficits which influence outcome. Screening, assessment and timely interventions are warranted to prevent poorer developmental outcomes.


Similar content being viewed by others

References
Sullivan PB, Juszczak E, Lambert BR et al (2002) Impact of feeding problems in nutritional intake and growth: Oxford Feeding Study II. Dev Child Med Neurol 44:461–467
Carey AM, McClelland D, McCarthy H (2011) A survey of paediatric nutrition care in paediatric dietetics throughout the UK and Ireland. J Human Nutr Diet 24(3):278–279
Marchand V, Canadian Paediatric Society, Nutrition and Gastroenterology Committee (2009) Nutrition in neurologically impaired children. Paeditr Child Health 14(6):395–401
Kuperminc MN, Stevenson RD (2008) Growth and nutrition disorders in children with cerebral palsy. Dev Disabil Res Rev 14:137–146
Bohmer CJ, Niezen DE, Boer MC et al (1999) The prevalence of gastroesophageal reflux in institutionalised intellectually disabled individuals. Am J Gastroenterol 94:804–810
Linscheid TR, Budd KS, Rasake LK (2003) Pediatric feeding problems. In: Roberts MC (ed) Handbook of paediatric psychology, 3rd edn. Guilford Press, New York, pp 482–498
Wright C, Birks E (2000) Risk factors for failure to thrive: a population based survey. Child Care Health Dev 26:5–16
Kuban KC, Allied EN, O’Shea TM et al (2009) Developmental correlates of head circumference at birth and 2 years in a cohort of extremely low gestational age newborns. J Pediatr 155:344–349
Mustsuo K, Palmer JB (2008) Anatomy and physiology of feeding and swallowing—normal and abnormal. Phys Med Rehabil Clin N AM 19:691–707
Shields WD (2000) Catastrophic epilepsy in childhood. Epilepsia 41(2):S2–S6
Bertolil S, Cardinali S, Veggiotti P et al (2006) Evaluation of nutritional status in children with refractory epilepsy. Nutr J 5:14
Arvedson JC (2008) Assessment of pediatric dysphagia and feeding disorders: clinical and instrumental approaches. Dev Disabil Res Rev 14:118–127
Santoro A, Dasso Lang MB, Moretti E et al (2012) A proposed multidisciplinary approach to identifying feeding abnormalities in children with cerebral palsy. J Child Neurol 27:708–712
Erkin G, Culha O, Ozel S et al (2010) Feeding and gastrointestinal problems in children with cerebral palsy. Int J Rehabil Res 33:218–224
Parkes J, Hill NAN, Platt MJ et al (2010) Oromotor dysfunction and communication impairments in children with cerebral palsy: a register study. Dev Med Child Neurol 52:1113–1119
Brooks J, Day S, Shavelle R et al (2011) Low weight, morbidity and mortality in children with cerebral palsy: new clinical growth charts. Paediatrics 128:299–307
Sullivan PB, McIntyre E (2005) Gastrointestinal problems in disabled children. Curr Paediatr 15:347–353
The importance of nutrition far the person with epilepsy. Nutrition information centre. Stellenboch University (NICUS) [homepage on the Internet]. http://www.sun.ac.za/nicus
SACN (Scientific Advisory Committee on Nutrition) (2010) Iron and Health. The Stationary Office, London, p 373
Idadinatia P, Pollitt E (1993) Reversal of development delays in iron-deficient anaemic infants treated with iron. Lancet 341:1–4
Wittenbrook W (2011) Nutritional assessment and intervention in cerebral palsy. Pract Gastroenterol 16:21–32
Wolff J, Sinesi M (2011) Enteral management of children with neurological disease. Support Line 33(5):3–10
Parrish CR (2011) Nutritional assessment and intervention in cerebral palsy. Pract Gastroenterol
Squires J, Bricker D Ages and stages questionaires, (ASQ-3) (3rd ed). Brookes publishing, Baltimore. www.agesandstages.com
Schlenker J, Cocking J, Gilley J (2003) Development of nutrition screening checklist for children with special needs. DC Paediatr Nutr 1:4
UK-WHO growth charts. RCPCH 2010. www.growthcharts.rcpch.ac.uk
Food Safety Authority of Ireland (2011) Scientific recommendations for healthy eating guidelines in Ireland. Dublin
Great Ormond Street Hospital (2000) Nutritonal requirements for children in health and disease, 3rd edn. Great Ormond Street Hospital for Children NHS Trust, London
Gibson RS (2005) Principles of nutritional assessment, 2nd edn. Oxford Press, New York
Corp IBM (2011) IBM SPSS statistics for windows, version 20.0. IBM Corp, Armonk
Schwartz SM, Corredor J, Fisher-Medina J et al (2001) Diagnosis and treatment of feeding disorders in children with developmental disabilities. Pediatrics 108:167
Wiskin AE, Owens DR, Cornelius VR et al (2012) Paediatric nutrition risk scores in clinical practice: children with inflammatory bowel disease. J Hum Nutr Diet 25:319–322
Position of the American Dietetic Association (2010) Providing nutrition services for people with developmental disabilities and special health care needs. J Am Diet Assoc 110:296–307
Rietmeijer-Mentink M, Paulis W, Middelkoop M et al (2013) Difference between parental perception and actual weight status of children: a systematic review. Matern Child Nutr 9(1):3–22
Andrew MJ, Sullivan PB (2010) Growth in cerebral palsy. Nutr Clin Pract 25:357–361
Campanozzi A, Capano G, Mele E et al (2007) Impact of malnutrition on gastrointestinal disorders and gross motor abilities in children with cerebral palsy. Brain Dev 29:25–29
Lionti T, Reid SM, Reddihough D et al (2013) Monitoring height and weight: findings from a developmental paediatric service. J Paediatr Child Health 49:1063–1068
Khalessi AR, Stephanie M (2013) A month of breastfeeding associated with greater adherence to paediatric nutrition guidelines. J Reprod Infant Psychol 31:299–308
Sullivan PB, Lambert B, Rose M et al (2000) Prevalence and severity of feeding and nutritional problems in children with neurological impairment: Oxford Feeding Study. Dev Med Child Neurol 42:10–80
Sommerville H, Wood J, Shun A et al (2008) Gastrointestinal and nutritional problems in severe developmental disability. Dev Med Child Neurol 50:712–716
Veugelers R, Benninga MA, Calis EA et al (2010) Prevalence and clinical presentation of constipation in children with severe generalised cerebral palsy. Dev Med Child Neurol 52:216–221
Borowitz SM, Sutplen JL (2004) Recurrent vomiting and persistent gastroesophageal reflux caused by unrecognised constipation. Clin Pediatr (Phila) 43:461–466
Sheridan KJ (2009) Osteoporosis in adults with cerebral palsy. Dev Med Child Neurol 51(4):38–51
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We wish to declare that there are no conflicts of interest arising.
Funding
Funding was not received for completion of this research.
Rights and permissions
About this article
Cite this article
Malone, C., Sharif, F. & Glennon-Slattery, C. Growth and nutritional risk in children with developmental delay. Ir J Med Sci 185, 839–846 (2016). https://doi.org/10.1007/s11845-015-1377-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-015-1377-3