Abstract
Purpose
For young women who were diagnosed with cancer prior to having children, reproductive potential might affect the quality of life (QoL). This systematic review looks at fertility issues in young female cancer patients, focusing on their influence on psychological well-being, specific fertility-related interventions and reproductive decisions.
Methods
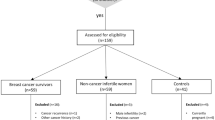
Thirteen medical and social science databases were searched for relevant articles up to December 2012, according to PRISMA guidelines. Twenty-six articles meeting the eligibility criteria were included in the review, along with 5 additional papers that missed the inclusion criteria narrowly. Narrative synthesis was used to analyse the studies.
Results
Depression, anxiety and quality of life (QoL) seemed to be related to the perceptions of reproductive issues rather than to the fertility status based on the type of treatment received. Fertility-related interventions improved patients’ QoL, decisional regret, and decisional conflict. Finally, cancer influenced women’s reproductive decisions. Pursuing pregnancy was affected mainly by worries about child’s and mother’s health. Decisions about treatment were influenced by the wish to preserve fertility. The generalisability of these results might be undermined by small sample sizes and homogeneity of participants within and across the studies. Inferences about causality of associations are problematic due to predominantly cross-sectional design.
Implications for Cancer Survivors
The existing literature gives preliminary insight into the importance of fertility for young women diagnosed with cancer. However, more research is needed in order to offer patients comprehensive care.
Similar content being viewed by others
References
Aziz NM, Rowland JH. Trends and advances in cancer survivorship research: challenge and opportunity. Semin Radiat Oncol. 2003. doi:10.1016/S1053-4296(03)00024-9.
Dow KH. Having children after breast cancer. Cancer Pract. 1994;2(6):407–13.
Siegel K, Gorey E, Gluhoski V. Pregnancy decision making among women previously treated for breast cancer. J Psychosoc Oncol. 1997. doi:10.1300/j077v15n01_03.
Siegel K, Gluhoski V, Gorey E. Age-related distress among young women with breast cancer. J Psychosoc Oncol. 1999. doi:10.1300/J077v17n01_01.
Connell S, Patterson C, Newman B. A qualitative analysis of reproductive issues raised by young Australian women. Health Care Women Int. 2006. doi:10.1080/07399330500377580.
Yee S, Abrol K, McDonald M, Tonelli M, Liu KE. Addressing oncofertility needs: views of female cancer patients in fertility preservation. J Psychosoc Oncol. 2012. doi:10.1080/07347332.2012.664257.
Mean age of mothers at first childbirth. In: OECD Family Database. Organisation for Economic Co-operation and Development. 2012. http://www.oecd.org/social/soc/SF2.3%20Mean%20age%20of%20mother%20at%20first%20childbirth%20-%20updated%20240212.pdf. Accessed 3 Mar 2014
Wallace WH, Anderson RA, Irvine DS. Fertility preservation for young patients with cancer: who is at risk and what can be offered? Lancet Oncol. 2005. doi:10.1016/S1470-2045(05)70092-9.
Knobf MT. Reproductive and hormonal sequelae of chemotherapy in women. Premature menopause and impaired fertility can result, effects that are especially disturbing to young women. Am J Nurs. 2006;106(3 Suppl):60–5.
Duffy C, Allen S. Medical and psychosocial aspects of fertility after cancer. Cancer J. 2009. doi:10.1097/PPO.0b013e3181976602.
Lee MC, Gray J, Han HS, Plosker S. Fertility and reproductive considerations in premenopausal patients with breast cancer. Cancer Control. 2010;17(3):162–72.
Barthelmes L, Gateley CA. Tamoxifen and pregnancy. Breast. 2004. doi:10.1016/j.breast.2004.08.007.
Thewes B, Meiser B, Taylor A, Phillips KA, Pendlebury S, Capp A, et al. Fertility- and menopause-related information needs of younger women with a diagnosis of early breast cancer. J Clin Oncol. 2005. doi:10.1200/JCO.2005.07.773.
Breast Cancer Treatment (PDQ®). National Cancer Institute. 2013. http://www.cancer.gov/cancertopics/pdq/treatment/breast/healthprofessional/page6#Section_95. Accessed 7 Feb 2013
Lee SJ, Schover LR, Partridge AH, Patrizio P, Wallace WH, Hagerty K, et al. American Society of Clinical Oncology recommendations on fertility preservation in cancer patients. J Clin Oncol. 2006. doi:10.1200/jco.2006.06.5888.
Loren AW, Mangu PB, Beck LN, Brennan L, Magdalinski AJ, Partridge AH, et al. Fertility preservation for patients with cancer: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol. 2013. doi:10.1200/jco.2013.49.2678.
Klock SC, Zhang JX, Kazer RR. Fertility preservation for female cancer patients: early clinical experience. Fertil Steril. 2010. doi:10.1016/j.fertnstert.2009.03.028.
Quinn GP, Vadaparampil S, Gwede C, Miree C, King LM, Clayton HB, et al. Discussion of fertility preservation with newly diagnosed patients: oncologists’ views. J Cancer Surviv. 2007. doi:10.1007/s11764-007-0019-9.
Duffy C, Allen S, Clark M. Discussions regarding reproductive health for young women with breast cancer undergoing chemotherapy. J Clin Oncol. 2005. doi:10.1200/jco.2005.01.134.
Quinn GP, Vadaparampil ST, Bell-Ellison BA, Gwede CK, Albrecht TL. Patient–physician communication barriers regarding fertility preservation among newly diagnosed cancer patients. Soc Sci Med. 2008. doi:10.1016/j.socscimed.2007.09.013.
Partridge AH, Gelber S, Peppercorn J, Sampson E, Knudsen K, Laufer M, et al. Web-based survey of fertility issues in young women with breast cancer. J Clin Oncol. 2004. doi:10.1200/jco.2004.01.159.
Partridge AH, Ruddy KJ. Fertility and adjuvant treatment in young women with breast cancer. Breast. 2007. doi:10.1016/j.breast.2007.07.029.
Adams E, McCann L, Armes J, Richardson A, Stark D, Watson E, et al. The experiences, needs and concerns of younger women with breast cancer: a meta-ethnography. Psychooncology. 2011. doi:10.1002/pon.1792.
Goncalves V, Sehovic I, Quinn G. Childbearing attitudes and decisions of young breast cancer survivors: a systematic review. Hum Reprod Update. 2014. doi:10.1093/humupd/dmt039.
Holton S, Kirkman M, Rowe H, Fisher J. The childbearing concerns and related information needs and preferences of women of reproductive age with a chronic, noncommunicable health condition: a systematic review. Womens Health Issues. 2012. doi:10.1016/j.whi.2012.08.001.
Howard-Anderson J, Ganz PA, Bower JE, Stanton AL. Quality of life, fertility concerns, and behavioral health outcomes in younger breast cancer survivors: a systematic review. J Natl Cancer Inst. 2012. doi:10.1093/jnci/djr541.
Peate M, Meiser B, Hickey M, Friedlander M. The fertility-related concerns, needs and preferences of younger women with breast cancer: a systematic review. Breast Cancer Res Treat. 2009. doi:10.1007/s10549-009-0401-6.
Wenzel L, Dogan-Ates A, Habbal R, Berkowitz R, Goldstein DP, Bernstein M, et al. Defining and measuring reproductive concerns of female cancer survivors. J Natl Cancer Inst Monogr. 2005. doi:10.1093/jncimonographs/lgi017.
Thomas F, Renaud F, Benefice E, De Meeus T, Guegan J-F. International variability of ages at menarche and menopause: patterns and main determinants. Hum Biol. 2001:271–90.
Dargent D, Brun JL, Roy M, Remy I. Pregnancies following radical trachelectomy for invasive cervical cancer. Gynecol Oncol. 1994. doi:10.1006/gyno.1994.1020.
Carter J, Chi DS, Brown CL, Abu-Rustum NR, Sonoda Y, Aghajanian C, et al. Cancer-related infertility in survivorship. Int J Gynecol Cancer. 2010. doi:10.1111/IGC.0b013e3181bf7d3f.
Ganz PA, Greendale GA, Petersen L, Kahn B, Bower JE. Breast cancer in younger women: reproductive and late health effects of treatment. J Clin Oncol. 2003. doi:10.1200/jco.2003.04.196.
Sait KH. Conservative treatment of ovarian cancer safety, ovarian function preservation, reproductive ability, and emotional attitude of the patients in Saudi Arabia. Saudi Med J. 2011;32(9):913–8.
Letourneau JM, Ebbel EE, Katz PP, Katz A, Ai WZ, Chien AJ, et al. Pretreatment fertility counseling and fertility preservation improve quality of life in reproductive age women with cancer. Cancer. 2012. doi:10.1002/cncr.26459.
Letourneau JM, Smith JF, Ebbel EE, Craig A, Katz PP, Cedars MI, et al. Racial, socioeconomic, and demographic disparities in access to fertility preservation in young women diagnosed with cancer. Cancer. 2012. doi:10.1002/cncr.26649.
Peate M, Meiser B, Friedlander M, Zorbas H, Rovelli S, Sansom-Daly U, et al. It's now or never: fertility-related knowledge, decision-making preferences, and treatment intentions in young women with breast cancer—an Australian fertility decision aid collaborative group study. J Clin Oncol. 2011. doi:10.1200/jco.2010.31.2462.
Peate M, Meiser B, Cheah BC, Saunders C, Butow P, Thewes B, et al. Making hard choices easier: a prospective, multicentre study to assess the efficacy of a fertility-related decision aid in young women with early-stage breast cancer. Br J Cancer. 2012. doi:10.1038/bjc.2012.61.
Carter J, Sonoda Y, Abu-Rustum NR. Reproductive concerns of women treated with radical trachelectomy for cervical cancer. Gynecol Oncol. 2007. doi:10.1016/j.ygyno.2006.10.059.
Carter J, Sonoda Y, Baser RE, Raviv L, Chi DS, Barakat RR, et al. A 2-year prospective study assessing the emotional, sexual, and quality of life concerns of women undergoing radical trachelectomy versus radical hysterectomy for treatment of early-stage cervical cancer. Gynecol Oncol. 2010. doi:10.1016/j.ygyno.2010.07.016.
Kmet L, Lee R, Cook L. Standard quality assessment criteria for evaluating primary research papers from a variety of fields. In: HTA Initiative 13. 2004. http://www.ihe.ca/documents/HTA-FR13.pdf. Accessed 7 Feb 2014.
Viera AJ, Garrett JM. Understanding interobserver agreement: the kappa statistic. Fam Med. 2005;37(5):360–3.
Avis NE, Crawford S, Manuel J. Psychosocial problems among younger women with breast cancer. Psychooncology. 2004. doi:10.1002/pon.744.
Carter J, Raviv L, Sonoda Y, Chi DS, Abu-Rustum NR. Recovery issues of fertility-preserving surgery in patients with early-stage cervical cancer and a model for survivorship the physician checklist. Int J Gynecol Cancer. 2011. doi:10.1097/IGC.0b013e3182017989.
Bisseling K, Kondalsamy-Chennakesavan S, Bekkers RLM, Janda M, Obermair A. Depression, anxiety and body image after treatment for invasive stage one epithelial ovarian cancer. Aust N Z J Obstet Gynaecol. 2009. doi:10.1111/j.1479-828X.2009.01074.x.
Carter J, Rowland K, Chi D, Brown C, Abu-Rustum N, Castiel M, et al. Gynecologic cancer treatment and the impact of cancer-related infertility. Gynecol Oncol. 2005. doi:10.1016/j.ygyno.2004.12.019.
Gorman JR, Malcarne VL, Roesch SC, Madlensky L, Pierce JP. Depressive symptoms among young breast cancer survivors: the importance of reproductive concerns. Breast Cancer Res Treat. 2010. doi:10.1007/s10549-010-0768-4.
Ganz PA, Land SR, Geyer CE, Cecchini RS, Costantino JP, Pajon ER, et al. Menstrual history and quality-of-life outcomes in women with node-positive breast cancer treated with adjuvant therapy on the NSABP B-30 trial. J Clin Oncol. 2011. doi:10.1200/jco.2010.29.7689.
Mancini J, Rey D, Preau M, Malavolti L, Moatti JP. Infertility induced by cancer treatment: inappropriate or no information provided to majority of French survivors of cancer. Fertil Steril. 2008. doi:10.1016/j.fertnstert.2007.08.064.
Wenzel L, DeAlba I, Habbal R, Kluhsman BC, Fairclough D, Krebs LU, et al. Quality of life in long-term cervical cancer survivors. Gynecol Oncol. 2005. doi:10.1016/j.ygyno.2005.01.010.
Canada AL, Schover LR. The psychosocial impact of interrupted childbearing in long-term female cancer survivors. Psychooncology. 2012. doi:10.1002/pon.1875.
Meneses K, McNees P, Azuero A, Jukkala A. Evaluation of the Fertility and Cancer Project (FCP) among young breast cancer survivors. Psychooncology. 2010. doi:10.1002/pon.1648.
Reh AE, Lu L, Weinerman R, Grifo J, Krey L, Noyes N. Treatment outcomes and quality-of-life assessment in a university-based fertility preservation program: results of a registry of female cancer patients at 2 years. J Assist Reprod Genet. 2011. doi:10.1007/s10815-011-9559-z.
The WHOQOL Group. Development of the World Health Organization WHOQOL-BREF quality of life assessment. Psychol Med. 1998;28(03):551–8.
Diener E, Emmons RA, Larsen RJ, Griffin S. The satisfaction with life scale. J Pers Assess. 1985;49(1):71–5.
Brazier J, Harper R, Jones N, O'cathain A, Thomas K, Usherwood T, et al. Validating the SF-36 health survey questionnaire: new outcome measure for primary care. Br Med J. 1992;305(6846):160.
Brady MJ, Cella DF, Mo F, Bonomi AE, Tulsky DS, Lloyd SR, et al. Reliability and validity of the functional assessment of cancer therapy-breast quality-of-life instrument. J Clin Oncol. 1997;15(3):974–86.
Brehaut JC, O'Connor AM, Wood TJ, Hack TF, Siminoff L, Gordon E, et al. Validation of a decision regret scale. Med Decis Making. 2003. doi:10.1177/0272989X03256005.
Zanagnolo V, Sartori E, Trussardi E, Pasinetti B, Maggino T. Preservation of ovarian function, reproductive ability and emotional attitudes in patients with malignant ovarian tumors. Eur J Obstet Gyn R B. 2005. doi:10.1016/j.ejogrb.2005.04.010.
Huyghe E, Sui D, Odensky E, Schover LR. Needs assessment survey to justify establishing a Reproductive Health Clinic at a Comprehensive Cancer Center. J Sex Med. 2009. doi:10.1111/j.1743-6109.2008.01005.x.
Braun M, Hasson-Ohayon I, Perry S, Kaufman B, Uziely B. Motivation for giving birth after breast cancer. Psychooncology. 2005. doi:10.1002/pon.844.
Patel A, Sreedevi M, Malapati R, Sutaria R, Schoenhage MB, Patel AR, et al. Reproductive health assessment for women with cancer: a pilot study. Am J Obstet Gynecol. 2009. doi:10.1016/j.ajog.2009.04.021.
Atkinson TM, Noce NS, Hay J, Rafferty BT, Brady MS. Illness-related distress in women with clinically localized cutaneous melanoma. Ann Surg Oncol. 2012. doi:10.1245/s10434-012-2635-5.
Rippy EE, Karat IF, Kissin MW. Pregnancy after breast cancer: the importance of active counselling and planning. Breast. 2009. doi:10.1016/j.breast.2009.08.003.
Scanlon M, Blaes A, Geller M, Majhail NS, Lindgren B, Haddad T. Patient satisfaction with physician discussions of treatment impact on fertility. J Cancer. 2012. doi:10.7150/jca.4408.
Gorman JR, Roesch SC, Parker BA, Madlensky L, Saquib N, Newman VA, et al. Physical and mental health correlates of pregnancy following breast cancer. Psychooncology. 2010. doi:10.1002/pon.1614.
Gershenson DM, Miller AM, Champion VL, Monahan PO, Zhao QQ, Cella D, et al. Reproductive and sexual function after platinum-based chemotherapy in long-term ovarian germ cell tumor survivors: a gynecologic oncology group study. J Clin Oncol. 2007. doi:10.1200/jco.2006.08.4590.
Schover LR, Rybicki LA, Martin BA, Bringelsen KA. Having children after cancer—a pilot survey of survivors' attitudes and experiences. Cancer. 1999. doi:10.1002/(sici)1097-0142(19990815)86:4<697::aid-cncr20>3.0.co;2-j.
Boss EA, van Golde RJ, Beerendonk CC, Massuger LF. Pregnancy after radical trachelectomy: a real option? Gynecol Oncol. 2005. doi:10.1016/j.ygyno.2005.07.071.
Jolley JA, Battista L, Wing DA. Management of pregnancy after radical trachelectomy: case reports and systematic review of the literature. Am J Perinatol. 2007. doi:10.1055/s-2007-986680.
Leventhal H, Meyer D, Nerenz D. The common sense representation of illness danger. In: Rachman S, editor. Contributions to medical psychology. Oxford: Pergamon Pr; 1980. p. 7–30.
Leventhal H, Leventhal EA, Contrada RJ. Self-regulation, health, and behavior: a perceptual-cognitive approach. Psychol Health. 1998. doi:10.1080/08870449808407425.
Simard S, Thewes B, Humphris G, Dixon M, Hayden C, Mireskandari S, et al. Fear of cancer recurrence in adult cancer survivors: a systematic review of quantitative studies. J Cancer Surviv. 2013. doi:10.1007/s11764-013-0272-z.
Stacey D, Légaré F, Col NF, Bennett CL, Barry MJ, Eden KB et al. Decision aids for people facing health treatment or screening decisions. Cochrane Database Syst Rev. 2014(1). doi:10.1002/14651858.CD001431.pub4
Bruera E, Sweeney C, Calder K, Palmer L, Benisch-Tolley S. Patient preferences versus physician perceptions of treatment decisions in cancer care. J Clin Oncol. 2001;19(11):2883–5.
Degner LF, Sloan JA. Decision making during serious illness: what role do patients really want to play? J Clin Epidemiol. 1992. doi:10.1016/0895-4356(92)90110-9.
Degner LF, Kristjanson LJ, Bowman D, et al. Information needs and decisional preferences in women with breast cancer. JAMA. 1997. doi:10.1001/jama.1997.03540420081039.
Blanchard CG, Labrecque MS, Ruckdeschel JC, Blanchard EB. Information and decision-making preferences of hospitalized adult cancer patients. Soc Sci Med. 1988. doi:10.1016/0277-9536(88)90343-7.
Gaston CM, Mitchell G. Information giving and decision-making in patients with advanced cancer: a systematic review. Soc Sci Med. 2005. doi:10.1016/j.socscimed.2005.04.015.
Jenkins V, Fallowfield L, Saul J. Information needs of patients with cancer: results from a large study in UK cancer centres. Br J Cancer. 2001. doi:10.1054/bjoc.2000.1573.
Mills ME, Sullivan K. The importance of information giving for patients newly diagnosed with cancer: a review of the literature. J Clin Nurs. 1999. doi:10.1046/j.1365-2702.1999.00296.x.
Street Jr RL, Makoul G, Arora NK, Epstein RM. How does communication heal? Pathways linking clinician–patient communication to health outcomes. Patient Educ Couns. 2009. doi:10.1016/j.pec.2008.11.015.
Gray NJ, Klein JD, Noyce PR, Sesselberg TS, Cantrill JA. Health information-seeking behaviour in adolescence: the place of the internet. Soc Sci Med. 2005. doi:10.1016/j.socscimed.2004.08.010.
Rideout V. Generation Rx.com. What are young people really doing online? Mark Health Serv. 2002;22(1):26–30.
Bender JL, Jimenez-Marroquin M-C, Jadad AR. Seeking support on Facebook: a content analysis of breast cancer groups. J Med Internet Res. 2011. doi:10.2196/jmir.1560.
Davison KP, Pennebaker JW, Dickerson SS. Who talks? The social psychology of illness support groups. Am Psychol. 2000. doi:10.1037/0003-066X.55.2.205.
Gustafson DH, Wise M, McTavish F, Taylor JO, Wolberg W, Stewart J, et al. Development and pilot evaluation of a computer-based support system for women with breast cancer. J Psychosoc Oncol. 1994. doi:10.1300/J077V11N04_05.
Gustafson DH, Hawkins R, Pingree S, McTavish F, Arora NK, Mendenhall J, et al. Effect of computer support on younger women with breast cancer. J Gen Intern Med. 2001. doi:10.1046/j.1525-1497.2001.016007435.x.
Lieberman MA, Golant M, Giese–Davis J, Winzlenberg A, Benjamin H, Humphreys K, et al. Electronic support groups for breast carcinoma. Cancer. 2003. doi:10.1002/cncr.11145.
van den Berg SW, Gielissen MF, Ottevanger PB, Prins JB. Rationale of the BREAst cancer e-healTH [BREATH] multicentre randomised controlled trial: an internet-based self-management intervention to foster adjustment after curative breast cancer by decreasing distress and increasing empowerment. BMC Cancer. 2012. doi:10.1186/1471-2407-12-394.
Winzelberg AJ, Classen C, Alpers GW, Roberts H, Koopman C, Adams RE, et al. Evaluation of an internet support group for women with primary breast cancer. Cancer. 2003. doi:10.1002/cncr.11174.
Treasure T, Bewley S, Bhattacharya S, Brian K, Child T, Davies M et al. Fertility: Assessment and treatment for people with fertility problems. In: NICE clinical guidelines. National Institute for Health and Care Excellence. 2013. http://publications.nice.org.uk/fertility-cg156/recommendations. Accessed 14 Mar 2014.
Quinn GP, Vadaparampil ST, Lee J-H, Jacobsen PB, Bepler G, Lancaster J, et al. Physician referral for fertility preservation in oncology patients: a national study of practice behaviors. J Clin Oncol. 2009;27(35):5952–7. doi:10.1200/jco.2009.23.0250.
Peddie VL, Porter MA, Barbour R, Culligan D, MacDonald G, King D, et al. Factors affecting decision making about fertility preservation after cancer diagnosis: a qualitative study. BJOG. 2012. doi:10.1111/j.1471-0528.2012.03368.x.
Dursun P, LeBlanc E, Nogueira MC. Radical vaginal trachelectomy (Dargent's operation): a critical review of the literature. Eur J Surg Oncol. 2007. doi:10.1016/j.ejso.2006.11.021.
Kahneman D, Tversky A. Prospect theory: an analysis of decision under risk. Econometrica. 1979. doi:10.2307/1914185.
Treadwell JR, Lenert LA. Health values and prospect theory. Med Decis Making. 1999. doi:10.1177/0272989X9901900313.
Blakely LJ, Buzdar AU, Lozada JA, Shullaih SA, Hoy E, Smith TL, et al. Effects of pregnancy after treatment for breast carcinoma on survival and risk of recurrence. Cancer. 2004. doi:10.1002/cncr.11929.
Gelber S, Coates AS, Goldhirsch A, Castiglione-Gertsch M, Marini G, Lindtner J, et al. Effect of pregnancy on overall survival after the diagnosis of early-stage breast cancer. J Clin Oncol. 2001;19(6):1671–5.
Ives A, Saunders C, Bulsara M, Semmens J. Pregnancy after breast cancer: population based study. Br Med J. 2007. doi:10.1136/bmj.39035.667176.55.
Fosså SD, Magelssen H, Melve K, Jacobsen AB, Langmark F, Skjærven R. Parenthood in survivors after adulthood cancer and perinatal health in their offspring: a preliminary report. J Natl Cancer Inst Monogr. 2005. doi:10.1093/jncimonographs/lgi019.
Kenney LB, Nicholson HS, Brasseux C, Mills JL, Robison LL, Zeltzer LK, et al. Birth defects in offspring of adult survivors of childhood acute lymphoblastic leukemia: a Childrens Cancer Group/National Institutes of Health report. Cancer. 1996. doi:10.1002/(SICI)1097-0142(19960701)78:1<169::AID-CNCR23>3.0.CO;2-X.
Hynie M, Burns LH. Cross-cultural issues in infertility counseling. In: Covington SN, Hammer BL, editors. Infertility Counseling: a comprehensive handbook for clinicians. Cambridge: Cambridge University Press; 2006. p. 61–82.
Funding
Aleksandra Sobota’s PhD is funded by the Danuta Richardson Medical Scholarship. This systematic review has not received any additional funding.
Conflict of interest
Aleksandra Sobota and Gozde Ozakinci declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
No animal or human studies were carried out by the authors for this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sobota, A., Ozakinci, G. Fertility and parenthood issues in young female cancer patients—a systematic review. J Cancer Surviv 8, 707–721 (2014). https://doi.org/10.1007/s11764-014-0388-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-014-0388-9