Abstract
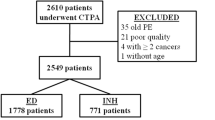
Recent guidelines for diagnosing acute pulmonary embolism (PE) are based on clinical decision rules and d-dimer. d-dimer measurement is recommended only for patients who are ‘PE-unlikely’. We aimed to assess the current guidelines for cancer patients and to determine an optimal d-dimer cut-off level. This retrospective observational study was conducted in the emergency department of Asan Medical Center (Seoul, Korea) between 02/2017 and 09/2017 for the development cohort and between 06/2018 and 02/2019 for the validation cohort. Among adult active cancer patients with suspected PE, we included those who were ‘PE-unlikely’ according to Wells’ criteria and who underwent d-dimer testing and computed tomographic pulmonary angiography (CTPA). A total of 498 patients (227 in the development cohort and 271 in the validation cohort) were included, and PE was diagnosed in 8.8% and 18.5% of patients, respectively. The optimal d-dimer cut-off level was 2.0 μg/mL. This elevated cut-off level showed a much higher specificity of 21.3% (95% confidence interval [CI] 16.2–27.3%) and 21.7% (95% CI 16.8–7.6%) in the development and validation sets, respectively, compared with the specificity of 4.4% (95% CI 2.3–8.1%) and 4.1% (95% CI 2.2–7.6%) using the age-adjusted cut-off. The new d-dimer cut-off value identified unnecessary CTPA for 21.3% of patients (absolute difference, 16.9%, 35 of 207) in the development cohort and 21.7% (absolute difference, 17.6%, 39 of 221) of patients in the validation cohort compared to using the standard age-adjusted cut-off. The elevated d-dimer cut-off value combined with Wells’ criteria might reduce unnecessary CTPA in active cancer patients with a ‘PE-unlikely’ classification. Further clinical trials are warranted to improve the PE diagnostic strategy in cancer patients.

Similar content being viewed by others
Availability of data and material
If you request the corresponding author by e-mail for justifiable reasons, it will be considered.
References
Khorana A, Francis C, Culakova E, Kuderer N, Lyman H (2007) Thromboembolism is a leading cause of death in cancer patients receiving outpatient chemotherapy. J Thromb Haemost 5(3):632–634
Donnellan E, Khorana AA (2017) Cancer and venous thromboembolic disease: a review. Oncologist 22(2):199
Elyamany G, Alzahrani AM, Bukhary EJ (2014) Cancer-associated thrombosis: an overview. Clin Med Insights Oncol 8:CMO18991
Streiff MB, Bockenstedt PL, Cataland SR, Chesney C, Eby C, Fanikos J, Fogerty AE, Gao S, Goldhaber SZ, Hassoun H (2013) Venous thromboembolic disease. J Natl Compr Cancer Netw 11(11):1402–1429
Konstantinides SV, Meyer G, Becattini C, Bueno H, Geersing G-J, Harjola V-P, Huisman MV, Humbert M, Jennings CS, Jiménez DJ (2020) 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS) The Task Force for the diagnosis and management of acute pulmonary embolism of the European Society of Cardiology (ESC). Eur Heart J 41(4):543–603
Righini M, Robert-Ebadi H, Le Gal GJ (2017) Diagnosis of acute pulmonary embolism. J Thromb Haemost 15(7):1251–1261
Righini M, Le Gal G, De Lucia S, Roy P, Meyer G, Aujesky D, Bounameaux H, Perrier A (2006) Clinical usefulness of d-dimer testing in cancer patients with suspected pulmonary embolism. Thromb Haemost 95(4):715
Di Nisio M, Sohne M, Kamphuisen P, Büller HR (2005) d-Dimer test in cancer patients with suspected acute pulmonary embolism. J Thromb Haemost 3(6):1239–1242
Douma RA, Mos IC, Erkens PM, Nizet TA, Durian MF, Hovens MM, van Houten AA, Hofstee HM, Klok FA, ten Cate H (2011) Performance of 4 clinical decision rules in the diagnostic management of acute pulmonary embolism: a prospective cohort study. Ann Intern Med 154(11):709–718
Chabloz P, Reber G, Boehlen F, Hohlfeld P, De Moerloose P (2001) TAFI antigen and d-dimer levels during normal pregnancy and at delivery. Br J Haematol 115(1):150–152
Chae B-R, Kim Y-J, Lee Y-S (2020) Prognostic accuracy of the sequential organ failure assessment (SOFA) and quick SOFA for mortality in cancer patients with sepsis defined by systemic inflammatory response syndrome (SIRS). Support Care Cancer 28(2):653–659
Stein PD, Fowler SE, Goodman LR, Gottschalk A, Hales CA, Hull RD, Leeper KV Jr, Popovich J Jr, Quinn DA, Sos TA (2006) Multidetector computed tomography for acute pulmonary embolism. N Engl J Med 354(22):2317–2327
Ceriani E, Combescure C, Le Gal G, Nendaz M, Perneger T, Bounameaux H, Perrier A, Righini M (2010) Clinical prediction rules for pulmonary embolism: a systematic review and meta-analysis. J Thromb Haemost 8(5):957–970
Wolf SJ, McCubbin TR, Feldhaus KM, Faragher JP, Adcock DM (2004) Prospective validation of Wells Criteria in the evaluation of patients with suspected pulmonary embolism. Ann Emerg Med 44(5):503–510
Schouten HJ, Geersing G, Koek H, Zuithoff NP, Janssen KJ, Douma RA, van Delden JJ, Moons KG, Reitsma JB (2013) Diagnostic accuracy of conventional or age adjusted d-dimer cut-off values in older patients with suspected venous thromboembolism: systematic review and meta-analysis. BMJ 346:f2492
Righini M, Van Es J, Den Exter PL, Roy P-M, Verschuren F, Ghuysen A, Rutschmann OT, Sanchez O, Jaffrelot M, Trinh-Duc A (2014) Age-adjusted d-dimer cut-off levels to rule out pulmonary embolism: the ADJUST-PE study. JAMA 311(11):1117–1124
Donati MB, Falanga A (2001) Pathogenetic mechanisms of thrombosis in malignancy. Acta Haematol 106(1–2):18–24
Molnar S, Guglielmone H, Lavarda M, Rizzi ML, Jarchum G (2007) Procoagulant factors in patients with cancer. Hematology 12(6):555–559
Lyman GH, Khorana AA (2009) Cancer, clots and consensus: new understanding of an old problem. J Clin Oncol 27(29):4821
Zhang L, Long Y, Xiao H, Yang J, Toulon P, Zhang Z (2018) Use of d-dimer in oral anticoagulation therapy. J Lab Hematol 40(5):503–507
Weitz JI, Eikelboom JW, Samama MM (2012) New antithrombotic drugs: antithrombotic therapy and prevention of thrombosis: American College of Chest Physicians evidence-based clinical practice guidelines. Chest 141(2):e120S-e151S
Ageno W, Gallus AS, Wittkowsky A, Crowther M, Hylek EM, Palareti G (2012) Oral anticoagulant therapy: antithrombotic therapy and prevention of thrombosis: American College of Chest Physicians evidence-based clinical practice guidelines. Chest 141(2):e44S-e88S
Author information
Authors and Affiliations
Contributions
HK—analysis and interpretation of data, and critical writing; YJK—analysis and interpretation of data, and critical writing; EJH—analysis and interpretation of data; BC—analysis and interpretation of data; YSL—conception and design, analysis and interpretation of data, critical writing and final approval.
Corresponding author
Ethics declarations
Conflict of interest
Not applicable.
Ethics approval
Our institutional review board approved the review of patient data (IRB no. 2017-1121).
Human and animal rights
This work has been conducted in full accordance with the ethical standards of the responsible institutional committee on human subjects as well as with the Helsinki Declaration.
Consent to participate
IRB waived informed consent due to its retrospective nature.
Consent for publication
Yes.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kwon, H., Kim, YJ., Her, EJ. et al. Elevation of the d-dimer cut-off level might be applicable to rule out pulmonary embolism for active cancer patients in the emergency department. Intern Emerg Med 17, 495–502 (2022). https://doi.org/10.1007/s11739-021-02730-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-021-02730-y