Abstract
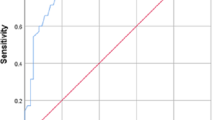
Anecdotal reports have suggested that hypokalemia is an independent predictor of mortality in patients with acute paraquat poisoning. However, the clinical significance of hypokalemia has not been systematically investigated in the early stage of paraquat poisoning. This study aimed to evaluate whether initial hypokalemia is a good predictor of mortality in patients with acute paraquat poisoning within 4 h. We retrospectively analyzed patients who were admitted to the emergency department after paraquat poisoning between September 2012 and January 2015. Demographic, clinical, and laboratory data were recorded, and the prognostic significance of hypokalemia was analyzed. A total of 120 patients were included. The 60-day mortality was 71.7 %. Serum potassium concentrations were significantly lower in non-survivors (3.1 ± 0.5 mmol/L) than in survivors (3.8 ± 0.3 mmol/L, P < 0.001). Independent predictors of death were amount of paraquat ingested (hazard ratio 1.005; 95 % confidence interval 1.002–1.007), serum potassium (0.498, 0.277–0.897), bicarbonate (0.934, 0.876–0.995), and white blood cell count (1.032, 1.001–1.065). For receiver operating characteristic curve analysis, serum potassium had an area under the curve of 0.852 (95 % confidence interval 0.784–0.920, P < 0.001), and the best cutoff value was 3.5 mmol/L (sensitivity, 88.2 %; specificity, 75.6 % in predicting survivors). Kaplan–Meier analysis showed that decreased serum potassium concentrations were associated with an increase in 60-day mortality (P < 0.001). Hypokalemia may be a reliable predictor in evaluating prognosis in paraquat poisoning within 4 h. The mechanism is not clear, and further studies verifying the precise mechanism of hypokalemia are required.



Similar content being viewed by others
References
Gawarammana IB, Buckley NA (2011) Medical management of paraquat ingestion. Br J Clin Pharmacol 72(5):745–757
Gil HW, Kang MS, Yang JO, Lee EY, Hong SY (2008) Association between plasma paraquat level and outcome of paraquat poisoning in 375 paraquat poisoning patients. Clin Toxicol (Phila) 46:515–518
Scherrmann JM, Houze P, Bismuth C, Bourdon R (1987) Prognostic value of plasma and urine paraquat concentration. Hum Toxicol 6:91–93
Hart TB, Nevitt A, Whitehead A (1984) A new statistical approach to the prognostic significance of plasma paraquat concentrations. Lancet 2:1222–1223
Senarathna L et al (2009) Prediction of outcome after paraquat poisoning by measurement of the plasma paraquat concentration. QJM 102:251–259
Lee Y et al (2012) Arterial lactate as a predictor of mortality in emergency department patients with paraquat intoxication. Clin Toxicol (Phila) 50:52–56
Liu X, Ma T, Qu B, Ji Y, Liu Z (2013) Prognostic value of initial arterial lactate level and lactate metabolic clearance rate in patients with acute paraquat poisoning. Am J Emerg Med 1–6
Zhang J et al (2015) The significance of serum uric acid level in humans with acute paraquat poisoning. Sci Rep 5:9168
Kang C et al (2013) Absolute lymphocyte count as a predictor of mortality in emergency department patients with paraquat poisoning. PLoS One 8:e78160
Mohamed F, Buckley NA, Jayamanne S et al (2015) Kidney damage biomarkers detect acute kidney injury but only functional markers predict mortality after paraquat ingestion. Toxicol Lett 237(2):140–150. doi:10.1016/j.toxlet.2015.06.008
Li Y, Wang M, Gao Y et al (2015) Abnormal pancreatic enzymes and their prognostic role after acute paraquat poisoning. Sci Rep 5:17299
Kim DS, Kang C, Kim DH et al (2015) External validation of the prognostic index in acute paraquat poisoning. Hum Exp Toxicol
Persson H, Sjöberg G, Haines J, Pronczuk GJ (1998) Poisoning severity score: grading of acute poisoning. J Toxicol Clin Toxicol 36:205–213
Huang NC, Lin SL, Hung YM, Hung SY, Chung HM (2003) Severity assessment in acute paraquat poisoning by analysis of APACHE II score. J Formos Med Assoc 102:782–787
Xu S, Hu H, Jiang Z et al (2015) APACHE score, severity index of paraquat poisoning, and serum lactic acid concentration in the prognosis of paraquat poisoning of Chinese patients. Pediatr Emerg Care 31(2):117–121
Weng CH et al (2012) Sequential organ failure assessment score can predict mortality in patients with paraquat intoxication. PLoS One 7:e51743
Wilks MF et al (2008) Improvement in survival after paraquat ingestion following introduction of a new formulation in Sri Lanka. PLoS Med 5:e49
Chang MW, Chang SS, Lee CC, Sheu BF, Young YR (2008) Hypokalemia and hypothermia are associated with 30-day mortality in patients with acute paraquat poisoning. Am J Med Sci 335(6):451–456
Lin TJ, Hung DZ, Yen HT, Ger J, Deng JF (1994) Survival of paraquat intoxication complicated with mediastinal emphysema: a case report. Zhonghua Yi Xue Za Zhi (Taipei) 54(5):363–367
Seok S, Kim YH, Gil HW, Song HY, Hong SY (2012) The time between paraquat ingestion and a negative dithionite urine test in an independent risk factor for death and organ failure in acute paraquat intoxication. J Korean Med Sci 27(9):993–998. doi:10.3346/jkms.2012.27.9.993
Yin Y, Guo X, Zhang SL, Sun CY (2013) Analysis of paraquat intoxication epidemic (2002–2011) within China. Biomed Environ Sci 26(6):509–512
Eddleston M, Wilks MF, Buckley NA (2003) Prospects for treatment of paraquat-induced lung fibrosis with immunosuppressive drugs and the need for better prediction of outcome: a systematic review. QJM 96(11):809–824 (review)
Coca SG, Perazella MA, Buller GK (2005) The cardiovascular implications of hypokalemia. Am J Kidney Dis 45(2):233–247 (review)
Gaduputi V, Chandrala C, Abbas N, Tariq H, Chilimuri S, Balar B (2014) Prognostic significance of hypokalemia in hepatic encephalopathy. Hepatogastroenterology 61(133):1170–1174
Szeto CC, Chow KM, Kwan BC, Leung CB, Chung KY, Law MC, Li PK (2005) Hypokalemia in Chinese peritoneal dialysis patients: prevalence and prognostic implication. Am J Kidney Dis 46(1):128–135
Jensen HK, Brabrand M, Vinholt PJ, Hallas J, Lassen AT (2015) Hypokalemia in acute medical patients: risk factors and prognosis. Am J Med 128(1):60–67
Giri SN, Curry DL, Stabenfeldt G, Spangler WL, Chandler DB, Schiedt MJ (1983) Effects of paraquat on plasma glucose, cortisol, catecholamines, and insulin in the beagle. Environ Res 30(1):80–88
Mohammadi-Bardbori A, Ghazi-Khansari M (2008) Alternative electron acceptors: proposed mechanism of paraquat mitochondrial toxicity. Environ Toxicol Pharmacol 26(1):1–5
Xu L, Xu J, Wang Z (2014) Molecular mechanisms of paraquat-induced acute lung injury: a current review. Drug Chem Toxicol 37(2):130–134
Perez GO, Oster JR, Vaamonde CA (1981) Serum potassium concentration in acidemic states. Nephron 27(4–5):233–243 (review)
Jensen HK, Brabrand M, Vinholt PJ, Hallas J, Lassen AT (2015) Hypokalemia in acute medical patients: risk factors and prognosis. Am J Med 128(1):60–67
El-Sherif N, Turitto G (2011) Electrolyte disorders and arrhythmogenesis. Cardiol J. 18(3):233–245 (review)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by the Projects of Medical and Health Technology Development Program in Shandong Province (project number: 2014WS0084).
Conflict of interest
The authors declare that they have no conflicts of interests.
Statement of human and animal rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Liu, ZQ., Wang, HS. & Gu, Y. Hypokalemia is a biochemical signal of poor prognosis for acute paraquat poisoning within 4 hours. Intern Emerg Med 12, 837–843 (2017). https://doi.org/10.1007/s11739-016-1491-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-016-1491-x