Abstract
Introduction
Non-alcoholic fatty liver disease (NAFLD) is considered the most common liver disease worldwide and is highly associated with obesity. The prevalences of both conditions have markedly increased in the Western civilization. Bariatric surgery is the most effective treatment for morbid obesity and its comorbidities such as NAFLD.
Objectives
Measure postoperative liver fat fraction (LFF) in bariatric patients by using in-opposed-phase MRI, a widely available clinical tool validated for the quantification of liver fat
Methods
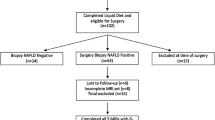
Retrospective analyses of participants, who underwent laparoscopic Roux-Y-gastric-bypass (17) or laparoscopic sleeve gastrectomy (2) were performed using magnetic resonance imaging (MRI), bioelectrical impedance analysis (BIA), and anthropometric measurements 1 day before surgery, as well as 6, 12, and 24 weeks after surgery, LFF was calculated from fat-only and water-only MR images.
Results
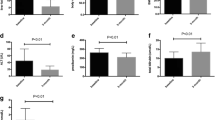
Six months after surgery, a significant decrease of LFF and liver volume has been observed along with weight loss, decreased waist circumference, and parameters obtained by body fat measured by BIA. LFF significantly correlated with liver volume in the postoperative course.
Conclusions
MRI including in-opposed-phase imaging of the liver can detect the quantitative decrease of fatty infiltration within the liver after bariatric surgery and thus could be a valuable tool to monitor NAFLD/NASH postoperatively.




Similar content being viewed by others
References
Browning JD, Szczepaniak LS, Dobbins R, et al. Prevalence of hepatic steatosis in an urban population in the United States: impact of ethnicity. Hepatology. 2004;40(6):1387–95.
Dietrich P, Hellerbrand C. Non-alcoholic fatty liver disease, obesity and the metabolic syndrome. Best Pract Res Clin Gastroenterol. 2014;28(4):637–53.
Vernon G, Baranova A, Younossi ZM. Systematic review: the epidemiology and natural history of non-alcoholic fatty liver disease and non-alcoholic steatohepatitis in adults. Aliment Pharmacol Ther. 2011;34(3):274–85.
Joseph AE, Saverymuttu SH, al-Sam S, et al. Comparison of liver histology with ultrasonography in assessing diffuse parenchymal liver disease. Clin Radiol. 1991;43(1):26–31.
Ble M, Procopet B, Miquel R, et al. Transjugular liver biopsy. Clin Liver Dis. 2014;18(4):767–78.
Rockey DC, Caldwell SH, Goodman ZD, et al. American Association for the Study of liver D. Liver biopsy Hepatology. 2009;49(3):1017–44.
Schwenzer NF, Springer F, Schraml C, et al. Non-invasive assessment and quantification of liver steatosis by ultrasound, computed tomography and magnetic resonance. J Hepatol. 2009;51(3):433–45.
Kuhn JP, Hernando D, Mensel B, et al. Quantitative chemical shift-encoded MRI is an accurate method to quantify hepatic steatosis. J Magn Reson Imaging. 2014;39(6):1494–501.
Reeder SB, Cruite I, Hamilton G, et al. Quantitative assessment of liver fat with magnetic resonance imaging and spectroscopy. J Magn Reson Imaging. 2011;34(4):729–49.
Mottin CC, Moretto M, Padoin AV, et al. The role of ultrasound in the diagnosis of hepatic steatosis in morbidly obese patients. Obes Surg. 2004;14(5):635–7.
Christou NV, MacLean LD. Effect of bariatric surgery on long-term mortality. Adv Surg. 2005;39:165–79.
Sjostrom L, Narbro K, Sjostrom CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357(8):741–52.
Lassailly G, Caiazzo R, Buob D, et al. Bariatric surgery reduces features of nonalcoholic steatohepatitis in morbidly obese patients. Gastroenterology. 2015;149(2):379–88. quiz e15-6
Wree A, Schlattjan M, Bechmann LP, et al. Adipocyte cell size, free fatty acids and apolipoproteins are associated with non-alcoholic liver injury progression in severely obese patients. Metabolism. 2014;63(12):1542–52.
Mummadi RR, Kasturi KS, Chennareddygari S, et al. Effect of bariatric surgery on nonalcoholic fatty liver disease: systematic review and meta-analysis. Clin Gastroenterol Hepatol. 2008;6(12):1396–402.
Otto M, Farber J, Haneder S, Michaely H, Kienle P, Hasenberg T. Postoperative Changes in Body Composition-Comparison of Bioelectrical Impedance Analysis and Magnetic Resonance Imaging in Bariatric Patients. Obes Surg. 2014.
Kyle UG, Bosaeus I, De Lorenzo AD, et al. Bioelectrical impedance analysis-part II: utilization in clinical practice. Clin Nutr. 2004;23(6):1430–53.
Dixon WT. Simple proton spectroscopic imaging. Radiology. 1984;153(1):189–94.
Lazo M, Clark JM. The epidemiology of nonalcoholic fatty liver disease: a global perspective. Semin Liver Dis. 2008;28(4):339–50.
Ahmed A, Wong RJ, Harrison SA. Nonalcoholic Fatty Liver Disease Review: Diagnosis, Treatment, and Outcomes. Clin Gastroenterol Hepatol. 2015.
Ertle J, Dechene A, Sowa JP, et al. Non-alcoholic fatty liver disease progresses to hepatocellular carcinoma in the absence of apparent cirrhosis. Int J Cancer. 2011;128(10):2436–43.
Dyson J, Jaques B, Chattopadyhay D, et al. Hepatocellular cancer: the impact of obesity, type 2 diabetes and a multidisciplinary team. J Hepatol. 2014;60(1):110–7.
Immonen H, Hannukainen JC, Iozzo P, et al. Effect of bariatric surgery on liver glucose metabolism in morbidly obese diabetic and non-diabetic patients. J Hepatol. 2014;60(2):377–83.
Ribaric G, Buchwald JN, McGlennon TW. Diabetes and weight in comparative studies of bariatric surgery vs conventional medical therapy: a systematic review and meta-analysis. Obes Surg. 2014;24(3):437–55.
Boza C, Riquelme A, Ibanez L, et al. Predictors of nonalcoholic steatohepatitis (NASH) in obese patients undergoing gastric bypass. Obes Surg. 2005;15(8):1148–53.
Reha JL, Lee S, Hofmann LJ. Prevalence and predictors of nonalcoholic steatohepatitis in obese patients undergoing bariatric surgery: a Department of Defense experience. Am Surg. 2014;80(6):595–9.
Xanthakos SA, Jenkins TM, Kleiner DE, et al. High prevalence of nonalcoholic fatty liver disease in adolescents undergoing bariatric surgery. Gastroenterology. 2015;149(3):623–34. e8
Hamer OW, Aguirre DA, Casola G, et al. Fatty liver: imaging patterns and pitfalls. Radiographics. 2006;26(6):1637–53.
Wu CH, Ho MC, Jeng YM, et al. Quantification of hepatic steatosis: a comparison of the accuracy among multiple magnetic resonance techniques. J Gastroenterol Hepatol. 2014;29(4):807–13.
Johansson L, Roos M, Kullberg J, et al. Lipid mobilization following roux-en-Y gastric bypass examined by magnetic resonance imaging and spectroscopy. Obes Surg. 2008;18(10):1297–304.
Heath ML, Kow L, Slavotinek JP, et al. Abdominal adiposity and liver fat content 3 and 12 months after gastric banding surgery. Metabolism. 2009;58(6):753–8.
Thomas EL, Hamilton G, Patel N, et al. Hepatic triglyceride content and its relation to body adiposity: a magnetic resonance imaging and proton magnetic resonance spectroscopy study. Gut. 2005;54(1):122–7.
Colles SL, Dixon JB, Marks P, et al. Preoperative weight loss with a very-low-energy diet: quantitation of changes in liver and abdominal fat by serial imaging. Am J Clin Nutr. 2006;84(2):304–11.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Statement of Informed Consent
Informed consent was obtained from all individual participants included in the study.
Financial Supports
None.
Additional information
Dennis Hedderich and Till Hasenberg contributed equally to this publication
Rights and permissions
About this article
Cite this article
Hedderich, D.M., Hasenberg, T., Haneder, S. et al. Effects of Bariatric Surgery on Non-alcoholic Fatty Liver Disease: Magnetic Resonance Imaging Is an Effective, Non-invasive Method to Evaluate Changes in the Liver Fat Fraction. OBES SURG 27, 1755–1762 (2017). https://doi.org/10.1007/s11695-016-2531-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-016-2531-3