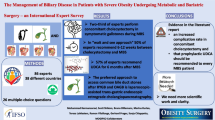
Background
Nonalcoholic fatty liver disease (NAFLD) has been increasingly recognized as a common chronic liver condition. Previous studies have been variable regarding the histological outcomes after rapid weight loss. The aim of this study was to characterize the histopathologic changes in NASH following laparoscopic Roux-en-Y Gastric Bypass surgery (LRYGBP).
Methods
We retrospectively analyzed paired needle liver biopsies taken during and following LRYGBP in 39 patients according to the recent NIH-based NAFLD criteria.
Results
The cohort included 33 females and 6 males (range 24–7 years). 23 patients (58.9%) had steatohepatitis, 12 with fatty liver (30.7%), and 4 were normal (10.2%). Follow-up needle liver biopsies were performed at a mean interval of 18 months (range 6–1 months). No significant differences in length or number of portal tracts between the paired biopsies were noted. The mean decrease in weight and BMI was 50.2 kg and 18.2 kg/m2, respectively. The initial prevalence of hepatic pathology: steatosis (89.7%), hepatocellular ballooning (58.9%), and centrilobular/perisinusoidal fibrosis (50%) improved significantly after LRYGBP: steatosis (2.9%), ballooning (0%), and centrilobular fibrosis (25%). Mitigation in the lobular inflammation score (2.23 ±–.63 vs 1.95 ±–.56, P––.01) and stage of fibrosis (1.14 ±–.05 to 0.72 ±–.97, P––.002) were also noted. However, no improvements were detected in portal tract inflammation and fibrosis.
Conclusions
Over a mean period of 18 months, histological improvements and resolution of NASH occurs after LRYGBP. Long-term studies are warranted to assess for potential changes in the portal regions or relapse of NASH that could result with weight regain or malnutrition.
Similar content being viewed by others
References
O’Brien PE, Dixon JB. The extent of the problem of obesity. Am J Surg 2002; 184: 4S–S.
Abrams GA, Kunde SS, Lazenby AJ et al. Portal fibrosis and hepatic steatosis in morbidly obese subjects: A spectrum of nonalcoholic fatty liver disease. Hepatology 2004; 40: 475–3.
Harrison SA, Di Bisceglie AM. Advances in the understanding and treatment of nonalcoholic fatty liver disease. Drugs 2003; 63: 2379–4.
Ludwig J, Viggiano TR, McGill DB et al. Nonalcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease. Mayo Clin Proc 1980; 55: 434–.
Brunt EM, Janney CG, Di Bisceglie AM et al. Nonalcoholic steatohepatitis: a proposal for grading and staging the histological lesions. Am J Gastroenterol 1999; 94: 2467–4.
Kleiner DE, Brunt EM, Van Natta M et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 2005; 41: 1313–1.
Sanyal AJ. AGA technical review on nonalcoholic fatty liver disease. Gastroenterology 2002; 123: 1705–5.
Rosenthal RJ, Szomstein S, Kennedy CI et al. Laparoscopic surgery for morbid obesity: 1,001 consecutive bariatric operations performed at the bariatric institute, Cleveland Clinic Florida. Obes Surg 2006; 16: 119–4.
Clark JM, Alkhuraishi AR, Solga SF et al. Roux-en-Y gastric bypass improves liver histology in patients with non-alcoholic fatty liver disease. Obes Res 2005; 13: 1180–.
Mattar SG, Velcu LM, Rabinovitz M et al. Surgicallyinduced weight loss significantly improves nonalcoholic fatty liver disease and the metabolic syndrome. Ann Surg 2005; 242: 610–; discussion 618–0.
Mathurin P, Gonzalez F, Kerdraon O et al. The evolution of severe steatosis after bariatric surgery is related to insulin resistance. Gastroenterology 2006; 130: 1617–4.
Barker KB, Palekar NA, Bowers SP et al. Non-alcoholic steatohepatitis: effect of Roux-en-Y gastric bypass surgery. Am J Gastroenterol 2006; 101: 368–3.
Klein S, Mittendorfer B, Eagon JC et al. Gastric bypass surgery improves metabolic and hepatic abnormalities associated with nonalcoholic fatty liver disease. Gastroenterology 2006; 130: 1564–2.
Dixon JB, Bhathal PS, Hughes NR et al. Nonalcoholic fatty liver disease: Improvement in liver histological analysis with weight loss. Hepatology 2004; 39: 1647–4.
Korenkov M, Sauerland S, Junginger T. Surgery for obesity. Curr Opin Gastroenterol 2005; 21: 679–3.
Chitturi S, Farrell GC. Etiopathogenesis of nonalcoholic steatohepatitis. Semin Liver Dis 2001; 21: 27–1.
Sanyal AJ, Campbell-Sargent C, Mirshahi F et al. Nonalcoholic steatohepatitis: association of insulin resistance and mitochondrial abnormalities. Gastroenterology 2001; 120: 1183–2.
Chitturi S, Abeygunasekera S, Farrell GC et al. NASH and insulin resistance: Insulin hypersecretion and specific association with the insulin resistance syndrome. Hepatology 2002; 35: 373–.
Marchesini G, Bugianesi E, Forlani G et al. Nonalcoholic fatty liver, steatohepatitis, and the metabolic syndrome. Hepatology 2003; 37: 917–3.
Neuschwander-Tetri BA, Brunt EM, Wehmeier KR et al. Improved nonalcoholic steatohepatitis after 48 weeks of treatment with the PPAR-gamma ligand rosiglitazone. Hepatology 2003; 38: 1008–7.
Sanyal AJ, Mofrad PS, Contos MJ et al. A pilot study of vitamin E versus vitamin E and pioglitazone for the treatment of nonalcoholic steatohepatitis. Clin Gastroenterol Hepatol 2004; 2: 1107–5.
Promrat K, Lutchman G, Uwaifo GI et al. A pilot study of pioglitazone treatment for nonalcoholic steatohepatitis. Hepatology 2004; 39: 188–6.
Bugianesi E, Marzocchi R, Villanova N et al. Non-alcoholic fatty liver disease/non-alcoholic steatohepatitis (NAFLD/NASH): treatment. Best Pract Res Clin Gastroenterol 2004; 18: 1105–6.
Huang MA, Greenson JK, Chao C et al. One-year intense nutritional counseling results in histological improvement in patients with non-alcoholic steatohepatitis: a pilot study. Am J Gastroenterol 2005; 100: 1072–1.
Rucker RD Jr, Chan EK, Horstmann J et al. Searching for the best weight reduction operation. Surgery 1984; 96: 624–1.
Luyckx FH, Desaive C, Thiry A et al. Liver abnormalities in severely obese subjects: effect of drastic weight loss after gastroplasty. Int J Obes 1998; 22: 222–.
Stratopoulos C, Papakonstantinou A, Terzis I et al. Changes in liver histology accompanying massive weight loss after gastroplasty for morbid obesity. Obes Surg 2005; 15: 1154–0.
Csendes A, Smok G, Burgos AM. Histological findings in the liver before and after gastric bypass. Obes Surg 2006; 16: 607–1.
de Almeida SR, Rocha PR, Sanches MD et al. Roux-en-Y gastric bypass improves the nonalcoholic steatohepatitis (NASH) of morbid obesity. Obes Surg 2006; 16: 270–.
Zimmerman HJ, Ishak KG. Hepatic injury due to drugs and toxins. In: MacSween RN, Burt AD, Ishak KG et al, eds. Pathology of Liver, 4th Edn. London: Churchill Livingstone 2002: 654–.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liu, X., Lazenby, A.J., Clements, R.H. et al. Resolution of Nonalcoholic Steatohepatits after Gastric Bypass Surgery. OBES SURG 17, 486–492 (2007). https://doi.org/10.1007/s11695-007-9086-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-007-9086-2